Abstract
Background
Dysphagia can result from shock, trauma, aging, head and neck neoplasms, and some cerebrovascular diseases or neuromotor degenerative disorders. Swallowing rehabilitation therapy combined with postural control of the neck, head, and body can be effective for patients with dysphagia. Though the lateral decubitus posture has been a favorable option for swallowing rehabilitation therapy, available clinical data pertaining to it are scarce.
Methods
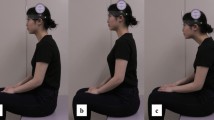
Twenty-seven healthy volunteers were enrolled in this study. The subjects underwent a repetitive saliva swallowing test, food swallowing test, and water swallowing test. The trials were performed in four different positions: upright sitting position, lateral decubitus position with the head raised to 60°, lateral decubitus position with the head raised to 30°, and complete lateral decubitus position. After each trial, the subjects were asked to declare the swallowing difficulty utilizing a visual analogue scale. Swallowing time and swallowing sound level were recorded simultaneously, as objective evaluation in each trial. We analyzed the visual analogue scale scores, swallowing time, and swallowing sound levels for all the four positions.
Results
The results of the visual analogue scale of the water swallowing test in the sitting position were significantly lower than those of the complete lateral decubitus position (p < 0.01). However, statistical significance was not detected in swallowing time or the swallowing sound level among the four different positions. Although subjective discomfort in swallowing was identified, difficulty of swallowing was not objectively evident in the trials, irrespective of the position.
Conclusions
A complete lateral decubitus position can be an effective and safe position in swallowing.





Similar content being viewed by others
Data availability
N/A
Code availability
N/A
References
Sura L, Madhavan A, Carnaby G, Crary MA (2012) Dysphagia in the elderly: management and nutritional considerations. Clin Interv Aging 7:287–298. https://doi.org/10.2147/CIA.S23404
Leslie P, Carding PN, Wilson JA (2003) Investigation and management of chronic dysphagia. BMJ 326:433–436. https://doi.org/10.1136/bmj.326.7386.433
Tibbling L, Gustafsson B (1991) Dysphagia and its consequences in the elderly. Dysphagia 6:200–202. https://doi.org/10.1007/BF02493526
Langmore SE, Terpenning MS, Schork A, Chen Y, Murray JT, Lopatin D, Loesche WJ (1998) Predictors of aspiration pneumonia: how important is dysphagia? Dysphagia 13:69–81. https://doi.org/10.1007/PL00009559
Sekizawa K, Matsui T, Nakagawa T, Nakayama K, Sasaki H (1998) ACE inhibitors and pneumonia. Lancet 352:1069. https://doi.org/10.1016/S0140-6736(05)60114-6
Ebihara T, Takahashi H, Ebihara S, Okazaki T, Sasaki T, Watando A, Nemoto M, Sasaki H (2005) Capsaicin troche for swallowing dysfunction in older people. J Am Geriatr Soc 53:824–828. https://doi.org/10.1111/j.1532-5415.2005.53261.x
Ohrui T (2005) Preventive strategies for aspiration pneumonia in elderly disabled persons. Tohoku J Exp Med 207:3–12. https://doi.org/10.1620/tjem.207.3
Solazzo A, Monaco L, Del Vecchio L, Tamburrini S, Iacobellis F, Berritto D, Pizza NL, Reginelli A, Di Martino N, Grassi R (2012) Investigation of compensatory postures with videofluoromanometry in dysphagia patients. World J Gastroenterol 18:2973–2978. https://doi.org/10.3748/wjg.v18.i23.2973
Tsukada T, Taniguchi H, Ootaki S, Yamada Y, Inoue M (2009) Effects of food texture and head posture on oropharyngeal swallowing. J Appl Physiol 106:1848–1857. https://doi.org/10.1152/japplphysiol.91295.2008
