Abstract
Purpose
Obstructive sleep apnoea (OSA) is a prevalent disorder, characterised by collapse of the upper airways during sleep. The impact of sleep-disordered breathing on pulmonary function indices is however currently not well described. The aim of the study was to evaluate diurnal change in lung function indices in a cohort of patients with OSA and relate pulmonary function changes to disease severity.
Methods
42 patients with OSA and 73 healthy control subjects participated in the study. Asthma and COPD were excluded in all volunteers following a clinical and spirometric assessment. Spirometry was then performed in all subjects in the evening and the morning following a polysomnography study.
Results
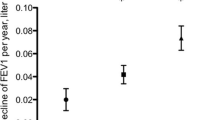
There was no difference in evening or morning FEV1 or FVC between patients and control subjects (p > 0.05). Neither FEV1 nor FVC changed in control subjects overnight (p > 0.05). In contrast, FEV1 significantly increased from evening (2.18/1.54–4.46/L) to morning measurement (2.26/1.42–4.63/L) in OSA without any change in FVC. The FEV1 increase in OSA was related to male gender, obesity and the lack of treatment with statins or β-blockers (all p < 0.05). A tendency for a direct correlation was apparent between overnight FEV1 change and RDI (p = 0.05, r = 0.30).
Conclusions
Diurnal variations in spirometric indices occur in patients with OSA and FEV1 appears to increase in subjects with OSA overnight. These changes occur in the absence of change in FVC and are directly related to the severity of OSA. These findings dictate a need to consider time of lung function measurement.


Similar content being viewed by others
References
Strollo PJ Jr, Rogers RM (1996) Obstructive sleep apnea. N Engl J Med 334(2):99–104. doi:10.1056/NEJM199601113340207
Abdeyrim A, Zhang Y, Li N, Zhao M, Wang Y, Yao X, Keyoumu Y, Yin T (2015) Impact of obstructive sleep apnea on lung volumes and mechanical properties of the respiratory system in overweight and obese individuals. BMC Pulm Med 15:76. doi:10.1186/s12890-015-0063-6
Onal E, Leech JA, Lopata M (1985) Relationship between pulmonary function and sleep-induced respiratory abnormalities. Chest 87(4):437–441
Abdeyrim A, Li N, Shao L, Heizhati M, Wang Y, Yao X, Abulikemu S, Zhang D, Chang G, Yin T, Li C, Meng J, Zhao M, Zhou L, Hong J, Zhang Y (2016) What can impulse oscillometry and pulmonary function testing tell us about obstructive sleep apnea: a case–control observational study? Sleep Breath 20(1):61–68. doi:10.1007/s11325-015-1185-z
Owens RL, Malhotra A, Eckert DJ, White DP, Jordan AS (2010) The influence of end-expiratory lung volume on measurements of pharyngeal collapsibility. J Appl Physiol 108(2):445–451. doi:10.1152/japplphysiol.00755.2009
Bednarek M, Plywaczewski R, Jonczak L, Zielinski J (2005) There is no relationship between chronic obstructive pulmonary disease and obstructive sleep apnea syndrome: a population study. Respiration 72(2):142–149. doi:10.1159/000084044
Teodorescu M, Barnet JH, Hagen EW, Palta M, Young TB, Peppard PE (2015) Association between asthma and risk of developing obstructive sleep apnea. JAMA 313(2):156–164. doi:10.1001/jama.2014.17822
Bikov A, Hull JH, Kunos L (2016) Exhaled breath analysis, a simple tool to study the pathophysiology of obstructive sleep apnoea. Sleep Med Rev 27:1–8. doi:10.1016/j.smrv.2015.07.005
Kunos L, Bikov A, Lazar Z, Korosi BZ, Benedek P, Losonczy G, Horvath I (2015) Evening and morning exhaled volatile compound patterns are different in obstructive sleep apnoea assessed with electronic nose. Sleep Breath 19(1):247–253. doi:10.1007/s11325-014-1003-z
Carpagnano GE, Kharitonov SA, Resta O, Foschino-Barbaro MP, Gramiccioni E, Barnes PJ (2003) 8-Isoprostane, a marker of oxidative stress, is increased in exhaled breath condensate of patients with obstructive sleep apnea after night and is reduced by continuous positive airway pressure therapy. Chest 124(4):1386–1392
Chua AP, Aboussouan LS, Minai OA, Paschke K, Laskowski D, Dweik RA (2013) Long-term continuous positive airway pressure therapy normalizes high exhaled nitric oxide levels in obstructive sleep apnea. J Clin Sleep Med 9(6):529–535. doi:10.5664/jcsm.2740
Olopade CO, Christon JA, Zakkar M, Hua C, Swedler WI, Scheff PA, Rubinstein I (1997) Exhaled pentane and nitric oxide levels in patients with obstructive sleep apnea. Chest 111(6):1500–1504
Narkiewicz K, van de Borne PJ, Montano N, Dyken ME, Phillips BG, Somers VK (1998) Contribution of tonic chemoreflex activation to sympathetic activity and blood pressure in patients with obstructive sleep apnea. Circulation 97(10):943–945
Marrone O, Riccobono L, Salvaggio A, Mirabella A, Bonanno A, Bonsignore MR (1993) Catecholamines and blood pressure in obstructive sleep apnea syndrome. Chest 103(3):722–727
