Abstract
Purpose
Although it has been reported that superoxide dismutase (SOD) is related to obstructive sleep apnea (OSA), the results are controversial. In addition, the effects of the continuous positive airway pressure (CPAP) treatment on SOD levels are also inconsistent. The primary purpose of the present meta-analysis is to determine the relationship between the circulating SOD levels and OSA.
Methods
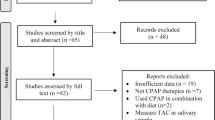
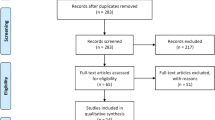
The studies included in this meta-analysis were selected from the PubMed, Embase, Cochrane Library, and Scopus databases. Two researchers independently reviewed the studies. Data analysis was performed using Stata 15.1. The overall effects were measured using the standardized mean difference (SMD) with a 95% confidence interval (CI). A random-effects model or a fixed-effects model was used, depending on the heterogeneity of the studies.
Results
A total of 14 studies were included, comprising 1240 patients and 457 controls. The results showed that the circulating SOD levels of the patients with OSA were significantly lower than that of the control group (SMD = − 1.645, 95% CI = − 2.279 to − 1.011, P < 0.001). We also studied changes in the circulating SOD levels in patients with OSA after the CPAP treatment. No significant difference was observed in the circulating SOD levels after the CPAP treatment (SMD = − 0.028, 95% CI = − 0.218 to 0.162, P = 0.772).
Conclusion
The results suggested that patients with OSA have reduced levels of SOD and were related to disease severity. The results also indicated that circulating SOD levels may be a reliable marker for detecting systemic oxidative stress in patients with OSA. However, the circulating SOD levels were not affected by the short-term (4–12 weeks) CPAP treatment. Therefore, further large-scale, well-designed randomized controlled trials with a longer CPAP therapy (more than 6 months preferably) and good adherence to the treatment are needed to investigate this issue.





Similar content being viewed by others
References
Arnaud C, Bochaton T, Pepin JL, Belaidi E (2020) Obstructive sleep apnoea and cardiovascular consequences: pathophysiological mechanisms. Arch Cardiovasc Dis 113(5):350–358. https://doi.org/10.1016/j.acvd.2020.01.003
Brieger K, Schiavone S, Miller FJ Jr, Krause KH (2012) Reactive oxygen species: from health to disease. Swiss Med Wkly 142:w13659. https://doi.org/10.4414/smw.2012.13659
Papachristoforou E, Lambadiari V, Maratou E, Makrilakis K (2020) Association of glycemic indices (hyperglycemia, glucose variability, and hypoglycemia) with oxidative stress and diabetic complications. J Diabetes Res 2020(1):1–17
Prabhakar NR, Peng YJ, Nanduri J (2020) Hypoxia-inducible factors and obstructive sleep apnea. J Clin Invest 130(10):5042–5051. https://doi.org/10.1172/JCI137560(2020)
Chang JC, Lien CF, Lee WS, Chang HR, Hsu YC, Luo YP, Jeng JR, Hsieh JC, Yang KT (2019) Intermittent hypoxia prevents myocardial mitochondrial Ca(2+) overload and cell death during ischemia/reperfusion: the role of reactive oxygen species. Cells 8(6):564. https://doi.org/10.3390/cells8060564
Gistera A, Hansson GK (2017) The immunology of atherosclerosis. Nat Rev Nephrol 13(6):368–380. https://doi.org/10.1038/nrneph.2017.51
Wang W, Kang PM (2020) Oxidative stress and antioxidant treatments in cardiovascular diseases. Antioxidants 9(12):1292
Murri M, García-Delgado R, Alcázar-Ramírez J, De Fernández RL, Fernández-Ramos A, Cardona F, Tinahones FJ (2011) Continuous positive airway pressure therapy reduces oxidative stress markers and blood pressure in sleep apnea-hypopnea syndrome patients. Biol Trace Elem Res 143(3):1289–1301. https://doi.org/10.1007/s12011-011-8969-1
Yang XH, Liu X, Shang J, Liu HG, Xu YJ (2013) Correlation between the serum level of advanced oxidation protein products and the cognitive function in patients with obstructive sleep apnea hypopnea syndrome. Chin J tuberc Respir Dis 36(4):274–279
Alzoghaibi MA, Bahammam AS (2005) Lipid peroxides, superoxide dismutase and circulating IL-8 and GCP-2 in patients with severe obstructive sleep apnea: a pilot study. Sleep Breath 9(3):119–126. https://doi.org/10.1007/s11325-005-0022-1
Ntalapascha M, Makris D, Kyparos A, Tsilioni I, Kostikas K, Gourgoulianis K, Kouretas D, Zakynthinos E (2013) Oxidative stress in patients with obstructive sleep apnea syndrome. Sleep Breath 17(2):549–555. https://doi.org/10.1007/s11325-012-0718-y
Borges YG, Cipriano LHC, Aires R, Zovico PVC, Campos FV, de Araújo MTM, Gouvea SA (2020) Oxidative stress and inflammatory profiles in obstructive sleep apnea: are short-term CPAP or aerobic exercise therapies effective? Sleep Breath 24(2):541–549. https://doi.org/10.1007/s11325-019-01898-0
Wu K, Su X, Li G, Zhang N (2016) Antioxidant carbocysteine treatment in obstructive sleep apnea syndrome: a randomized clinical trial. PLoS ONE 11(2):e0148519
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2010) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg 8(5):336–341. https://doi.org/10.1016/j.ijsu.2010.02.007
Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M, Tugwell P (2000) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. Oxford. http://www.ohri.ca/programs/clinical_epidemiology/oxford.htm. Accessed 1 Sept 2021
Jadad AR, Moore RA, Carroll D, Jenkinson C, Reynolds DJ, Gavaghan DJ, McQuay HJ (1996) Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials 17(1):1–12. https://doi.org/10.1016/0197-2456(95)00134-4
Wan X, Wang W, Liu J, Tong T (2014) Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol 14:135. https://doi.org/10.1186/1471-2288-14-135
Duval S, Tweedie R (2000) Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics 56(2):455–463. https://doi.org/10.1111/j.0006-341x.2000.00455.x
Lee SD, Ju G, Choi JA, Kim JW, Yoon IY (2012) The association of oxidative stress with central obesity in obstructive sleep apnea. Sleep Breath 16(2):511–517. https://doi.org/10.1007/s11325-011-0536-7
Wang P, Li J, Cao H, Shen Y (2014) The effect of oxidative stress on obstructive sleep apnea-hypopnea syndrome combined with hypertension. J Clin Otorhinolaryngol Head Neck Surg 28(9):604–606
Wang Y, Zhang PP, Han XQ, Wang L, Fu AS, Wang HY (2019) Effects of glutathione on oxidative stress, leptin and adiponectin in patients with obstructive sleep apnea complicated with metabolic syndrome. J Clin Otorhinolaryngol Head Neck Surg 33(8):726–729. https://doi.org/10.13201/j.issn.1001-1781.2019.08.011
Liu HG, Liu K, Zhou YN, Xu YJ (2009) Relationship between reduced nicotinamide adenine dinucleotide phosphate oxidase subunit p22phox gene polymorphism and obstructive sleep apnea-hypopnea syndrome in the Chinese Han population. Chin Med J 122(12):1369–1374. https://doi.org/10.3760/cma.j.issn.0366-6999.2009.12.003
Jiang Q, Li TP, Pang B, Wang X, Wang YF (2016) Severe obstructive sleep apnea-hypopnea syndrome with latent renal dysfunction: analysis of 238 cases. J South Med Univ 36(3):339–344
Peres BU, Allen AH, Shah A, Fox N, Ayas N (2020) Obstructive sleep apnea and circulating biomarkers of oxidative stress: a cross-sectional study. Antioxidants 9(6):476
Zhou L, Ouyang R, Luo H, Peng Y, Chen P, Ren S, Liu G (2018) Dysfunction of Nrf2-ARE signaling pathway: potential pathogenesis in the development of neurocognitive impairment in patients with moderate to severe obstructive sleep apnea-hypopnea syndrome. Oxid Med Cell Longev 2018:3529709. https://doi.org/10.1155/2018/3529709
Campos-Rodriguez F, Asensio-Cruz MI, Cordero-Guevara J, Jurado-Gamez B, Carmona-Bernal C, Gonzalez-Martinez M, Troncoso MF, Sanchez-Lopez V, Arellano-Orden E, Garcia-Sanchez MI et al (2019) Effect of continuous positive airway pressure on inflammatory, antioxidant, and depression biomarkers in women with obstructive sleep apnea: a randomized controlled trial. Sleep. https://doi.org/10.1093/sleep/zsz145
Wang X, Wang Y, Cai Z, Lu X, Li Z, Chen Y, Zu G, Li T (2018) Alterations of IGF-1, complement C3 and superoxide dismutase in patients with moderate-to-severe obstructive sleep apnea hypopnea syndrome. Biomark Med 12(3):217–228. https://doi.org/10.2217/bmm-2017-0099
Eleutherio ECA, Magalhães RSS, de Araújo BA, Monteiro JRN, de Holanda PL (2021) SOD1, more than just an antioxidant. Arch Biochem Biophys 697:108701. https://doi.org/10.1016/j.abb.2020.108701
Zhou W, Li S, Wan N, Zhang Z, Guo R, Chen B (2012) Effects of various degrees of oxidative stress induced by intermittent hypoxia in rat myocardial tissues. Respirology 17(5):821–829. https://doi.org/10.1111/j.1440-1843.2012.02157.x
Atkeson A, Yeh SY, Malhotra A, Jelic S (2009) Endothelial function in obstructive sleep apnea. Prog Cardiovasc Dis 51(5):351–362. https://doi.org/10.1016/j.pcad.2008.08.002
Lee KH, Cha M, Lee BH (2020) Neuroprotective effect of antioxidants in the brain. Int J Mol Sci 21(19):7152
Torkanlou K, Bibak B, Abbaspour A, Abdi H, Saleh Moghaddam M, Tayefi M, Mohammadzadeh E, Bana HS, Aghasizade M, Ferns GA, Avan A, Ghayour MM (2016) Reduced serum levels of zinc and superoxide dismutase in obese individuals. Ann Nutr Metab 69(3–4):232–236. https://doi.org/10.1159/000454894
Strehlow K, Rotter S, Wassmann S, Adam O, Grohe C, Laufs K, Bohm M, Nickenig G (2003) Modulation of antioxidant enzyme expression and function by estrogen. Circ Res 93(2):170–177. https://doi.org/10.1161/01.RES.0000082334.17947.11
Acknowledgements
This work was supported by the Chinese National Natural Science Foundation (grant number: 81670080).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
As this is a meta-analysis, it did not involve any study on actual human or animal subjects. Hence, this review does not require approval of an ethics board.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tian, Z., Sun, H., Kang, J. et al. Association between the circulating superoxide dismutase and obstructive sleep apnea: a meta-analysis. Eur Arch Otorhinolaryngol 279, 1663–1673 (2022). https://doi.org/10.1007/s00405-021-07064-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-021-07064-1