Abstract
Purpose
Oral potentially malignant disorders (OPMDs) may have varying degrees of oral epithelial dysplasia (OED). Traditional grading schemes separate OED into three-tiers (mild, moderate, and severe). Alternatively, a binary grading system has been previously proposed that stratifies OED into low-risk and high-risk categories based on a quantitative threshold of dysplastic pathologic characteristics. This systematic review evaluates the predictive value of a binary OED grading system and examines agreement between pathologists.
Methods
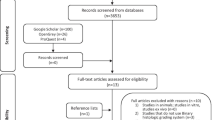
This meta-analysis queried 4 databases (PubMed, Ovid-MEDLINE, Cochrane, and SCOPUS) and includes 4 studies evaluating binary OED grading systems. Meta-analysis of proportions and correlations was performed to pool malignant transformation rates (MTR), risk of malignant transformation between OED categories, and measures of interobserver agreement.
Results
Pooled analysis of 629 lesions from 4 different studies found a six-time increased odds of malignant transformation in high-risk lesions over low-risk lesions [odds ratio (OR) 6.14, 95% 1.18–15.38]. Reported ORs ranged from 2.8 to 22.4. The overall MTR was 26.8%, with the high-risk and low-risk lesions having MTRs of 57.9% (95% CI 0.386–0.723) and 12.7% (95% CI − 0.210 to 0.438), respectively. Pooled unweighted interobserver kappa values for the binary grading system and three-tiered system were 0.693 (95% CI 0.640–0.740) and 0.388 (95% CI 0.195–0.552), respectively.
Conclusion
Binary grading of OED into low-risk and high-risk categories may effectively determine malignant potential, with improved interobserver agreement over three-tiered grading. Improved grading schemes of OED may help guide management (watchful waiting vs. excision) of these OPMDs.



Similar content being viewed by others
References
Chi AC, Day TA, Neville BW (2015) Oral cavity and oropharyngeal squamous cell carcinoma—an update. CA Cancer J Clin 65(5):401–421
Cancer Facts & Figures 2019 (2019) https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2019/cancer-facts-and-figures-2019.pdf
Choi S, Myers JN (2008) Molecular pathogenesis of oral squamous cell carcinoma: implications for therapy. J Dent Res 87(1):14–32
Reibel JGN, Hille J et al (2017) Oral potentially malignant disorders and oral epithelial dysplasia. In: El-Naggar AKCJ, Grandis JR, et al. (eds) WHO Classification of Head and Neck Tumours, 4th edn. International Agency for Research on Cancer, Lyon, pp 112–113
Shirani S, Kargahi N, Razavi SM, Homayoni S (2014) Epithelial dysplasia in oral cavity. Iran J Med Sci 39(5):406–417
Silverman S Jr, Gorsky M, Lozada F (1984) Oral leukoplakia and malignant transformation. A follow-up study of 257 patients. Cancer 53(3):563–568
Lumerman H, Freedman P, Kerpel S (1995) Oral epithelial dysplasia and the development of invasive squamous cell carcinoma. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 79(3):321–329
Ho PS, Chen PL, Warnakulasuriya S, Shieh TY, Chen YK, Huang IY (2009) Malignant transformation of oral potentially malignant disorders in males: a retrospective cohort study. BMC Cancer 9:260
Arduino PG, Surace A, Carbone M et al (2009) Outcome of oral dysplasia: a retrospective hospital-based study of 207 patients with a long follow-up. J Oral Pathol Med 38(6):540–544
Neville BW, Day TA (2002) Oral cancer and precancerous lesions. CA Cancer J Clin. 52(4):195–215
Pindborg JJ, Reichart PA, Smith CJWI (1997) Histological typing of cancer and precancer of the oral mucosa. WHO International Histological Classification of Tumours, 2nd edn. Springer, Berlin
