Abstract
Introduction
The Video Head Impulse Test (vHIT) is a safe and reliable assessment of peripheral vestibular function. Many studies tested its accuracy in clinical settings for differential diagnosis and quantification of the vestibulo-oculomotor reflex (VOR) in various disorders. However, the results of its application after lesions of the CNS are discordant and have never been studied in rehabilitation. This study aims to assess the VOR performance in a sample of stroke survivors.
Methods
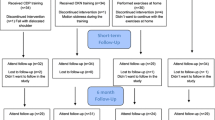
This is a cross-sectional study on 36 subacute and chronic stroke survivors; only persons with first-ever stroke and able to walk independently, even with supervision, were included. We performed VOR assessments for each semicircular canal by vHIT and balance assessments by the Berg Balance Scale and the MiniBESTest scale.
Results
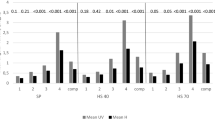
Two hundred and sixteen semicircular canals were assessed using the Head Impulse paradigm (in both the vertical and horizontal planes), while 72 semicircular canals were assessed using the Suppressed Head Impulse paradigm (horizontal plane). There was a high prevalence of participants with dysfunctional canals, particularly for the left anterior and right posterior canals, which were each prevalent in more than one-third of our sample. Furthermore, 16 persons showed an isolated canal dysfunction. The mean VOR gain for the vertical canals had confidence intervals out of the normal values (0.74–0.91 right anterior; 0.74–0.82 right posterior; 0.73–0.87 left anterior).
Conclusion
Our findings suggest that peripheral vestibular function may be impaired in people with stroke; a systematic assessment in a rehabilitation setting could allow a more personalized and patient-centred approach.


Similar content being viewed by others
References
MacDougall HG, McGarvie LA, Halmagyi GM, Curthoys IS, Weber KP (2013) Application of the video head impulse test to detect vertical semicircular canal dysfunction. Otol Neurotol Off Publ Am Otol Soc Am Neurotol Soc Eur Acad Otol Neurotol 34(6):974–979. https://doi.org/10.1097/MAO.0b013e31828d676d
Manzari L, Princi AA, De Angelis S, Tramontano M (2021) Clinical value of the video head impulse test in patients with vestibular neuritis: a systematic review. Eur Arch Oto-Rhino-Laryngol Off J Eur Fed Oto-Rhino-Laryngol Soc EUFOS Affil Ger Soc Oto-Rhino-Laryngol 278(11):4155–4167. https://doi.org/10.1007/s00405-021-06803-8
Manzari L, Orejel Bustos AS, Princi AA, Tramontano M (2022) Video suppression head impulses and head impulses paradigms in patients with vestibular neuritis: a comparative study. Healthcare 10(10):1926. https://doi.org/10.3390/healthcare10101926
MacDougall HG, Weber KP, McGarvie LA, Halmagyi GM, Curthoys IS (2009) The video head impulse test: diagnostic accuracy in peripheral vestibulopathy. Neurology 73(14):1134–1141. https://doi.org/10.1212/WNL.0b013e3181bacf85
Kim HJ, Lee SH, Park JH, Choi JY, Kim JS (2014) Isolated vestibular nuclear infarction: report of two cases and review of the literature. J Neurol 261(1):121–129. https://doi.org/10.1007/s00415-013-7139-0
Nham B, Wang C, Reid N et al (2023) Modern vestibular tests can accurately separate stroke and vestibular neuritis. J Neurol 270(4):2031–2041. https://doi.org/10.1007/s00415-022-11473-5
Ha SH, Lee DK, Park G et al (2023) Prospective analysis of video head impulse tests in patients with acute posterior circulation stroke. Front Neurol 14:1256826. https://doi.org/10.3389/fneur.2023.1256826
Pavlović I, Ruška B, Pavičić T et al (2017) Video head impulse test can detect brainstem dysfunction in multiple sclerosis. Mult Scler Relat Disord 14:68–71. https://doi.org/10.1016/j.msard.2017.04.001
Grove CR, Wagner A, Yang VB, Loyd BJ, Dibble LE, Schubert MC (2022) Greater disability is associated with worse vestibular and compensatory oculomotor functions in people living with multiple sclerosis. Brain Sci 12(11):1519. https://doi.org/10.3390/brainsci12111519
Berkiten G, Tutar B, Atar S et al (2023) Assessment of the clinical use of vestibular evoked myogenic potentials and the video head impulse test in the diagnosis of early-stage Parkinson’s disease. Ann Otol Rhinol Laryngol 132(1):41–49. https://doi.org/10.1177/00034894211067838
Morrison M, Korda A, Zamaro E et al (2022) Paradigm shift in acute dizziness: is caloric testing obsolete? J Neurol 269(2):853–860. https://doi.org/10.1007/s00415-021-10667-7
