Abstract
Purpose
The aim of this study was to test a mucosal release method for decreasing the occurrence of malodourous smells after septorhinoplasty by preventing formation of debris pockets after surgery.
Methods
This study included 50 adult patients from 18 to 45 years of age who underwent open septorhinoplasty from January to May 2019. Patients were divided into two groups. The first group had intradomal (transdomal) sutures without submucosal release, while the second group had mucosal release. All patients had scheduled post-op visits at 1, 2, 4, and 8 weeks and 6 months.
Results
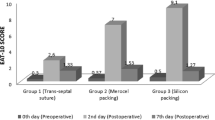
The overall postoperative rate of malodorous smell in both mucosal release and non-mucosal release patients at 2 weeks, 8 weeks and 6 months was 43.1%, 31.4% and 5.9%, respectively. Patients 36–45 years of age had a higher rate of postoperative malodorous smell with 55.6% at 2 weeks, decreasing to 33.3% at 8 weeks, and to less than 1% at 6 months. At 2 weeks after surgery, only 20% of the mucosal release group reported a malodorous smell compared to 65.4% in the non-mucosal release group. The rate was 8% at 8 weeks, and less than 1% at 6 months in the mucosal release group compared to 53.8% at 8 weeks and 11.5% at 6 months in the non-mucosal release group.
Conclusions
Utilizing absorbable polydioxanone sutures and releasing the vestibular mucosa of the LLC significantly reduced the rate of postoperative malodorous smell for septorhinoplasty patients with intradomal (transdomal) single-dome suturing.




Similar content being viewed by others
References
Deems DA, Doty RL, Settle RG et al (1991) Smell and taste disorders, a study of 750 patients from the University of Pennsylvania smell and taste center. Arch Otolaryngol Head Neck Surg 117:519–528
Türk B, Akpinar M, Altundağ A, Özkahraman Kirik M, Ünsal O, Uslu Coşkun B (2017) The effect of external approach septoplasty on olfactory function. J Craniofac Surg 28:1675–1678
Oka H, Tsuzuki K, Takebayashi H et al (2013) Olfactory changes after endoscopic sinus surgery in patients with chronic rhinosinusitis. Auris Nasus Larynx 40:452–457
Alobid I, Haro J, Mullol J (2010) Smell disorders. In: Anniko M, Bernal- Sprekelsen M, Bonkowsky V, Bradley P, Iurato S (eds) Otorhinolaryngology, Head & Neck Surgery. Springer-Verlag, Berlin, pp 287–290
Estrem SA, Renner G (1987) Disorders of smell and taste. Otolaryngol Clinics N Am 20:133–147
Golding-Wood DG, Holmstrom M, Scadding GK et al (1996) The treatment of hyposmia with intranasal steroids. J Laryngol Otol 110:132–135
Seiden AM, Duncan J (2001) The diagnosis of a conductive olfactory loss. Laryngoscope 111:9–14
Champion R (1966) Anosmia associated with corrective rhinoplasty. Br J Plast Surg 19:182–185
Fokkens W, Lund V, Bachert C et al (2005) EAACI position paper on rhinosinusitis and nasal polyps executive summary. Allergy 60:583–601
Shemshadi H, Azimian M, Onsori MA, Azizabadi Farahani M (2008) Olfactory function following open rhinoplasty: a 6-month follow-up study. BMC Ear Nose Throat Disord 8:6
Razmpa E, Saedi B, Safavi A, Mohammadi S (2013) Olfactory function after nasal plastic surgery. B-ENT 9:269–275
Briner HR, Simmen D, Jones N (2003) Impaired sense of smell in patients with nasal surgery. Clin Otolaryngol & Allied Sci 28:417–419. https://doi.org/10.1046/j.1365-2273.2003.00735.x
Kimmelman CP (1994) The risk of olfaction from nasal surgery. Laryngoscope 104:981–988
Pade J, Hummel T (2008) Olfactory function following nasal surgery. Laryngoscope 118:1260–1264. https://doi.org/10.1097/MLG.0b013e318170b5cb
Pfaar O, Huttenbrink KB, Hummel T (2004) Assessment of olfactory function after septoplasty: a longitudinal study. Rhinology 42:195–199
Philpott CM, Rimal D, Tassone P et al (2008) A study of olfactory testing in patients with rhinological pathology in the ENT clinic. Rhinology 46:34–39
Poirrier AL, Ahluwalia S, Goodson A et al (2013) Is the sino-nasal outcome test-22 a suitable evaluation for septorhinoplasty? Laryngoscope 123:76–81. https://doi.org/10.1002/lary.23615
Niechajev I (2015) Comparison of various rhinoplasty techniques and long-term results. Aesthet Plast Surg 39:474–477. https://doi.org/10.1007/s00266-015-0506-8
Schriever VA, Gupta N, Pade J et al (2013) Olfactory function following nasal surgery: a one-year follow-up. Eur Arch Otorhinolaryngol 270:107–111. https://doi.org/10.1007/s00405-012-1972-0
Erdogan M, Cingi C, Seren E et al (2013) Evaluation of nasal airway alterations associated with septorhinoplasty by both objective and subjective methods. Eur Arch Otorhinolaryngol 270:99–106. https://doi.org/10.1007/s00405-012-1974-y
Vuyk HD (1995) Suture tip plasty. Rhinology 33:30–38
Nedev PK (2009) Cranio-caudal transdomal sutures for the nasal tip correction. Eur Arch Otorhinolaryngol 266:237–242. https://doi.org/10.1007/s00405-008-0758-x
Goldman IB (1954) Surgical tips on the nasal tip. Eye Ear Nose Throat Mon 33:583–591
Daniel RK (1993) The nasal tip. In: Daniel RK (ed) Aesthetic plastic surgery: Rhinoplasty, 2nd edn. Little, Brown and Company, Boston
Gruber RP, Weintraub J, Pomerantz J (2008) Suture techniques for the nasal tip. Aesthetic Surg J 28:92–100
Polydioxanone sutures. Surgical suture information. DemeTECH Corporation. https://www.demetech.us/polydioxanonesuture.php. Accessed 25 June 2015.
Acknowledgements
The authors would like to thank the members of the research team who participated in the study. Special thanks to the Otorhinolaryngology Department at King Abdulaziz Medical City and the Medical Education Department at King Saud bin Abdulaziz University for Health Sciences for their technical support.
Funding
This research did not receive any specific grants from public, commercial, or non-profit funding agencies.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
This paper was reviewed and ethically approved by King Abdullah International Medical Research Center, Riyadh, Saudi Arabia.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 9792 kb)
Rights and permissions
About this article
Cite this article
Alghonaim, Y., Arafat, A.S. & Alobaid, F. Postoperative malodorous smell in open septorhinoplasty: the effect of intradomal suturing with mucosal release. Eur Arch Otorhinolaryngol 278, 703–709 (2021). https://doi.org/10.1007/s00405-020-06307-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-020-06307-x