Abstract
Purpose
This study was designed to identify risk factors for post-operative complications in micro-anastomosed osteomyocutaneous free flaps (MOFF) and analyzed their consequences in long term.
Methods
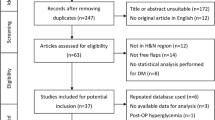
A retrospective review of 100 MOFF realized between May 2007 and October 2019 was performed. Demographic data, perioperative management and postoperative complications were enrolled and analyzed in a multivariate model. Patients were followed for ≥ 6 months.
Results
Major surgical complication rate was 20% with 5% of overall free flap failure rate and 6% of anastomosis salvage surgery. Risk identified for major surgical complication was alcohol consumption (p = 0.0054). Minor surgical complications occurred in 26% of patients mostly due to infections (19%). No significant risk factor was associated to minor surgical complications. Major and minor medical complication rates were, respectively, 10% and 10%. Risk identified for major medical complication were age over 70 (p = 0.0253) and history of chemotherapy (p = 0.0277). Risk identified for minor medical complication were alcohol consumption p = 0.0232) and a history of radiotherapy (p = 0.0329).
Conclusions
Alcoholism is an independent risk factor for the surgical complication of MOFF that must be taken into account before surgery. Patients with a history of chemotherapy, radiotherapy or who are over 70 years of age are at greater risk of postoperative medical complications and require special attention.
Similar content being viewed by others
References
Bozec A, Poissonnet G, Converset S, Lattes L, Chamorey E, Vallicioni J et al (2007) Mandibular reconstruction with osseous free flaps: functional results. Ann Otolaryngol Chir Cervicofac 124(1):16–24
Novakovic D, Patel RS, Goldstein DP, Gullane PJ (2009) Salvage of failed free flaps used in head and neck reconstruction. Head Neck Oncol 1:33
Patel RS, McCluskey SA, Goldstein DP, Minkovich L, Irish JC, Brown DH et al (2010) Clinicopathologic and therapeutic risk factors for perioperative complications and prolonged hospital stay in free flap reconstruction of the head and neck. Head Neck 32(10):1345–1353
Ferrier MB, Spuesens EB, Le Cessie S, Baatenburg de Jong RJ (2005) Comorbidity as a major risk factor for mortality and complications in head and neck surgery. Arch Otolaryngol Head Neck Surg. 131(1):27–32
Poisson M, Longis J, Schlund M, Pere M, Michel G, Delagranda A et al (2019) Postoperative morbidity of free flaps in head and neck cancer reconstruction: a report regarding 215 cases. Clin Oral Investig 23(5):2165–2171
Classen DA, Ward H (2006) Complications in a consecutive series of 250 free flap operations. Ann Plastic Surg 56(5):557–561
Kuo Y-R, Jeng S-F, Lin K-M, Hou S-J, Su C-Y, Chien C-Y et al (2008) Microsurgical tissue transfers for head and neck reconstruction in patients with alcohol-induced mental disorder. Ann Surg Oncol 15(1):371–377
Suh JD, Sercarz JA, Abemayor E, Calcaterra TC, Rawnsley JD, Alam D et al (2004) Analysis of outcome and complications in 400 cases of microvascular head and neck reconstruction. Arch Otolaryngol Head Neck Surg 130(8):962–966
O’Brien CJ, Lee KK, Stern HS, Traynor SJ, Bron L, Tew PJ et al (1998) Evaluation of 250 free-flap reconstructions after resection of tumours of the head and neck. Aust N Z J Surg 68(10):698–701
WHO (2000) International guide for monitoring alcohol consumption and related harm. Genève, pp 1–209
Crawley MB, Sweeny L, Ravipati P, Heffelfinger R, Krein H, Luginbuhl A et al (2019) Factors associated with free flap failures in head and neck reconstruction. Otolaryngol Head Neck Surg 161(4):598–604
Hirigoyen MB, Urken ML, Weinberg H (1995) Free flap monitoring: a review of current practice. Microsurgery 16(11):723–726 (discussion 727)
Brown JS, Devine JC, Magennis P, Sillifant P, Rogers SN, Vaughan ED (2003) Factors that influence the outcome of salvage in free tissue transfer. Br J Oral Maxillofac Surg 41(1):16–20
Okazaki M, Asato H, Takushima A, Sarukawa S, Nakatsuka T, Yamada A et al (2007) Analysis of salvage treatments following the failure of free flap transfer caused by vascular thrombosis in reconstruction for head and neck cancer. Plast Reconstr Surg 119(4):1223–1232
Genther DJ, Gourin CG (2012) The effect of alcohol abuse and alcohol withdrawal on short-term outcomes and cost of care after head and neck cancer surgery. Laryngoscope 122(8):1739–1747
Gallivan KH, Reiter D (2001) Acute alcohol withdrawal and free flap mandibular reconstruction outcomes. Arch Facial Plast Surg 3(4):264–266
Szabo G, Saha B (2015) Alcohol’s effect on host defense. Alcohol Res 37(2):159–170
Souza-Smith FM, Simon L, Siggins R, Molina PE (2019) Alcohol-induced mesenteric lymphatic permeability: link to immunometabolic modulation of perilymphatic adipose tissue. Int J Mol Sci 20(17):4097
Lau AH, Szabo G, Thomson AW (2009) Antigen-presenting cells under the influence of alcohol. Trends Immunol 30(1):13–22
Blackwell KE, Azizzadeh B, Ayala C, Rawnsley JD (2002) Octogenarian free flap reconstruction: complications and cost of therapy. Otolaryngol Head Neck Surg 126(3):301–306
Beausang ES, Ang EE, Lipa JE, Irish JC, Brown DH, Gullane PJ et al (2003) Microvascular free tissue transfer in elderly patients: the Toronto experience. Head Neck 25(7):549–553
Bengtson BP, Schusterman MA, Baldwin BJ, Miller MJ, Reece GP, Kroll SS et al (1993) Influence of prior radiotherapy on the development of postoperative complications and success of free tissue transfers in head and neck cancer reconstruction. Am J Surg 166(4):326–330
Arce K, Bell RB, Potter JK, Buehler MJ, Potter BE, Dierks EJ (2012) Vascularized free tissue transfer for reconstruction of ablative defects in oral and oropharyngeal cancer patients undergoing salvage surgery following concomitant chemoradiation. Int J Oral Maxillofac Surg 41(6):733–738
Klug C, Berzaczy D, Reinbacher H, Voracek M, Rath T, Millesi W et al (2006) Influence of previous radiotherapy on free tissue transfer in the head and neck region: evaluation of 455 cases. Laryngoscope 116(7):1162–1167
Acknowledgements
Estelle Le Pabic [Department Inserm, CIC 1414 (Centre d’Investigation Clinique), Rennes University Hospital, Rennes, France.]
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare for this publication and no financial support.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lambert, C., Creff, G., Mazoue, V. et al. Risk factors associated with early and late free flap complications in head and neck osseous reconstruction. Eur Arch Otorhinolaryngol 280, 811–817 (2023). https://doi.org/10.1007/s00405-022-07619-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-022-07619-w