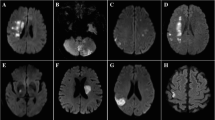
Abstract
Research suggests that the etiology of lacunar stroke is different from that of other stroke subtypes. This could imply an altered response to thrombolysis, but data concerning the efficacy of rt-PA in lacunar stroke is limited and inconsistent. From our prospectively collected stroke database, we identified patients with an MRI-confirmed purely lacunar stroke that were treated in our Stroke Unit between 2004 and 2011. We compared both the clinical course (NIHSS, deterioration, mRS at 3 months) and the MRI findings between patients who either received or did not receive rt-PA. In comparison to patients who obtained standard medical care (n = 468), acute lacunar stroke patients treated with rt-PA (n = 69) were more severely affected on admission (median NIHSS of 5 vs. 3; p < 0.001) and presented less frequently with a lacunar syndrome (74 vs. 88 %; p = 0.003). The clinical course was more favorable in patients treated with rt-PA (median NIHSS improvement of 3 vs. 1; p < 0.001), while functional deficit after 3 months was similar in both groups (median mRS of 2; p = 0.211). Overall complication rates did not differ significantly between the two groups, but while we did not detect symptomatic intracranial hemorrhage, hemorrhagic transformation was more frequent in thrombolyzed patients (11.6 vs. 1.9 %; p = 0.001). Patients with acute lacunar stroke benefited from thrombolysis without additional complications. Thus, patients with suspected acute lacunar stroke or lacunar syndrome should not be treated differently than other stroke populations.


Similar content being viewed by others
References
The NINDS t-PA Stroke Study Group (1997) Generalized efficacy of t-PA for acute stroke. Subgroup analysis of the NINDS t-PA Stroke Trial. Stroke 28:2119–2125. doi:10.1161/01.STR.28.11.2119
Adams HP Jr, Davis PH, Leira EC, Chang KC, Bendixen BH, Clarke WR, Woolson RF, Hansen MD (1999) Baseline NIH Stroke Scale score strongly predicts outcome after stroke: a report of the Trial of Org 10172 in Acute Stroke Treatment (TOAST). Neurology 53:126–131
Amarenco P, Bogousslavsky J, Caplan LR, Donnan GA, Hennerici MG (2009) New approach to stroke subtyping: the A-S-C-O (phenotypic) classification of stroke. Cerebrovasc Dis 27:502–508
Bailey EL, Smith C, Sudlow CL, Wardlaw JM (2012) Pathology of lacunar ischemic stroke in humans—a systematic review. Brain Pathol 22:583–591
Bamford J, Sandercock P, Jones L, Warlow C (1987) The natural history of lacunar infarction: the Oxfordshire Community Stroke Project. Stroke 18:545–551
Baumgartner RW, Sidler C, Mosso M, Georgiadis D (2003) Ischemic lacunar stroke in patients with and without potential mechanism other than small-artery disease. Stroke 34:653–659
Cocho D, Belvis R, Marti-Fabregas J, Bravo Y, Aleu A, Pagonabarraga J, Molina-Porcel L, Diaz-Manera J, San Roman L, Martinez-Lage M, Martinez A, Moreno M, Marti-Vilalta JL (2006) Does thrombolysis benefit patients with lacunar syndrome? Eur Neurol 55:70–73
Fazekas F, Chawluk JB, Alavi A, Hurtig HI, Zimmerman RA (1987) MR signal abnormalities at 1.5 T in Alzheimer’s dementia and normal aging. AJR Am J Roentgenol 149:351–356
Fluri F, Hatz F, Rutgers MP, Georgiadis D, Sekoranja L, Schwegler G, Sarikaya H, Weder B, Muller F, Luthy R, Arnold M, Reichhart M, Mattle HP, Tettenborn B, Nedeltchev K, Hungerbuhler HJ, Sztajzel R, Baumgartner RW, Michel P, Lyrer PA, Engelter ST (2010) Intravenous thrombolysis in patients with stroke attributable to small artery occlusion. Eur J Neurol 17:1054–1060
