Abstract
Introduction
The aim of this retrospective study was to assess the efficacy of Salivary Bypass Tube (SBT) for preventing pharyngo-cutaneous fistula (PCF) in a recent cohort of patients who underwent primary and salvage total laryngectomy (TL).
Methods
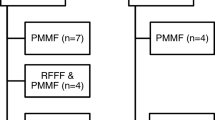
A consecutive series of 133 patients who underwent total laryngectomy between 1997 and 2019 was reviewed. The incidence of PCF was compared between patients who did not receive SBT (nSBT group; n = 55) and those preventively receiving SBT (SBT group; n = 78) in both primary and salvage TL. Risk factors for PCF were evaluated in a univariate and multivariate analyses.
Results
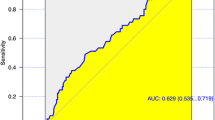
The overall PCF rate was 30%. Preoperative characteristics were similar between the nSBT and SBT groups, except for older age (p = 0.016), lower preoperative hemoglobin (p = 0.043), and lesser neoadjuvant chemotherapy (p = 0.015) in the SBT group. The rate of PCF the nSBT group, was 41.5%, compared to 21.8% in the SBT group (p = 0.020). In multivariate analysis, only the use of SBT was associated with lower risk of PCF (OR = 0.41 (95% CI 0.19–0.89), p = 0.026). This effect was verified only in the subgroup of patient operated for salvage TL (OR = 0.225; 95% CI 0.09–0.7; p = 0.008).
Conclusion
The use of SBT in our series in salvage TL, appears to be associated with a decreased risk of PCF.
Similar content being viewed by others
Data availability
The data sets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.
References
Kamhieh Y, Fox H, Hallett E, Berry S (2018) Routine use of salivary bypass tubes in laryngectomy patients: systematic review. J Laryngol Otol 132:380–384
Hasan Z, Dwivedi RC, Gunaratne DA, Virk SA, Palme CE, Riffat F (2017) Systematic review and meta-analysis of the complications of salvage total laryngectomy. Eur J Surg Oncol 43:42–51
Virtaniemi JA et al (2001) The incidence and etiology of postlaryngectomy pharyngocutaneous fistulae. Head Neck. https://doi.org/10.1002/1097-0347(200101)23:1%3c29::AID-HED5%3e3.0.CO;2-P
Busoni M, Deganello A, Gallo O (2015) Fistola faringocutanea dopo laringectomia totale: analisi dei fattori di rischio, della prognosi e delle modalità di trattamento. Acta Otorhinolaryngol Ital 35(6):400–405
White HN, Golden B, Sweeny L, Carroll WR, Magnuson JS, Rosenthal EL (2012) Assessment and incidence of salivary leak following laryngectomy. Laryngoscope 122(8):1796–1799. https://doi.org/10.1002/lary.23443
Boscolo-Rizzo P, De Cillis G, Marchiori C, Carpenè S, Da Mosto MC (2008) Multivariate analysis of risk factors for pharyngocutaneous fistula after total laryngectomy. Eur Arch Otorhinolaryngol 265(8):929–936. https://doi.org/10.1007/s00405-007-0562-z
Paydarfar JA, Birkmeyer NJ (2006) Complications in head and neck surgery: a meta-analysis of postlaryngectomy pharyngocutaneous fistula. Arch Otolaryngol Head Neck Surg 132(1):67–72
Ganly I, Patel S, Matsuo J, Singh B, Kraus D, Boyle J et al (2005) Postoperative complications of salvage total laryngectomy. Cancer 103(10):2073–2081. https://doi.org/10.1002/cncr.20974
Erdag MA, Arslanoglu S, Onal K, Songu M, Tuylu AO (2013) Pharyngocutaneous fistula following total laryngectomy: multivariate analysis of risk factors. Eur Arch Otorhinolaryngol 270(1):173–179. https://doi.org/10.1007/s00405-012-2111-7
Liang JW, Li ZD, Li SC, Fang FQ, Zhao YJ, Li YG (2015) Pharyngocutaneous fistula after total laryngectomy: a systematic review and meta-analysis of risk factors. Auris Nasus Larynx 42:353–359
