Abstract
Purpose
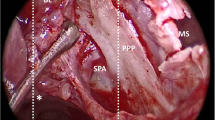
The main objective was to perform an image-guided (CT) assessment of the efficacy of the CAVI-T™ balloon to compress the sphenopalatine artery (SPA) on cadaver heads, for the management of epistaxis. The secondary objectives were to analyse the deployment and stability of this balloon according to the volume injected into the nasal cavity, to optimise its use.
Methods
A descriptive anatomical study was performed. The catheterization of the SPA was performed on four fresh-frozen heads with a SPA approach through the maxillary sinus, leaving the nasal cavity unscathed. Computed Tomography images were acquired without and with the balloon, inflated by injections of progressive volumes of diluted iodine, for optimal contrast with the surrounding tissues. We evaluated the positioning of the balloon according to two predetermined markers on the device.
Results
Out of 68 image-guided acquisitions, the CAVI-T™ balloon compressed the SPA in 88% of cases. The other nasal cavity structures were compressed in 86% to 100% of the cases, depending on the positioning of the CAVI-T™ balloon, therefore allowing a complete obstruction of the nasal cavity. The device remained stable upon inflation and did not obstruct the nasopharynx.
Conclusion
The CAVI-T™ balloon provided effective compression of the SPA and the different structures of the nasal cavity.




Similar content being viewed by others
References
Nikolaou G, Holzmann D, Soyka MB (2013) Discomfort and costs in epistaxis treatment. Eur Arch Oto-Rhino-Laryngol Off J Eur Fed Oto-Rhino-Laryngol Soc EUFOS Affil Ger Soc Oto-Rhino-Laryngol - Head Neck Surg 270(8):2239–2244. https://doi.org/10.1007/s00405-012-2339-2
Petruson B, Rudin R (1975) The frequency of epistaxis in a male population sample. Rhinology 13(3):129–133
Smith J, Siddiq S, Dyer C, Rainsbury J, Kim D (2011) Epistaxis in patients taking oral anticoagulant and antiplatelet medication: prospective cohort study. J Laryngol Otol 125(1):38–42. https://doi.org/10.1017/S0022215110001921
Purkey MR, Seeskin Z, Chandra R (2014) Seasonal variation and predictors of epistaxis. Laryngoscope 124(9):2028–2033. https://doi.org/10.1002/lary.24679
Bequignon E, Vérillaud B, Robard L et al (2017) Guidelines of the French Society of Otorhinolaryngology (SFORL). First-line treatment of epistaxis in adults. Eur Ann Otorhinolaryngol Head Neck Dis 134(3):185–189. https://doi.org/10.1016/j.anorl.2016.09.008
de Bonnecaze G, Gallois Y, Chaynes P et al (2017) Intractable epistaxis: which arteries are responsible? An angiographic study. Surg Radiol Anat SRA 39(11):1203–1207. https://doi.org/10.1007/s00276-017-1856-5
Douglas R, Wormald P-J (2007) Update on epistaxis. Curr Opin Otolaryngol Head Neck Surg 15(3):180–183. https://doi.org/10.1097/MOO.0b013e32814b06ed
Tunkel DE, Anne S, Payne SC, et al (2020) Clinical Practice Guideline: Nosebleed (Epistaxis). Otolaryngol--Head Neck Surg Off J Am Acad Otolaryngol-Head Neck Surg 162(1_suppl):S1–S38. https://doi.org/10.1177/0194599819890327
Hopkins C, Browne JP, Slack R et al (2006) Complications of surgery for nasal polyposis and chronic rhinosinusitis: the results of a national audit in England and Wales. Laryngoscope 116(8):1494–1499. https://doi.org/10.1097/01.mlg.0000230399.24306.50
Krulewitz NA, Fix ML (2019) Epistaxis. Emerg Med Clin North Am 37(1):29–39. https://doi.org/10.1016/j.emc.2018.09.005
Debry C, Fath L, Nakhleh L et al (2020) Pilot clinical trial of an asymmetrical balloon in the treatment of epistaxis in adult patients. Rhinol Online 3:89–99
Viducich RA, Blanda MP, Gerson LW (1995) Posterior epistaxis: clinical features and acute complications. Ann Emerg Med 25(5):592–596. https://doi.org/10.1016/s0196-0644(95)70169-9
Strach K, Schröck A, Wilhelm K et al (2011) Endovascular treatment of epistaxis: indications, management, and outcome. Cardiovasc Intervent Radiol 34(6):1190–1198. https://doi.org/10.1007/s00270-011-0155-5
Cohen JE, Moscovici S, Gomori JM, Eliashar R, Weinberger J, Itshayek E (2012) Selective endovascular embolization for refractory idiopathic epistaxis is a safe and effective therapeutic option: technique, complications, and outcomes. J Clin Neurosci Off J Neurosurg Soc Australas 19(5):687–690. https://doi.org/10.1016/j.jocn.2011.08.019