Fuentes B, Martinez-Sanchez P, de Lecinana MA, Egido J, Reig-Rosello G, Diaz-Otero F, Sanchez V, Simal P, Ximenez-Carrillo A, Garcia-Pastor A, Ruiz-Ares G, Garcia-Garcia A, Masjuan J, Vivancos-Mora J, Gil-Nunez A, Diez-Tejedor E (2012) Efficacy of intravenous thrombolysis according to stroke subtypes: the Madrid stroke network data. Eur J Neurol 19:1568–1574
Furlan A, Higashida R, Wechsler L, Gent M, Rowley H, Kase C, Pessin M, Ahuja A, Callahan F, Clark WM, Silver F, Rivera F (1999) Intra-arterial prourokinase for acute ischemic stroke. The PROACT II study: a randomized controlled trial. Prolyse in acute cerebral thromboembolism. JAMA 282:2003–2011
Hsia AW, Sachdev HS, Tomlinson J, Hamilton SA, Tong DC (2003) Efficacy of IV tissue plasminogen activator in acute stroke: does stroke subtype really matter? Neurology 61:71–75
Hwang YH, Seo JG, Lee HW, Park SP, Suh CK (2008) Early neurological deterioration following intravenous recombinant tissue plasminogen activator therapy in patients with acute lacunar stroke. Cerebrovasc Dis 26:355–359
Ingall TJ, O’Fallon WM, Asplund K, Goldfrank LR, Hertzberg VS, Louis TA, Christianson TJ (2004) Findings from the reanalysis of the NINDS tissue plasminogen activator for acute ischemic stroke treatment trial. Stroke 35:2418–2424
Kablau M, Alonso A, Hennerici MG, Fatar M (2012) Treatment with tPA predicts better outcome even if MCA occlusion persists. Int J Stroke 8(7):496–502
Konishi J, Yamada K, Kizu O, Ito H, Sugimura K, Yoshikawa K, Nakagawa M, Nishimura T (2005) MR tractography for the evaluation of functional recovery from lenticulostriate infarcts. Neurology 64:108–113
Larrue V, von Kummer RR, Muller A, Bluhmki E (2001) Risk factors for severe hemorrhagic transformation in ischemic stroke patients treated with recombinant tissue plasminogen activator: a secondary analysis of the European-Australasian Acute Stroke Study (ECASS II). Stroke 32:438–441
Lee SJ, Saver JL, Liebeskind DS, Ali L, Ovbiagele B, Kim D, Vespa P, Froehler M, Tenser M, Gadhia J, Starkman S (2010) Safety of intravenous fibrinolysis in imaging-confirmed single penetrator artery infarcts. Stroke 41:2587–2591
Lie C, Hirsch JG, Rossmanith C, Hennerici MG, Gass A (2004) Clinicotopographical correlation of corticospinal tract stroke: a color-coded diffusion tensor imaging study. Stroke 35:86–92
Makin SD, Turpin S, Dennis MS, Wardlaw JM (2013) Cognitive impairment after lacunar stroke: systematic review and meta-analysis of incidence, prevalence and comparison with other stroke subtypes. J Neurol Neurosurg Psychiatry 84:893–900
Moncayo J, Devuyst G, Van Melle G, Bogousslavsky J (2000) Coexisting causes of ischemic stroke. Arch Neurol 57:1139–1144
Nedeltchev K, Schwegler B, Haefeli T, Brekenfeld C, Gralla J, Fischer U, Arnold M, Remonda L, Schroth G, Mattle HP (2007) Outcome of stroke with mild or rapidly improving symptoms. Stroke 38:2531–2535
Norrving B (2003) Long-term prognosis after lacunar infarction. Lancet Neurol 2:238–245
Ohara T, Yamamoto Y, Tamura A, Ishii R, Murai T (2010) The infarct location predicts progressive motor deficits in patients with acute lacunar infarction in the lenticulostriate artery territory. J Neurol Sci 293:87–91
