Abstract
Purpose
While the need for preventive strategies to reduce the incidence of aspiration pneumonia has been indicated, it is also important to investigate effective training methods to improve cough function, which is associated with the development of aspiration pneumonia. This study aimed to investigate whether a 4-week home-based unsupervised cough training (CT) or inspiratory muscle training (IMT) program was effective in improving cough strength in older adults.
Methods
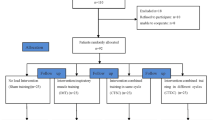
Fifty-three ambulatory older adults without airflow limitations were randomly assigned to one of three groups: a CT group (n = 18), an IMT group (n = 18), or a control group (n = 17). The CT and IMT groups performed home-based unsupervised training with a device for 4 weeks. Cough strength (cough peak flow), forced vital capacity, and respiratory muscle strength were assessed at the 4-week and 16-week follow-up. Intention-to-treat analyses were performed to investigate differences between the three groups using linear mixed models.
Results
At the 4-week follow-up, the CT group showed significant increases in cough peak flow and forced vital capacity compared with the control group, while the IMT group showed significant increases in inspiratory muscle strength compared with the cough training and control groups. At the 16-week follow-up, the CT group showed a significant increase in cough peak flow compared with the IMT group.
Conclusion
These preliminary results suggest that a 4-week home-based CT program may have short-term effectiveness in improving cough peak flow in ambulatory older adults.
Trial registration: This trial was registered on UMIN-CTR on 01/05/2018 (UMIN000031656).

Similar content being viewed by others
Data Availability
All data generated or analyzed during this study are included in this published article and its supplementary information file.
References
Ministry of Health, Labour and Welfare (2021) Summary of vital statistics: trends in leading causes of death. https://www.mhlwgojp/english/database/db-hw/populate/dl/E03pdf Accessed 19 Nov 2021
Teramoto S, Fukuchi Y, Sasaki H, Sato K, Sekizawa K, Matsuse T, Japanese Study Group on Aspiration Pulmonary Disease (2008) High incidence of aspiration pneumonia in community- and hospital-acquired pneumonia in hospitalized patients: a multicenter, prospective study in Japan. J Am Geriatr Soc 56:577–579. https://doi.org/10.1111/j.1532-5415.2008.01597.x
Ebihara S, Sekiya H, Miyagi M, Ebihara T, Okazaki T (2016) Dysphagia, dystussia, and aspiration pneumonia in elderly people. J Thorac Dis 8:632–639. https://doi.org/10.21037/jtd.2016.02.60
Lee KK, Davenport PW, Smith JA et al (2021) Global physiology and pathophysiology of cough: part 1: cough phenomenology—CHEST Guideline and Expert Panel Report. Chest 159:282–293. https://doi.org/10.1016/j.chest.2020.08.2086
Bianchi C, Baiardi P, Khirani S, Cantarella G (2012) Cough peak flow as a predictor of pulmonary morbidity in patients with dysphagia. Am J Phys Med Rehabil 91:783–788. https://doi.org/10.1097/PHM.0b013e3182556701
Hegland KW, Davenport PW, Brandimore AE, Singletary FF, Troche MS (2016) Rehabilitation of swallowing and cough functions following stroke: an expiratory muscle strength training trial. Arch Phys Med Rehabil 97:1345–1351. https://doi.org/10.1016/j.apmr.2016.03.027
Pitts T, Bolser D, Rosenbek J, Troche M, Okun MS, Sapienza C (2009) Impact of expiratory muscle strength training on voluntary cough and swallow function in Parkinson disease. Chest 135:1301–1308. https://doi.org/10.1378/chest.08-1389
Reyes A, Castillo A, Castillo J, Cornejo I (2018) The effects of respiratory muscle training on peak cough flow in patients with Parkinson’s disease: a randomized controlled study. Clin Rehabil 32:1317–1327. https://doi.org/10.1177/0269215518774832
Kim J, Davenport P, Sapienza C (2009) Effect of expiratory muscle strength training on elderly cough function. Arch Gerontol Geriatr 48:361–366. https://doi.org/10.1016/j.archger.2008.03.006
Sasaki M (2007) The effect of expiratory muscle training on pulmonary function in normal subjects. J Phys Ther Sci 19:197–203. https://doi.org/10.1589/jpts.19.197
Kulnik ST, Birring SS, Moxham J, Rafferty GF, Kalra L (2015) Does respiratory muscle training improve cough flow in acute stroke? Pilot randomized controlled trial. Stroke 46:447–453. https://doi.org/10.1161/STROKEAHA.114.007110
Suzuki A, Kaneko H (2020) Effect of a voluntary cough intensity improvement program for community-dwelling elderly. Rigakuryoho Kagaku 35:597–601. https://doi.org/10.1589/rika.35.597
McCool FD (2006) Global physiology and pathophysiology of cough: ACCP evidence-based clinical practice guidelines. Chest 129:48S-53S. https://doi.org/10.1378/chest.129.1_suppl.48S
