Abstract
Purpose
The purpose of this study was to assess whether the infrahyoid skeletal muscle index (IHSMI) can be used instead of the L3 skeletal muscle index (L3SMI) to define sarcopenia and predict prognosis in patients with locally advanced head and neck squamous cell carcinoma (LHNSCC).
Methods
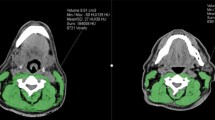
Patients treated for LHNSCC between January 2009 and April 2018 were assessed. The muscular area at the L3 transverse process and infrahyoid was contoured on absorption-corrected computed tomography prior to treatment. Sarcopenia based on L3SMI (S-L) was defined as values of < 52.4 cm2/m2 for men and < 38.5 cm2/m2 for women. Sarcopenia based on IHSMI (S-I) was determined via receiver operating curve analysis. Overall survival (OS) and cause-specific survival (CSS) curves were constructed using the Kaplan–Meier method.
Results
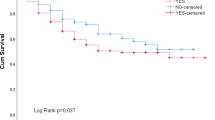
In total, 101 patients were analyzed. The median follow-up period was 19 months (range 3–101 month). S-L and S-I were identified in 74 (73.3%) and 56 patients (55.4%), respectively. The 5-year OS rate did not differ between patients with and without S-L (64.9% vs. 79.2%, p = 0.635), whereas the rate was lower in patients with S-I than without S-I (57.1% vs. 93.0%, p = 0.006). Similarly, the 5-year CSS rate did not differ between patients with and without S-L (77.0% vs. 82.3%, p = 0.523), but the rate was lower in patients with S-I (61.2% vs. 93.0%, p = 0.02).
Conclusion
Pretreatment S-I, but not S-L, was a good predictor of OS and CSS in patients with LHNSCC.




Similar content being viewed by others
Data availability
The data generated or analyzed during the current study are included in this article.
Code availability
Not applicable to this study.
References
Dechaphunkul T, Martin L, Alberda C, Olson K, Baracos V, Gramlich L (2013) Malnutrition assessment in patients with cancers of the head and neck: a call to action and consensus. Crit Rev Oncol Hematol 88:459–476. https://doi.org/10.1016/j.critrevonc.2013.06.003
Prado CM, Lieffers JR, Bowthorpe L, Baracos VE, Mourtzakis M, McCargar LJ (2013) Sarcopenia and physical function in overweight patients with advanced cancer. Can J Diet Pract Res 74:69–74. https://doi.org/10.3148/74.2.2013.69
Surov A, Wienke A (2021) Low skeletal muscle mass predicts relevant clinical outcomes in head and neck squamous cell carcinoma. A meta analysis. Ther Adv Med Oncol 13:17588359211008844. https://doi.org/10.1177/17588359211008844
Matsuyama R, Maeda K, Yamanaka Y, Ishida Y, Kato R, Nonogaki T, Shimizu A, Ueshima J, Kazaoka Y, Hayashi T, Ito K, Furuhashi A, Ono T, Mori N (2021) Assessing skeletal muscle mass based on the cross-sectional area of muscles at the 12th thoracic vertebra level on computed tomography in patients with oral squamous cell carcinoma. Oral Oncol 113:105126. https://doi.org/10.1016/j.oraloncology.2020.105126
Prado CM, Lieffers JR, McCargar LJ, Reiman T, Sawyer MB, Martin L, Baracos VE (2008) Prevalence and clinical implications of sarcopenic obesity in patients with solid tumours of the respiratory and gastrointestinal tracts: a population-based study. Lancet Oncol 9:629–635. https://doi.org/10.1016/S1470-2045(08)70153-0
Antoun S, Lanoy E, Iacovelli R, Albiges-Sauvin L, Loriot Y, Merad-Taoufik M, Fizazi K, di Palma M, Baracos VE, Escudier B (2013) Skeletal muscle density predicts prognosis in patients with metastatic renal cell carcinoma treated with targeted therapies. Cancer 119:3377–3384. https://doi.org/10.1002/cncr.28218
Kanda Y (2013) Investigation of the freely available easy-to-use software ’EZR’ for medical statistics. Bone Marrow Transplant 48:452–458. https://doi.org/10.1038/bmt.2012.244
