Abstract
Purpose
This clinical trial aimed to investigate the effects of different nasal packing methods and transseptal suture technique on swallowing after septoplasty.
Methods
This randomized prospective study consists of 180 consecutive patients with septal deviation. All the patients underwent septoplasty. All the patients were randomly assigned to three groups. In group A, transseptal sutures were used for septal stabilization. In group B, both nasal passages were packed with Merocel tampons for septal stabilization. In group C, both nasal passages were packed with Doyle silicone splints for septal stabilization. For the evaluation of swallowing, the Eating Assessment Tool (EAT-10) questionnaire and a visual analog scale (VAS) were administered to all the patients preoperatively and on the second and seventh postoperative days.
Results
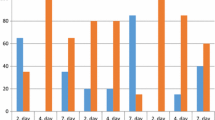
One hundred and twenty two of the patients (67.7%) were female and 58 of them (32.2%) were male. The mean age was 32.41 ± 12.37 years (range: 18–57 years). Both EAT-10 and VAS scores on the second postoperative day were significantly higher than the preoperative scores in all the groups (p < 0.05). The transseptal suture group had significantly lower EAT-10 and VAS scores on the second postoperative day than the Merocel packing and silicone packing groups (p < 0.05). Both EAT-10 and VAS scores on the postop 7th day significantly decreased in all groups compared to the postop second day (p < 0.05).
Conclusions
Septoplasty affects swallowing, regardless of whether a tampon is applied. Transeptal suturing has a lesser effect on swallowing than other techniques. Although silicone packing is a less invasive method, it negatively affects swallowing, similar to Merocel packing. The transseptal suture technique is more comfortable than the other techniques in terms of swallowing function in the postoperative period.


Similar content being viewed by others
References
Nunez DA, Martin FW (1991) An evaluation of post-operative packing in nasal septal surgery. Clin Otolaryngol Allied Sci 16:549–550. https://doi.org/10.1111/j.1365-2273.1991.tb00971.x
Weber R, Keerl R, Hochapfel F et al (2001) Packing in endonasal surgery. Am J Otolaryngol Head Neck Med Surg 22:306–320. https://doi.org/10.1053/ajot.2001.26499
Bernardo MT, Alves S, Lima NB et al (2013) Septoplasty with or without postoperative nasal packing? prospective study. Braz J Otorhinolaryngol 79:471–474. https://doi.org/10.5935/1808-8694.20130084
Günaydın RÖ, Aygenc E, Karakullukcu S et al (2011) Nasal packing and transseptal suturing techniques: surgical and anaesthetic perspectives. Eur Arch Oto-Rhino-Laryngol 268:1151–1156. https://doi.org/10.1007/s00405-011-1542-x
Logemann JA (1998) Evaluation and treatment of swallowing disorders, 2nd edn. Pro-Ed, Austin
Dodds WJ, Stewart ET, Logemann JA (1990) Physiology and radiology of the normal oral and pharyngeal phases of swallowing. Am J Roentgenol 154:953–963. https://doi.org/10.2214/ajr.154.5.2108569
Matsuo K, Palmer JB (2008) Anatomy and physiology of feeding and swallowing: normal and abnormal. Phys Med Rehabil Clin N Am 19:691–707. https://doi.org/10.1016/j.pmr.2008.06.001
Ayuse T, Hisamatsu N, Yamaguchi T et al (2020) Efficacy of nasal high flow therapy on the coordination between breathing and swallowing of saliva during daytime nap in chronic obstructive pulmonary disease patients: a single center, randomized crossover controlled study. Medicine (Baltimore) 99:e21778. https://doi.org/10.1097/MD.0000000000021778
Printza A, Triaridis S, Kalaitzi M et al (2020) Dysphagia prevalence, attitudes, and related quality of life in patients with multiple sclerosis. Dysphagia 35:677–684. https://doi.org/10.1007/s00455-019-10075-0
