Abstract
Purpose
To develop predictive nomograms of lymph vascular space invasion (LVSI) in patients with early-stage cervical cancer.
Methods
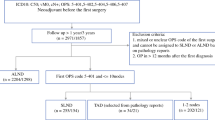
We identified 403 patients with cervical cancer from the Affiliated Hospital of Jiangnan University from January 2015 to December 2019. Patients were divided into the training set (n = 242) and the validation set (n = 161), with patients in the training set subdivided into LVSI (+) and LVSI (−) groups according to postoperative pathology. Preoperative hematologic indexes were compared between the two subgroups. Univariate and multivariate logistic regression analyses were used to analyze the independent risk factors for LVSI, from which a nomogram was constructed using the R package.
Results
LVSI (+) was present in 94 out of 242 patients in the training set, accompanied by a significant increase in the preoperative squamous cell carcinoma antigen (SCC), white blood cells (WBC), neutrophil (NE), platelet (PLT), neutrophil-to-lymphocyte ratio (NLR), platelet-to-lymphocyte ratio (PLR), systemic inflammation index (SII), and tumor size (P < 0.05). Univariate analysis showed that SCC, WBC, NE, NLR, PLR, SII, and tumor size were correlated with LVSI (P < 0.05), and multivariate analysis showed that tumor size, SCC, WBC, and NLR were independent risk factors for LVSI (P < 0.05). A nomogram was correspondingly established with good performance in predicting LVSI [training: ROC-AUC = 0.845 (95% CI: 0.731–0.843) and external validation: ROC-AUC = 0.704 (95% CI: 0.683–0.835)] and high accuracy (training: C-index = 0.787; external validation: C-index = 0.759).
Conclusion
The nomogram based on preoperative tumor size, SCC, WBC, and NLR had excellent accuracy and discriminative capability to assess the risk of LVSI in early-stage cervical cancer patients.



Similar content being viewed by others
Data availability
The data used and analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- LVSI:
-
Lymph vascular space invasion
- CC:
-
Cervical cancer
- SCC:
-
Squamous cell carcinoma antigen
- WBC:
-
White blood cells
- NE:
-
Neutrophil
- PLT:
-
Platelet
- PLR:
-
Platelet-to-lymphocyte ratio
- NLR:
-
Neutrophil-to-lymphocyte ratio
- SII:
-
Systemic inflammation index
References
Gillies RJ, Anderson AR, Gatenby RA, Morse DL (2010) The biology underlying molecular imaging in oncology: from genome to anatome and back again. Clin Radiol 65(7):517–521
Lambin P, Rios-Velazquez E, Leijenaar R, Carvalho S, van Stiphout RG, Granton P, Zegers CM, Gillies R, Boellard R, Dekker A et al (2012) Radiomics: extracting more information from medical images using advanced feature analysis. Eur J Cancer 48(4):441–446
Graves S, Seagle BL, Strohl AE, Shahabi S, Nieves-Neira W (2017) Survival after pelvic exenteration for cervical cancer: a national cancer database study. Int J Gynecol Cancer 27(2):390–395
Levinson K, Beavis AL, Purdy C, Rositch AF, Viswanathan A, Wolfson AH, Kelly MG, Tewari KS, McNally L, Guntupalli SR et al (2021) Beyond Sedlis-A novel histology-specific nomogram for predicting cervical cancer recurrence risk: an NRG/GOG ancillary analysis. Gynecol Oncol 162(3):532–538
Sullivan T, Yacoub JH, Harkenrider MM, Small W Jr, Surucu M, Shea SM (2018) Providing MR imaging for cervical cancer brachytherapy: lessons for radiologists. Radiographics 38(3):932–944
Wu Q, Shi D, Dou S, Shi L, Liu M, Dong L, Chang X, Wang M (2019) Radiomics analysis of multiparametric MRI evaluates the pathological features of cervical squamous cell carcinoma. J Magn Reson Imaging 49(4):1141–1148
Li J, Li S, Chen R, Lu X (2017) Increased risk of poor survival in ovarian cancer patients with high expression of SNAI2 and lymphovascular space invasion. Oncotarget 8(6):9672–9685
Matsuo K, Sheridan TB, Mabuchi S, Yoshino K, Hasegawa K, Studeman KD, Im DD, Rosenshein NB, Roman LD, Sood AK (2014) Estrogen receptor expression and increased risk of lymphovascular space invasion in high-grade serous ovarian carcinoma. Gynecol Oncol 133(3):473–479
