Abstract
Introduction
Successful frozen-thawed embryo transfer (FTET) depends on multiple factors among which the woman’s vaginal microbiota has recently been considered important. Using probiotic products, such as Lactovag in infertile women, the vaginal microbiome can become close to the healthy status.
Objectives
The aim of this study was to evaluate the effect of Lactovag on normalizing vaginal microbiome, as well as its role in improving pregnancy outcomes in FTET cycles.
Patients and methods
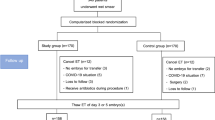
This randomized blinded clinical trial was conducted on 103 patients undergoing Assisted Reproductive Technology (ART) treatment at a tertiary university-based hospital between January and August of 2019. In the experiment group, the vaginal suppository Lactavag was prescribed, whereas in the control group, patients did not receive any microbiome supplements. Then, the pregnancy rate was compared in the two groups.
Results
There were no significant differences in baseline characteristics between the two study groups (p > 0.05). Positive B hCG was present in 28% (n = 26) of women, clinical pregnancy was achieved in 23.4% (n = 22) of them and fetal heart rate was detected in 21.3% (n = 20). These proportions were higher in the Lactovag group, although these differences were not significant (p > 0.05). Results showed that although transferring fetuses with grade A increased the odds of pregnancy with 1.53 (p = 0.001) folds, this ratio would be improved using Lactovag;1.68 (P value = 0.008).
Conclusions
It seems that the vaginal microbiota critically interplays with women's health and reproduction. A probiotic agent such as Lactovag can be useful in normalizing this environment and improving pregnancy outcomes in infertile women.

Similar content being viewed by others
Data availability
The data is available per request from corresponding author.
References
Agarwal A, Mulgund A, Hamada A, Chyatte MR (2015) A unique view on male infertility around the globe. Reprod Biol Endocrinol 26(13):37. https://doi.org/10.1186/s12958-015-0032-1
Petropanagos A, Cattapan A, Baylis F, Leader A (2015) Social egg freezing: risk, benefits and other considerations. CMAJ 187(9):666–669. https://doi.org/10.1503/cmaj.141605
Cho I, Blaser MJ (2012) The human microbiome: at the interface of health and disease. Nat Rev Genet 13(4):260–270. https://doi.org/10.1038/nrg3182
Oakley BB, Fiedler TL, Marrazzo JM, Fredricks DN (2008) Diversity of human vaginal bacterial communities and associations with clinically defined bacterial vaginosis. Appl Environ Microbiol 74(15):4898–4909. https://doi.org/10.1128/AEM.02884-07
Redondo-Lopez V, Cook RL, Sobel JD (1990) Emerging role of lactobacilli in the control and maintenance of the vaginal bacterial microflora. Rev Infect Dis 12(5):856–872. https://doi.org/10.1093/clinids/12.5.856
Cribby S, Taylor M, Reid G (2008) Vaginal microbiota and the use of probiotics. Interdisciplinary perspectives on infectious diseases. Interdiscip Perspect Infect Dis. 2008:256490. https://doi.org/10.1155/2008/256490
Simoes JA, Aroutcheva A, Heimler I, Shott S, Faro S (2001) Bacteriocin susceptibility of Gardnerella vaginalis and its relationship to biotype, genotype, and metronidazole susceptibility. Am J Obstet Gynecol 185(5):1186–1190. https://doi.org/10.1067/mob.2001.118144
van Oostrum N, De Sutter P, Meys J, Verstraelen H (2013) Risks associated with bacterial vaginosis in infertility patients: a systematic review and meta-analysis. Hum Reprod 28(7):1809–1815. https://doi.org/10.1093/humrep/det096
Haahr T, Jensen J, Thomsen L, Duus L, Rygaard K, Humaidan P (2016) Abnormal vaginal microbiota may be associated with poor reproductive outcomes: a prospective study in IVF patients. Hum Reprod 31(4):795–803. https://doi.org/10.1093/humrep/dew026
Tachedjian G, Aldunate M, Bradshaw CS, Cone RA (2017) The role of lactic acid production by probiotic Lactobacillus species in vaginal health. Res Microbiol 168(9–10):782–792. https://doi.org/10.1016/j.resmic.2017.04.001
Dominguez-Bello MG, Costello EK, Contreras M, Magris M, Hidalgo G, Fierer N et al (2010) Delivery mode shapes the acquisition and structure of the initial microbiota across multiple body habitats in newborns. Proc Natl Acad Sci USA 107(26):11971–11975. https://doi.org/10.1073/pnas.1002601107
