Abstract
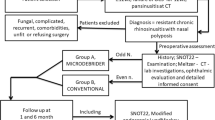
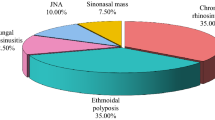
To conduct a prospective randomized controlled trial investigating the efficacy and safety of powered versus conventional endoscopic sinus surgery instruments in the management of sinonasal polyposis. Two hundred patients with sinonasal polyposis who failed conservative therapy were included in the study. They were equally randomized into powered and conventional instruments groups. A subjective visual analogue scale (VAS), endoscopic examination, saccharine clearance time and coronal CT were done preoperatively. Intraoperatively, the operative time, the surgical conditions and degrees of dryness of the operative field were carefully rated and recorded. Postoperatively, VAS, polyp grades, saccharine clearance time, the number of endoscopic debridement and time to mucosalization were recorded. Complications, smoothness of postoperative course were reported. Both groups experienced a significant improvement in the VAS with no statistically significant difference in symptom improvement between the two groups except for olfaction where there was significant improvement in the powered group. Similarly, the two groups demonstrated a significant improvement in the objective parameters including polyp grade and saccharine clearance time changes, but no significant difference between the two groups was found. The operative time as well as the surgical conditions and dryness of the operative field score were significantly better in the powered group. There was a tendency for improvement in the number of endoscopic debridement and time to mucosalization in powered group when compared to conventional instruments group, but this did not reach statistical significance. The incidence of postoperative synechiae was significantly lower in powered endoscopic group. Powered endoscopic sinus surgery offers a better therapeutic approach for patients with sinonasal polyposis when compared to endoscopic surgery with the conventional instruments. It provides a bloodless dry operative field with better visualization for a more precise, less traumatic procedure with minimal intraoperative complications and shorter operative time. Additionally, patients have a smoother postoperative course, less incidence of synechiae, with a tendency for a faster healing.
Similar content being viewed by others
References
Becker SS (2009) Surgical management of polyps in the treatment of nasal airway obstruction. Otolaryngol Clin North Am 42(2):377–385
Setliff RC, Parsons DS (1994) The “Hummer”: new instrumentation for functional endoscopic sinus surgery. Am J Rhinol 8:275–278
Bernstein JM, Lebowitz RA, Jacobs JB (1998) Initial report on postoperative healing after endoscopic sinus surgery with the microdebrider. Otolaryngol Head Neck Surg 118(6):800–803
Stammberger H (1991) Functional endoscopic sinus surgery. BC Decker, Philadelphia
Gross CW, Becker DG (1996) Power instrumentation in endoscopic sinus surgery. Oper Tech Otolaryngol–Head Neck Surg 7(3):236–241
Lund VJ, Kennedy DW (1995) Quantification for staging sinusitis. Ann Otol Rhinol Laryngol Suppl 167:17–21
Mackay IS, Lund VJ (1997) Imaging and staging. In: Lildholdt T, Mygind N (eds) Nasal polyposis. An inflammatory disease and its treatment. Munksgaard, Copenhagen, pp 137–144
Jaccobi KE, Bohn BE, Rickauer JA, Jaccobi C, Hemmerling TM (2000) Moderate controlled hypotension with sodium nitroprusside does not improve surgical conditions or decrease blood loss in endoscopic sinus surgery. J Clin Anaesth 12:202–207
Badia L, Lund V (2001) Topical corticosteroids in nasal polyposis. Drugs 61(5):573–578
Waguespack R (1995) Mucociliary clearance patterns following endoscopic sinus surgery. Laryngoscope 105(7 Pt 2 Suppl 71):1–40
Stankiewicz JA (1987) Complications of intranasal endoscopic ethmoidectomy. Laryngoscope 97:1270–1273
Lazar RH, Younis RT, Long TE (1993) Functional endonasal sinus surgery in adults and children. Laryngoscope 103:1–5
Gaskins RE (1994) Scarring in endoscopic ethmoidectomy. Am J Rhinol 8(271):274
Jacobs JB, Gittelman P, Holliday R (1990) Endoscopic sinus surgery for ostiomeatal disease. Am J Rhinol 4:41–43
Krouse JH, Christmas DA (1996) Powered instrumentation in functional endoscopic sinus surgery II: a comparative study. Ear Nose Throat J 75:42–44
Selivanova O, Kuehnemund M, Mann WJ, Amedee RG (2003) Comparison of conventional instruments and mechanical debriders for surgery of patients with chronic sinusitis. Am J Rhinol 17(4):197–202
Sauer M, Lemmens W, Vauterin T, Jorissen M (2007) Comparing the microdebrider and standard instruments in endoscopic sinus surgery: a double-blind randomised study. B-ENT 3(1):1–7
Bruggers S, Sindwani R (2009) Evolving trends in powered endoscopic sinus surgery. Otolaryngol Clin North Am 42(5):789–798
Bruggers S, Sindwani R (2009) Innovations in microdebrider technology and design. Otolaryngol Clin North Am 42(5):781–787
Ecevit MC, Sutay S, Erdag TK (2008) The microdébrider and its complications in endoscopic surgery for nasal polyposis. J Otolaryngol Head Neck Surg 37(2):160–164
Conflict of interest
The authors have no conflict of interest, financial or otherwise with any organization.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Saafan, M.E., Ragab, S.M., Albirmawy, O.A. et al. Powered versus conventional endoscopic sinus surgery instruments in management of sinonasal polyposis. Eur Arch Otorhinolaryngol 270, 149–155 (2013). https://doi.org/10.1007/s00405-012-1969-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-012-1969-8