Abstract
Background and purpose
The diagnostic value of non-contrast CT (NCCT) in acute stroke imaging remains indispensable, especially under emergency conditions with limited resources. The radiological conjugate eye deviation (RCED) has been demonstrated as a NCCT sign to predict acute ischemic stroke (AIS) or AIS secondary to large vessel occlusion (LVO) in recent studies. We performed a meta-analysis to gain a better understanding into the predictive role of RCED for AISs and LVO-AISs.
Methods
We conducted a systematic literature search using PubMed, Embase, and Cochrane. The search focused on studies published between January 2000 and August 2020 that reported the predictive value of RCED for the diagnosis of AIS or LVO-AIS. Principal measurements of the meta-analysis were the overall sensitivity, specificity, the positive likelihood ratio (PLR), and the negative likelihood ratio (NLR) of RCED in predicting AIS and LVO-AIS.
Results
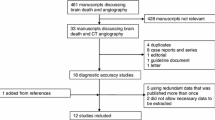
We included 11 studies (n = 2304). For AIS, RCED had a sensitivity of 0.37 (95% CI 0.27–0.47), a specificity of 0.86 (95% CI 0.73–0.93), the area under the receiver operating characteristic curve (AUC) was 0.58 (95% CI 0.53–0.62), PLR was 2.5 (95% CI 1.5–4.4), and NLR was 0.74 (95% CI 0.65–0.84). For LVO-AIS, RCED had a sensitivity of 0.63 (95% CI 0.46–0.77), a specificity of 0.77 (95% CI 0.71–0.82), AUC was 0.63 (95% CI 0.46–0.77), PLR was 2.7 (95% CI 1.7–4.3), and NLR was 0.49 (95% CI 0.3–0.78).
Conclusion
RCED can be used to predict LVO-AIS. It is expected that this method will be extensively used and validated in acute stroke imaging, especially under emergency conditions with limited resources.






Similar content being viewed by others
References
Berkhemer OA, Fransen PSS, Beumer D et al (2015) A randomized trial of intraarterial treatment for acute ischemic stroke. New Engl J Med 372:11–20. https://doi.org/10.1056/NEJMoa1411587
Saver JL (2006) Time is brain—quantified. Stroke 37:263–266. https://doi.org/10.1161/01.STR.0000196957.55928.ab
Aronovich BD, Reider-Groswasser II, Segev Y et al (2004) Early CT changes and outcome of ischemic stroke. Eur J Neurol 11:63–65. https://doi.org/10.1046/j.1351-5101.2003.00708.x
Alshoabi S, Alnajmani R, Shamsuddin M et al (2019) Early signs of middle cerebral artery infarction on multidetector computed tomography: review of 20 cases. Brain Circ 5:27–31. https://doi.org/10.4103/bc.bc_28_18
Haussen DC, Lima A, Frankel M et al (2015) Sulcal effacement with preserved gray-white junction a sign of reversible ischemia. Stroke 46:1704–1706. https://doi.org/10.1161/strokeaha.115.009304
Manno EM, Nichols DA, Fulgham JR et al (2003) Computed tomographic determinants of neurologic deterioration in patients with large middle cerebral artery infarctions. Mayo Clin Proc 78:156–160. https://doi.org/10.4065/78.2.156
Sarikaya B, Provenzale J (2010) Frequency of various brain parenchymal findings of early cerebral ischemia on unenhanced CT scans. Emerg Radiol 17:381–390. https://doi.org/10.1007/s10140-010-0870-2
Shah NH, Bhatt N, Tipirneni A et al (2017) Conjugate eye deviation on CT associated with worse outcomes despite IV thrombolysis. Neurohospitalist 7:74–77. https://doi.org/10.1177/1941874416674603
Attenhofer KS, Hailey L, Mortin M et al (2018) The sustained DeyeCOM sign as a predictor of large vessel occlusions and stroke mimics. J Stroke Cerebrovasc Dis 27:1466–1470. https://doi.org/10.1016/j.jstrokecerebrovasdis.2017.12.035
Kobayashi M (2018) Horizontal gaze deviation on computed tomography: the visual criterion and lesion characteristics in ischemic stroke. Acta Neurol Belg 118:581–587. https://doi.org/10.1007/s13760-018-0949-1
