Abstract
Purpose
Concurrent cisplatin-based chemotherapy and radiotherapy (CCRT) plus brachytherapy is the standard treatment for locally advanced cervical cancer (LACC). Platinum-based neoadjuvant chemotherapy (NACT) followed by radical hysterectomy is an alternative for patients with stage IB2–IIB disease. Therefore, the correct pre-treatment staging is essential to the proper management of this disease. Pelvic magnetic resonance imaging (MRI) is the gold standard examination but studies about MRI accuracy in the detection of lymph node metastasis (LNM) in LACC patients show conflicting data. Machine learning (ML) is emerging as a promising tool for unraveling complex non-linear relationships between patient attributes that cannot be solved by traditional statistical methods. Here we investigated whether ML might improve the accuracy of MRI in the detection of LNM in LACC patients.
Methods
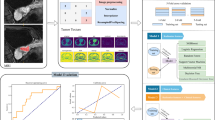
We analyzed retrospectively LACC patients who underwent NACT and radical hysterectomy from 2015 to 2020. Demographic, clinical and MRI characteristics before and after NACT were collected, as well as information about post-surgery histopathology. Random features elimination wrapper was used to determine an attribute core set. A ML algorithm, namely Extreme Gradient Boosting (XGBoost) was trained and validated with tenfold cross-validation. The performances of the algorithm were assessed.
Results
Our analysis included n.92 patients. FIGO stage was IB2 in n.4/92 (4.3%), IB3 in n.42/92 (45%), IIA1 in n.1/92 (1.1%), IIA2 in n.16/92 (17.4%) and IIB in n.29/92 (31.5%). Despite detected neither at pre-treatment and post-treatment MRI in any patients, LNM occurred in n.16/92 (17%) patients. The attribute core set used to train ML algorithms included grading, histotypes, age, parity, largest diameter of lesion at either pre- and post-treatment MRI, presence/absence of fornix infiltration at pre-treatment MRI and FIGO stage. XGBoost showed a good performance (accuracy 89%, precision 83%, recall 78%, AUROC 0.79).
Conclusions
We developed an accurate model to predict LNM in LACC patients in NACT, based on a ML algorithm requiring few easy-to-collect attributes.



Similar content being viewed by others
Data availability
Data are not freely available due to local Ethics Committee privacy issues. Authors will consider data sharing upon specific request to local Ethics Committee.
References
Frumovitz M, Sun CC, Schover LR, Munsell MF, Jhingran A, Wharton JT et al (2005) Quality of life and sexual functioning in cervical cancer survivors. J Clin Oncol 23(30):7428–7436
Small W, Bacon MA, Bajaj A, Chuang LT, Fisher BJ, Harkenrider MM et al (2017) Cervical cancer: a global health crisis. Cancer 123(13):2404–2412
Arezzo F, Cormio G, Loizzi V, Cazzato G, Cataldo V, Lombardi C et al (2021) HPV-negative cervical cancer: a narrative review. Diagnostics 11(6):952
Marth C, Landoni F, Mahner S, McCormack M, Gonzalez-Martin A, Colombo N et al (2018) Cervical cancer: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol 29(Suppl 4):iv262
Lee SI, Atri M (2019) 2018 FIGO staging system for uterine cervical cancer: enter cross-sectional imaging. Radiology 292(1):15–24
Biewenga P, van der Velden J, Mol BWJ, Stalpers LJA, Schilthuis MS, van der Steeg JW et al (2011) Prognostic model for survival in patients with early stage cervical cancer. Cancer 117(4):768–776
Bourgioti C, Chatoupis K, Moulopoulos LA (2016) Current imaging strategies for the evaluation of uterine cervical cancer. World J Radiol 8(4):342–354
Ruengkhachorn I, Therasakvichya S, Warnnissorn M, Leelaphatanadit C, Sangkarat S, Srisombat J (2015) Pathologic risk factors and oncologic outcomes in early-stage cervical cancer patients treated by radical hysterectomy and pelvic lymphadenectomy at a Thai University Hospital: a 7 year retrospective review. Asian Pac J Cancer Prev 16(14):5951–5956
