Abstract
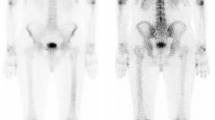
Differentiation between cerebral radionecrosis and intracranial relapse in irradiated nasopharyngeal carcinoma (NPC) patients challenges the clinicians, especially when clinical manifestation and MRI findings are inconclusive. A 63-year-old NPC patient had intermittent dizziness and unsteady gait 3 years after irradiation. An ice water caloric test revealed absent response on the right ear, which was compatible with an enhanced lesion at the right temporal lobe on MRI scan. Furthermore, abnormal focally increased uptake over the anteriomedial aspect of the right temporal lobe was disclosed on 18-fluoro-2-deoxyglucose (FDG) positron emission tomography (PET), which suggested intracranial relapse. Conversely, serological study for Epstein-Barr viral titer was within normal limits, arguing against either recurrent or metastatic NPC. Hence, thallium (Tl)-201 single photon emission computed tomography (SPECT) was subsequently conducted, which failed to demonstrate abnormal thallium accumulation in the corresponding area. Accordingly, radiation necrosis of the temporal lobe rather than intracranial relapse is considered. The patient was rather well without locoregional recurrence or distant metastasis 2 years after presentation.



Similar content being viewed by others
References
Hong RL, Ting LL, Ko JY, Hsu MM, Sheen TS, Lou PJ, Wang CC, Chung NN, Lui T. (2001) Induction chemotherapy with mitomycin, epirubicin, cisplatin, flurouracil, and leucovorin followed by radiotherapy in the treatment of locoregionally advanced nasopharyngeal carcinoma. J Clin Oncol 19:4305–4313
Chong FH, Fan YF (1997) Detection of recurrent nasopharyngeal carcinoma, MR imaging versus CT. Radiology 202:463–470
Kao CH, ChangLai SP, Chieng PU, Yen RF, Yen TC (1998) Detection of recurrent or persistent nasopharyngeal carcinoma after radiotherapy with 18-fluoro-2-deoxyglucose positron emission tomography and comparison with computed tomography. J Clin Oncol 16:3550–3555
Yen RH, Hung RL, Pan MH, Wang YH, Huang KM, Lui T, Kao CH (2003) 18-fluoro-2-deoxyglucose positron emission tomography in detecting residual/recurrent nasopharyngeal carcinoma and comparison with magnetic resonance imaging. Cancer 98:283–287
Hu JQ, Guan YH, Zhao LZ, Xie SX, Guo Z, Liang ZH (1991) Delayed radiation encephalopathy after radiotherapy for nasopharyngeal cancer: A CT study of 45 cases. J Comput Assist Tomo 15:181–187
Woo E, Lam K, Yu YL, Ma J, Wang C, Yeung RTT (1988) Temporal lobe and hypothalamic-pituitary dysfunction after radiotherapy for nasopharyngeal carcinoma: a distinct clinical syndrome. J Neurol Neurosurg Psychiatry 51:1302–1307
Liu SH, Chang JT, Ng SH, Chan SC, Yen TC (2004) False positive fluoro-18 fluorodeoxy-D-glucose positron emission tomography finding caused by osteoradionecrosis in a nasopharyngeal carcinoma patient. Br J Radiol 77:257–260
Yang TL, Young YH (2004) Radiation-induced otitis media -study by a new test, vestibular evoked myogenic potential. Int J Radiat Oncol Biol Phys 60:295–301
Henle G, Henle W (1976) Epstein-Barr virus-specific IgA serum antibodies as an out-standing feature of nasopharyngeal carcinoma. Int J Cancer 17:1–7
Huang TW, Young Y-H (2002) Differentiation between cerebellopontine angle tumors in cancer patients. Otol Neurotol 23:975–979
Tai CJ, Liang JA, Yang SN, Tsai MH, Lin CC, Kao CH (2003) Detection of recurrent nasopharyngeal carcinoma with thallium-201 single photon emission computed tomography in patients with indeterminate magnetic resonance imaging findings after radiotherapy. Head Neck 25:227–231
Sehweil AM, McKillop JH, Milroy R, Wilson R, Abdel-Dayem HM, Omar YT (1989) Mechanism of201Tl uptake in tumors. Eur J Nucl Med 15:376–379
Acknowledgements
This work was supported by the National Science Council grant NSC 93-2314-B002-114, Taipei, Taiwan.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wang, CT., Young, YH. Potential usefulness of Tl-201 SPECT for differentiating radionecrosis in an irradiated nasopharyngeal carcinoma patient. Eur Arch Otorhinolaryngol 263, 135–138 (2006). https://doi.org/10.1007/s00405-005-0964-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-005-0964-8