Pressoir M, Desné S, Berchery D, Rossignol G, Poiree B, Meslier M, Traversier S, Vittot M, Simon M, Gekiere JP, Meuric J, Serot F, Falewee MN, Rodrigues I, Senesse P, Vasson MP, Chelle F, Maget B, Antoun S, Bachmann P (2010) Prevalence, risk factors and clinical implications of malnutrition in French Comprehensive Cancer Centres. Br J Cancer 102:966–971. https://doi.org/10.1038/sj.bjc.6605578
Blum D, Stene GB, Solheim TS, Fayers P, Hjermstad MJ, Baracos VE, Fearon K, Strasser F, Kaasa S, Euro-Impact (2014) Validation of the consensus-definition for Cancer cachexia and evaluation of a classification model–a study based on data from an international multicentre project (EPCRC-CSA). Ann Oncol 25:1635–1642. https://doi.org/10.1093/annonc/mdu086
Langius JA, Bakker S, Rietveld DH, Kruizenga HM, Langendijk JA, Weijs PJ, Leemans CR (2013) Critical weight loss is a major prognostic indicator for disease-specific survival in patients with head and neck cancer receiving radiotherapy. Br J Cancer 109:1093–1099. https://doi.org/10.1038/bjc.2013.458
Bokhorst-de V, van der Schueren MA, van Leeuwen PA, Sauerwein HP, Kuik DJ, Snow GB, Quak JJ (1997) Assessment of malnutrition parameters in head and neck cancer and their relation to postoperative complications. Head Neck 19:419–425. https://doi.org/10.1002/(sici)1097-0347(199708)19:5%3c419::aid-hed9%3e3.0.co;2-2
Huiskamp LFJ, Chargi N, Devriese LA, de Jong PA, de Bree R (2020) The predictive and prognostic value of low skeletal muscle mass for dose-limiting toxicity and survival in head and neck cancer patients receiving concomitant cetuximab and radiotherapy. Eur Arch Otorhinolaryngol 277:2847–2858. https://doi.org/10.1007/s00405-020-05972-2
Rijn-Dekker MI, Bosch L, Van Den Hoek JGM, Bijl HP, Van Aken ESM, Van der Hoorn A, van der Hoorn A, Oosting SF, Halmos GB, Witjes MJH, van der Laan HP, Langendijk JA, Steenbakkers RJHM (2020) Impact of sarcopenia on survival and late toxicity in head and neck cancer patients treated with radiotherapy. Radiother Oncol 147:103–110. https://doi.org/10.1016/j.radonc.2020.03.014
Karsten RT, Al-Mamgani A, Bril SI, Tjon-A-Joe S, Van der Molen L, De Boer JP, Hilgers FJM, Smeele LE, van den Brekel MWM, Stuiver MM (2019) Sarcopenia, a strong determinant for prolonged feeding tube dependency after chemoradiotherapy for head and neck cancer. Head Neck 41:4000–4008. https://doi.org/10.1002/hed.25938
Caburet C, Farigon N, Mulliez A, Mom T, Boirie Y, Gilain L, Saroul N (2020) Impact of nutritional status at the outset of assessment on postoperative complications in head and neck cancer. Eur Ann Otorhinolaryngol Head Neck Dis 137:393–398. https://doi.org/10.1016/j.anorl.2019.12.005
Funding
The authors received no funding support.
Author information
Authors and Affiliations
Contributions
DY, MO, EA, KT, MT, TN, and KS were involved in study design. DY, MO, EA, and KS were involved in data interpretation. DY, MO, and EA were involved in the data analysis. All the authors critically revised the report, commented on drafts of the manuscript, and approved the final report.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest.
Ethical approval
This retrospective cohort study was approved by the institutional ethical board (Approval number: SH4112). This clinical investigation was conducted according to the Declaration of Helsinki principles.
Consent to participate
The requirement for written informed consent was waived.
Consent for publication
Not applicable to this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yunaiyama, D., Okubo, M., Arizono, E. et al. Sarcopenia at the infrahyoid level as a prognostic factor in patients with advanced-stage non-virus-related head and neck carcinoma. Eur Arch Otorhinolaryngol 279, 3131–3137 (2022). https://doi.org/10.1007/s00405-021-07147-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-021-07147-z