Matsuo K, Shimada M, Saito T, Takehara K, Tokunaga H, Watanabe Y et al (2018) Risk stratification models for para-aortic lymph node metastasis and recurrence in stage IB-IIB cervical cancer. J Gynecol Oncol 29(1):e11
Sakuragi N, Satoh C, Takeda N, Hareyama H, Takeda M, Yamamoto R et al (1999) Incidence and distribution pattern of pelvic and paraaortic lymph node metastasis in patients with Stages IB, IIA, and IIB cervical carcinoma treated with radical hysterectomy. Cancer 85(7):1547–1554
Arezzo F, La Forgia D, Venerito V, Moschetta M, Tagliafico AS, Lombardi C et al (2021) A machine learning tool to predict the response to neoadjuvant chemotherapy in patients with locally advanced cervical cancer. Appl Sci 11(2):823
Rose PG, Ali S, Watkins E, Thigpen JT, Deppe G, Clarke-Pearson DL et al (2007) Long-term follow-up of a randomized trial comparing concurrent single agent cisplatin, cisplatin-based combination chemotherapy, or hydroxyurea during pelvic irradiation for locally advanced cervical cancer: a Gynecologic Oncology Group Study. J Clin Oncol 25(19):2804–2810
Mirnezami R, Nicholson J, Darzi A (2012) Preparing for precision medicine. N Engl J Med 366(6):489–491
Lambin P, Rios-Velazquez E, Leijenaar R, Carvalho S, van Stiphout RGPM, Granton P et al (2012) Radiomics: extracting more information from medical images using advanced feature analysis. Eur J Cancer 48(4):441–446
Scalco E, Rizzo G (2017) Texture analysis of medical images for radiotherapy applications. Br J Radiol 90(1070):20160642
Neoadjuvant Chemotherapy for Locally Advanced Cervical Cancer Meta-analysis Collaboration (2003) Neoadjuvant chemotherapy for locally advanced cervical cancer: a systematic review and meta-analysis of individual patient data from 21 randomised trials. Eur J Cancer 39(17):2470–2486
Lucia F, Visvikis D, Desseroit MC, Miranda O, Malhaire JP, Robin P et al (2018) Prediction of outcome using pretreatment 18F-FDG PET/CT and MRI radiomics in locally advanced cervical cancer treated with chemoradiotherapy. Eur J Nucl Med Mol Imaging 45(5):768–786
Venerito V, Angelini O, Cazzato G, Lopalco G, Maiorano E, Cimmino A et al (2021) A convolutional neural network with transfer learning for automatic discrimination between low and high-grade synovitis: a pilot study. Intern Emerg Med 16(6):1457–1465
Cazzato G, Colagrande A, Cimmino A, Arezzo F, Loizzi V, Caporusso C et al (2021) Artificial intelligence in dermatopathology: new insights and perspectives. Dermatopathology 8(3):418–425
Johnson KW, Torres Soto J, Glicksberg BS, Shameer K, Miotto R, Ali M et al (2018) Artificial Intelligence in Cardiology. J Am Coll Cardiol 71(23):2668–2679
Pandit A, Radstake TRDJ (2020) Machine learning in rheumatology approaches the clinic. Nat Rev Rheumatol febbraio 16(2):69–70
Baldini C, Ferro F, Luciano N, Bombardieri S, Grossi E (2018) Artificial neural networks help to identify disease subsets and to predict lymphoma in primary Sjögren’s syndrome. Clin Exp Rheumatol 36(Suppl 112(3)):137–144
Eisenhauer EA, Therasse P, Bogaerts J, Schwartz LH, Sargent D, Ford R et al (2009) New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer 45(2):228–247
Cohen JF, Korevaar DA, Altman DG, Bruns DE, Gatsonis CA, Hooft L et al (2016) STARD 2015 guidelines for reporting diagnostic accuracy studies: explanation and elaboration. BMJ Open 6(11):e012799
Heus P, Damen JAAG, Pajouheshnia R, Scholten RJPM, Reitsma JB, Collins GS et al (2018) Poor reporting of multivariable prediction model studies: towards a targeted implementation strategy of the TRIPOD statement. BMC Med 16(1):120
Venerito V, Lopalco G, Abbruzzese A, Colella S, Morrone M, Tangaro S et al (2022) A machine learning approach to predict remission in patients with psoriatic arthritis on treatment with secukinumab. Front Immunol 13:917939
Arezzo F, Loizzi V, La Forgia D, Moschetta M, Tagliafico AS, Cataldo V et al (2021) Radiomics analysis in ovarian cancer: a narrative review. Appl Sci 11(17):7833
Venerito V, Emmi G, Cantarini L, Leccese P, Fornaro M, Fabiani C et al (2022) Validity of machine learning in predicting giant cell arteritis flare after glucocorticoids tapering. Front Immunol 13:860877