Zhao Y, Yang N, Wang X, Huang Y, Zhou X, Zhang D (2020) Potential roles of lymphovascular space invasion based on tumor characteristics provide important prognostic information in T1 tumors with ER and HER2 positive breast cancer. Clin Transl Oncol 22(12):2275–2285
Li X, Xu C, Yu Y, Guo Y, Sun H (2021) Prediction of lymphovascular space invasion using a combination of tenascin-C, cox-2, and PET/CT radiomics in patients with early-stage cervical squamous cell carcinoma. BMC Cancer 21(1):866
Han S, Liu X, Ju S, Mu W, Abulikemu G, Zhen Q, Yang J, Zhang J, Li Y, Liu H et al (2023) New mechanisms and biomarkers of lymph node metastasis in cervical cancer: reflections from plasma proteomics. Clin Proteomics 20(1):35
Bouvard V, Wentzensen N, Mackie A, Berkhof J, Brotherton J, Giorgi-Rossi P, Kupets R, Smith R, Arrossi S, Bendahhou K et al (2021) The IARC perspective on cervical cancer screening. N Engl J Med 385(20):1908–1918
Zannoni GF, Travaglino A, Raffone A, Arciuolo D, D’Alessandris N, Scaglione G, Tralongo P, Inzani F, Angelico G, Santoro A (2021) Depth of stromal invasion as the most prognostically relevant regression system in locally advanced cervical cancer after neoadjuvant treatment: a systematic review and meta analysis grading. Diagnostics. https://doi.org/10.3390/diagnostics11101772
Santoro A, Angelico G, Inzani F, Arciuolo D, Spadola S, Valente M, D’Alessandris N, Piermattei A, Fiorentino V et al (2020) Standard ultrastaging compared to one-step nucleic acid amplification (OSNA) for the detection of sentinel lymph node metastases in early stage cervical cancer. Int J Gynecol Cancer 30(12):1871–1877
Gorostidi Pulgar Diaz M, de la Noval B, Gil-Ibanez B, Lago Leal V, Jaunarena Marin I, Padilla IP (2017) lymphovascular space invasion for endometrial cancer: undertreatment and overtreatment risks: a survey of the Spanish gynecologic oncology group. Int J Gynecol Cancer 27(6):1191–1199
Logani S, Herdman AV, Little JV, Moller KA (2008) Vascular “pseudo invasion” in laparoscopic hysterectomy specimens: a diagnostic pitfall. Am J Surg Pathol 32(4):560–565
Benedet JL, Odicino F, Maisonneuve P, Beller U, Creasman WT, Heintz AP, Ngan HY, Pecorelli S (2003) Carcinoma of the cervix uteri. Int J Gynaecol Obstet 83(Suppl 1):41–78
Xie X, Song K, Cui B, Jiang J, Yang X, Kong B (2018) A comparison of the prognosis between adenocarcinoma and squamous cell carcinoma in stage IB-IIA cervical cancer. Int J Clin Oncol 23(3):522–531
Koh WJ, Abu-Rustum NR, Bean S, Bradley K, Campos SM, Cho KR, Chon HS, Chu C, Clark R, Cohn D et al (2019) Cervical cancer, version 32019, NCCN clinical practice guidelines in oncology. J Natl Compr Canc Netw 17(1):64–84
Park KJ, Selinger CI, Alvarado-Cabrero I, Duggan MA, Kiyokawa T, Mills AM, Ordi J, Otis CN, Plante M, Stolnicu S et al (2022) Dataset for the reporting of carcinoma of the cervix: recommendations from the international collaboration on cancer reporting (ICCR). Int J Gynecol Pathol Off Int Soc Gynecol Pathol 41(Suppl 1):S64-s89
Santoro A, Inzani F, Angelico G, Arciuolo D, Bragantini E, Travaglino A, Valente M, D’Alessandris N, Scaglione G, Sfregola S et al (2023) Recent advances in cervical cancer management: a review on novel prognostic factors in primary and recurrent tumors. Cancers. https://doi.org/10.3390/cancers15041137
Salvatici M, Achilarre MT, Sandri MT, Boveri S, Vanna Z, Landoni F (2016) Squamous cell carcinoma antigen (SCC-Ag) during follow-up of cervical cancer patients: Role in the early diagnosis of recurrence. Gynecol Oncol 142(1):115–119
Chan YM, Ng TY, Ngan HY, Wong LC (2002) Monitoring of serum squamous cell carcinoma antigen levels in invasive cervical cancer: is it cost-effective? Gynecol Oncol 84(1):7–11
Kubik S, Moszynska-Zielinska M, Fijuth J, Tomalczyk A, Jesionek-Kupnicka D, Ura L, Gottwald LM (2019) Assessment of the relationship between serum squamous cell carcinoma antigen (SCC-Ag) concentration in patients with locally advanced squamous cell carcinoma of the uterine cervix and the risk of relapse. Prz Menopauzalny 18(1):23–26
Grivennikov SI, Greten FR, Karin M (2010) Immunity, inflammation, and cancer. Cell 140(6):883–899