Barnes LEJ, Reichart P, Sidransky S (2005) World Health Organisation Classification of Tumours, Pathology and Genetics, Head and Neck Tumours. International Agency for Research on Cancer Press, Lyon
(2017) WHO Classification of Head and Neck Tumours, vol 9, 4 edn. IARC Press, Lyon
Dong Y, Chen Y, Tao Y et al (2019) Malignant transformation of oral leukoplakia treated with carbon dioxide laser: a meta-analysis. Lasers Med Sci 34(1):209–221
Mehanna HM, Rattay T, Smith J, McConkey CC (2009) Treatment and follow-up of oral dysplasia—a systematic review and meta-analysis. Head Neck 31(12):1600–1609
Awadallah M, Idle M, Patel K, Kademani D (2018) Management update of potentially premalignant oral epithelial lesions. Oral Surg Oral Med Oral Pathol Oral Radiol 125(6):628–636
Kujan O, Oliver RJ, Khattab A, Roberts SA, Thakker N, Sloan P (2006) Evaluation of a new binary system of grading oral epithelial dysplasia for prediction of malignant transformation. Oral Oncol 42(10):987–993
Diajil A, Robinson CM, Sloan P, Thomson PJ (2013) Clinical outcome following oral potentially malignant disorder treatment: a 100 patient cohort study. Int J Dent 2013:809248
Pindborg JJ, Reibel J, Holmstrup P (1985) Subjectivity in evaluating oral epithelial dysplasia, carcinoma in situ and initial carcinoma. J Oral Pathol 14(9):698–708
Abbey LM, Kaugars GE, Gunsolley JC et al (1995) Intraexaminer and interexaminer reliability in the diagnosis of oral epithelial dysplasia. Oral Surg Oral Med Oral Pathol Oral Radiol Endodontol 80(2):188–191
Karabulut A, Reibel J, Therkildsen MH, Praetorius F, Nielsen HW, Dabelsteen E (1995) Observer variability in the histologic assessment of oral premalignant lesions. J Oral Pathol Med 24(5):198–200
Fischer DJ, Epstein JB, Morton TH, Schwartz SM (2004) Interobserver reliability in the histopathologic diagnosis of oral pre-malignant and malignant lesions. J Oral Pathol Med 33(2):65–70
Warnakulasuriya S, Reibel J, Bouquot J, Dabelsteen E (2008) Oral epithelial dysplasia classification systems: predictive value, utility, weaknesses and scope for improvement. J Oral Pathol Med 37(3):127–133
Nankivell P, Williams H, Matthews P et al (2013) The binary oral dysplasia grading system: validity testing and suggested improvement. Oral Surg Oral Med Oral Pathol Oral Radiol 115(1):87–94
Kujan O, Khattab A, Oliver RJ, Roberts SA, Thakker N, Sloan P (2007) Why oral histopathology suffers inter-observer variability on grading oral epithelial dysplasia: an attempt to understand the sources of variation. Oral Oncol 43(3):224–231
Pilati S, Bianco BC, Vieira D, Modolo F (2017) Histopathologic features in actinic cheilitis by the comparison of grading dysplasia systems. Oral Dis 23(2):219–224
Camara PR, Dutra SN, Takahama Junior A, Fontes K, Azevedo RS (2016) A comparative study using WHO and binary oral epithelial dysplasia grading systems in actinic cheilitis. Oral Dis 22(6):523–529
Liu W, Shi LJ, Wu L et al (2012) Oral cancer development in patients with leukoplakia–clinicopathological factors affecting outcome. PLoS ONE 7(4):e34773
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339:b2535
Viera AJ, Garrett JM (2005) Understanding interobserver agreement: the kappa statistic. Fam Med 37(5):360–363
Jeremy Howick ICJLL, Glasziou P, Greenhalgh T, Heneghan C, Liberati A, Moschetti I, Phillips B, Thornton H, Goddard O, Hodgkinson M. The Oxford 2011 levels of evidence. http://www.cebm.net/index.aspx?o1/45653
Higgins JPT GS (2011) Cochrane Handbook for Systematic Reviews of Interventions. Version 5.1.0. The Cochrane Collaboration
Sterne JA, Hernán MA, Reeves BC et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919