Casalino G, Castellano G, Consiglio A et al. (2021) MicroRNA expression classification for pediatric multiple sclerosis identification. J Ambient Intell Human Comput. https://doi.org/10.1007/s12652-021-03091-2
Kamel E, Sheikh S, Huang X (2020) Data-driven predictive models for residential building energy use based on the segregation of heating and cooling days. Energy 206:118045
LeCun Y, Bengio Y, Hinton G (2015) Deep learning. Nature 521(7553):436–444
Petrillo A, Fusco R, Di Bernardo E, Petrosino T, Barretta ML, Porto A et al (2022) Prediction of breast cancer histological outcome by radiomics and artificial intelligence analysis in contrast-enhanced mammography. Cancers 14(9):2132
Toledo T (2021) sknet: a python framework for machine learning in complex networks. J Open Source Softw 6:3864
Altukhova O (2020) Choice of method imputation missing values for obstetrics clinical data. Proced Computer Sci. https://doi.org/10.1016/j.procs.2020.09.093
Rawashdeh H, Awawdeh S, Shannag F, Henawi E, Faris H, Obeid N et al (2020) Intelligent system based on data mining techniques for prediction of preterm birth for women with cervical cerclage. Comput Biol Chem 85:107233
Xiao M, Yan C, Fu B, Yang S, Zhu S, Yang D et al (2020) Risk prediction for postpartum depression based on random forest. Zhong Nan Da Xue Xue Bao Yi Xue Ban 45(10):1215–1222
Khalilia M, Chakraborty S, Popescu M (2011) Predicting disease risks from highly imbalanced data using random forest. BMC Med Inform Decis Mak 11:51
Krstajic D, Buturovic LJ, Leahy DE, Thomas S (2014) Cross-validation pitfalls when selecting and assessing regression and classification models. J Cheminformatics 6(1):10
Ranganathan S, Nakai K, Schonbach C (2019) Encyclopedia of bioinformatics and computational biology, vol 1–3. Elsevier, Amsterdam
Venerito V, Angelini O, Fornaro M, Cacciapaglia F, Lopalco G, Iannone F (2022) A machine learning approach for predicting sustained remission in rheumatoid arthritis patients on biologic agents. J Clin Rheumatol 28(2):e334–e339
Kuhn M, Johnson K (2013) An introduction to feature selection. In: Kuhn M, Johnson K (eds) Applied predictive modeling. Springer, New York, pp 487–519. https://doi.org/10.1007/978-1-4614-6849-3_19
Arezzo F, Cormio G, La Forgia D, Santarsiero CM, Mongelli M, Lombardi C et al (2022) A machine learning approach applied to gynecological ultrasound to predict progression-free survival in ovarian cancer patients. Arch Gynecol Obstet. https://doi.org/10.1007/s00404-022-06578-1
Kim HS, Kim JY, Park NH, Kim K, Chung HH, Kim YB et al (2010) Matched-case comparison for the efficacy of neoadjuvant chemotherapy before surgery in FIGO stage IB1-IIA cervical cancer. Gynecol Oncol 119(2):217–224
Vizza E, Corrado G, Zanagnolo V, Tomaselli T, Cutillo G, Mancini E et al (2014) Neoadjuvant chemotherapy followed by robotic radical hysterectomy in locally advanced cervical cancer: a multi-institution study. Gynecol Oncol 133(2):180–185
Koh WJ, Abu-Rustum NR, Bean S, Bradley K, Campos SM, Cho KR et al (2019) Cervical cancer, version 3.2019, NCCN clinical practice guidelines in oncology. J Natl Compr Cancer Netw 17(1):64–84
Angioli R, Plotti F, Montera R, Aloisi A, Luvero D, Capriglione S et al (2012) Neoadjuvant chemotherapy plus radical surgery followed by chemotherapy in locally advanced cervical cancer. Gynecol Oncol 127(2):290–296
Shoji T, Takatori E, Furutake Y, Takada A, Nagasawa T, Omi H et al (2016) Phase II clinical study of neoadjuvant chemotherapy with CDDP/CPT-11 regimen in combination with radical hysterectomy for cervical cancer with a bulky mass. Int J Clin Oncol 21(6):1120–1127
Mori T, Makino H, Okubo T, Fujiwara Y, Sawada M, Kuroboshi H et al (2019) Multi-institutional phase II study of neoadjuvant irinotecan and nedaplatin followed by radical hysterectomy and the adjuvant chemotherapy for locally advanced, bulky uterine cervical cancer: A Kansai Clinical Oncology Group study (KCOG-G1201). J Obstet Gynaecol Res 45(3):671–678
