Abstract
Purpose
Skeletal muscle mass (SMM) depletion and sarcopenia as predictors of postoperative complications and poorer overall survival (OS) have been validated in many surgical fields through cross-sectional imaging (CT, MRI), with potential limitations. We evaluated it in a stage III–IV head and neck squamous cell carcinoma (HNSCC) surgical cohort through ultrasound (US) of rectus femoris muscle (RF), a quick, cheap, repeatable alternative.
Methods
Patients submitted to surgical treatment with curative purpose were recruited and prospectively evaluated through clinical, biometric, biochemical, surgical, pathological and functional prognosticators and with preoperative US of RF with regards to 30-day complications and OS.
Results
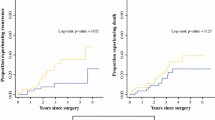
Forty-seven patients completed the study. RF cross-sectional area (RF-CSA) was used to identify patients with low SMM (CSA ≤ 0.97 cm2: 18/47, 38.3%). RF-CSA was lower in complicated cases (0.95 ± 0.48 vs 1.41 ± 0.49 cm2; p = 0.003), remaining the only independent predictor of postoperative complications at multivariate analysis, with a model including ASA score and modified Frailty index (OR 9.84; p = 0.004). SMM depletion significantly impaired OS (13.6 ± 2.9 vs 26.3 ± 2.1 months; p = 0.017), being its only independent prognosticator at multivariate Cox regression analysis (OR 4.42; p = 0.033).
Conclusion
RF-CSA, evaluated with US, seems a reliable method for identification of patients with low SMM in a stage III–IV HNSCC cohort, defining a subset at high-risk of 30-day complications and poorer OS.




Similar content being viewed by others
References
Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A (2015) Global cancer statistics, 2012. CA 65(2):87–108
Marur S, Forastiere AA (2008) Head and neck cancer: changing epidemiology, diagnosis, and treatment. Mayo Clin Proc 83(4):489–501
Piccirillo JF, Lacy PD, Basu A, Spitznagel EL (2002) Development of a new head and neck cancer-specific comorbidity index. Arch Otolaryngol Head Neck Surg 128(10):1172–1179
Piccirillo JF, Tierney RM, Costas I, Grove L, Spitznagel EL Jr (2004) Prognostic importance of comorbidity in a hospital-based cancer registry. JAMA 291(20):2441–2447
Ferrier MB, Spuesens EB, Le Cessie S, Baatenburg de Jong RJ (2005) Comorbidity as a major risk factor for mortality and complications in head and neck surgery. Arch Otolaryngol Head Neck Surg 131(1):27–32
Eley KA, Shah R, Bond SE, Watt-Smith SR (2012) A review of post-operative feeding in patients undergoing resection and reconstruction for oral malignancy and presentation of a pre-operative scoring system. Br J Oral Maxillofac Surg 50(7):601–605
Hall SF, Rochon PA, Streiner DL, Paszat LF, Groome PA, Rohland SL (2002) Measuring comorbidity in patients with head and neck cancer. Laryngoscope 112(11):1988–1996
Friedlander AH, Tajima T, Kawakami KT, Wang MB, Tomlinson J (2008) The relationship between measures of nutritional status and masticatory function in untreated patients with head and neck cancer. J Oral Maxillofac Surg 66(1):85–92
Alshadwi A, Nadershah M, Carlson ER, Young LS, Burke PA, Daley BJ (2013) Nutritional considerations for head and neck cancer patients: a review of the literature. J Oral Maxillofac Surg 71(11):1853–1860
Rosenberg IH (1997) Sarcopenia: origins and clinical relevance. J Nutr 127(5 Suppl):990S–991S
Marzetti E, Calvani R, Tosato M, Cesari M, Di Bari M, Cherubini A et al (2017) Sarcopenia: an overview. Aging Clin Exp Res 29(1):11–17
Grimby G, Saltin B (1983) The ageing muscle. Clin Physiol 3(3):209–218
Cruz-Jentoft AJ, Landi F, Schneider SM, Zuniga C, Arai H, Boirie Y et al (2014) Prevalence of and interventions for sarcopenia in ageing adults: a systematic review. Report of the international sarcopenia initiative (EWGSOP and IWGS). Age Ageing 43(6):748–759