Holzmann D, Kaufmann T, Pedrini P, Valavanis A (2003) Posterior epistaxis: endonasal exposure and occlusion of the branches of the sphenopalatine artery. Eur Arch Oto-Rhino-Laryngol Off J Eur Fed Oto-Rhino-Laryngol Soc EUFOS Affil Ger Soc Oto-Rhino-Laryngol - Head Neck Surg 260(8):425–428. https://doi.org/10.1007/s00405-003-0618-7
de Bonnecaze G, Gallois Y, Bonneville F, Vergez S, Chaput B, Serrano E (2018) Transnasal endoscopic sphenopalatine artery ligation compared with embolization for intractable epistaxis: a long-term analysis. Am J Rhinol Allergy 32(3):188–193. https://doi.org/10.1177/1945892418768584
Snyderman CH, Goldman SA, Carrau RL, Ferguson BJ, Grandis JR (1999) Endoscopic sphenopalatine artery ligation is an effective method of treatment for posterior epistaxis. Am J Rhinol 13(2):137–140. https://doi.org/10.2500/105065899782106805
Wareing MJ, Padgham ND (1998) Osteologic classification of the sphenopalatine foramen. Laryngoscope 108(1 Pt 1):125–127. https://doi.org/10.1097/00005537-199801000-00024
McGarry GW, Aitken D (1991) Intranasal balloon catheters: how do they work? Clin Otolaryngol Allied Sci 16(4):388–392. https://doi.org/10.1111/j.1365-2273.1991.tb00955.x
Jiang Y, Acquadro MA (2004) Upper airway obstruction caused by a double-cuffed nasal balloon after extubation. J Clin Anesth 16(4):301–304. https://doi.org/10.1016/j.jclinane.2003.09.010
Lau BW, Paspaliaris A (2018) RapidRhino herniation causing airway obstruction. Am J Emerg Med 36(7):1322.e3-1322.e4. https://doi.org/10.1016/j.ajem.2018.03.072
Badran K, Malik TH, Belloso A, Timms MS (2005) Randomized controlled trial comparing Merocel and RapidRhino packing in the management of anterior epistaxis. Clin Otolaryngol Off J ENT-UK Off J Neth Soc Oto-Rhino-Laryngol Cervico-Facial Surg 30(4):333–337. https://doi.org/10.1111/j.1365-2273.2005.01019.x
Iqbal IZ, Jones GH, Dawe N et al (2017) Intranasal packs and haemostatic agents for the management of adult epistaxis: systematic review. J Laryngol Otol 131(12):1065–1092. https://doi.org/10.1017/S0022215117002055
Loftus PA, Wise SK, Nieto D, Panella N, Aiken A, DelGaudio JM. (2016) Intranasal volume increases with age: Computed tomography volumetric analysis in adults. The Laryngoscope 126(10):2212-2215. https://doi.org/10.1002/lary.26064
Turhan B, Kervancioglu P, Yalcin ED (2019) The radiological evaluation of the nasal cavity, conchae and nasal septum volumes by stereological method: A retrospective cone-beam computed tomography study. Adv Clin Exp Med Off Organ Wroclaw Med Univ 28(8):1021–1026. https://doi.org/10.17219/acem/98960
Kim YS, Kim YH, Kim NH, Kim SH, Kim KR, Kim K-S (2011) A prospective, randomized, single-blinded controlled trial on biodegradable synthetic polyurethane foam as a packing material after septoplasty. Am J Rhinol Allergy 25(2):e77-79. https://doi.org/10.2500/ajra.2011.25.3600
Acknowledgements
This work benefited from State aid managed by the French National Research Agency (ANR) under the “investissements d’avenir” program with the reference ANR-10-IAHU-02.
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Contributions
G. Trau, A. Venkatasamy: conduct, analysis and presentation. I. Djennaoui, M. Renaud, L. Fath: conduct and analysis. S. Ciftci: conduct and presentation.
Corresponding author
Ethics declarations
Conflict of interests
No conflicts of interest or financial relationships to disclose.
Ethics approval
The ethical committee of the Strasbourg University Hospital and Faculty of Medicine confirms that the work entitled « An image-guided (CT) assessment of a new asymmetric balloon for the treatment of epistaxis» has been performed in accordance with the ethical and reglementary rules applied to studies on anatomical pieces.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Trau, G., Venkatasamy, A., Djennaoui, I. et al. An image-guided (CT) assessment of a new asymmetric balloon for the treatment of epistaxis. Eur Arch Otorhinolaryngol 278, 4823–4830 (2021). https://doi.org/10.1007/s00405-021-06758-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-021-06758-w