Abstract
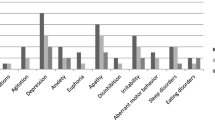
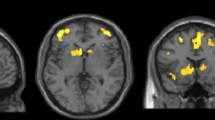
Depression is highly common in Progressive Supranuclear Palsy (PSP) and is a meaningful determinant of quality of life. However, neurobiological and neuroimaging correlates of this neuropsychiatric disturbance in PSP patients are still unknown. In this study, we aimed to investigate the topographical distribution of morphometric changes associated with depression in PSP patients using cortical thickness. Forty patients with PSP were evaluated at baseline with clinical rating scales and MRI scans. Based on the response to the 15-item Geriatric Depression Scale we identified 21 PSP patients with depression (GDS-15 score ≥ 5) and 19 PSP patients without depression (GDS-15 score < 5). In vertex-wise analysis, comparison of cortical thickness between PSP patients with and without depression was performed using a general linear model. PSP patients with depressions showed reduced cortical thickness in temporo-parieto-occipital areas, more pronounced in the right hemisphere. These findings propose neurobiological conceptualizations of depression in PSP as being associated with a multiregional pattern of morphometric grey matter reduction.

Similar content being viewed by others
References
Boxer AL, Yu JT, Golbe LI, Litvan I, Lang AE, Höglinger GU (2017) Advances in progressive supranuclear palsy: new diagnostic criteria, biomarkers, and therapeutic approaches. Lancet Neurol 16(7):552–563
Hauw JJ, Daniel SE, Dickson D, Horoupian DS, Jellinger K, Lantos PL et al (1994) Preliminary NINDS neuropathologic criteria for Steele-Richardson-Olszewski syndrome (progressive supranuclear palsy). Neurology 44(11):2015–2019
Jellinger KA, Bancher C, Hauw JJ, Verny M (1995) Progressive supranuclear palsy: neuropathologically based diagnostic clinical criteria. J Neurol Neurosurg Psychiatry 59(1):106
Bloise MC, Berardelli I, Roselli V, Pasquini M, Stirpe P, Colosimo C et al (2014) Psychiatric disturbances in patients with progressive supranuclear palsy: a case-control study. Parkinsonism Relat Disord 20(9):965–968
Santangelo G, Cuoco S, Pellecchia MT, Erro R, Barone P, Picillo M (2018) Comparative cognitive and neuropsychiatric profiles between Parkinson’s disease, multiple system atrophy and progressive supranuclear palsy. J Neurol 265(11):2602–2613
Esmonde T, Giles E, Gibson M, Hodges JR (1996) Neuropsychological performance, disease severity, and depression in progressive supranuclear palsy. J Neurol 243(9):638–643
Radicati FG, Martinez Martin P, Fossati C, Chaudhuri KR, Torti M, Rodriguez Blazquez C et al (2017) Non motor symptoms in progressive supranuclear palsy: prevalence and severity. NPJ Parkinsons Dis 3:35
Flavell J, Nestor PJ (2021) A systematic review of apathy and depression in progressive supranuclear palsy. J Geriatr Psychiatry Neurol. https://doi.org/10.1177/0891988721993545
Winter Y, Spottke AE, Stamelou M, Cabanel N, Eggert K, Höglinger GU et al (2011) Health-related quality of life in multiple system atrophy and progressive supranuclear palsy. Neurodegener Dis 8(6):438–446
Aarsland D, Litvan I, Larsen JP (2001) Neuropsychiatric symptoms of patients with progressive supranuclear palsy and Parkinson’s disease. J Neuropsychiatry Clin Neurosci 13(1):42–49
Painous C, Martí MJ, Simonet C, Garrido A, Valldeoriola F, Muñoz E et al (2020) Prediagnostic motor and non-motor symptoms in progressive supranuclear palsy: the step-back PSP study. Parkinsonism Relat Disord 74:67–73
Schrag A, Sheikh S, Quinn NP, Lees AJ, Selai C, Mathias C et al (2010) A comparison of depression, anxiety, and health status in patients with progressive supranuclear palsy and multiple system atrophy. Mov Disord 25(8):1077–1081
