Abstract
Background
Whether antituberculosis (anti-TB) treatment in patients with chronic viral hepatitis affects the incidence and onset time of drug-induced hepatotoxicity (DIH) is still controversial. The aim of this retrospective study was to find out whether chronic viral hepatitis affects the incidence and onset time of DIH.
Methods
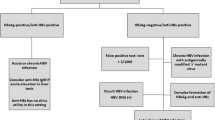
All patients diagnosed with active TB and being treated at a tertiary referral hospital between 2002 and 2009 were identified from medical records, from which 553 patients were enrolled in the study. The incidence and onset of DIH in patients with and without chronic viral hepatitis (controls) were compared.
Results
The incidence of DIH was similar in patients with and without chronic hepatitis (8 % [32/392] vs. 7 % [11/161], P > 0.05). The incidence of transient liver function impairment (TLI) was significantly lower in controls than in chronic hepatitis patients (2 % [9/392] vs. 12 % [20/161], P < 0.001. The mean onset times of DIH in the control, hepatitis B virus (HBV), and hepatitis C virus (HCV) groups were not significantly different (40, 39, and 67 days, respectively, all P > 0.05). The mean onset times of TLI in the control, HBV, and HCV groups were significantly different (23, 48, and 68 days, respectively, all P < 0.05).
Conclusions
Liver function impairment during anti-TB therapy in patients with chronic viral hepatitis was due to mostly TLI, with TLI occurring later than in controls. Chronic viral hepatitis had no significant effect on the incidence of DIH.
Similar content being viewed by others
References
Dye C, Scheele S, Dolin P, Pathania V, Raviglione MC (1999) Consensus statement. Global burden of tuberculosis: estimated incidence, prevalence, and mortality by country. WHO Global Surveillance and Monitoring Project. JAMA 282(7):677–686
Blumberg HM, Burman WJ, Chaisson RE, Daley CL, Etkind SC, Friedman LN, Fujiwara P, Grzemska M, Hopewell PC, Iseman MD, Jasmer RM, Koppaka V, Menzies RI, O’Brien RJ, Reves RR, Reichman LB, Simone PM, Starke JR, Vernon AA (2003) American Thoracic Society/Centers for Disease Control and Prevention/Infectious Diseases Society of America: treatment of tuberculosis. Am J Respir Crit Care Med 167(4):603–662. doi:10.1164/rccm.167.4.603
Liao CM, Hsieh NH, Huang TL, Cheng YH, Lin YJ, Chio CP, Chen SC, Ling MP (2012) Assessing trends and predictors of tuberculosis in Taiwan. BMC Public Health 12:29. doi:10.1186/1471-2458-12-29
Chen CJ, Yang HI (2011) Natural history of chronic hepatitis B REVEALed. J Gastroenterol Hepatol 26(4):628–638. doi:10.1111/j.1440-1746.2011.06695.x
Lee MH, Yang HI, Jen CL, Lu SN, Yeh SH, Liu CJ, You SL, Sun CA, Wang LY, Chen WJ, Chen CJ (2011) Community and personal risk factors for hepatitis C virus infection: a survey of 23,820 residents in Taiwan in 1991–1992. Gut 60(5):688–694. doi:10.1136/gut.2010.220889
Døssing M, Wilcke JT, Askgaard DS, Nybo B (1996) Liver injury during antituberculosis treatment: an 11-year study. Tuber Lung Dis 77(4):335–340
Pande JN, Singh SP, Khilnani GC, Khilnani S, Tandon RK (1996) Risk factors for hepatotoxicity from antituberculosis drugs: a case–control study. Thorax 51(2):132–136
Schaberg T, Rebhan K, Lode H (1996) Risk factors for side-effects of isoniazid, rifampin and pyrazinamide in patients hospitalized for pulmonary tuberculosis. Eur Respir J 9(10):2026–2030
Amarapurkar DN, Prabhudesai PP, Kalro RH, Desai HG (1993) Antituberculosis drug-induced hepatitis and HBsAg carriers. Tuber Lung Dis 74(3):215–216
Hwang SJ, Wu JC, Lee CN, Yen FS, Lu CL, Lin TP, Lee SD (1997) A prospective clinical study of isoniazid-rifampicin-pyrazinamide-induced liver injury in an area endemic for hepatitis B. J Gastroenterol Hepatol 12(1):87–91
Lee BH, Koh WJ, Choi MS, Suh GY, Chung MP, Kim H, Kwon OJ (2005) Inactive hepatitis B surface antigen carrier state and hepatotoxicity during antituberculosis chemotherapy. Chest 127(4):1304–1311. doi:10.1378/chest.127.4.1304
