Abstract
Objective
To investigate the predictive value of the Controlling Nutritional Status (CONUT) score on hyperemesis gravidarum (HG) severity, hospitalization, and length of stay.
Materials and methods
This retrospective cross-sectional study, conducted between December 2022 and June 2023, involved two groups. Group 1 comprised 52 pregnant women diagnosed with HG in the first trimester, receiving hospitalization and treatment. Group 2 included 105 pregnant women diagnosed with HG in the first trimester, managed and treated as outpatients. The CONUT score was calculated with the formula: Serum albumin score + total lymphocyte score + total cholesterol score. This score is calculated with a number of points between 0 and 12. The interpretation of the score involves four categories: normal (0–1), light (2–4), moderate (5–8), and severe (9–12).
Results
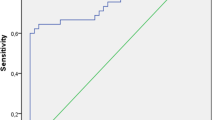
The CONUT score differed significantly between the hospitalized (4, IQR: 2.25–5) and outpatient groups (2, IQR: 2–3) (p < 0.001). A CONUT score >3 was associated with the need for hospitalization, demonstrating a sensitivity of 60%, a specificity of 84% (p < 0.001). The CONUT score was the parameter with the highest odds ratio (OR) value among the parameters related to the need for hospitalization, and each unit increase in the CONUT score increased the need for hospitalization by 1.683 times [OR = 1.683 (95% CI: 1.042–2.718), p = 0.033]. A positive correlation was found between the CONUT score and the duration of hospital stay (r = 0.316, p = 0.023).
Conclusions
This study suggests CONUT score as a valuable tool for predicting HG severity, hospitalization need, and duration of hospital stay.



Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding authors upon reasonable request.
References
Boelig RC, Barton SJ, Saccone G, Kelly AJ, Edwards SJ, Berghella V (2018) Interventions for treating hyperemesis gravidarum: a Cochrane systematic review and meta-analysis. J Matern-Fetal Neonatal Med Off J Eur Assoc Perinat Med Fed Asia Ocean Perinat Soc Int Soc Perinat Obstet 31:2492–2505. https://doi.org/10.1080/14767058.2017.1342805
Bayraktar B, Balıkoğlu M, Bayraktar MG, Kanmaz AG (2021) The effects of hyperemesis gravidarum on the oral glucose tolerance test values and gestational diabetes. Prague Med Rep 122:285–293. https://doi.org/10.14712/23362936.2021.26
Li N, Xue Z, Xu H, Yang P, Wang K, Li L, Kang H, Wang M, Deng Y, Li X, Wang Y, Zhu J, Yu P, Zhou S (2023) Evaluation of nausea and vomiting in the first trimester on the risk of adverse birth outcomes and the contribution of genetic polymorphisms: a pilot prospective study. Arch Gynecol Obstet 308:1713–1721. https://doi.org/10.1007/s00404-022-06851-3
Nurmi M, Rautava P, Gissler M, Vahlberg T, Polo-Kantola P (2022) Readmissions due to hyperemesis gravidarum: a nation-wide Finnish register study. Arch Gynecol Obstet 306:1519–1529. https://doi.org/10.1007/s00404-022-06448-w
Goodwin TM (2008) Hyperemesis gravidarum. Obstet Gynecol Clin North Am 35:401–417, viii. https://doi.org/10.1016/j.ogc.2008.04.002
Committee on Practice Bulletins-Obstetrics (2018) ACOG practice bulletin no. 189: nausea and vomiting of pregnancy. Obstet Gynecol 131:e15–e30. https://doi.org/10.1097/AOG.0000000000002456
Wang X, Yang G, Li K, Yang F, Liang X, Wu S (2024) Efficacy and safety of acupressure in nausea and vomiting during pregnancy: a systematic review and meta-analysis of randomized controlled trials. Arch Gynecol Obstet 309:1237–1248. https://doi.org/10.1007/s00404-023-07313-0
London V, Grube S, Sherer DM, Abulafia O (2017) Hyperemesis gravidarum: a review of recent literature. Pharmacology 100:161–171. https://doi.org/10.1159/000477853
Bailit JL (2005) Hyperemesis gravidarium: epidemiologic findings from a large cohort. Am J Obstet Gynecol 193:811–814. https://doi.org/10.1016/j.ajog.2005.02.132
Jayawardena R, Majeed S, Sooriyaarachchi P, Abeywarne U, Ranaweera P (2023) The effects of pyridoxine (vitamin B6) supplementation in nausea and vomiting during pregnancy: a systematic review and meta-analysis. Arch Gynecol Obstet 308:1075–1084. https://doi.org/10.1007/s00404-023-06925-w