McMillan DC (2013) The systemic inflammation-based Glasgow prognostic score: a decade of experience in patients with cancer. Cancer Treat Rev 39(5):534–540
Davies C, Pan H, Godwin J, Gray R, Arriagada R, Raina V, Abraham M, Medeiros Alencar VH, Badran A, Bonfill X et al (2013) Long-term effects of continuing adjuvant tamoxifen to 10 years versus stopping at 5 years after diagnosis of oestrogen receptor-positive breast cancer: ATLAS, a randomised trial. Lancet 381(9869):805–816
Kemal Y, Yucel I, Ekiz K, Demirag G, Yilmaz B, Teker F, Ozdemir M (2014) Elevated serum neutrophil to lymphocyte and platelet to lymphocyte ratios could be useful in lung cancer diagnosis. Asian Pac J Cancer Prev 15(6):2651–2654
Vesely MD, Schreiber RD (2013) Cancer immunoediting: antigens, mechanisms, and implications to cancer immunotherapy. Ann N Y Acad Sci 1284(1):1–5
Heeren AM, Kenter GG, Jordanova ES, de Gruijl TD (2015) CD14(+) macrophage-like cells as the linchpin of cervical cancer perpetrated immune suppression and early metastatic spread: a new therapeutic lead? Oncoimmunology 4(6):e1009296
Zhu M, Feng M, He F, Han B, Ma K, Zeng X, Liu Z, Liu X, Li J, Cao H et al (2018) Pretreatment neutrophil-lymphocyte and platelet-lymphocyte ratio predict clinical outcome and prognosis for cervical Cancer. Clin Chim Acta 483:296–302
Wu J, Chen M, Liang C, Su W (2017) Prognostic value of the pretreatment neutrophil-to-lymphocyte ratio in cervical cancer: a meta-analysis and systematic review. Oncotarget 8(8):13400–13412
Huang H, Liu Q, Zhu L, Zhang Y, Lu X, Wu Y, Liu L (2019) Prognostic value of preoperative systemic immune-inflammation index in patients with cervical cancer. Sci Rep 9(1):3284
Zheng RR, Huang M, Jin C, Wang HC, Yu JT, Zeng LC, Zheng FY, Lin F (2016) Cervical cancer systemic inflammation score: a novel predictor of prognosis. Oncotarget 7(12):15230–15242
Jiang K, Ai Y, Li Y, Jia L (2022) Nomogram models for the prognosis of cervical cancer: a SEER-based study. Front Oncol 12:961678
Cui L, Yu T, Kan Y, Dong Y, Luo Y, Jiang X (2022) Multi-parametric MRI-based peritumoral radiomics on prediction of lymph-vascular space invasion in early-stage cervical cancer. Diagn Interv Radiol 28(4):312–321
Du W, Wang Y, Li D, Xia X, Tan Q, Xiong X, Li Z (2021) Preoperative prediction of lymphovascular space invasion in cervical cancer with radiomics -based nomogram. Front Oncol 11:637794
Yu Z, Zhihui Q, Linrui L, Long L, Qibing W (2023) Machine learning-based models for assessing postoperative risk factors in patients with cervical cancer. Acad Radiol. https://doi.org/10.1016/j.acra.2023.09.031
Wu Y, Wang S, Chen Y, Liao Y, Yin X, Li T, Wang R, Luo X, Xu W, Zhou J et al (2023) A multicenter study on preoperative assessment of lymphovascular space invasion in early-stage cervical cancer based on multimodal MR radiomics. J Magn Reson Imaging 58(5):1638–1648
Acknowledgements
This study was funded by the Wuxi Taihu Lake Talent Plan, Support for Leading Talents in Medical and Health Profession. We thank Chang Xiong for her help in statistics and analysis of data.
Funding
This study was funded by the Wuxi Taihu Lake Talent Plan, Support for Leading Talents in Medical and Health Profession.
Author information
Authors and Affiliations
Contributions
QG: project development, data collection, data analysis, manuscript writing. YG: data analysis, Manuscript writing. YL: data analysis, manuscript writing. WL: data analysis. ZZ: data collection. YM: data collection. XX: data analysis, manuscript writing.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
This research was approved by the Ethics Committee of the Affiliated Hospital of Jiangnan University (No. LS2022040).
Consent to participate
Written informed consent was obtained from individual or guardian participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Guo, Q., Gao, Y., Lin, Y. et al. A nomogram of preoperative indicators predicting lymph vascular space invasion in cervical cancer. Arch Gynecol Obstet 309, 2079–2087 (2024). https://doi.org/10.1007/s00404-024-07385-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-024-07385-6