Abstract
Purpose
The literature is devoid of a comprehensive analysis of silicone airway stenting for benign central airway obstruction (BCAO). With the largest series in the literature to date, we aim to demonstrate the safety profile, pattern of re-intervention, and duration of silicone airway stents.
Methods
An institutional database was used to identify patients with BCAO who underwent rigid bronchoscopy with dilation and silicone stent placement between 2002 and 2015 at Rush University Medical Center.
Results
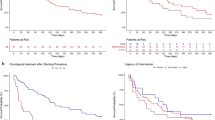
During the study period, 243 stents were utilized in 63 patients with BCAO. Pure tracheal stenosis was encountered in 71% (45/63), pure tracheomalacia in 11% (7/63), and a hybrid of both in 17% (11/63). Median freedom from re-intervention was 104 (IQR 167) days. Most common indications for re-intervention include mucus accumulation (60%; 131/220), migration (28%; 62/220), and intubation (8%; 18/220). The most common diameters of stent placed were 12 mm (94/220) and 14 mm (96/220). The most common lengths utilized were 30 mm (60/220) and 40 mm (77/220). Duration was not effected by stent size when placed for discrete stenosis. However, 14 mm stents outperformed 12 mm when tracheomalacia was present (157 vs. 37 days; p = 0.005). Patients with a hybrid stenosis fared better when longer stents were used (60 mm stents outlasted 40 mm stents 173 vs. 56 days; p = 0.05).
Conclusion
Rigid bronchoscopy with silicone airway stenting is a safe and effective option for the management of benign central airway obstruction. Our results highlight several strategies to improve stent duration.
Similar content being viewed by others
References
Puchalski J, Musani AI (2013) Tracheobronchial stenosis: causes and advances in management. Clin Chest Med 34:557–567
Cooper JD, Grillo HC (1969) The evolution of tracheal injury due to ventilatory assistance through cuffed tubes: a pathologic study. Ann Surg 169:334–348
Feist JH, Johnson TH, Wilson RJ (1975) Acquired tracheomalacia: etiology and differential diagnosis. Chest 68(3):340–345
Jokinen K, Palva T, Sutinen S, Nuutinen J (1977) Acquired tracheobronchomalacia. Ann Clin Res 9(2):52–57
Bhatt SP, Terry NL, Nath H et al (2016) Association between expiratory central airway collapse and respiratory outcomes among smokers. JAMA 315(5):498–505
Grillo HC, Donahue DM, Mathisen DJ et al (1995) Postintubation tracheal stenosis. Treatment and results. J Thorac Cardiovasc Surg 109:486–492
Auchincloss HG, Wright CD (2016) Complications after tracheal resection and reconstruction: prevention and treatment. J Thorac Dis 8(Suppl 2):S160–S167
Brichet A, Verkindre C, Dupont J et al (1999) Multidisciplinary approach to management of postintubation tracheal stenoses. Eur Respir J 13:888–893
Lagisetty KH, Gangadharan SP (2012) Tracheobronchoplasty for the treatment of tracheobronchomalacia. J Thorac Cardiovasc Surg 144(3):S58–S59
Dalar L, Karasulu L, Abul Y et al (2016) Bronchoscopic treatment in the management of benign tracheal stenosis: choices for simple and complex tracheal stenosis. Ann Thorac Surg 101:1310–1317
Dumon JF (1990) A dedicated tracheobronchial stent. Chest 97:328–332
Bacon JL, Patterson CM, Madden BP (2014) Indications and interventional options for non-resectable tracheal stenosis. J Thorac Dis 6(3):258–270
Ernst A, Majid A, Feller-Kopman D et al (2007) Airway stabilization with silicone stents for treating adult tracheobronchomalacia: a prospective observational study. Chest 132:609–616
Rahman NA, Fruchter O, Shitrit D et al (2010) Flexible bronchoscopic management of benign tracheal stenosis: long term follow up of 115 patients. J Cardiothorac Surg 17(5):2–6
Jeong BH, Um SW, Suh GY et al (2012) Results of interventional bronchoscopy in the management of postoperative tracheobronchial stenosis. J Thorac Cardiovasc Surg 144(1):217–222
Perotin JM, Jeanfaivre T, Deslee G et al (2011) Endoscopic management of idiopathic tracheal stenosis. Ann Thorac Surg 92(1):297–301
Breatnach E, Abbott GC, Fraser RG (1984) Dimensions of the normal human trachea. AJR Am J Roentgenol 142(5):903–906
Acknowledgements
This research is dedicated to the life and work of Dr. William H. Warren (1951–2016).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Karush, J.M., Seder, C.W., Raman, A. et al. Durability of Silicone Airway Stents in the Management of Benign Central Airway Obstruction. Lung 195, 601–606 (2017). https://doi.org/10.1007/s00408-017-0023-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-017-0023-4