Abstract
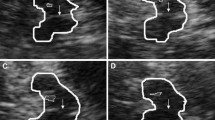
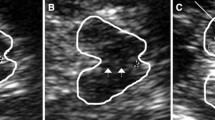
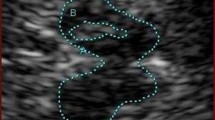
Substantia nigra (SN) hyperechogenicity—a sonographic vulnerability marker for Parkinson’s disease (PD)—has been recently described in patients with idiopathic REM sleep behaviour disorder (RBD). It is not known whether subjects with narcolepsy (who frequently have associated RBD) also show SN hyperechogenicity. The aim of this study was to (1) evaluate SN echogenicity in narcolepsy and (2) determine whether transcranial sonography (TCS) differs in narcoleptic subjects with and without RBD. A total of 16 patients with narcolepsy–cataplexy (7 had a concomitant, video-polysomnographically based diagnosis of RBD) were examined with TCS by two investigators blinded to the clinical data. The size of the SN echogenic area in both subgroups was within the range previously described for healthy subjects. The brainstem raphe, however, was reduced in five of seven narcoleptic subjects with RBD, whereas only two of nine narcoleptic subjects without RBD exhibited this TCS finding. We conclude that evaluation of SN echogenicity does not discriminate between both subgroups. The absence of SN hyperechogenicity in narcoleptic patients with RBD supports the hypothesis that SN hyperechogenicity in patients with presumed idiopathic RBD is an additional risk marker for subsequent evolvement of PD rather than an RBD-immanent finding. Reduced echogenicity of the brainstem raphe might indicate an involvement of the serotonergic system in narcoleptic subjects with RBD.
Similar content being viewed by others
References
Arnulf I, Konofal E, Merino-Andreu M, Houeto JL, Mesnage V, Welter ML, Lacomblez L, Golmard JL, Derenne JP, Agid Y (2002) Parkinson’s disease and sleepiness: an integral part of PD. Neurology 58:1019–1024
Behnke S, Berg D, Becker G (2003) Does ultrasound disclose a vulnerability factor for Parkinson’s disease? J Neurol 250(Suppl 1):24–27
Körner Y, Meindorfner C, Möller JC, Stiasny-Kolster K, Haja D, Cassel W, Oertel WH, Krüger HP (2004) Predictors of sudden onset of sleep in Parkinson’s disease. Mov Disord 19:1298–1305
Maeda T, Nagata K, Kondo H, Kanbayashi T (2006) Parkinson’s disease comorbid with narcolepsy presenting low CSF hypocretin/orexin level. Sleep Med 7:662
Schenck CH, Bundlie SR, Ettinger MG, Mahowald MW (1986) Chronic behavioral disorders of human REM sleep: a new category of parasomnia. Sleep 9:293–308
Stiasny-Kolster K, Clever SC, Möller JC, Oertel WH, Mayer G (2007) Olfactory dysfunction in patients with narcolepsy with and without REM sleep behaviour disorder. Brain 130:442–449
Thannickal TC, Lai YY, Siegel JM (2007) Hypocretin (orexin) cell loss in Parkinson’s disease. Brain 130:1586–1595
Unger MM, Möller JC, Stiasny-Kolster K, Mankel K, Berg D, Walter U, Hoeffken H, Mayer G, Oertel WH (2008) Assessment of idiopathic rapid-eye-movement sleep behaviour disorder by transcranial sonography, olfactory function test and FP-CIT-SPECT—the diverse pattern in this subgroup of subjects at risk for parkinsonian syndromes. Mov Disord 23:596–599
Walter U, Dressler D, Wolters A, Wittstock M, Benecke R (2006) Overactive bladder in Parkinson’s disease: alteration of brainstem raphe detected by transcranial sonography. Eur J Neurol 13:1291–1297
Walter U, Behnke S, Eyding J, Niehaus L, Postert T, Seidel G, Berg D (2007) Transcranial brain parenchyma sonography in movement disorders: state of the art. Ultrasound Med Biol 33:15–25
Walter U, Dressler D, Wolters A, Wittstock M, Benecke R (2007) Transcranial brain sonography findings in clinical subgroups of idiopathic Parkinson’s disease. Mov Disord 22:48–54
Acknowledgments
This work was supported by grants from the BMBF (funding code: 01GI0401) and the Willy und Monika Pitzer Stiftung.
Conflict of interest statement
The authors declare that there is no conflict of interest regarding this work.
Author information
Authors and Affiliations
Corresponding author
Additional information
W.H. Oertel and G. Mayer contributed equally to this work.
Rights and permissions
About this article
Cite this article
Unger, M.M., Möller, J.C., Ohletz, T. et al. Transcranial midbrain sonography in narcoleptic subjects with and without concomitant REM sleep behaviour disorder. J Neurol 256, 874–877 (2009). https://doi.org/10.1007/s00415-009-5032-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-009-5032-7