Abstract
Purpose
Cluster analysis has been proposed to examine phenotypic heterogeneity in chronic obstructive pulmonary disease (COPD). The aim of this study was to use cluster analysis to define COPD phenotypes and validate them by assessing their relationship with mortality.
Methods
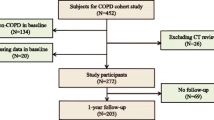
Male subjects with COPD were recruited to identify and validate COPD phenotypes. Seven variables were assessed for their relevance to COPD, age, FEV1 % predicted, BMI, history of severe exacerbations, mMRC, SpO2, and Charlson index. COPD groups were identified by cluster analysis and validated prospectively against mortality during a 4-year follow-up.
Results
Analysis of 332 COPD subjects identified five clusters from cluster A to cluster E. Assessment of the predictive validity of these clusters of COPD showed that cluster E patients had higher all cause mortality (HR 18.3, p < 0.0001), and respiratory cause mortality (HR 21.5, p < 0.0001) than those in the other four groups. Cluster E patients also had higher all cause mortality (HR 14.3, p = 0.0002) and respiratory cause mortality (HR 10.1, p = 0.0013) than patients in cluster D alone.
Conclusion
COPD patient with severe airflow limitation, many symptoms, and a history of frequent severe exacerbations was a novel and distinct clinical phenotype predicting mortality in men with COPD.


Similar content being viewed by others
Abbreviations
- AECOPD:
-
Acute exacerbation of COPD
- BMI:
-
Body mass index
- FEV1 :
-
Forced expiratory volume in one second
- mMRC:
-
Modified Medical Research Council
- PCA:
-
Principal component analysis
- SpO2 :
-
Arterial oxygen saturation
References
Garcia-Aymerich J, Gómez FP, Benet M et al (2011) Identification and prospective validation of clinically relevant chronic obstructive pulmonary disease (COPD) subtypes. Thorax 66:430–437
Burgel PR, Paillasseur JL, Caillaud D et al (2010) Clinical COPD phenotypes: a novel approach using principal component and cluster analyses. Eur Respir J 36:531–539
Burgel PR, Roche N, Paillasseur JL et al (2012) Clinical COPD phenotypes identified by cluster analyses: validation with mortality. Eur Respir J 40:495–512
Burgel PR, Paillasseur JL, Peene B et al (2012) Two distinct chronic obstructive pulmonary disease (COPD) phenotypes are associated with high risk of mortality. PLoS One 7(12):e51048
Weatherall M, Travers J, Shirtcliffe PM et al (2009) Distinct clinical phenotypes of airways disease defined by cluster analysis. Eur Respir J 34:812–818
Haldar P, Pavord ID, Shaw DE et al (2008) Cluster analysis and clinical asthma phenotypes. Am J Respir Crit Care Med 178:218–224
Cho MH, Washko GR, Hoffmann TJ et al (2010) Cluster analysis in severe emphysema subjects using phenotype and genotype data: an exploratory investigation. Respir Res 11:30
Han MK, Agusti A, Calverley PM et al (2010) Chronic obstructive pulmonary disease phenotypes: the future of COPD. Am J Respir Crit Care Med 182:598–604
Wardlaw AJ, Silverman M, Siva R et al (2005) Multi-dimensional phenotyping: towards a new taxonomy for airway disease. Clin Exp Allergy 35:1254–1262
Seemugal TAR, Donaldson GC, Paul EA et al (1998) Effect of exacerbation on quality of life in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med 157:1418–1422
Silverman EK (2007) Exacerbations in chronic obstructive pulmonary disease: do they contribute to disease progression? Proc Am Thorac Soc 4:586–590
Wedzicha JA, Seemungal TAR (2007) COPD exacerbations: defining their cause and prevention. Lancet 370:786–796
Hurst JR, Vestbo J, Anzueto A et al (2010) Susceptibility to exacerbation in chronic obstructive pulmonary disease. N Engl J Med 363:1128–1138
Soler-Cataluña JJ, Martinez-Garcia MA, Sánchez PR et al (2005) Severe acute exacerbations and mortality in patients with chronic obstructive pulmonary disease. Thorax 60:925–931
Garcia-Aymerich J, Farrero E, Félez MA et al (2003) Risk factors of readmission to hospital for a COPD exacerbation: a prospective study. Thorax 58:100–105
Celli BR, Jones P, Vestbo J et al (2008) The multidimensional BOD: association with mortality in the TORCH trial. Eur Respir J 32(Suppl. 52):42s