Machner B, Erber K, Choi JH, Trillenberg P, Sprenger A, Helmchen C (2021) Usability of the head impulse test in routine clinical practice in the emergency department to differentiate vestibular neuritis from stroke. Eur J Neurol 28(5):1737–1744. https://doi.org/10.1111/ene.14707
Sayed SZ, Abdul Wahat NH, Raymond AA, Hussein N, Wan Asyraf WZ, Omar M (2021) Quantitative vestibular function tests in posterior circulation stroke patients: a review. Med J Malaysia 76(6):898–905
HeravianShandiz J, Jafarzadeh S, Fathi H, Foroughipour M, Karimpour M (2021) Vestibulo ocular reflex in multiple sclerosis patients without any optic neuritis. J Optom 14(3):282–286. https://doi.org/10.1016/j.optom.2020.07.001
Ertugrul G, Konuskan B, Solmaz I, Anlar B, Aksoy S (2020) Vestibulo-ocular reflex involvement in childhood-onset multiple sclerosis. Mult Scler Relat Disord 44:102329. https://doi.org/10.1016/j.msard.2020.102329
Le TTC, Brewer K, Serrador J, Schubert MC (2020) Veterans with dizziness recruit compensatory saccades in each semicircular canal plane although VOR gain is normal. J Vestib Res Equilib Orientat 30(1):47–53. https://doi.org/10.3233/VES-200692
von Elm E, Altman DG, Egger M et al (2008) The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol 61(4):344–349. https://doi.org/10.1016/j.jclinepi.2007.11.008
Curthoys IS, Manzari L, Rey-Martinez J, Dlugaiczyk J, Burgess AM (2021) Enhanced eye velocity in head impulse testing—a possible indicator of endolymphatic hydrops. Front Surg 8:666390. https://doi.org/10.3389/fsurg.2021.666390
Zamaro E, SaberTehrani AS, Kattah JC, Eibenberger K, Guede CI, Armando L, Caversaccio MD, Newman-Toker DE, Mantokoudis G (2020) VOR gain calculation methods in video head impulse recordings. J Vestib Res 30(4):225–234. https://doi.org/10.3233/VES-200708
Manzari L, De Angelis S, Princi AA, Galeoto G, Tramontano M (2022) The Clinical use of the suppression head impulse paradigm in patients with vestibulopathy: a systematic review. Healthc Basel Switz 10(7):1182. https://doi.org/10.3390/healthcare10071182
Alfarghal M, Algarni MA, Sinha SK, Nagarajan A (2022) VOR gain of lateral semicircular canal using video head impulse test in acute unilateral vestibular hypofunction: a systematic review. Front Neurol 13:948462. https://doi.org/10.3389/fneur.2022.948462
Smith RM, Burgess C, Tahtis V, Marsden J, Seemungal BM (2023) Why are patients with acute traumatic brain injury not routinely assessed or treated for vestibular dysfunction in the UK? A qualitative study. BMJ Open 13(1):e067967. https://doi.org/10.1136/bmjopen-2022-067967
Meldrum D, Burrows L, Cakrt O et al (2020) Vestibular rehabilitation in Europe: a survey of clinical and research practice. J Neurol 267(Suppl 1):24–35. https://doi.org/10.1007/s00415-020-10228-4
Bonnì S, Ponzo V, Tramontano M et al (2019) Neurophysiological and clinical effects of blindfolded balance training (BBT) in Parkinson’s disease patients: a preliminary study. Eur J Phys Rehabil Med 55(2):176–182. https://doi.org/10.23736/S1973-9087.18.05126-2
Tramontano M, Piermaria J, Morone G, Reali A, Vergara M, Tamburella F (2019) Postural changes during exteroceptive thin plantar stimulation: the effect of prolonged use and different plantar localizations. Front Syst Neurosci 13:49. https://doi.org/10.3389/fnsys.2019.00049
Bent LR, McFadyen BJ, Inglis JT (2005) Vestibular contributions during human locomotor tasks. Exerc Sport Sci Rev 33(3):107–113. https://doi.org/10.1097/00003677-200507000-00002
Funding
Data are available under reasonable request to the corresponding author.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical statement
The study was approved by the Local Independent Ethics Committee with protocol number Prot. CE/2022_011 of Santa Lucia Foundation (Institute for Research and Healthcare). All procedures contributing to this work comply with the ethical standards of the relevant national and institutional guidelines on human experimentation and with the World Medical Association Declaration of Helsinki.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tramontano, M., Ferri, N., Turolla, A. et al. Video head impulse test in subacute and chronic stroke survivors: new perspectives for implementation of assessment in rehabilitation. Eur Arch Otorhinolaryngol (2024). https://doi.org/10.1007/s00405-024-08721-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00405-024-08721-x