Hakim F, Gozal D, Kheirandish-Gozal L (2012) Sympathetic and catecholaminergic alterations in sleep apnea with particular emphasis on children. Front Neurol 3:7. doi:10.3389/fneur.2012.00007
Cabezas GA, Graf PD, Nadel JA (1971) Sympathetic versus parasympathetic nervous regulation of airways in dogs. J Appl Physiol 31(5):651–655
Larsson K (1985) Studies of sympatho-adrenal reactivity and adrenoceptor function in bronchial asthma. Eur J Respir Dis Suppl 141:1–52
Canning BJ (2006) Reflex regulation of airway smooth muscle tone. J Appl Physiol 101(3):971–985. doi:10.1152/japplphysiol.00313.2006
Kushida CA, Littner MR, Morgenthaler T, Alessi CA, Bailey D, Coleman J Jr, Friedman L, Hirshkowitz M, Kapen S, Kramer M, Lee-Chiong T, Loube DL, Owens J, Pancer JP, Wise M (2005) Practice parameters for the indications for polysomnography and related procedures: an update for 2005. Sleep 28(4):499–521
Miller MR, Hankinson J, Brusasco V, Burgos F, Casaburi R, Coates A, Crapo R, Enright P, van der Grinten CP, Gustafsson P, Jensen R, Johnson DC, MacIntyre N, McKay R, Navajas D, Pedersen OF, Pellegrino R, Viegi G, Wanger J, Force AET (2005) Standardisation of spirometry. Eur Respir J 26(2):319–338. doi:10.1183/09031936.05.00034805
Faria AC, Lopes AJ, Jansen JM, Melo PL (2009) Evaluating the forced oscillation technique in the detection of early smoking-induced respiratory changes. Biomed Eng Online 8:22. doi:10.1186/1475-925X-8-22
Borsboom GJ, van Pelt W, van Houwelingen HC, van Vianen BG, Schouten JP, Quanjer PH (1999) Diurnal variation in lung function in subgroups from two Dutch populations: consequences for longitudinal analysis. Am J Respir Crit Care Med 159(4):1163–1171. doi:10.1164/ajrccm.159.4.9703106
Baruzzi A, Riva R, Cirignotta F, Zucconi M, Cappelli M, Lugaresi E (1991) Atrial natriuretic peptide and catecholamines in obstructive sleep apnea syndrome. Sleep 14(1):83–86
Horner RL, Brooks D, Kozar LF, Tse S, Phillipson EA (1995) Immediate effects of arousal from sleep on cardiac autonomic outflow in the absence of breathing in dogs. J Appl Physiol 79(1):151–162
Somers VK, Dyken ME, Mark AL, Abboud FM (1993) Sympathetic-nerve activity during sleep in normal subjects. N Engl J Med 328(5):303–307. doi:10.1056/nejm199302043280502
Spaak J, Egri ZJ, Kubo T, Yu E, Ando S, Kaneko Y, Usui K, Bradley TD, Floras JS (2005) Muscle sympathetic nerve activity during wakefulness in heart failure patients with and without sleep apnea. Hypertension 46(6):1327–1332. doi:10.1161/01.HYP.0000193497.45200.66
Barnes PJ, Fitzgerald GA, Dollery CT (1982) Circadian variation in adrenergic responses in asthmatic subjects. Clin Sci 62(4):349–354
Kapsimalis F, Kryger MH (2002) Gender and obstructive sleep apnea syndrome, part 2: mechanisms. Sleep 25(5):499–506
Shore SA, Fredberg JJ (2005) Obesity, smooth muscle, and airway hyperresponsiveness. J Allergy Clin Immunol 115(5):925–927. doi:10.1016/j.jaci.2005.01.064
Zeki AA, Franzi L, Last J, Kenyon NJ (2009) Simvastatin inhibits airway hyperreactivity: implications for the mevalonate pathway and beyond. Am J Respir Crit Care Med 180(8):731–740. doi:10.1164/rccm.200901-0018OC
Callaerts-Vegh Z, Evans KL, Dudekula N, Cuba D, Knoll BJ, Callaerts PF, Giles H, Shardonofsky FR, Bond RA (2004) Effects of acute and chronic administration of beta-adrenoceptor ligands on airway function in a murine model of asthma. Proc Natl Acad Sci USA 101(14):4948–4953. doi:10.1073/pnas.0400452101
Hetzel MR, Clark TJ (1980) Comparison of normal and asthmatic circadian rhythms in peak expiratory flow rate. Thorax 35(10):732–738
Joos GF, O’Connor B, Anderson SD, Chung F, Cockcroft DW, Dahlen B, DiMaria G, Foresi A, Hargreave FE, Holgate ST, Inman M, Lotvall J, Magnussen H, Polosa R, Postma DS, Riedler J (2003) Indirect airway challenges. Eur Respir J 21(6):1050–1068
Acknowledgments
The authors are grateful to Mrs. Monika Banlaky for her assistance in polysomnographic measurements and to Dr. James H Hull for English corrections. The authors are also grateful to Thor Medical and Elektro-Oxigén Inc. for providing spirometers and polysomnographic devices, respectively. Hungarian Respiratory Society provided financial support in the form of funding to David L Tarnoki (2014). This publication was supported by the Janos Bolyai Research Scholarship of the Hungarian Academy of Sciences to Andras Bikov.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Kunos, L., Lazar, Z., Martinovszky, F. et al. Overnight Changes in Lung Function of Obese Patients with Obstructive Sleep Apnoea. Lung 195, 127–133 (2017). https://doi.org/10.1007/s00408-016-9957-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-016-9957-1