Abstract
Purpose
Although the association between necrotizing otitis externa (NOE) and diabetes mellitus (DM) is well known, there is little knowledge in regards to the effects of DM and glycemic control on the outcome of NOE. The aim of the study was to determine the effects of DM duration and glycemic control, and in-hospital glycemic control on NOE severity.
Methods
A retrospective case series analysis, including all patients hospitalized between 1990 and 2018 due to NOE were included. Data collected included NOE disease characteristics, duration of DM, DM-associated comorbidities, glycated hemoglobin (HbA1c), urine microalbumin and in-hospital blood glucose measurements. Disease severity was defined based on duration of hospitalization (above or below 20 days) and need for surgery.
Results
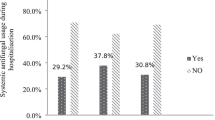
Eighty-nine patients were included in the study. Eighty-three patients (94.3%) had DM. Preadmission HbA1c was 8.13% (5.8–12.6%). Forty-nine patients (65.5%) had mean blood glucose of ≥ 140 mg/dL and 26 (34.5%) had ≤ 140 mg/dL. DM duration was 157.88 months among NOE patients who required surgery, and 127.6 months among patients who were treated conservatively (p value 0.25). HbA1c in patients hospitalized < 20 days was 7.6%, and 8.7% among NOE hospitalized ≥ 20 days (p value 0.027). Seven patients with mean blood glucose of ≤ 140 mg/dL had Pseudomonas Aeruginosa (PA-NOE) (26.7%), in comparison to 25 (51.0%) with mean blood glucose measurement of ≥ 140 mg/dL (p = 0.045).
Conclusions
HbA1c at admission is associated with longer hospitalization duration among NOE patients. Mean blood glucose during hospitalization was associated with a higher likelihood of PA infection, however, it had no effect on disease outcome.
Similar content being viewed by others
References
Berenholz L, Katzenell U, Harell M (2002) Evolving resistant pseudomonas to ciprofloxacin in malignant otitis externa. Laryngoscope 112(9):1619–1622. https://doi.org/10.1097/00005537-200209000-00017
Mani N, Sudhoff H, Rajagopal S, Moffat D, Axon PR (2007) Cranial nerve involvement in malignant external otitis: implications for clinical outcome. Laryngoscope 117(5):907–910. https://doi.org/10.1097/MLG.0b013e318039b30f
Peled C, El-Seid S, Bahat-Dinur A et al (2019) Necrotizing otitis externa-analysis of 83 cases: clinical findings and course of disease. Otol Neurotol 40(1):56–62. https://doi.org/10.1097/MAO.0000000000001986
Mahdyoun P, Pulcini C, Gahide I et al (2013) Necrotizing otitis externa: a systematic review. Otol Neurotol 34(4):620–629. https://doi.org/10.1097/MAO.0b013e3182804aee
Hollis S, Evans K (2011) Management of malignant (necrotising) otitis externa. J Laryngol Otol 125(12):1212–1217. https://doi.org/10.1017/S0022215110002550
Joshua BZ, Sulkes J, Raveh E, Bishara J, Nageris BI (2008) Predicting outcome of malignant external otitis. Otol Neurotol 29(3):339–343. https://doi.org/10.1097/MAO.0b013e3181661879
Loh S, Loh WS (2013) Malignant otitis externa: an Asian perspective on treatment outcomes and prognostic factors. Otolaryngol Head Neck Surg 148(6):991–996. https://doi.org/10.1177/0194599813482107
Franco-Vidal V, Blanchet H, Bebear C, Dutronc H, Darrouzet V (2007) Necrotizing external otitis: a report of 46 cases. Otol Neurotol 28(6):771–773. https://doi.org/10.1097/MAO.0b013e31805153bd
Cohen D, Friedman P (1987) The diagnostic criteria of malignant external otitis. J Laryngol Otol 101(3):216–221. https://doi.org/10.1017/s0022215100101562
American Diabetes Association (2019) Diabetes care in the hospital: standards of medical care in diabetes-2019. Diabetes Care 42(Suppl 1):S173–S181. https://doi.org/10.2337/dc19-S015
Peled C, Kraus M, Kaplan D (2018) Diagnosis and treatment of necrotising otitis externa and diabetic foot osteomyelitis—similarities and differences. J Laryngol Otol 132(9):775–779. https://doi.org/10.1017/S002221511800138X
Stern Shavit S, Soudry E, Hamzany Y, Nageris B (2016) Malignant external otitis: factors predicting patient outcomes. Am J Otolaryngol 37(5):425–430. https://doi.org/10.1016/j.amjoto.2016.04.005
Lee SK, Lee SA, Seon SW et al (2017) Analysis of prognostic factors in malignant external otitis. Clin Exp Otorhinolaryngol 10(3):228–235. https://doi.org/10.21053/ceo.2016.00612
Carfrae MJ, Kesser BW (2008) Malignant otitis externa. Otolaryngol Clin N Am 41(3):537–ix. https://doi.org/10.1016/j.otc.2008.01.004
Chen CN, Chen YS, Yeh TH, Hsu CJ, Tseng FY (2010) Outcomes of malignant external otitis: survival vs mortality. Acta Otolaryngol 130(1):89–94. https://doi.org/10.3109/00016480902971247
Naghibi M, Smith RP, Baltch AL et al (1987) The effect of diabetes mellitus on chemotactic and bactericidal activity of human polymorphonuclear leukocytes. Diabetes Res Clin Pract 4(1):27–35. https://doi.org/10.1016/s0168-8227(87)80030-x
Geerlings SE, Hoepelman AI (1999) Immune dysfunction in patients with diabetes mellitus (DM). FEMS Immunol Med Microbiol 26(3–4):259–265. https://doi.org/10.1111/j.1574-695X.1999.tb01397.x
Acknowledgements
No sources of support require acknowledgment and no funding were received for this work from any organization.
Author information
Authors and Affiliations
Contributions
PC: research design, data analysis, and writing. SR: statistical analysis. E-SS: data analysis and writing. NV: statistical analysis. KMD: data analysis and writing.
Corresponding author
Ethics declarations
Conflict of interest
The author declares no potential conflict of interest.
Availability of data and material
All data are presented in the presented article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Peled, C., Sadeh, R., El-Saied, S. et al. Diabetes and glycemic control in necrotizing otitis externa (NOE). Eur Arch Otorhinolaryngol 279, 1269–1275 (2022). https://doi.org/10.1007/s00405-021-06772-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-021-06772-y