Landi F, Liperoti R, Fusco D, Mastropaolo S, Quattrociocchi D, Proia A et al (2012) Sarcopenia and mortality among older nursing home residents. J Am Med Dir Assoc 13(2):121–126
Ida S, Watanabe M, Yoshida N, Baba Y, Umezaki N, Harada K et al (2015) Sarcopenia is a predictor of postoperative respiratory complications in patients with esophageal cancer. Ann Surg Oncol 22(13):4432–4437
Huang DD, Wang SL, Zhuang CL, Zheng BS, Lu JX, Chen FF et al (2015) Sarcopenia, as defined by low muscle mass, strength and physical performance, predicts complications after surgery for colorectal cancer. Colorectal Dis 17(11):O256–O264
Wang SL, Zhuang CL, Huang DD, Pang WY, Lou N, Chen FF et al (2016) Sarcopenia adversely impacts postoperative clinical outcomes following gastrectomy in patients with gastric cancer: a prospective study. Ann Surg Oncol 23(2):556–564
Pecorelli N, Carrara G, De Cobelli F, Cristel G, Damascelli A, Balzano G et al (2016) Effect of sarcopenia and visceral obesity on mortality and pancreatic fistula following pancreatic cancer surgery. Br J Surg 103(4):434–442
Carrara G, Pecorelli N, De Cobelli F, Cristel G, Damascelli A, Beretta L et al (2017) Preoperative sarcopenia determinants in pancreatic cancer patients. Clin Nutr 36(6):1649–1653
Harimoto N, Shirabe K, Yamashita YI, Ikegami T, Yoshizumi T, Soejima Y et al (2013) Sarcopenia as a predictor of prognosis in patients following hepatectomy for hepatocellular carcinoma. Br J Surg 100(11):1523–1530
Zhou G, Bao H, Zeng Q, Hu W, Zhang Q (2015) Sarcopenia as a prognostic factor in hepatolithiasis-associated intrahepatic cholangiocarcinoma patients following hepatectomy: a retrospective study. Int J Clin Exp Med 8(10):18245–18254
van Vugt JL, Braam HJ, van Oudheusden TR, Vestering A, Bollen TL, Wiezer MJ et al (2015) Skeletal muscle depletion is associated with severe postoperative complications in patients undergoing cytoreductive surgery with hyperthermic intraperitoneal chemotherapy for peritoneal carcinomatosis of colorectal cancer. Ann Surg Oncol 22(11):3625–3631
Achim V, Bash J, Mowery A, Guimaraes AR, Li R, Schindler J et al (2017) Prognostic indication of sarcopenia for wound complication after total laryngectomy. JAMA Otolaryngol Head Neck Surg 143(12):1159–1165
Bozkurt G, Elhassan HA, Mahmutoglu AS, Celebi I, McLeod RWJ, Soytas P et al (2018) Neck muscle mass index as a predictor of post-laryngectomy wound complications. Ann Otol Rhinol Laryngol 127(11):841–847
Bril SI, Pezier TF, Tijink BM, Janssen LM, Braunius WW, de Bree R (2019) Preoperative low skeletal muscle mass as a risk factor for pharyngocutaneous fistula and decreased overall survival in patients undergoing total laryngectomy. Head Neck 41(6):1745–1755
Chargi N, Bril SI, Emmelot-Vonk MH, de Bree R (2019) Sarcopenia is a prognostic factor for overall survival in elderly patients with head-and-neck cancer. Eur Arch Otorhinolaryngol 276(5):1475–1486
Fattouh M, Chang GY, Ow TJ, Shifteh K, Rosenblatt G, Patel VM et al (2019) Association between pretreatment obesity, sarcopenia, and survival in patients with head and neck cancer. Head Neck 41(3):707–714
Jung AR, Roh JL, Kim JS, Kim SB, Choi SH, Nam SY et al (2019) Prognostic value of body composition on recurrence and survival of advanced-stage head and neck cancer. Eur J Cancer 116:98–106
Nishikawa D, Hanai N, Suzuki H, Koide Y, Beppu S, Hasegawa Y (2018) The impact of skeletal muscle depletion on head and neck squamous cell carcinoma. ORL J Otorhinolaryngol Relat Spec 80(1):1–9
Stone L, Olson B, Mowery A, Krasnow S, Jiang A, Li R et al (2019) Association between sarcopenia and mortality in patients undergoing surgical excision of head and neck cancer. JAMA Otolaryngol Head Neck Surg 145(7):647–654
Stringer HJ, Wilson D (2018) The role of ultrasound as a diagnostic tool for sarcopenia. J Frailty Aging 7(4):258–261