Puhan MA, Garcia-Aymerich J, Frey M et al (2009) Expansion of the prognostic assessment of patients with chronic obstructive pulmonary disease: the updated BODE index and the ADO index. Lancet 374:704–711
Sin DD, Anthonisen NR, Soriano JB, Agusti AG (2006) Mortality in COPD: role of comorbidities. Eur Respir J 28:1245–1257
Incalzi RA, Fuso L, DeRosa M et al (1997) Co-morbidity contributes to predict mortality of patients with chronic obstructive pulmonary disease. Eur Respir J 10:2794–2800
Nocturnal Oxygen Therapy Trial Group (1980) Continuous or nocturnal oxygen therapy in hypoxemic chronic obstructive pulmonary disease: a clinical trial. Ann Intern Med 93:391–398
Global Initiative for Chronic Obstructive Lung Disease (GOLD) (2006) Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease, 2006 updated. National Heart, Lung and Blood Institute/World Health Organization, Bethesda
Blonshine S, Mottram CD, Wanger J (2005) Pulmonary Function Laboratory Management and Procedure Manual, 2nd edn. American Thoracic Society, New York
Chen CZ, Ou CY, Wang WL et al (2012) Using post-bronchodilator FEV1 is better than pre-bronchodilator FEV1 in evaluation of COPD severity. COPD 9:276–280
Hnizdo E, Glindmeyer HW, Petsonk EL et al (2006) Case definitions for chronic obstructive pulmonary disease. COPD 3:95–100
Hardie JA, Buist AS, Vollmer WM et al (2002) Risk of over-diagnosis of COPD in asymptomatic elderly never-smokers. Eur Respir J 20:1117–1122
Curtis JR (2008) Palliative and end-of-life care for patients with severe COPD. Eur Respir J 32:796–803
Brown DW, Croft JB, Greenlund KJ et al (2008) Deaths from chronic obstructive pulmonary disease: united States, 2000–2005. MMWR Surveill Summ 57:1229–1232
Blanchette CM, Berry SR, Lane SJ (2011) Advances in chronic obstructive pulmonary disease among older adults. Curr Opin Pulm Med 17:84–89
Pedone C, Scarlata S, Sorino C et al (2010) Does mild COPD affect prognosis in the elderly? BMC Pulm Med 10:35
Almagro P, Calbo E, Ochoa de Echagüen A et al (2002) Mortality after hospitalization for COPD. Chest 121:1441–1448
Groenewegen KH, Scholas AMWJ, Wouters E (2003) Mortality and mortality-related factors after hospitalization for acute exacerbation of COPD. Chest 124:459–1467
Johannessen A, Skorge TD, Bottai M et al (2013) Mortality by level of emphysema and airway wall thickness. Am J Respir Crit Care Med 187:602–608
Martinez FJ, Foster G, Curtis JL et al (2006) Predictors of mortality in patients with emphysema and severe airflow obstruction. Am J Respir Crit Care Med 173:1326–1334
O’Donnell DE, Laveneziana P (2006) Physiology and consequences of lung hyperinflation in COPD. Eur Respir Rev 15(100):61–67
Thomas M, Decramer M, O’Donnell DE (2013) No room to breathe: the importance of lung hyperinflation in COPD. Prim Care Respir J 22(1):101–111
Casanova C, Cote C, de Torres JP et al (2005) Inspiratory-to-total lung capacity ratio predicts mortality in patients with chronic obstructive pulmonary disease. Am J Respir Crit Care Med 171:591–597
Regional COPD Working Group (2003) COPD prevalence in 12 Asia-Pacific countries and regions: projections based on the COPD prevalence estimation model. Respirology 8:192–198
Tan WC, Ng TP (2008) COPD in Asia: where East meets West. Chest 133:517–527
Han MK, Martinez CH, Curtis JL et al (2012) Gender differences in AECOPD in the NIH-sponsored Azithronycin in COPD trial. Am J Respire Crit Care Med 185:A4448
Acknowledgments
This study was supported by Grants from the National Science Council of Taiwan (NSC 95-2314-B-006-026 and NSC 99-2314-B-006-040.). All authors have no financial interests related to the material in the manuscript.
Conflict of interest
The authors declare that there is no conflict of interest in this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chen, CZ., Wang, LY., Ou, CY. et al. Using Cluster Analysis to Identify Phenotypes and Validation of Mortality in Men with COPD. Lung 192, 889–896 (2014). https://doi.org/10.1007/s00408-014-9646-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-014-9646-x