Abstract
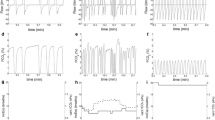
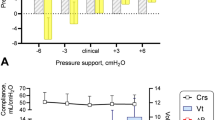
Blunted ventilatory responses to carbon dioxide indicate that respiratory control is impaired when ventilation is stimulated in individuals with tetraplegia; however, respiratory control during resting breathing has not been extensively studied in this population. Our objective was to evaluate respiratory control and sigh frequency during resting breathing in persons with tetraplegia. A prospective, two-group comparative study was performed. Breathing pattern was assessed in ten outpatients with chronic tetraplegia and eight age- and gender-matched able-bodied controls. Subjects were noninvasively monitored for 1 h, while seated and at rest. Tidal volume (VT) was calculated from the sum of the anteroposterior displacements of the rib cage and abdomen and the axial displacement of the chest wall. Inspiratory time (TI), VT, and the ratio of VT to inspiratory time (VT/TI) were calculated breath by breath. A sigh was defined as any breath greater than two or more times an individual’s mean VT. Minute ventilation, VT/TI, and sigh frequency were reduced in tetraplegia compared with controls (5.24 ± 1.15 vs. 7.16 ± 1.29 L/min, P < 0.005; 208 ± 45 vs. 284 ± 47 ml/s, P < 0.005; and 11 ± 7 vs. 42 ± 19 sighs/h, P < 0.0005, respectively). VT/TI was associated with sigh frequency in both groups (tetraplegia: R = 0.88; P = 0.001 and control: R = 0.70; P < 0.05). We concluded that reductions in minute ventilation, VT/TI, and sigh frequency suggest that respiratory drive is diminished during resting breathing in subjects with tetraplegia. These findings extend prior observations of disordered respiratory control during breathing stimulated by CO2 in tetraplegia to resting breathing.



Similar content being viewed by others
Abbreviations
- VT :
-
Tidal volume
- VE :
-
Minute ventilation
- TI :
-
Inspiratory time
- TE :
-
Expiratory time
- TTOT :
-
Total breath time
- RC:
-
Rib cage
- Ab:
-
Abdomen
- Xi:
-
Xiphi-umbilical distance
- P0.1 :
-
Mouth occlusion pressure at 100 ms
- CO2 :
-
Carbon dioxide
- SCI:
-
Spinal cord injury
- f:
-
Breathing frequency
- FVC:
-
Forced vital capacity
- FEV1 :
-
Forced expiratory volume in 1 s
- FEF25–75 :
-
Forced expiratory flow during 25–75% of the vital capacity
- PImax:
-
Maximal static inspiratory pressure
- PEmax:
-
Maximal static expiratory pressure
- REE:
-
Resting energy expenditure
References
Estenne M, DeTroyer A (1986) The effects of tetraplegia on chest wall statics. Am Rev Respir Dis 134:121–124
Kelling JS, DiMarco AF, Gottfried SB, Altose MD (1985) Respiratory responses to ventilatory loading following low cervical spinal cord injury. J Appl Physiol 59:1752–1756
McCool FD, Brown R, Mayewski RJ, Hyde RW (1988) Effects of posture on stimulated ventilation in quadriplegia. Am Rev Respir Dis 138:101–105
Manning HL, Brown R, Scharf SM, Leith DE, Weiss JW, Weinberger SE, Schwartzstein RM (1992) Ventilatory and P0.1 response to hypercapnia in quadriplegia. Respir Physiol 89:97–112
Lin KH, Wu HD, Chang CW, Wang TG, Wang YH (1998) Ventilatory and mouth occlusion pressure responses to hypercapnia in chronic tetraplegia. Arch Phys Med Rehabil 79:795–799
Milic-Emili J, Grunstein MM (1976) Drive and timing components of ventilation. Chest 70(1 Suppl):131–133
Loveridge BM, Dubo HI (1990) Breathing pattern in chronic quadriplegia. Arch Phys Med Rehabil 71:495–495
McKinley AC, Auchincloss HJ, Gilbert R, Nicholas JJ (1969) Pulmonary function, ventilatory control, and respiratory complications in quadriplegic subjects. Am Rev Respir Dis 100:526–532
Bodin P, Kreuter M, Bake B, Olsen MF (2003) Breathing patterns during breathing exercises in persons with tetraplegia. Spinal Cord 41:290–295
Askanazi J, Silverberg PA, Foster RJ, Hyman AI, Milic-Emili J, Kinney JM (1980) Effects of respiratory apparatus on breathing pattern. J Appl Physiol 48:577–580
Maxwell DL, Cover D, Hughes JMB (1985) Effect of respiratory apparatus on timing and depth of breathing in man. Respir Physiol 61:255–264
McCool FD, Wang J, Ebi KL (2002) Tidal volume and respiratory timing derived from a portable ventilation monitor. Chest 122:684–691
American Thoracic Society (1995) Standardization of spirometry, 1994 update. Am J Respir Crit Care Med 152:1107–1136
Ashba J, Garshick E, Tun CG, Lieberman SL, Polakoff DF, Blanchard JD, Brown R (1993) Spirometry—acceptability and reproducibility in spinal cord injured subjects. J Am Paraplegia Soc 16:197–203
Morris JF, Koski A, Johnson LC (1971) Spirometric standards for healthy nonsmoking adults. Am Rev Respir Dis 103:57–67
Baydur A (1991) Respiratory muscle strength and control of ventilation in patients with neuromuscular disease. Chest 99:330–338
Whitelaw WA, Derenne JP, Milic-Emili J (1975) Occlusion pressure as a measure of respiratory center output in conscious man. Respir Physiol 23:181–199
Lederer DH, Altose MD, Kelsen SG, Cherniack NS (1977) Comparison of occlusion pressure and ventilatory responses. Thorax 32:212–220
Hussain SN, Pardy RL, Dempsey JA (1985) Mechanical impedance as determinant of inspiratory neural drive during exercise in humans. J Appl Physiol 59:365–375
Tobin MJ (1992) Breathing pattern analysis. Intensive Care Med 18:193–201
Mollinger LA, Spurr GB, el Ghatit AZ, Barboriak JJ, Rooney CB, Davidoff DD, Bongard RD (1985) Daily energy expenditure and basal metabolic rates of patients with spinal cord injury. Arch Phys Med Rehabil 66:420–426
Liu MH, Spungen AM, Fink L, Losada M, Bauman WA (1996) Increased energy needs in patients with quadriplegia and pressure ulcers. Adv Wound Care 9:41–45
Manning H, McCool FD, Scharf SM, Brown R (1992) Oxygen cost of resistive-loaded breathing in quadriplegia. J Appl Physiol 73(3):825–831
Acknowledgments
This work was funded by the Department of Veterans Affairs Rehabilitation, Research and Development Service, Center of Excellence for the Medical Consequences of Spinal Cord Injury # B4162C and the United Spinal Association (formerly Eastern Paralyzed Veterans Association).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Spungen, A.M., Bauman, W.A., Lesser, M. et al. Breathing Pattern and Ventilatory Control in Chronic Tetraplegia. Lung 187, 375–381 (2009). https://doi.org/10.1007/s00408-009-9186-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00408-009-9186-y