Nijholt W, Scafoglieri A, Jager-Wittenaar H, Hobbelen JSM, van der Schans CP (2017) The reliability and validity of ultrasound to quantify muscles in older adults: a systematic review. J Cachexia Sarcopenia Muscle 8(5):702–712
Mueller N, Murthy S, Tainter CR, Lee J, Riddell K, Fintelmann FJ et al (2016) Can sarcopenia quantified by ultrasound of the rectus femoris muscle predict adverse outcome of surgical intensive care unit patients as well as frailty? A prospective, observational cohort study. Ann Surg 264(6):1116–1124
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD et al (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250(2):187–196
Arends J, Bachmann P, Baracos V, Barthelemy N, Bertz H, Bozzetti F et al (2017) ESPEN guidelines on nutrition in cancer patients. Clin Nutr 36(1):11–48
O'Neill JP, Shaha AR (2011) Nutrition management of patients with malignancies of the head and neck. Surg Clin N Am 91(3):631–639
Beeken L, Calman F (1994) A return to “normal eating” after curative treatment for oral cancer. What are the long-term prospects? Eur J Cancer B Oral Oncol 30B(6):387–392
Beaver ME, Matheny KE, Roberts DB, Myers JN (2001) Predictors of weight loss during radiation therapy. Otolaryngol Head Neck Surg 125(6):645–648
Boyle JO, Gumus ZH, Kacker A, Choksi VL, Bocker JM, Zhou XK et al (2010) Effects of cigarette smoke on the human oral mucosal transcriptome. Cancer Prev Res (Phila) 3(3):266–278
Ravasco P, Monteiro-Grillo I, Vidal PM, Camilo ME (2003) Nutritional deterioration in cancer: the role of disease and diet. Clin Oncol (R Coll Radiol) 15(8):443–450
Mick R, Vokes EE, Weichselbaum RR, Panje WR (1991) Prognostic factors in advanced head and neck cancer patients undergoing multimodality therapy. Otolaryngol Head Neck Surg 105(1):62–73
Swartz JE, Pothen AJ, Wegner I, Smid EJ, Swart KM, de Bree R et al (2016) Feasibility of using head and neck CT imaging to assess skeletal muscle mass in head and neck cancer patients. Oral Oncol 62:28–33
Prado CM, Lieffers JR, McCargar LJ, Reiman T, Sawyer MB, Martin L et al (2008) Prevalence and clinical implications of sarcopenic obesity in patients with solid tumours of the respiratory and gastrointestinal tracts: a population-based study. Lancet Oncol 9(7):629–635
Wendrich AW, Swartz JE, Bril SI, Wegner I, de Graeff A, Smid EJ et al (2017) Low skeletal muscle mass is a predictive factor for chemotherapy dose-limiting toxicity in patients with locally advanced head and neck cancer. Oral Oncol 71:26–33
Cruz-Jentoft AJ, Baeyens JP, Bauer JM, Boirie Y, Cederholm T, Landi F et al (2010) Sarcopenia: European consensus on definition and diagnosis: report of the European Working Group on sarcopenia in older people. Age Ageing 39(4):412–423
Funding
We have not received any form of financial support for the present work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors has potential conflict of interest to disclose.
Research involving human participants and/or animals
All performed procedures and retrospective data management were in accordance with the ethical standards of our institutional and national research ethical committee and with the principles stated in the Declaration of Helsinki “Ethical Principles for Medical Research Involving ‘Human Subjects”, adopted by the 18th World Medical Assembly (Helsinki, Finland, June 1964), and as amended most recently by the 64th World Medical Assembly (Fortaleza, Brazil, October 2013).
Informed consent
Informed consent for retrospective data management was obtained for all subjects.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Galli, A., Colombo, M., Carrara, G. et al. Low skeletal muscle mass as predictor of postoperative complications and decreased overall survival in locally advanced head and neck squamous cell carcinoma: the role of ultrasound of rectus femoris muscle. Eur Arch Otorhinolaryngol 277, 3489–3502 (2020). https://doi.org/10.1007/s00405-020-06123-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-020-06123-3