Park BH, Seo JH, Ko MH, Park SH (2013) Effect of 45 degrees reclining sitting posture on swallowing in patients with dysphagia. Yonsei Med J 54:1137–1142. https://doi.org/10.3349/ymj.2013.54.5.1137
Oh BM, Lee JH, Seo HG, Lee WH, Han TR, Jeong SU, Jeong HJ, Sim YJ (2018) Changes in hyolaryngeal movement during swallowing in the lateral decubitus posture. Ann Rehabil Med 42:416–424. https://doi.org/10.5535/arm.2018.42.3.416
Honda T, Baba T, Fujimoto K, Goto T, Nagao K, Harada M, Honda E, Ichikawa T (2016) Characterization of swallowing sound: preliminary investigation of normal subjects. PLoS ONE 11:e0168187. https://doi.org/10.1371/journal.pone.0168187
Persson E, Wårdh I, Östberg P (2019) Repetitive saliva swallowing test: norms, clinical relevance and the impact of saliva secretion. Dysphagia 34:271–278. https://doi.org/10.1007/s00455-018-9937-0
Oguchi K, Saitoh E, Mizuno M, Baba M, Okui M, Suzuki M (2000) The Repetitive Saliva Swallowing Test (RSST) as a screening test of functional dysphagia (1) normal values of RSST. Jpn J Rehabil Med 37:375–382 (In Japanese Abstract in English)
Oguchi K, Saitoh E, Baba M, Kusudo S, Tanaka T, Onogi K (2000) The Repetitive Saliva Swallowing Test (RSST) as a screening test of functional dysphagia (2) validity of RSST. Jpn J Rehabil Med 37:383–388 (In Japanese Abstract in English)
Tohara H, Saitoh E, Mays KA, Kuhlemeier K, Palmer JB (2003) Three tests for predicting aspiration without videofluorography. Dysphagia 18:126–134. https://doi.org/10.1007/s00455-002-0095-y
Taniwaki M, Gao Z, Nishinari K, Kohyama K (2013) Acoustic analysis of the swallowing sounds of food with different physical properties using the cervical auscultation method. J Texture Stud 44:169–175. https://doi.org/10.1111/jtxs.12009
Nakauma M, Ishihara S, Funami T, Nishinari K (2011) Swallowing profiles of food polysaccharide solutions with different flow behaviors. Food Hydrocoll 25:1165–1173. https://doi.org/10.1016/j.foodhyd.2010.11.003
Shinjo Y, Okitsu A, Ukeda I, Miyagi A, Domen K, Koyama T (2013) Effects of posture on subjective swallowing difficulty during screening tests for dysphagia. Int J Phys Med Rehabil 1:133. https://doi.org/10.4172/2329-9096.1000133
Morinière S, Boiron M, Alison D, Makris P, Beutter P (2008) Origin of the sound components during pharyngeal swallowing in normal subjects. Dysphagia 23:267–273. https://doi.org/10.1007/s00455-007-9134-z
Morinière S, Beutter P, Boiron M (2006) Sound component duration of healthy human pharyngoesophageal swallowing: a gender comparison study. Dysphagia 21:175–182. https://doi.org/10.1007/s00455-006-9023-x
Acknowledgements
We thank Drs. Masayuki Imamura, Takaya Majima, Takaharu Iida, and Hitoshi Nakagawa for their support of this study.
Funding
This study was financially supported by the Japan Society for the Promotion of Science (JSPS) KAKENHI, Grant Number JP 20K19260.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by MT, AG, and YM. The first draft of the manuscript was written by YM and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest concerning this study.
Ethical approval
The study protocol was approved by the Institutional Review Board of Hikari Hospital.
Informed consent
This research study involved human participants and all accepted principles of ethical and professional conduct have been followed.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Takagawa, M., Goda, A., Maki, Y. et al. Subjective and objective evaluation of swallowing in lateral decubitus positions examined in healthy volunteers. Eur Arch Otorhinolaryngol 279, 1071–1080 (2022). https://doi.org/10.1007/s00405-021-07001-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-021-07001-2