Pilz W, Passos VL, Verdonschot RJ et al (2020) Swallow-related quality of life and oropharyngeal dysphagia in myotonic dystrophy. Eur Arch Oto-Rhino-Laryngol 277:2357–2362. https://doi.org/10.1007/s00405-020-05964-2
Belafsky PC, Mouadeb DA, Rees CJ et al (2008) Validity and reliability of the eating assessment tool (EAT-10). Ann Otol Rhinol Laryngol 117:919–924. https://doi.org/10.1177/000348940811701210
Demir N, Serel Arslan S, İnal Ö, Karaduman AA (2016) Reliability and validity of the turkish eating assessment tool (T-EAT-10). Dysphagia 31:644–649. https://doi.org/10.1007/s00455-016-9723-9
Kumar L, Belaldavar BP, Bannur H (2017) Influence of deviated nasal septum on nasal epithelium: an analysis. Head Neck Pathol 11:501–505. https://doi.org/10.1007/s12105-017-0819-9
Most SP, Rudy SF (2017) Septoplasty: basic and advanced techniques. Facial Plast Surg Clin North Am 25:161–169. https://doi.org/10.1016/j.fsc.2016.12.002
Kayahan B, Ozer S, Suslu AE et al (2017) The comparison of the quality of life and intranasal edema between the patients with or without nasal packing after septoplasty. Eur Arch Oto-Rhino-Laryngol 274:1551–1555. https://doi.org/10.1007/s00405-016-4403-9
Özkiriş M, Kapusuz Z, Saydam L (2013) Comparison of nasal packs with transseptal suturing after nasal septal surgery. Am J Otolaryngol Head Neck Med Surg 34:308–311. https://doi.org/10.1016/j.amjoto.2012.12.012
Ekberg O, Hamdy S, Woisard V et al (2002) Social and psychological burden of dysphagia: its impact on diagnosis and treatment. Dysphagia 17:139–146. https://doi.org/10.1007/s00455-001-0113-5
McHorney CA, Earl Bricker D, Robbins J et al (2000) The SWAL-QOL outcomes tool for oropharyngeal dysphagia in adults: II Item reduction and preliminary scaling. Dysphagia 15:122–133. https://doi.org/10.1007/s004550010013
Hairston LE, Sauerland EK (1981) Electromyography of the human palate: discharge patterns of the levator and tensor Veli palatini. Electromyogr Clin Neurophysiol 21:287–297
Rodenstein DO, Stanescu DC (1984) Soft palate and oronasal breathing in humans. J Appl Physiol Respir Environ Exerc Physiol 57:651–657. https://doi.org/10.1152/jappl.1984.57.3.651
Ludlow CL (2015) Laryngeal reflexes: physiology, technique, and clinical use. J Clin Neurophysiol 32:284–293. https://doi.org/10.1097/WNP.0000000000000187
Selley WG, Flack FC, Ellis RE, Brooks WA (1989) Respiratory patterns associated with swallowing: Part 1. The normal adult pattern and changes with age. Age Ageing 18:168–172. https://doi.org/10.1093/ageing/18.3.168
Martin-Harris B, Brodsky MB, Price CC et al (2003) Temporal coordination of pharyngeal and laryngeal dynamics with breathing during swallowing: single liquid swallows. J Appl Physiol 94:1735–1743. https://doi.org/10.1152/japplphysiol.00806.2002
Matsuo K, Palmer JB (2009) Coordination of mastication, swallowing and breathing. Jpn Dent Sci Rev 45:31–40. https://doi.org/10.1016/j.jdsr.2009.03.004
Funding
The authors have no other funding financial relationships.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was approved by the local ethic committee (Okmeydanı training and research hospital) (No:1378).
Informed consent
The study design was a prospective randomized study and performed with human participants. Informed consent was obtained from all the participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sari, H., Atar, Y., Kumral, T.L. et al. Effects of nasal packing and transseptal suturing on swallowing after septoplasty. Eur Arch Otorhinolaryngol 279, 267–273 (2022). https://doi.org/10.1007/s00405-021-06854-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-021-06854-x