Abstract
Objectives
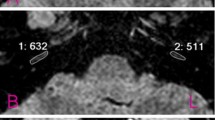
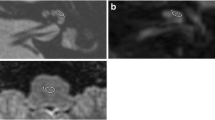
This study aimed to explore the diagnostic sensitivity of 3D heavily weighted T2-weighted MRI (T2MRI) and high-resolution computed tomography (HRCT) in patients with cochlear fibrosis associated with Streptococcus suis (S. suis) meningitis and the practicality of Cochlear implantation (CI) treatments.
Methods
Between January 2020 and December 2022, we enrolled four patients with rare cochlear S. suis meningitis with associated hearing loss despite aggressive or non-aggressive follow-up antibiotic treatment. Clinical imaging data, surgical performances and post-surgical-electrode impedance were evaluated.
Results
Combined with HRCT and T2MRI, the cochlea had varying degrees of fibrosis and ossification in different cases. However, the electrodes were successfully and wholly inserted after intraoperative removal of the ossified and fibrotic foci. Post-surgical electrode impedance values of MP1 + 2 mode were normal in all 4 cases at initial activation.
Conclusion
In patients with S. suis meningitis and associated cochlear fibrosis, T2MRI examination of the inner ear was more sensitive than HRCT. This research highlights the feasibility of CI treatment in S. suis meningitis patients with severe cochlear fibrosis.



Similar content being viewed by others
Data availability
The datasets analyzed during the current study are available from the corresponding author on reasonable request.
References
Huong VT, Ha N, Huy NT, Horby P, Nghia HD, Thiem VD et al (2014) Epidemiology, clinical manifestations, and outcomes of Streptococcus suis infection in humans. Emerg Infect Dis 20:1105–1114. https://doi.org/10.3201/eid2007.131594
Huong V, Long HB, Kinh NV, Ngan T, Dung V, Nadjm B et al (2018) Long-term outcomes of patients with Streptococcus suis infection in Viet Nam: a case-control study. J Infect 76:159–167. https://doi.org/10.1016/j.jinf.2017.09.019
Hlebowicz M, Jakubowski P, Smiatacz T (2019) Streptococcus suis meningitis: epidemiology, clinical presentation and treatment. Vector Borne Zoonotic Dis 19:557–562. https://doi.org/10.1089/vbz.2018.2399
Kerdsin A, Akeda Y, Takeuchi D, Dejsirilert S, Gottschalk M, Oishi K (2018) Genotypic diversity of Streptococcus suis strains isolated from humans in Thailand. Eur J Clin Microbiol Infect Dis 37:917–925. https://doi.org/10.1007/s10096-018-3208-8
Trakimas DR, Knoll RM, Castillo-Bustamante M, Kozin ED, Remenschneider AK (2021) Otopathologic analysis of patterns of postmeningitis labyrinthitis ossificans. Otolaryngol Head Neck Surg 164:175–181. https://doi.org/10.1177/0194599820934748
Bhatt SM, Lauretano A, Cabellos C, Halpin C, Levine RA, Xu WZ et al (1993) Progression of hearing loss in experimental pneumococcal meningitis: correlation with cerebrospinal fluid cytochemistry. J Infect Dis 167:675–683. https://doi.org/10.1093/infdis/167.3.675
Lun ZR, Wang QP, Chen XG, Li AX, Zhu XQ (2007) Streptococcus suis: an emerging zoonotic pathogen. Lancet Infect Dis 7:201–209. https://doi.org/10.1016/S1473-3099(07)70001-4
van Samkar A, Brouwer MC, Schultsz C, van der Ende A, van de Beek D (2015) Streptococcus suis meningitis: a systematic review and meta-analysis. PLoS Negl Trop Dis 9:e0004191. https://doi.org/10.1371/journal.pntd.0004191
Meijerink M, Ferrando ML, Lammers G, Taverne N, Smith HE, Wells JM (2012) Immunomodulatory effects of Streptococcus suis capsule type on human dendritic cell responses, phagocytosis and intracellular survival. PLoS ONE 7:e35849. https://doi.org/10.1371/journal.pone.0035849
Xu L, Lin L, Lu X, Xiao P, Liu R, Wu M et al (2021) Acquiring high expression of suilysin enable non-epidemic Streptococccus suis to cause streptococcal toxic shock-like syndrome (STSLS) through NLRP3 inflammasome hyperactivation. Emerg Microbes Infect 10:1309–1319. https://doi.org/10.1080/22221751.2021.1908098
Vaillancourt K, Bonifait L, Grignon L, Frenette M, Gottschalk M, Grenier D (2013) Identification and characterization of a new cell surface protein possessing factor H-binding activity in the swine pathogen and zoonotic agent Streptococcus suis. J Med Microbiol 62:1073–1080. https://doi.org/10.1099/jmm.0.057877-0
van de Beek D, Cabellos C, Dzupova O, Esposito S, Klein M, Kloek AT et al (2016) ESCMID guideline: diagnosis and treatment of acute bacterial meningitis. Clin Microbiol Infect 22(Suppl 3):S37-62. https://doi.org/10.1016/j.cmi.2016.01.007
Bamphensin N, Chopjitt P, Hatrongjit R, Boueroy P, Fittipaldi N, Gottschalk M et al (2021) Non-penicillin-susceptible Streptococcus suis isolated from humans. Pathogens 10:1178. https://doi.org/10.3390/pathogens10091178
Tinling SP, Colton J, Brodie HA (2004) Location and timing of initial osteoid deposition in postmeningitic labyrinthitis ossificans determined by multiple fluorescent labels. Laryngoscope 114:675–680. https://doi.org/10.1097/00005537-200404000-00015
van Loon MC, Hensen EF, de Foer B, Smit CF, Witte B, Merkus P (2013) Magnetic resonance imaging in the evaluation of patients with sensorineural hearing loss caused by meningitis: implications for cochlear implantation. Otol Neurotol 34:845–854. https://doi.org/10.1097/MAO.0b013e31828dafee
Booth TN, Roland P, Kutz JW Jr, Lee K, Isaacson B (2013) High-resolution 3-D T2-weighted imaging in the diagnosis of labyrinthitis ossificans: emphasis on subtle cochlear involvement. Pediatr Radiol 43:1584–1590. https://doi.org/10.1007/s00247-013-2747-5
Kaya S, Paparella MM, Cureoglu S (2016) Pathologic findings of the cochlea in labyrinthitis ossificans associated with the round window membrane. Otolaryngol Head Neck Surg 155:635–640. https://doi.org/10.1177/0194599816651245
Kaya S, Tsuprun V, Hizli Ö, Paparella MM, Cureoglu S (2016) Quantitative assessment of cochlear histopathologic findings in patients with suppurative labyrinthitis. JAMA Otolaryngol Head Neck Surg 142:364–369. https://doi.org/10.1001/jamaoto.2015.3803
Acknowledgements
The authors would like to thank all patients who participated in the study. This work was supported by the National Natural Science Foundation of China (82271156).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design.
Corresponding author
Ethics declarations
Conflict of interest
There are no conflicts of interest, financial, or otherwise.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Jiang, S., Tan, X., Shu, F. et al. Cochlear implantation for rare Streptococcus suis meningitis with hearing loss. Eur Arch Otorhinolaryngol (2024). https://doi.org/10.1007/s00405-024-08730-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00405-024-08730-w