Abstract
Background
White matter hyperintensities (WMH) have an effect on cognition and are increased in severity among individuals with amnestic mild cognitive impairment (aMCI). The influence of WMH on progression of aMCI to Alzheimer’s disease (AD) is less clear.
Methods
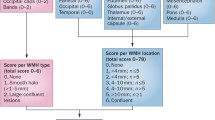
Data were drawn from a three-year prospective, double blind, placebo controlled clinical trial that examined the effect of donepezil or vitamin E on progression from aMCI to AD. WMH from multiple brain regions were scored on MR images obtained at entry into the trial from a subset of 152 study participants using a standardized visual rating scale. Cox proportional hazards models adjusting for age, education and treatment arm were used to investigate the role of WMH on time to progression.
Results
55 of the 152 (36.2 %) aMCI subjects progressed to AD. Only periventricular hyperintensities (PVH) were related to an increased risk of AD within three years (HR = 1.59, 95 % CI = 1.24 – 2.05, p-value < 0.001). Correcting for medial temporal lobe atrophy or the presence of lacunes did not change statistical significance.
Conclusion
PVH are associated with an increased risk of progression from aMCI to AD. This suggests that PVH, an MRI finding thought to represent cerebrovascular damage, contributes to AD onset in vulnerable individuals independent of Alzheimer pathology.
Similar content being viewed by others
References
Morris JC, Price AL (2001) Pathologic correlates of nondemented aging, mild cognitive impairment, and early-stage Alzheimer’s disease. J Mol Neurosci 17:101–118
Petersen RC, Smith GE, Waring SC, Ivnik RJ, Tangalos EG, Kokmen E (1999) Mild cognitive impairment: clinical characterization and outcome. Arch Neurol 56:303–308
Price JL, Morris JC (1999) Tangles and plaques in nondemented aging and «preclinical» Alzheimer’s disease. Ann Neurol 45:358–368
Petersen RC (2004) Mild cognitive impairment as a diagnostic entity. J Intern Med 256:183–194
Bennett DA, Wilson RS, Schneider JA, et al. (2002) Natural history of mild cognitive impairment in older persons. Neurology 59:198–205
Ganguli M, Dodge HH, Shen C, DeKosky ST (2004) Mild cognitive impairment, amnestic type: an epidemiologic study. Neurology 63:115–121
Morris JC, Storandt M, Miller JP, et al. (2001) Mild cognitive impairment represents early-stage Alzheimer disease. Arch Neurol 58:397–405
Petersen RC (2000) Mild cognitive impairment: transition between aging and Alzheimer’s disease. Neurologia 15:93–101
DeCarli C, Miller BL, Swan GE, Reed T, Wolf PA, Carmelli D (2001) Cerebrovascular and brain morphologic correlates of mild cognitive impairment in the National Heart, Lung, and Blood Institute Twin Study. Arch Neurol 58:643–647
Lopez OL, Jagust WJ, Dulberg C, et al. (2003) Risk factors for mild cognitive impairment in the Cardiovascular Health Study Cognition Study: part 2. Arch Neurol 60:1394–1399
Riley KP, Snowdon DA, Markesbery WR (2002) Alzheimer’s neurofibrillary pathology and the spectrum of cognitive function: findings from the Nun Study. Ann Neurol 51:567–577
Englund E (2002) Neuropathology of white matter lesions in vascular cognitive impairment. Cerebrovasc Dis 13(Suppl 2):11–15
Nordahl CW, Ranganath C, Yonelinas AP, DeCarli C, Reed BR, Jagust WJ (2005) Different mechanisms of episodic memory failure in mild cognitive impairment. Neuropsychologia 43:1688–1697
DeCarli C, Murphy DG, Tranh M, et al. (1995) The effect of white matter hyperintensity volume on brain structure, cognitive performance, and cerebral metabolism of glucose in 51 healthy adults. Neurology 45:2077–2084
Tullberg M, Fletcher E, DeCarli C, et al. (2004) White matter lesions impair frontal lobe function regardless of their location. Neurology 63:246–253