Hedges LVOI (1985) Statistical methods for meta-analysis. Academic, London
Egger MDSG, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315(7109):629–634
Sterne JAEM (2001) Funnel plots for detecting bias in meta-analysis: guidelines on choice of axis. J Clin Epidemiol 54(10):1046–1055
Sterne JACSA, Ioannidis JPA et al (2011) Recommendations for examining and interpreting funnel plot asymmetry in meta-analyses of randomised controlled trials. BMJ (Clinical research ed) 343:d4002
Centre for Evidence-Based Medicine (2009) Oxford centre for evidence-based medicine—levels of evidence. https://www.cebm.net/2009/06/oxford-centre-evidence-based-medicine-levels-evidence-march-2009/. Accessed 6 Feb 2020
Hu Y, Liu H (2014) Diagnostic variability of laryngeal premalignant lesions: histological evaluation and carcinoma transformation. Otolaryngol Head Neck Surg 150(3):401–406
Karatayli-Ozgursoy S, Pacheco-Lopez P, Hillel AT, Best SR, Bishop JA, Akst LM (2015) Laryngeal dysplasia, demographics, and treatment: a single-institution, 20-year review. JAMA Otolaryngol Head Neck Surg 141(4):313–318
Weller MD, Nankivell PC, McConkey C, Paleri V, Mehanna HM (2010) The risk and interval to malignancy of patients with laryngeal dysplasia; a systematic review of case series and meta-analysis. Clin Otolaryngol 35(5):364–372
Spielmann PM, Palmer T, McClymont L (2010) 15-Year review of laryngeal and oral dysplasias and progression to invasive carcinoma. Eur Arch Otorhinolaryngol 267(3):423–427
Crissman JD, Sakr W (2001) Squamous neoplasia of the upper aerodigestive tract: intraepithelial and invasive squamous cell carcinoma. In: Head and neck surgical pathology
Cho KJ, Song JS (2018) Recent changes of classification for squamous intraepithelial lesions of the head and neck. Arch Pathol Lab Med 142(7):829–832
McHugh ML (2012) Interrater reliability: the kappa statistic. Biochem Med (Zagreb) 22(3):276–282
Author information
Authors and Affiliations
Contributions
FY conceptualization, methodology, formal analysis, data curation, writing—original draft, writing—review and editing. PDR data curation, writing—original draft, writing—review and editing. SAN formal analysis, writing—review and editing. ACC writing—review and editing, supervision. BWN review and editing, supervision. TAD conceptualization, methodology, writing—review and editing, supervision. All authors approved the final version to be published.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
Ethical approval was not required as this did not involve individual patient data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
405_2020_6036_MOESM1_ESM.tif
Supplementary file1 Supplemental Figure 1 Funnel plot of studies included in meta-analysis of determining odds ratio of malignant transformation of high-risk lesions over low-risk lesions (TIF 112 kb)
405_2020_6036_MOESM2_ESM.tif
Supplementary file2 Supplemental Figure 2 Risk of bias graph. A review of authors’ judgments about each risk of bias item presented as percentages across all included studies. (TIF 185 kb)
405_2020_6036_MOESM3_ESM.tif
Supplementary file3 Supplemental Figure 3 Risk of bias summary. A review of authors’ judgments about each risk of bias item for each included study (TIF 179 kb)
Rights and permissions
About this article
Cite this article
Yan, F., Reddy, P.D., Nguyen, S.A. et al. Grading systems of oral cavity pre-malignancy: a systematic review and meta-analysis. Eur Arch Otorhinolaryngol 277, 2967–2976 (2020). https://doi.org/10.1007/s00405-020-06036-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-020-06036-1