Kaneko H, Suzuki A, Horie J (2019) Relationship of cough strength to respiratory function, physical performance, and physical activity in older adults. Respir Care 64:828–834. https://doi.org/10.4187/respcare.06490
Mills DE, Johnson MA, Barnett YA, Smith WH, Sharpe GR (2015) The effects of inspiratory muscle training in older adults. Med Sci Sports Exerc 47:691–697. https://doi.org/10.1249/MSS.0000000000000474
Souza H, Rocha T, Pessoa M et al (2014) Effects of inspiratory muscle training in elderly women on respiratory muscle strength, diaphragm thickness and mobility. J Gerontol A Biol Sci Med Sci 69:1545–1553. https://doi.org/10.1093/gerona/glu182
Kaneko H, Suzuki A (2021) Association of cough peak flow with chest and abdominal wall mobility in older adults. Rigakuryoho Kagaku 36:197–201. https://doi.org/10.1589/rika.36.197
Kaneko H, Iketaka K, Urakawa A, Noguchi N (2017) Estimating diaphragm movement from abdominal wall movement measurements made by a simple device. Rigakuryoho Kagaku 32:359–363. https://doi.org/10.1589/rika.32.359
van der Maarel-Wierink CD, Vanobbergen JN, Bronkhorst EM, Schols JM, de Baat C (2013) Oral health care and aspiration pneumonia in frail older people: a systematic literature review. Gerodontology 30:3–9. https://doi.org/10.1111/j.1741-2358.2012.00637.x
Momosaki R, Yasunaga H, Matsui H, Horiguchi H, Fushimi K, Abo M (2015) Effect of early rehabilitation by physical therapists on in-hospital mortality after aspiration pneumonia in the elderly. Arch Phys Med Rehabil 96:205–209. https://doi.org/10.1016/j.apmr.2014.09.014
Wu CP, Chen YW, Wang MJ, Pinelis E (2017) National trends in admission for aspiration pneumonia in the United States, 2002–2012. Ann Am Thorac Soc 14:874–879. https://doi.org/10.1513/AnnalsATS.201611-867OC
Foley A, Hillier S, Barnard R (2011) Effectiveness of once-weekly gym-based exercise programmes for older adults post discharge from day rehabilitation: a randomised controlled trial. Br J Sports Med 45:978–986. https://doi.org/10.1136/bjsm.2009.063966
Laveneziana P, Albuquerque A, Aliverti A et al (2019) ERS statement on respiratory muscle testing at rest and during exercise. Eur Respir J. https://doi.org/10.1183/13993003.01214-2018
Miller MR, Hankinson J, Brusasco V et al (2005) Standardisation of spirometry. Eur Respir J 26:319–338. https://doi.org/10.1183/09031936.05.00034805
Kubota M, Kobayashi H, Quanjer PH, Omori H, Tatsumi K, Kanazawa M (2014) Reference values for spirometry, including vital capacity, in Japanese adults calculated with the LMS method and compared with previous values. Respir Investig 52:242–250. https://doi.org/10.1016/j.resinv.2014.03.003
American Thoracic Society/European Respiratory Society (2002) ATS/ERS Statement on respiratory muscle testing. Am J Respir Crit Care Med 166:518–624. https://doi.org/10.1164/rccm.166.4.518
Cohen J (1988) Statistical power analysis for the behavioral sciences, 2nd edn. Lawrence Erlbaum Associates, New Jersey
Folland JP, Williams AG (2007) The adaptations to strength training: morphological and neurological contributions to increased strength. Sports Med 37:145–168. https://doi.org/10.2165/00007256-200737020-00004
Ferraro FV, Gavin JP, Wainwright T, McConnell A (2019) The effects of 8 weeks of inspiratory muscle training on the balance of healthy older adults: a randomized, double-blind, placebo-controlled study. Physiol Rep 7:e14076. https://doi.org/10.14814/phy2.14076
Sancho J, Servera E, Diaz J, Marin J (2004) Comparison of peak cough flows measured by pneumotachograph and a portable peak flow meter. Am J Phys Med Rehabil 83:608–612. https://doi.org/10.1097/01.phm.0000133431.70907.a2
Acknowledgements
The authors thank all the participants who took part in this study and the staffs who helped with the data collection.
Funding
This work was supported by the Japan Society for the Promotion of Science (JSPS KAKENHI Grant number JP17K01792).
Author information
Authors and Affiliations
Contributions
Conceptualization: HK and JH; Methodology: HK and AS; Formal analysis and investigation: HK and AS; Writing—original draft preparation: HK; Writing—review and editing: HK, AS, and JH; Funding acquisition: HK; Resources: HK and AS; Supervision: HK and JH.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical Approval
Approval was granted by the Institutional Review Board of International University of Health and Welfare in April 2017 (17-Ifh-002).
Consent to Participate
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kaneko, H., Suzuki, A. & Horie, J. Effects of Cough Training and Inspiratory Muscle Training on Cough Strength in Older Adults: A Randomized Controlled Trial. Lung 200, 49–57 (2022). https://doi.org/10.1007/s00408-022-00509-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-022-00509-2