Jiang NN, Fong C, Sahlas DJ et al (2019) Degree of conjugate gaze deviation on CT predicts proximal vessel occlusion and may expedite endovascular therapy. J Stroke Cerebrovasc Dis 28:1093–1098. https://doi.org/10.1016/j.jstrokecerebrovasdis.2018.12.037
McCluskey G, Hunter A, Best E et al (2019) Radiological eye deviation as a predictor of large vessel occlusion in acute ischaemic stroke. Eur Stroke J 4:419–420. https://doi.org/10.1177/2396987319845581
Mahajan V, Minshew PT, Khoury J et al (2008) Eye position information on CT increases the identification of acute ischemic hypoattenuation. Am J Neuroradiol 29:1144–1146. https://doi.org/10.3174/ajnr.A0995
Berger MF, Pross RD, Ilg UJ et al (2006) Deviation of eyes and head in acute cerebral stroke. BMC Neurol 6:23. https://doi.org/10.1186/1471-2377-6-23
Schwartz KM, Ahmed AT, Fugate JE et al (2012) Frequency of eye deviation in stroke and non-stroke patients undergoing head CT. Neurocrit Care 17:45–48. https://doi.org/10.1007/s12028-012-9717-x
McKean D, Kudari M, Landells M et al (2014) Validating a threshold of ocular gaze deviation for the prediction of acute ischaemic stroke. Clin Radiol 69:1244–1248. https://doi.org/10.1016/j.crad.2014.07.011
Coffman CR, Raman R, Ernstrom K et al (2015) The DeyeCOM sign: predictive value in acute stroke code evaluations. J Stroke Cerebrovasc Dis 24:1299–1304. https://doi.org/10.1016/j.jstrokecerebrovasdis.2015.01.040
Kaditis DG, Zintzaras E, Sali D et al (2016) Conjugate eye deviation as predictor of acute cortical and subcortical ischemic brain lesions. Clin Neurol Neurosurg 143:80–85. https://doi.org/10.1016/j.clineuro.2016.02.011
Spokoyny I, Chen JY, Raman R et al (2016) Visual determination of conjugate eye deviation on computed tomography scan predicts diagnosis of stroke code patients. J Stroke Cerebrovasc Dis 25:2809–2813. https://doi.org/10.1016/j.jstrokecerebrovasdis.2016.07.039
Payabvash S, Qureshi I, Qureshi AI (2016) Clinical implications of eye deviation on admission CT examination of acute ischaemic stroke patients. Clin Radiol 71:1314.e11-e15. https://doi.org/10.1016/j.crad.2016.08.002
Lesley WS, Rangaswamy R, Smith KH et al (2009) Predicting acute ischemic stroke by measuring the degree of ocular gaze deviation (Prevost’s sign) on CT. J Neurointerv Surg 1:32–34. https://doi.org/10.1136/jnis.2009.000281
Liberati A, Altman DG, Tetzlaff J et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. Bmj Br Med J. https://doi.org/10.1136/bmj.b2700
Phipps MS, Cronin CA (2020) Management of acute ischemic stroke. Bmj Br Med J. https://doi.org/10.1136/bmj.l6983
Whiting PF, Rutjes AWS, Westwood ME et al (2011) QUADAS-2: A revised tool for the quality assessment of diagnostic accuracy studies. Ann Intern Med 155:529-U104. https://doi.org/10.7326/0003-4819-155-8-201110180-00009
Reitsma JB, Glas AS, Rutjes AWS et al (2005) Bivariate analysis of sensitivity and specificity produces informative summary measures in diagnostic reviews. J Clin Epidemiol 58:982–990. https://doi.org/10.1016/j.jclinepi.2005.02.022
Walter S, Kostpopoulos P, Haass A et al (2010) Bringing the hospital to the patient: first treatment of stroke patients at the emergency site. PLoS ONE. https://doi.org/10.1371/journal.pone.0013758
Walter S, Ragoschke-Schumm A, Lesmeister M et al (2018) Mobile stroke unit use for prehospital stroke treatment: an update. Radiologe 58:24–28. https://doi.org/10.1007/s00117-018-0408-2
Fassbender K, Grotta JC, Walter S et al (2017) Mobile stroke units for prehospital thrombolysis, triage, and beyond: benefits and challenges. Lancet Neurol 16:227–237. https://doi.org/10.1016/s1474-4422(17)30008-x