DeCarli C (2003) The role of cerebrovascular disease in dementia. Neurologist 9:123–136
DeCarli C, Mungas D, Harvey D, et al. (2004) Memory impairment, but not cerebrovascular disease, predicts progression of MCI to dementia. Neurology 63:220–227
Wolf H, Ecke GM, Bettin S, Dietrich J, Gertz HJ (2000) Do white matter changes contribute to the subsequent development of dementia in patients with mild cognitive impairment? A longitudinal study. Int J Geriatr Psychiatry 15:803–812
Petersen RC, Thomas RG, Grundman M, et al. (2005) Vitamin E and donepezil for the treatment of mild cognitive impairment. N Engl J Med 352:2379–2388
DeCarli C, Frisoni GB, Clark CM, et al. (2007) Qualitative estimates of medial temporal atrophy as a predictor of progression from mild cognitive impairment to dementia. Arch Neurol 64:108–115
Grundman M, Petersen RC, Ferris SH, et al. (2004) Mild cognitive impairment can be distinguished from Alzheimer disease and normal aging for clinical trials. Arch Neurol 61:59–66
Wechsler D (1987) WMS-R Wechsler Memory Scale – Revised Manual. New York, Harcourt Brace Jovanovich Inc
Hughes CP, Berg L, Danziger WL, Coben LA, Martin RL (1982) A new clinical scale for the staging of dementia. Br J Psychiatry 140:566–572
McKhann G, Drachman D, Folstein M, Katzman R, Price D, Stadlan EM (1984) Clinical diagnosis of Alzheimer’s disease: report of the NINCDS-ADRDA Work Group under the auspices of Department of Health and Human Services Task Force on Alzheimer’s Disease. Neurology 34:939–944
Grundman M, Sencakova D, Jack CR Jr, et al. (2002) Brain MRI hippocampal volume and prediction of clinical status in a mild cognitive impairment trial. J Mol Neurosci 19:23–27
Grundman M, Jack CR Jr, Petersen RC, et al. (2003) Hippocampal volume is associated with memory but not monmemory cognitive performance in patients with mild cognitive impairment. J Mol Neurosci 20:241–248
Scheltens P, Barkhof F, Leys D, et al. (1993) A semiquantative rating scale for the assessment of signal hyperintensities on magnetic resonance imaging. J Neurol Sci 114:7–12
Scheltens P, Leys D, Barkhof F, et al. (1992) Atrophy of medial temporal lobes on MRI in «probable» Alzheimer’s disease and normal ageing: diagnostic value and neuropsychological correlates. J Neurol Neurosurg Psychiatry 55:967–972
Burns JM, Church JA, Johnson DK, et al. (2005) White matter lesions are prevalent but differentially related with cognition in aging and early Alzheimer disease. Arch Neurol 62:1870–1876
de Groot JC, de Leeuw FE, Oudkerk M, et al. (2002) Periventricular cerebral white matter lesions predict rate of cognitive decline. Ann Neurol 52:335–341
Prins ND, van Dijk EJ, den Heijer T, et al. (2004) Cerebral white matter lesions and the risk of dementia. Arch Neurol 61:1531–1534
de la Torre JC (2002) Vascular basis of Alzheimer’s pathogenesis. Ann N Y Acad Sci 977:196–215
Launer LJ (2002) Demonstrating the case that AD is a vascular disease: epidemiologic evidence. Ageing Res Rev 1:61–77
Pansari K, Gupta A, Thomas P (2002) Alzheimer’s disease and vascular factors: facts and theories. Int J Clin Pract 56:197–203
van der Flier WM, Middelkoop HA, Weverling-Rijnsburger AW, et al. (2004) Interaction of medial temporal lobe atrophy and white matter hyperintensities in AD. Neurology 62:1862–1864
Schneider JA, Wilson RS, Bienias JL, Evans DA, Bennett DA (2004) Cerebral infarctions and the likelihood of dementia from Alzheimer disease pathology. Neurology 62:1148–1155
Snowdon DA, Greiner LH, Mortimer JA, Riley KP, Greiner PA, Markesbery WR (1997) Brain infarction and the clinical expression of Alzheimer disease. The Nun Study. JAMA 277:813–817
Vermeer SE, Prins ND, den Heijer T, Hofman A, Koudstaal PJ, Breteler MM (2003) Silent brain infarcts and the risk of dementia and cognitive decline. N Engl J Med 348:1215–1222