Tsai RM, Lobach I, Bang J, Whitwell JL, Senjem ML, Jack CR Jr et al (2016) Clinical correlates of longitudinal brain atrophy in progressive supranuclear palsy. Parkinsonism Relat Disord 28:29–35
Bang J, Lobach IV, Lang AE, Grossman M, Knopman DS, Miller BL et al (2016) Predicting disease progression in progressive supranuclear palsy in multicenter clinical trials. Parkinsonism Relat Disord 28:41–48
Lamb R, Rohrer JD, Lees AJ, Morris HR (2016) Progressive supranuclear palsy and corticobasal degeneration: pathophysiology and treatment options. Curr Treat Options Neurol 18(9):42
Wise T, Cleare AJ, Herane A, Young AH, Arnone D (2014) Diagnostic and therapeutic utility of neuroimaging in depression: an overview. Neuropsychiatr Dis Treat 10:1509–1522
Kandilarova S, Stoyanov D, Sirakov N, Maes M, Specht K (2019) Reduced grey matter volume in frontal and temporal areas in depression: contributions from voxel-based morphometry study. Acta Neuropsychiatr 31(5):252–257
Arnone D, Job D, Selvaraj S, Abe O, Amico F, Cheng Y et al (2016) Computational meta-analysis of statistical parametric maps in major depression. Hum Brain Mapp 37(4):1393–1404
Chagas MH, Linares IM, Garcia GJ, Hallak JE, Tumas V, Crippa JA (2013) Neuroimaging of depression in Parkinson’s disease: a review. Int Psychogeriatr 25(12):1953–1961
Feldmann A, Illes Z, Kosztolanyi P, Illes E, Mike A, Kover F et al (2008) Morphometric changes of gray matter in Parkinson’s disease with depression: a voxel-based morphometry study. Mov Disord 23(1):42–46
Abé C, Ekman CJ, Sellgren C, Petrovic P, Ingvar M, Landén M (2016) Cortical thickness, volume and surface area in patients with bipolar disorder types I and II. J Psychiatry Neurosci 41(4):240–250
Zuo Z, Ran S, Wang Y, Li C, Han Q, Tang Q et al (2019) Asymmetry in cortical thickness and subcortical volume in treatment-naïve major depressive disorder. NeuroImage Clinical. 21:101614
Niu M, Wang Y, Jia Y, Wang J, Zhong S, Lin J et al (2017) Common and specific abnormalities in cortical thickness in patients with major depressive and bipolar disorders. EBioMedicine 16:162–171
Peterson BS, Weissman MM (2011) A brain-based endophenotype for major depressive disorder. Annu Rev Med 62:461–474
Litvan I, Agid Y, Calne D, Campbell G, Dubois B, Duvoisin RC et al (1996) Clinical research criteria for the diagnosis of progressive supranuclear palsy (Steele-Richardson-Olszewski syndrome): report of the NINDS-SPSP international workshop. Neurology 47(1):1–9
Boxer AL, Lang AE, Grossman M, Knopman DS, Miller BL, Schneider LS et al (2014) Davunetide in patients with progressive supranuclear palsy: a randomised, double-blind, placebo-controlled phase 2/3 trial. Lancet Neurol 13(7):676–685
Folstein MF, Folstein SE, McHugh PR (1975) “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12(3):189–198
Goetz CG, Tilley BC, Shaftman SR, Stebbins GT, Fahn S, Martinez-Martin P et al (2008) Movement Disorder Society-sponsored revision of the Unified Parkinson’s Disease Rating Scale (MDS-UPDRS): scale presentation and clinimetric testing results. Mov Disord 23(15):2129–2170
Golbe LI, Ohman-Strickland PA (2007) A clinical rating scale for progressive supranuclear palsy. Brain 130(Pt 6):1552–1565
Morris JC (1993) The Clinical Dementia Rating (CDR): current version and scoring rules. Neurology 43(11):2412–2414
Pfeffer RI, Kurosaki TT, Harrah CH Jr, Chance JM, Filos S (1982) Measurement of functional activities in older adults in the community. J Gerontol 37(3):323–329
Yesavage JA, Brink TL, Rose TL, Lum O, Huang V, Adey M et al (1982) Development and validation of a geriatric depression screening scale: a preliminary report. J Psychiatr Res 17(1):37–49
Dahnke R, Yotter RA, Gaser C (2013) Cortical thickness and central surface estimation. Neuroimage 65:336–348