Geeganage G, Iturrino J, Shainker SA, Ballou S, Rangan V, Nee J (2023) Emergency department burden of hyperemesis gravidarum in the United States from 2006 to 2014. AJOG Glob Rep 3:100166. https://doi.org/10.1016/j.xagr.2023.100166
Uemura S, Iwashita T, Ichikawa H, Iwasa Y, Mita N, Shiraki M, Shimizu M (2022) Impact of Controlling nutritional status (CONUT) in patients with unresectable advanced pancreatic cancer receiving multi-agent chemotherapy: a single center, retrospective cohort study. Pancreatol Off J Int Assoc Pancreatol IAP Al 22:304–310. https://doi.org/10.1016/j.pan.2022.01.010
Çi̇ntesun E, Seçilmiş Kerimoğlu Ö, Celik C, Işık E (2021) Evaluation of prognostic nutritional status in late-onset fetal growth restriction. J Clin Obstet Gynecol 31:14–19. https://doi.org/10.5336/jcog.2020-79476
Yuan J, Wang Q, Cheng J, Wang J, Zhang Y (2023) Using preoperative control nutritional status scores as prognostic factors for endometrial cancer. Front Oncol 13:1126576. https://doi.org/10.3389/fonc.2023.1126576
Yamaura T, Arizumi F, Maruo K, Kishima K, Yoshie N, Kusukawa T, Imamura F, Tachibana T (2022) The impact of controlling nutritional status (CONUT) score on functional prognosis in hospitalized elderly patients with acute osteoporotic vertebral fractures. BMC Geriatr 22:1002. https://doi.org/10.1186/s12877-022-03708-x
Ignacio de Ulíbarri J, González-Madroño A, de Villar NGP, González P, González B, Mancha A, Rodríguez F, Fernández G (2005) CONUT: a tool for controlling nutritional status. First validation in a hospital population. Nutr Hosp 20:38–45
Rhodes VA, Watson PM, Johnson MH (1984) Development of reliable and valid measures of nausea and vomiting. Cancer Nurs 7:33–41
Koren G, Boskovic R, Hard M, Maltepe C, Navioz Y, Einarson A (2002) Motherisk-PUQE (pregnancy-unique quantification of emesis and nausea) scoring system for nausea and vomiting of pregnancy. Am J Obstet Gynecol 186:S228-231. https://doi.org/10.1067/mob.2002.123054
Tan PC, Jacob R, Quek KF, Omar SZ (2006) Indicators of prolonged hospital stay in hyperemesis gravidarum. Int J Gynaecol Obstet Off Organ Int Fed Gynaecol Obstet 93:246–247. https://doi.org/10.1016/j.ijgo.2006.03.012
Koot MH, Grooten IJ, Post JAMV, Bais JMJ, Ris-Stalpers C, Naaktgeboren CA, Niemeijer MN, Bremer HA, van der Ham DP, Heidema WM, Huisjes A, Kleiverda G, Kuppens SM, van Laar JOEH, Langenveld J, van der Made F, Papatsonis D, Pelinck MJ, Pernet PJ, van Rheenen-Flach L, Rijnders RJ, Scheepers HCJ, Vogelvang TE, Mol BW, Roseboom TJ, Painter RC (2020) Ketonuria is not associated with hyperemesis gravidarum disease severity. Eur J Obstet Gynecol Reprod Biol 254:315–320. https://doi.org/10.1016/j.ejogrb.2020.08.014
Ustün Y, Engin-Ustün Y, Dökmeci F, Söylemez F (2004) Serum concentrations of lipids and apolipoproteins in normal and hyperemetic pregnancies. J Matern-Fetal Neonatal Med Off J Eur Assoc Perinat Med Fed Asia Ocean Perinat Soc Int Soc Perinat Obstet 15:287–290. https://doi.org/10.1080/14767050410001680028
Aksoy H, Aksoy AN, Ozkan A, Polat H (2009) Serum lipid profile, oxidative status, and paraoxonase 1 activity in hyperemesis gravidarum. J Clin Lab Anal 23:105–109. https://doi.org/10.1002/jcla.20298
Funding
The authors received no financial support for this article’s research, authorship, and publication.
Author information
Authors and Affiliations
Contributions
GK and BB conducted the population study, analyzed and interpreted the data, and wrote the article. ZS, STS, BTC, GA, MB participated in data analysis, interpretation, and manuscript revision. IO and CTI participated in data collection and interpretation of results. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study was approved by the Ethics Committee of Ankara Etlik City Hospital (approval number: AESH-EK1-2023-276). This study was conducted in accordance with the principles of the Declaration of Helsinki on the Ethical Principles of Medical Research.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Karabay, G., Bayraktar, B., Seyhanli, Z. et al. Evaluation of controlling nutritional status (CONUT) score in the prognosis of hyperemesis gravidarum. Arch Gynecol Obstet (2024). https://doi.org/10.1007/s00404-024-07534-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00404-024-07534-x