Wong WM, Wu PC, Yuen MF, Cheng CC, Yew WW, Wong PC, Tam CM, Leung CC, Lai CL (2000) Antituberculosis drug-related liver dysfunction in chronic hepatitis B infection. Hepatology 31(1):201–206. doi:10.1002/hep.510310129
Wu JC, Lee SD, Yeh PF, Chan CY, Wang YJ, Huang YS, Tsai YT, Lee PY, Ting LP, Lo KJ (1990) Isoniazid-rifampin-induced hepatitis in hepatitis B carriers. Gastroenterology 98(2):502–504
Ungo JR, Jones D, Ashkin D, Hollender ES, Bernstein D, Albanese AP, Pitchenik AE (1998) Antituberculosis drug-induced hepatotoxicity. The role of hepatitis C virus and the human immunodeficiency virus. Am J Respir Crit Care Med 157(6 Pt 1):1871–1876
Yee D, Valiquette C, Pelletier M, Parisien I, Rocher I, Menzies D (2003) Incidence of serious side effects from first-line antituberculosis drugs among patients treated for active tuberculosis. Am J Respir Crit Care Med 167(11):1472–1477. doi:10.1164/rccm.200206-626OC
Yew WW, Leung CC (2006) Antituberculosis drugs and hepatotoxicity. Respirology 11(6):699–707. doi:10.1111/j.1440-1843.2006.00941.x
Joint Tuberculosis Committee of the British Thoracic Society (1998) Chemotherapy and management of tuberculosis in the United Kingdom: recommendations 1998. Thorax 53(7):536–548
Turktas H, Unsal M, Tulek N, Oruc O (1994) Hepatotoxicity of antituberculosis therapy (rifampicin, isoniazid and pyrazinamide) or viral hepatitis. Tuber Lung Dis 75(1):58–60. doi:10.1016/0962-8479(94)90104-X
Tost JR, Vidal R, Cayla J, Diaz-Cabanela D, Jimenez A, Broquetas JM (2005) Severe hepatotoxicity due to anti-tuberculosis drugs in Spain. Int J Tuberc Lung Dis 9(5):534–540
Whittington RM (1991) Fatal hepatotoxicity of anti-tubercular chemotherapy. Lancet 338(8774):1083–1084
Devarbhavi H, Dierkhising R, Kremers WK (2010) Antituberculosis therapy drug-induced liver injury and acute liver failure. Hepatology 52(2):798–799; author reply 799–800. doi:10.1002/hep.23805
Devarbhavi H, Singh R, Patil M, Sheth K, Adarsh CK, Balaraju G (2013) Outcome and determinants of mortality in 269 patients with combination anti-tuberculosis drug-induced liver injury. J Gastroenterol Hepatol 28(1):161–167. doi:10.1111/j.1440-1746.2012.07279.x
Kumar R, Bhatia V, Khanal S, Sreenivas V, Gupta SD, Panda SK, Acharya SK (2010) Antituberculosis therapy-induced acute liver failure: magnitude, profile, prognosis, and predictors of outcome. Hepatology 51(5):1665–1674. doi:10.1002/hep.23534
Wang JY, Liu CH, Hu FC, Chang HC, Liu JL, Chen JM, Yu CJ, Lee LN, Kao JH, Yang PC (2011) Risk factors of hepatitis during anti-tuberculous treatment and implications of hepatitis virus load. J Infect 62(6):448–455. doi:10.1016/j.jinf.2011.04.005
Chien JY, Huang RM, Wang JY, Ruan SY, Chien YJ, Yu CJ, Yang PC (2010) Hepatitis C virus infection increases hepatitis risk during anti-tuberculosis treatment. Int J Tuberc Lung Dis 14(5):616–621
Girling DJ (1982) Adverse effects of antituberculosis drugs. Drugs 23(1–2):56–74
Sun HY, Chen YJ, Gau CS, Chang SC, Luh KT (2009) A prospective study of hepatitis during antituberculous treatment in Taiwanese patients and a review of the literature. J Formos Med Assoc 108(2):102–111
Liu Q, Garner P, Wang Y, Huang B, Smith H (2008) Drugs and herbs given to prevent hepatotoxicity of tuberculosis therapy: systematic review of ingredients and evaluation studies. BMC Public Health 8:365. doi:10.1186/1471-2458-8-365
Stickel F, Schuppan D (2007) Herbal medicine in the treatment of liver diseases. Dig Liver Dis 39(4):293–304. doi:10.1016/j.dld.2006.11.004
Lee SD, Wang YJ, Lu RH, Chan CY, Lo KJ, Moeckli R (1994) Seroprevalence of antibody to hepatitis E virus among Chinese subjects in Taiwan. Hepatology 19(4):866–870
Conflict of interest
The authors have no conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Liu, YM., Cheng, YJ., Li, YL. et al. Antituberculosis Treatment and Hepatotoxicity in Patients with Chronic Viral Hepatitis. Lung 192, 205–210 (2014). https://doi.org/10.1007/s00408-013-9535-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-013-9535-8