Abstract
Introduction
We performed a real-life retrospective analysis to assess the impact of long-acting bronchodilator therapy and associated exposure to inhaled corticosteroids (ICS) on all-cause and cardiovascular mortality in patients with chronic obstructive pulmonary disease (COPD).
Methods
We used record linkage data from patients with a diagnosis of COPD in Tayside, Scotland, between 2001 and 2010. All-cause and cardiovascular mortality were assessed using Cox proportional hazard regression.
Results
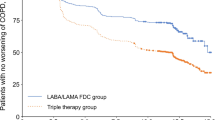
A total of 4,133 patients were included, mean FEV1 of 59.5 %, mean age of 68.9 years and mean follow-up of 4.6 years. There were 623 who were exposed to long-acting bronchodilators only and 3,510 to long-acting bronchodilators plus ICS. 1,372 patients (33 %) died during the study period. Compared with controls taking only long-acting bronchodilators either alone or in combination, all-cause mortality was reduced in patients taking long-acting muscarinic antagonist (LAMA) + ICS as dual therapy: adjusted hazard ratio 0.62 (95 % CI 0.45–0.85), but not by long-acting beta-agonist (LABA) + ICS: adjusted hazard ratio 1.02 (95 % CI 0.80–1.31). Cardiovascular mortality was not reduced by dual therapy with either LABA or LAMA and concomitant ICS exposure. All-cause and cardiovascular mortality were both reduced in patients taking triple therapy with LABA + LAMA + ICS: adjusted hazard ratio 0.51 (95 % CI 0.41–0.64) and 0.56 (95 % CI 0.35–0.90), respectively.
Conclusion
In patients exposed to ICS, concomitant use of LAMA alone as dual therapy or in combination with LABA as triple therapy were associated with reductions in all-cause mortality, while concomitant use of LABA without LAMA conferred no reduction. Moreover, only triple therapy was found to confer benefits on cardiovascular mortality.
Similar content being viewed by others
References
National Institute for Health and Clinical Excellence (2010) Chronic obstructive pulmonary disease. NICE guideline (update) consultation. National Institute for Health and Clinical Excellence, London
Calverley PMA, Anderson JA, Celli B, Ferguson GT, Jenkins C, Jones PW et al (2007) Salmeterol and fluticasone propionate and survival in chronic obstructive pulmonary disease. N Engl J Med 356:775–789
Tashkin DP, Celli B, Senn S, Burkhart D, Kesten S, Menjoge S et al (2008) A 4-year trial of tiotropium in chronic obstructive pulmonary disease. N Engl J Med 359:1543–1554
Salpeter SR, Ormiston TM, Salpeter EE (2004) Cardiovascular effects of beta-agonists in patients with asthma and COPD: a meta-analysis. Chest 125:2309–2321
Singh S, Loke YK, Enright P, Furberg CD (2013) Pro-arrhythmic and pro-ischaemic effects of inhaled anticholinergic medications. Thorax 68:114–116
Beasley R, Singh S, Loke YK, Enright P, Furberg CD (2012) Call for worldwide withdrawal of tiotropium Respimat mist inhaler. BMJ 345:e7390
Hohlfeld J, Sharma A, van Noord J et al (2014) Pharmacokinetics and pharmacodynamics of tiotropium solution and tiotropium powder in chronic obstructive pulmonary disease. J Clin Pharmacol 54(4):405–414. doi:10.1002/jcph.215
Wise RA, Anzueto A, Cotton D, Dahl R, Devins T, Disse B et al (2013) Tiotropium Respimat inhaler and the risk of death in COPD. N Engl J Med 369:1491–1501
Short PM, Williamson PA, Elder DH, Lipworth SI, Schembri S, Lipworth BJ (2012) The impact of tiotropium on mortality and exacerbations when added to inhaled corticosteroids and long-acting beta-agonist therapy in COPD. Chest 141:81–86
Janson C, Larsson K, Lisspers KH, Ställberg B, Stratelis G, Goike H et al (2013) Pneumonia and pneumonia related mortality in patients with COPD treated with fixed combinations of inhaled corticosteroid and long acting beta2 agonist: observational matched cohort study (PATHOS). BMJ 346:f3306
Lee TA, Pickard AS, Au DH, Bartle B, Weiss KB (2008) Risk for death associated with medications for recently diagnosed chronic obstructive pulmonary disease. Ann Intern Med 149:380–390
Gershon A, Croxford R, Calzavara A, To T, Stanbrook MB, Upshur R et al (2013) Cardiovascular safety of inhaled long-acting bronchodilators in individuals with chronic obstructive pulmonary disease long-acting bronchodilators in COPD long-acting bronchodilators in COPD. JAMA Intern Med 173:1175–1185
Lee TA, Wilke C, Joo M, Stroupe KT, Krishnan JA, Schumock GT et al (2009) Outcomes associated with tiotropium use in patients with chronic obstructive pulmonary disease. Arch Intern Med 169:1403–1410
Dong YH, Lin HH, Shau WY, Wu YC, Chang CH, Lai MS (2013) Comparative safety of inhaled medications in patients with chronic obstructive pulmonary disease: systematic review and mixed treatment comparison meta-analysis of randomised controlled trials. Thorax 68:48–56
Acknowledgments
This study was funded by Scottish Centre for Respiratory Research, University of Dundee departmental funds.
Conflict of interest
Following are the conflicts of interest/financial disclosures of the authors: Arvind Manoharan has received support from Teva to attend the 2013 European Respiratory Society Congress and Chiesi to attend the 2014 meeting. Philip Short has received support from GSK to attend the European Respiratory Society Congress 2013. William Anderson has received support Chiesi to attend the European Respiratory Society Congress 2013. Brian Lipworth is on the advisory board/has done consulting activity for Chiesi, Boehringer-Ingelheim, Teva & Cipla; he is on the speaker bureau for Teva and received support from Boehringer-Ingelheim to attend the British Thoracic Society/European Respiratory Society Congress 2013. The Scottish Centre for Respiratory Research, University of Dundee has received unrestricted grant support from Chiesi, Teva & Almirall.
Ethical Standard
This manuscript complies with the current laws of the United Kingdom.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Manoharan, A., Short, P.M., Anderson, W.J. et al. Impact of Long-Acting Bronchodilators and Exposure to Inhaled Corticosteroids on Mortality in COPD: A Real-Life Retrospective Cohort Study. Lung 192, 649–652 (2014). https://doi.org/10.1007/s00408-014-9611-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-014-9611-8