Potter G, Doubal F, Jackson C, Sudlow C, Dennis M, Wardlaw J (2010) Associations of clinical stroke misclassification (‘clinical-imaging dissociation’) in acute ischemic stroke. Cerebrovasc Dis 29:395–402
Samuelsson M, Soderfeldt B, Olsson GB (1996) Functional outcome in patients with lacunar infarction. Stroke 27:842–846
Shobha N, Fang J, Hill MD (2012) Do lacunar strokes benefit from thrombolysis?. Evidence from the Registry of the Canadian Stroke Network, Int J Stroke
Steinke W, Ley SC (2002) Lacunar stroke is the major cause of progressive motor deficits. Stroke 33:1510–1516
Takase K, Murai H, Tasaki R, Miyahara S, Kaneto S, Shibata M, Takashima N (2011) Initial MRI findings predict progressive lacunar infarction in the territory of the lenticulostriate artery. Eur Neurol 65:355–360
Thomalla G, Sobesky J, Kohrmann M, Fiebach JB, Fiehler J, Zaro Weber O, Kruetzelmann A, Kucinski T, Rosenkranz M, Rother J, Schellinger PD (2007) Two tales: hemorrhagic transformation but not parenchymal hemorrhage after thrombolysis is related to severity and duration of ischemia: MRI study of acute stroke patients treated with intravenous tissue plasminogen activator within 6 h. Stroke 38:313–318
Toni D, Iweins F, von Kummer R, Busse O, Bogousslavsky J, Falcou A, Lesaffre E, Lenzi GL (2000) Identification of lacunar infarcts before thrombolysis in the ECASS I study. Neurology 54:684–688
Wahlgren N, Ahmed N, Davalos A, Ford GA, Grond M, Hacke W, Hennerici MG, Kaste M, Kuelkens S, Larrue V, Lees KR, Roine RO, Soinne L, Toni D, Vanhooren G (2007) Thrombolysis with alteplase for acute ischaemic stroke in the Safe Implementation of Thrombolysis in Stroke-Monitoring Study (SITS-MOST): an observational study. Lancet 369:275–282
Wardlaw JM, Smith C, Dichgans M (2013) Mechanisms of sporadic cerebral small vessel disease: insights from neuroimaging. Lancet neurol 12:483–497
Weimar C, Ringelstein EB, Diener HC (2007) Monitoring stroke units: management, outcome, efficiency. Nervenarzt 78:957–966
Wolf ME, Sauer T, Kern R, Szabo K, Hennerici MG (2012) Multiple subcortical acute ischemic lesions reflect small vessel disease rather than cardiogenic embolism. J Neurol 259:1951–1957
Conflicts of interest
Dr. Griebe, Mrs. Fischer, Dr. Kablau, Dr. Eisele, Dr. Wolf, and Dr. Chatzikonstantinou report no disclosures. Dr. Gass has received honoraria for lecturing, travel expenses for attending meetings, and financial support for research from Bayer Schering, Biogen Idec, Merck Serono, Novartis, and TEVA Neurosciences. Dr. Hennerici is consultant to and has served on advisory boards during the previous 2 years for Servier, Bayer, Boehringer Ingelheim, and received grants from DFG, BMBF, EU and other organizations supporting clinical trials in the Department of Neurology at University Heidelberg in UMM Mannheim. He is Editor in Chief of the journal Cerebrovascular Diseases and board member of other international journals. Dr. Szabo received funding from the German Research Foundation (DFG). She is a member of the editorial board of the journal Cerebrovascular Diseases.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Griebe, M., Fischer, E., Kablau, M. et al. Thrombolysis in patients with lacunar stroke is safe: an observational study. J Neurol 261, 405–411 (2014). https://doi.org/10.1007/s00415-013-7212-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-013-7212-8