Abstract
Purpose
Day-case thyroid surgery has been endorsed by the American Thyroid Association and the British Association of Day Surgery. Despite the many benefits of day surgery, day-case thyroid surgery is not widely practiced. We describe the use of sensitivity analysis modelling and cost analysis in determining and refining the patient cohort that safely meet the threshold for a new day-case thyroid lobectomy service at a tertiary referral head and neck centre.
Methods
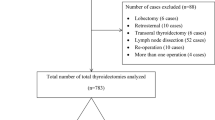
All cases of first-time thyroid lobectomy were identified between 2015 and Q2 2019. Patients suitable for day-case thyroid lobectomy were identified retrospectively, according to the following criteria: Age < 65 years, ASA grade < 3, BMI < 30 kg/m2 and distance from tertiary unit < / = 30 min. Sensitivity analysis was undertaken, manipulating each parameter in turn to assess the effect on eligibility and associated cost-savings.
Results
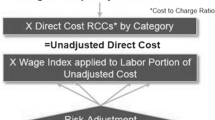
259 Thyroid lobectomy procedures were performed, 173 of these met inclusion criteria. Sensitivity analysis revealed that after increasing all day-case parameters by four increments, eligibility increased from 47 (27%) to 112 patients (64.7%), with only one outpatient to inpatient conversion. Multivariate logistical regression analysis found that age was the only variable to increase the risk of adverse outcomes (OR = 1.10, p < 0.05). Using data from the NHS reference costs, if 60% of all thyroid lobectomies nationally were undertaken as day-case, this would have amounted to savings of £26.3 m over five years.
Conclusion
Through sensitivity analysis, we determined that we could safely offer day-case thyroid lobectomy to 64.7% of our patient cohort.
Similar content being viewed by others
References
BADS Council (2019) BADS Directory of procedures [S.l.]: British Association of DA
Terris D, Snyder S, Carneiro-Pla D, Inabnet W, Kandil E, Orloff L et al (2013) American thyroid association statement on outpatient thyroidectomy. Thyroid 23(10):1193–1202
Lee D, Chin C, Hong C, Perera S, Witterick I (2017) Outpatient versus inpatient thyroidectomy: a systematic review and meta-analysis. Head Neck 40(1):192–202. https://doi.org/10.1002/hed.24934
Orosco R, Lin H, Bhattacharyya N (2015) Ambulatory thyroidectomy. Otolaryngol-Head Neck Surg 152(6):1017–1023. https://doi.org/10.1177/0194599815577603
Lacroix C, Potard G, Clodic C, Mornet E, Valette G, Marianowski R (2014) Outpatient hemithyroidectomy. Eur Ann Otorhinolaryngol Head Neck Dis 131(1):21–26. https://doi.org/10.1016/j.anorl.2013.01.005
Snyder S, Hamid K, Roberson C et al (2010) Outpatient thyroidectomy is safe and reasonable: experience with more than 1000 planned outpatient procedures. J Am Coll Surg 210(5):575–582. https://doi.org/10.1016/j.jamcollsurg.2009.12.037
Tewary A (1993) Day-case tonsillectomy: a review of the literature. J Laryngol Otol 107(8):703–705. https://doi.org/10.1017/s0022215100124181
Briggs C, Irving G, Mann C, Cresswell A, Englert L, Peterson M et al (2009) Introduction of a day-case laparoscopic cholecystectomy service in the UK: a critical analysis of factors influencing same-day discharge and contact with primary care providers. Ann R Coll Surg Engl 91(7):583–590
International guidelines for groin hernia management (2018) Hernia 22(1):1–165
Appleby J (2019) Day-case surgery: a good news story for the NHS. The King's Fund. https://www.kingsfund.org.uk/blog/2015/07/day-case-surgery-good-news-story-nhs. Accessed 19 Oct 2019
Lemos P, Pinto A, Morais G et al (2009) Patient satisfaction following day surgery. J Clin Anesth 21(3):200–205. https://doi.org/10.1016/j.jclinane.2008.08.016
Quemby D, Stocker M (2014) Day surgery development and practice: key factors for a successful pathway. Contin Educ Anaesth Crit Care Pain 14(6):256–261. https://doi.org/10.1093/bjaceaccp/mkt066
Alkire B, Raykar N, Shrime M et al (2015) Global access to surgical care: a modelling study. Lancet Glob Health 3(6):e316–e323. https://doi.org/10.1016/s2214-109x(15)70115-4
Verguet S, Alkire B, Bickler S et al (2015) Timing and cost of scaling up surgical services in low-income and middle-income countries from 2012 to 2030: a modelling study. Lancet Glob Health 3:S28–S37. https://doi.org/10.1016/s2214-109x(15)70086-0
Pearse R, Moreno R, Bauer P et al (2012) Mortality after surgery in Europe: a 7 day cohort study. Lancet 380(9847):1059–1065. https://doi.org/10.1016/s0140-6736(12)61148-9
Bailey C, Ahuja M, Bartholomew K et al (2019) Guidelines for day-case surgery 2019. Anaesthesia 74(6):778–792. https://doi.org/10.1111/anae.14639
Emmett S, Sudoko C, Tucci D et al (2019) Expanding access: cost-effectiveness of cochlear implantation and deaf education in Asia. Otolaryngol Head Neck Surg 161(4):672–682. https://doi.org/10.1177/0194599819849917
Kerwat D, Zargaran A, Bharamgoudar R et al (2018) Early laparoscopic cholecystectomy is more cost-effective than delayed laparoscopic cholecystectomy in the treatment of acute cholecystitis. ClinicoEcon Outcomes Res 10:119–125. https://doi.org/10.2147/ceor.s149924
Grimes CE, Henry JA, Maraka J, Mkandawire NC, Cotton M (2013) Cost-effectiveness of surgery in low-and middle-income countries: a systematic review. World J Surg 38(1):252–263. https://doi.org/10.1007/s00268-013-2243-y
Chao T, Sharma K, Mandigo M et al (2014) Cost-effectiveness of surgery and its policy implications for global health: a systematic review and analysis. Lancet Glob Health 2(6):e334–e345. https://doi.org/10.1016/s2214-109x(14)70213-x
Chadwick D, Kinsman R, Walton P (2017) Fifth national audit report. The British Association of Endocrine & Thyroid Surgeons, p 101. https://www.baets.org.uk/wp-content/uploads/BAETS-Audit-National-Report-2017.pdf. Accessed 31 Mar 2020
Reference Costs 2017/18: highlights, analysis and introduction to the data. NHS Improvement, 2018, p 5. https://improvement.nhs.uk/documents/1972/1_-_Reference_costs_201718.pdf. Accessed 31 Mar 2020
Acknowledgements
We would like to thank Mr Brian Fish, Mr Piyush Jani and Mr Furrat Amen for their contributions, without whom this project would not have been possible. No funding or ethical approval was required and there is no conflict of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
This work describes a retrospective study of existing hospital data to model a future protocol. Ethical approval was not required for this work. This work was reviewed and approved by the quality assurance lead for the hospital.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sheikh, Z., Irune, E. Day-case thyroid lobectomy parameters at a tertiary referral head and neck centre: a sensitivity and cost analysis. Eur Arch Otorhinolaryngol 277, 2527–2531 (2020). https://doi.org/10.1007/s00405-020-05921-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-020-05921-z