Cummings JL, Benson DF (1988) Psychological dysfunction accompanying subcortical dementias. Annu Rev Med 39:53–61
American Psychiatry Association (1994) Diagnostic and statistical manual of mental disorders, 4th ed. Washington, American Psychiatry Association
Barkhof F, Scheltens P (2006) Is the whole brain periventricular? J Neurol Neurosurg Psychiatry 77:143–144
DeCarli C, Fletcher E, Ramey V, Harvey D, Jagust WJ (2005) Anatomical mapping of white matter hyperintensities (WMH): exploring the relationships between periventricular WMH, deep WMH, and total WMH burden. Stroke 36:50–55
Desmond DW (2004) The neuropsychology of vascular cognitive impairment: is there a specific cognitive deficit? J Neurol Sci 226:3–7
Selden NR, Gitelman DR, Salamon- Murayama N, Parrish TB, Mesulam MM (1998) Trajectories of cholinergic pathways within the cerebral hemispheres of the human brain. Brain 121(Pt 12):2249–2257
Fazekas F, Kleinert R, Offenbacher H, et al. (1993) Pathologic correlates of incidental MRI white matter signal hyperintensities. Neurology 43:1683–1689
Olichney JM, Hansen LA, Lee JH, Hofstetter CR, Katzman R, Thal LJ (2000) Relationship between severe amyloid angiopathy, apolipoprotein E genotype, and vascular lesions in Alzheimer’s disease. Ann N Y Acad Sci 903:138–143
DeCarli C, Reed T, Miller BL, Wolf PA, Swan GE, Carmelli D (1999) Impact of apolipoprotein E epsilon4 and vascular disease on brain morphology in men from the NHLBI twin study. Stroke 30:1548–1553
van Straaten EC, Fazekas F, Rostrup E, et al. (2006) Impact of white matter hyperintensities scoring method on correlations with clinical data: the LADIS study. Stroke 37:836–840
Visser PJ, Verhey FR, Hofman PA, Scheltens P, Jolles J (2002) Medial temporal lobe atrophy predicts Alzheimer’s disease in patients with minor cognitive impairment. J Neurol Neurosurg Psychiatry 72:491–497
Salloway S, Ferris S, Kluger A, et al. (2004) Efficacy of donepezil in mild cognitive impairment: a randomized placebo-controlled trial. Neurology 63:651–657
Thal LJ, Ferris SH, Kirby L, et al. (2005) A randomized, double-blind, study of rofecoxib in patients with mild cognitive impairment. Neuropsychopharmacology 30:1204–1215
Ancelin ML, Christen Y, Ritchie K (2007) Is antioxidant therapy a viable alternative for mild cognitive impairment? Examination of the evidence. Dement Geriatr Cogn Disord 24:1–19
Hull M, Berger M, Heneka M (2006) Disease-modifying therapies in Alzheimer’s disease: how far have we come? Drugs 66:2075–2093
Burns A, O’Brien J, Auriacombe S, et al. (2006) Clinical practice with antidementia drugs: a consensus statement from British Association for Psychopharmacology. J Psychopharmacol 20:732–755
Dufouil C, Chalmers J, Coskun O, et al. (2005) Effects of blood pressure lowering on cerebral white matter hyperintensities in patients with stroke: the PROGRESS (Perindopril Protection Against Recurrent Stroke Study) Magnetic Resonance Imaging Substudy. Circulation 112:1644–1650
Hanon O, Forette F (2004) Prevention of dementia: lessons from SYST-EUR and PROGRESS. J Neurol Sci 226:71–74
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
*Members of the Alzheimer’s Disease Cooperative Study who participated in this MRI study are presented in the appendix at the end of the paper.
Rights and permissions
About this article
Cite this article
van Straaten, E.C.W., Harvey, D., Scheltens, P. et al. Periventricular white matter hyperintensities increase the likelihood of progression from amnestic mild cognitive impairment to dementia. J Neurol 255, 1302–1308 (2008). https://doi.org/10.1007/s00415-008-0874-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-008-0874-y