Salah RM, Allam AM, Magdy AM, Mohamed AS (2013) Bacterial vaginosis and infertility: cause or association? Eur J Obstet Gynecol Reprod Biol 167(1):59–63. https://doi.org/10.1016/j.ejogrb.2012.10.031
Swidsinski A, Verstraelen H, Loening-Baucke V, Swidsinski S, Mendling W, Halwani Z (2013) Presence of a polymicrobial endometrial biofilm in patients with bacterial vaginosis. PLoS ONE 8(1):e53997. https://doi.org/10.1371/journal.pone.0053997
Mitchell CM, Haick A, Nkwopara E, Garcia R, Rendi M, Agnew K et al (2015) Colonization of the upper genital tract by vaginal bacterial species in nonpregnant women. Am J Obstet Gynecol 212(5):611.e1–9. https://doi.org/10.1016/j.ajog.2014.11.043
Sirota I, Zarek SM, Segars JH (2014) Potential influence of the microbiome on infertility and assisted reproductive technology. Semin Reprod Med. 32(1):35–42. https://doi.org/10.1055/s-0033-1361821
Schmitt C, Sobel JD, Meriwether C (1992) Bacterial vaginosis: treatment with clindamycin cream versus oral metronidazole. Obstet Gynecol 79(6):1020–1023
Reid G, Seidenfeld A (1997) Drug resistance amongst uropathogens isolated from women in a suburban population: laboratory findings over 7 years. Can J Urol 4(4):432–437
Heinemann C, Reid G (2005) Vaginal microbial diversity among postmenopausal women with and without hormone replacement therapy. Can J Microbiol 51(9):777–781. https://doi.org/10.1139/w05-070
Fredricks DN, Fiedler TL, Marrazzo JM (2005) Molecular identification of bacteria associated with bacterial vaginosis. N Engl J Med 353(18):1899–1911. https://doi.org/10.1056/NEJMoa043802
Burton JP, Reid G (2002) Evaluation of the bacterial vaginal flora of 20 postmenopausal women by direct (Nugent score) and molecular (polymerase chain reaction and denaturing gradient gel electrophoresis) techniques. J Infect Dis 186(12):1770–1780. https://doi.org/10.1086/345761
Burton JP, Cadieux PA, Reid G (2003) Improved understanding of the bacterial vaginal microbiota of women before and after probiotic instillation. Appl Environ Microbiol 69(1):97–101. https://doi.org/10.1128/aem.69.1.97-101.2003
Devillard E, Burton JP, Hammond J-A, Lam D, Reid G (2004) Novel insight into the vaginal microflora in postmenopausal women under hormone replacement therapy as analyzed by PCR-denaturing gradient gel electrophoresis. Eur J Obstet Gynecol Reprod Biol 117(1):76–81. https://doi.org/10.1016/j.ejogrb.2004.02.001
Hill JE, Goh SH, Money DM, Doyle M, Li A, Crosby WL et al (2005) Characterization of vaginal microflora of healthy, nonpregnant women by chaperonin-60 sequence-based methods. Am J Obstet Gynecol 193(3 Pt 1):682–692. https://doi.org/10.1016/j.ajog.2005.02.094
Antonio MA, Hawes SE, Hillier SL (1999) The identification of vaginal Lactobacillus species and the demographic and microbiologic characteristics of women colonized by these species. J Infect Dis 180(6):1950–1956. https://doi.org/10.1086/315109
Vásquez A, Jakobsson T, Ahrné S, Forsum U, Molin G (2002) Vaginal Lactobacillus flora of healthy Swedish women. J Clin Microbiol 40(8):2746–2749. https://doi.org/10.1128/jcm.40.8.2746-2749.2002
Galask RP (1988) Vaginal colonization by bacteria and yeast. Am J Obstet Gynecol 158(4):993–995. https://doi.org/10.1016/0002-9378(88)90111-1
Funding
No funding was received for conducting this research.
Author information
Authors and Affiliations
Contributions
All authors passed four criteria for authorship contribution based on recommendations of the International Committee of Medical Journal Editors. FD and ZRa participated in the Conception and design of the study, library searches and assembling relevant literature, critical review of the paper, supervising the writing of the paper, and Database management. ZRe, FA, ME, SH and EF participated in Data collection, library searches and assembling relevant literature, writing the article, and critical review of the report. All Authors read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they do not have any conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tanha, F.D., Rahmani, Z., Rezaei, Z. et al. The effect of normalizing vaginal microbiome using Lactovag in improving pregnancy outcomes in frozen embryo transfer cycles: a randomized clinical trial. Arch Gynecol Obstet 308, 1587–1592 (2023). https://doi.org/10.1007/s00404-023-07147-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-023-07147-w