Grau C, Johansen LV, Hansen HS, Andersen E, Godballe C, Andersen LJ et al (2003) Salvage laryngectomy and pharyngocutaneous fistulae after primary radiotherapy for head and neck cancer: a national survey from DAHANCA. Head Neck 25(9):711–716. https://doi.org/10.1002/hed.10237
Montgomery WW (1978) Salivary bypass tube. Ann Otol Rhinol Laryngol 87(2):159–162. https://doi.org/10.1177/000348947808700202
Sobin LH, Gospodarowicz MK, Wittekind C (eds) (2009) TNM classification of malignant tumours, 7th edn. Wiley-Blackwell, Chichester, UK
Dindo D, Demartines N, Clavien P-A (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
Sayles M, Grant DG (2014) Preventing pharyngo-cutaneous fistula in total laryngectomy: a systematic review and meta-analysis. Laryngoscope 124:1150–1163
Walton B, Vellucci J, Patel PB, Jennings K, McCammon S, Underbrink MP (2018) Post-Laryngectomy stricture and pharyngocutaneous fistula: review of techniques in primary pharyngeal reconstruction in laryngectomy. Clin Otolaryngol 43(1):109–116. https://doi.org/10.1111/coa.12905
Maclean J, Cotton S, Perry A (2008) Variation in surgical methods used for total laryngectomy in Australia. J Laryngol Otol 122(7):728–732
Maclean J, Szczesniak M, Cotton S, Cook I, Perry A (2011) Impact of a laryngectomy and surgical closure technique on swallow biomechanics and dysphagia severity. Otolaryngol Head Neck Surg 144(1):21–28
Davis RK, Vincent ME, Shapshay SM, Strong MS (1982) The anatomy and complications of “T” versus vertical closure of the hypopharynx after laryngectomy. Laryngoscope 92(1):16–22
Pitroda SP, Khodarev NN, Huang L, Uppal A, Wightman SC, Ganai S et al (2018) Integrated molecular subtyping defines a curable oligometastatic state in colorectal liver metastasis. Nat Commun 9(1):1793
Qureshi SS, Chaturvedi P, Pai PS, Chaukar DA, Deshpande MS, Pathak KA et al (2005) A prospective study of pharyngocutaneous fistulas following total laryngectomy. J Cancer Res Ther 1(1):51–56
Lorenzo JG, Martínez VM, Quera AR, Aroca AC, Vilas ML, Agustí MQ et al (2017) Modifications in the treatment of advanced laryngeal cancer throughout the last 30 years. Eur Arch Otorhinolaryngol 274(9):3449–3455. https://doi.org/10.1007/s00405-017-4639-z
Punthakee X, Zaghi S, Nabili V, Knott PD, Blackwell KE (2013) Effects of salivary bypass tubes on fistula and stricture formation. JAMA Facial Plast Surg 15(3):219–225
León X, Quer M, Burgués J (1999) Montgomery® salivary bypass tube in the reconstruction of the hypopharynx. Cost-benefit study. Ann Otol Rhinol Laryngol 108(9):864–868
Bondi S, Giordano L, Limardo P, Bussi M (2013) Role of Montgomery salivary stent placement during pharyngolaryngectomy, to prevent pharyngocutaneous fistula in high-risk patients. J Laryngol Otol 127(1):54–57
Acknowledgements
We acknowledge the contribution of a medical writer, Sandy Field, PhD, for English language editing of this document.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to disclose.
Ethical approval
The study was approved by the Ethics Committee of Institute Jules Bordet (CE3144).
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bohlok, A., Richet, T., Quiriny, M. et al. The effect of salivary bypass tube use on the prevention of pharyngo-cutaneous fistulas after total laryngectomy. Eur Arch Otorhinolaryngol 279, 311–317 (2022). https://doi.org/10.1007/s00405-021-07082-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-021-07082-z