Goel V, Gold B, Kapur S, Houle S (1998) Neuroanatomical correlates of human reasoning. J Cogn Neurosci 10(3):293–302
Pourtois G, de Gelder B, Bol A, Crommelinck M (2005) Perception of facial expressions and voices and of their combination in the human brain. Cortex 41(1):49–59
Wildgruber D, Riecker A, Hertrich I, Erb M, Grodd W, Ethofer T et al (2005) Identification of emotional intonation evaluated by fMRI. Neuroimage 24(4):1233–1241
Buckner RL, Andrews-Hanna JR, Schacter DL (2008) The brain’s default network: anatomy, function, and relevance to disease. Ann N Y Acad Sci 1124:1–38
Ferri J, Schmidt J, Hajcak G, Canli T (2016) Emotion regulation and amygdala-precuneus connectivity: focusing on attentional deployment. Cogn Affect Behav Neurosci 16(6):991–1002
Mulders PC, van Eijndhoven PF, Schene AH, Beckmann CF, Tendolkar I (2015) Resting-state functional connectivity in major depressive disorder: a review. Neurosci Biobehav Rev 56:330–344
Zanigni S, Sambati L, Evangelisti S, Testa C, Calandra-Buonaura G, Manners DN et al (2017) Precuneal thickness and depression in parkinson disease. Neurodegener Dis 17(2–3):97–102
Brenneis C, Seppi K, Schocke M, Benke T, Wenning GK, Poewe W (2004) Voxel based morphometry reveals a distinct pattern of frontal atrophy in progressive supranuclear palsy. J Neurol Neurosurg Psychiatry 75(2):246–249
Cordato NJ, Pantelis C, Halliday GM, Velakoulis D, Wood SJ, Stuart GW et al (2002) Frontal atrophy correlates with behavioural changes in progressive supranuclear palsy. Brain 125(Pt 4):789–800
Blin J, Baron JC, Dubois B, Pillon B, Cambon H, Cambier J et al (1990) Positron emission tomography study in progressive supranuclear palsy. Brain hypometabolic pattern and clinicometabolic correlations. Arch Neurol 47(7):747–752
Mackin RS, Tosun D, Mueller SG, Lee J-Y, Insel P, Schuff N et al (2013) Patterns of reduced cortical thickness in late-life depression and relationship to psychotherapeutic response. Am J Geriatr Psychiatry 21(8):794–802
Steele JC, Richardson JC, Olszewski J (1964) Progressive supranuclear palsy. A heterogeneous degeneration involving the brain stem, basal ganglia and cerebellum with vertical gaze and pseudobulbar palsy, nuchal dystonia and dementia. Arch Neurol 10:333–359
Murley AG, Rowe JB (2018) Neurotransmitter deficits from frontotemporal lobar degeneration. Brain 141(5):1263–1285
Acknowledgements
Data used in preparation of this article were obtained from the 4-Repeat Tauopathy Neuroimaging Initiative (4RTNI) database (http://4rtni-ftldni.ini.usc.edu). The investigators at 4RTNI contributed to the design and implementation of 4RTNI and/or provided data, but did not participate in analysis or writing of this report (unless otherwise listed).
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflicts of interest
Nothing to report.
Ethical approval
Approval for the 4RTNI protocol has been granted by institutional review board at the study site. Research involves only previously collected and fully anonymised data so further ethical approval was not required.
Additional information
Data used in preparation of this article were obtained from the 4-Repeat Tauopathy Neuroimaging Initiative (4RTNI) database (http://4rtni-ftldni.ini.usc.edu). The investigators at 4RTNI contributed to the design and implementation of 4RTNI and/or provided data, but did not participate in analysis or writing of this report (unless otherwise listed).
Rights and permissions
About this article
Cite this article
Urso, D., Tafuri, B., De Blasi, R. et al. Imaging correlates of depression in progressive supranuclear palsy. J Neurol 269, 3522–3528 (2022). https://doi.org/10.1007/s00415-021-10939-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-021-10939-2