Powers WJ, Rabinstein AA, Ackerson T et al (2019) Guidelines for the early management of patients with acute ischemic stroke: 2019 update to the 2018 guidelines for the early management of acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 50:E344–E418. https://doi.org/10.1161/str.0000000000000211
Smith EE, Kent DM, Bulsara KR et al (2018) Accuracy of prediction instruments for diagnosing large vessel occlusion in individuals with suspected stroke: a systematic review for the 2018 guidelines for the early management of patients with acute ischemic stroke. Stroke 49:E111–E122. https://doi.org/10.1161/str.0000000000000160
Ozdemir O, Leung A, Bussiere M et al (2008) Hyperdense internal carotid artery sign—A CT sign of acute ischemia. Stroke 39:2011–2016. https://doi.org/10.1161/strokeaha.107.505230
Mair G, Boyd EV, Chappell FM et al (2015) Sensitivity and specificity of the hyperdense artery sign for arterial obstruction in acute ischemic stroke. Stroke 46:102–107. https://doi.org/10.1161/strokeaha.114.007036
Leary MC, Kidwell CS, Villablanca JP et al (2003) Validation of computed tomographic middle cerebral artery “Dot” sign—an angiographic correlation study. Stroke 34:2636–2640. https://doi.org/10.1161/01.Str.0000092123.00938.83
Koga M, Saku Y, Toyoda K et al (2003) Reappraisal of early CT signs to predict the arterial occlusion site in acute embolic stroke. J Neurol Neurosurg Psychiatry 74:649–653. https://doi.org/10.1136/jnnp.74.5.649
Kamalian S, Kemmling A, Borgie RC et al (2013) Admission insular infarction > 25% is the strongest predictor of large mismatch loss in proximal middle cerebral artery stroke. Stroke 44:3084–3089. https://doi.org/10.1161/strokeaha.113.002260
Kattah JC, Pula J, Newman-Toker DE (2011) Ocular lateropulsion as a central oculomotor sign in acute vestibular syndrome is not posturally dependent. Ann N Y Acad Sci 1233:249–255. https://doi.org/10.1111/j.1749-6632.2011.06160.x
Sato S, Koga M, Yamagami H et al (2012) Conjugate eye deviation in acute intracerebral hemorrhage stroke acute management with urgent risk-factor assessment and improvement-ICH (SAMURAI-ICH) study. Stroke 43:2898–2903. https://doi.org/10.1161/strokeaha.112.666750
Frusch KJM, Houben R, Schreuder FHBM et al (2016) Association between eye position on brain scan and hospital mortality in acute intracerebral hemorrhage. Eur J Neurol 23:831–835. https://doi.org/10.1111/ene.12951
Jiang NN, Wu W, Fong C et al (2020) Role of radiological eye deviation in imaging occult cases of acute large vessel occlusion. J Stroke Cerebrovasc Dis. https://doi.org/10.1016/j.jstrokecerebrovasdis.2020.104687
McVerry F, McCluskey G, Best E et al (2020) Radiological eye deviation and hyperdense vessel signs in large vessel occlusion of patients with acute ischemic stroke. J Stroke Cerebrovasc Dis. https://doi.org/10.1016/j.jstrokecerebrovasdis.2020.104744
Fink JN, Selim MH, Kumar S et al (2005) Insular cortex infarction in acute middle cerebral artery territory stroke—predictor of stroke severity and vascular lesion. Arch Neurol 62:1081–1085. https://doi.org/10.1001/archneur.62.7.1081
Min S-H, Kim J-T, Kang K-W et al (2020) Acute insular infarction: early outcomes of minor stroke with proximal artery occlusion. PLoS ONE. https://doi.org/10.1371/journal.pone.0229836
Funding
None.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflicts of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Ethical approval
The manuscript does not contain clinical studies or patient data.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Li, M., Liang, W., Yue, P. et al. Does radiological conjugate eye deviation sign play a role in acute stroke imaging? A meta-analysis. J Neurol 269, 1142–1153 (2022). https://doi.org/10.1007/s00415-021-10540-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-021-10540-7