Abstract
Introduction
Lung cancer is the leading cause of cancer death in the USA, claiming more than 140,000 deaths annually. Delays in diagnosis and treatment can lead to missed opportunities for both curative and life prolonging therapies. This study aimed to evaluate duration of time to diagnosis and first treatment, as well as investigate reasons for delays in care.
Methods
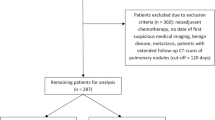
This retrospective study included all lung cancer cases diagnosed by Stony Brook’s Lung Cancer Evaluation Center (LCEC) between 2013 and 2019. Demographic, radiologic, pathologic and clinical variables were investigated, including cancer staging, histology, and medical and family histories. Evaluations included the determination of median time from initial encounter to diagnosis, median time from diagnosis to start of treatment and an exploration of the factors that influence possible causes for delays in care.
Results
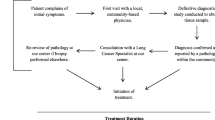
The LCEC’s comprehensive multidisciplinary lung nodule program yielded a median length of time from CT to PET of 11 days, PET to procedure of 13 days, procedure to treatment consult of 9 days, and from consult to treatment of 9 days. LCEC patients experienced an overall median of 44 days from initial presentation to first treatment compared to the national ideal of 62 days, thereby representing a 29% reduction in time from first CT to onset of treatment.
Conclusion
Delays in lung cancer diagnosis and treatment can negatively impact patient morbidity and mortality. This study suggests that a coordinated multidisciplinary lung cancer program may reduce delays in care, thereby improving patient outcomes.
Similar content being viewed by others
References
Jones GS, Baldwin DR (2018) Recent advances in the management of lung cancer. Clin Med 18:s41–s46
Ellis PM (2012) The importance of multidisciplinary team management of patients with non-small-cell lung cancer. Curr Onc 19:S7–S15
Bilfinger TV et al (2018) Survival Outcomes Among Lung Cancer Patients Treated Using a Multidisciplinary Team Approach. Clin Lung Canc 19(4):346–351
Siegel RL, Miller KD (2019) Cancer statistics. CA Cancer J Clin 69(1):7–34
Mackillop WJ (2007) Killing time: the consequences of delays in radiotherapy. Radiother Oncol 84(1):1–4
The Lung Clinical Expert Group (2017) National Optimal Clinical Pathway for suspected and confirmed lung cancer:Referral to treatment.
Koyi H, Hillerdal G, Branden E (2002) Patient’s and doctors’ delays in the diagnosis of chest tumors. Lung Canc 35(1):53–57
Bjerager M et al (2006) Delay in diagnosis of lung cancer in general practice. Br J Gen Pract 56(532):863–868
Barrett J, Hamilton W (2008) Pathways to the diagnosis of lung cancer in the UK: a cohort study. BMC Fam Pract 9:31. https://doi.org/10.1186/1471-2296-9-31
Hamann HA et al (2014) Stigma among patients with lung cancer: a patient-reported measurement model. Psycho-oncol 23(1):81–92
Dirkse D, a, (2014) Shame, guilt, and communication in lung cancer patients and their partners. Curr Oncol 21(5):e718–e722
Halpern MT, Holden DJ (2012) Disparities in timeliness of care for U.S. Medicare patients diagnosed with cancer. Curr Oncol 19(6):e404–e413
Ellis PM, Vandermeer R (2011) Delays in the diagnosis of lung cancer. J Thorac Dis 3(3):183–188
Salomaa ER et al (2005) Delays in the diagnosis and treatment of lung cancer. Chest 128(4):2282–2288
Stinchcombe TE et al (2007) Beliefs among physicians in the diagnostic and therapeutic approach to non-small cell lung cancer. J Thorac Oncol 2(9):819–826
Leiro-Fernández V et al (2019) Predicting delays in lung cancer diagnosis and staging. Thorac Canc 10(2):296–303
Vidaver RM et al (2016a) Typical Time to Treatment of Patients With Lung Cancer in a Multisite US-based study. J Oncol Pract 12(6):e643–e653
Yorio JT et al (2009) Lung cancer diagnostic and treatment intervals in the United States: a health care disparity? J Thorac Oncol 4(11):1322–1330
Sung MR, Leighl NB (2019) Improving lung cancer diagnosis: the evolving role of patients and care providers. J Thorac Dis 11:S422–S424
Blandin Knight S et al (2017) Progress and prospects of early detection in lung cancer. Open Biol. https://doi.org/10.1098/rsob.170070
Moody A, Muers M, Forman D (2004) Delays in managing lung cancer. Thorax 59(1):1–3
Olsson JK, Schultz EM, Gould MK (2009) Timeliness of care in patients with lung cancer: a systematic review. Thorax 64(9):749–756
Vidaver RM et al (2016b) Typical Time to Treatment of Patients With Lung Cancer in a Multisite US-based study. J Oncol Prac 12(6):e643–e653
Denton E, Conron M (2016) Improving outcomes in lung cancer: the value of the multidisciplinary health care team. J Multidisciplin Healthcare 9:137–144
Janssen A et al (2017) Interdisciplinary eHealth practice in cancer care: a review of the literature. Internat J Environment Res Publ Health 14(11):1289. https://doi.org/10.3390/ijerph14111289
Abdulrahman GO (2011) The effect of multidisciplinary team care on cancer management. The Pan Afric Med Journ 9(1):20. https://doi.org/10.4314/pamj.v9i1.71195
Gaga M et al (2013) An official American Thoracic Society/European Respiratory Society statement: the role of the pulmonologist in the diagnosis and management of lung cancer. Am J Respir Crit Care Med 188(4):503–507
Wright FC et al (2007) Multidisciplinary cancer conferences: a systematic review and development of practice standards. Eur J Cancer 43(6):1002–1010
Mambwere M, Kerr S, Hardavella G (2018) Holistic needs assessment (HNA) in lung cancer patients; bridging health and social care. Europ Respirat Journ. https://doi.org/10.1183/13993003.congress-2018.PA2073
Stokstad T et al (2017) Medical complexity and time to lung cancer treatment—a three-year retrospective chart review. BMC Health Serv Res 17:45. https://doi.org/10.1186/s12913-016-1952-y
Giuliani ME et al (2016) The prevalence and nature of supportive care needs in lung cancer patients. Curr Oncol 23(4):258–265
Moore S et al (2002) Nurse led follow up and conventional medical follow up in management of patients with lung cancer: randomised trial. BMJ. https://doi.org/10.1136/bmj.325.7373.1145
Chapple A, Ziebland S, McPherson A (2004) Stigma, shame, and blame experienced by patients with lung cancer: qualitative study. BMJ. https://doi.org/10.1136/bmj.38111.639734.7C
Carlson LE et al (2004) High levels of untreated distress and fatigue in cancer patients. Br J Canc 90(12):2297–2304
Vinod SK (2015) Decision making in lung cancer—how applicable are the guidelines? Clin Oncol 27(2):125–131
Nemesure B, Albano D, Bilfinger T (2020) Lung cancer recurrence and mortality outcomes over a 10-year period using a multidisciplinary team approach. Canc Epidem 68:101804. https://doi.org/10.1016/j.canep.2020.101804
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Albano, D., Bilfinger, T., Feraca, M. et al. A Multidisciplinary Lung Cancer Program: Does It Reduce Delay Between Diagnosis and Treatment?. Lung 198, 967–972 (2020). https://doi.org/10.1007/s00408-020-00404-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-020-00404-8