Cazzato G, Colagrande A, Cimmino A, Caporusso C, Candance PMV, Trabucco SMR et al (2021) Urological melanoma: a comprehensive review of a rare subclass of mucosal melanoma with emphasis on differential diagnosis and therapeutic approaches. Cancers 13(17):4424
Rydzewska L, Tierney J, Vale CL, Symonds PR (2012) Neoadjuvant chemotherapy plus surgery versus surgery for cervical cancer. Cochrane Database Syst Rev 12:CD007406
Kim HS, Sardi JE, Katsumata N, Ryu HS, Nam JH, Chung HH et al (2013) Efficacy of neoadjuvant chemotherapy in patients with FIGO stage IB1 to IIA cervical cancer: an international collaborative meta-analysis. Eur J Surg Oncol 39(2):115–124
Cazzato G, Colagrande A, Arezzo F, Resta L, Ingravallo G (2021) “Black ovaries”: an uncommon case of first systemic recurrence of melanoma. Reports 4(2):13
Gadducci A, Cosio S (2020) Neoadjuvant chemotherapy in locally advanced cervical cancer: review of the literature and perspectives of clinical research. Anticancer Res 40(9):4819–4828
Chen H, Liang C, Zhang L, Huang S, Wu X (2008) Clinical efficacy of modified preoperative neoadjuvant chemotherapy in the treatment of locally advanced (stage IB2 to IIB) cervical cancer: randomized study. Gynecol Oncol 110(3):308–315
Gadducci A, Teti G, Barsotti C, Tana R, Fanucchi A, Orlandini C et al (2010) Clinicopathological variables predictive of clinical outcome in patients with FIGO stage Ib2-IIb cervical cancer treated with cisplatin-based neoadjuvant chemotherapy followed by radical hysterectomy. Anticancer Res 30(1):201–208
Uegaki K, Shimada M, Sato S, Deura I, Naniwa J, Sato S et al (2014) Outcome of stage IB2-IIB patients with bulky uterine cervical cancer who underwent neoadjuvant chemotherapy followed by radical hysterectomy. Int J Clin Oncol 19(2):348–353
Benedetti-Panici P, Greggi S, Scambia G, Amoroso M, Salerno MG, Maneschi F et al (1998) Long-term survival following neoadjuvant chemotherapy and radical surgery in locally advanced cervical cancer. Eur J Cancer 34(3):341–346
Balleyguier C, Sala E, Da Cunha T, Bergman A, Brkljacic B, Danza F et al (2011) Staging of uterine cervical cancer with MRI: guidelines of the European Society of Urogenital Radiology. Eur Radiol 21(5):1102–1110
Bipat S, Glas AS, van der Velden J, Zwinderman AH, Bossuyt PMM, Stoker J (2003) Computed tomography and magnetic resonance imaging in staging of uterine cervical carcinoma: a systematic review. Gynecol Oncol 91(1):59–66
Arezzo F, Cazzato G, Loizzi V, Ingravallo G, Resta L, Cormio G (2021) Peritoneal tuberculosis mimicking ovarian cancer: gynecologic ultrasound evaluation with histopathological confirmation. Gastroenterol Insights 12(2):278–282
Choi HJ, Roh JW, Seo SS, Lee S, Kim JY, Kim SK et al (2006) Comparison of the accuracy of magnetic resonance imaging and positron emission tomography/computed tomography in the presurgical detection of lymph node metastases in patients with uterine cervical carcinoma: a prospective study. Cancer 106(4):914–922
Narayan K, Hicks RJ, Jobling T, Bernshaw D, McKenzie AF (2001) A comparison of MRI and PET scanning in surgically staged loco-regionally advanced cervical cancer: potential impact on treatment. Int J Gynecol Cancer 11(4):263–271
Nanthamongkolkul K, Hanprasertpong J (2018) Predictive factors of pelvic lymph node metastasis in early-stage cervical cancer. Oncol Res Treat 41(4):194–198
Yu F, Chen Y, Huang L, Nie G (2016) Risk factors of node metastasis in cervical carcinoma. Eur J Gynaecol Oncol 37(5):662–665
Wu C, Li L, Xiao X, Sun A, Lin W, Li A (2019) Risk factors of regional lymph node metastasis in patients with cervical cancer. Open Life Sci 14:208–213
Minig L, Fagotti A, Scambia G, Salvo G, Patrono MG, Haidopoulos D et al (2018) Incidence of lymph node metastases in women with low-risk early cervical cancer (<2 cm) without lymph-vascular invasion. Int J Gynecol Cancer 28(4):788–793
Kilic C, Kimyon Comert G, Cakir C, Yuksel D, Codal B, Kilic F et al (2021) Recurrence pattern and prognostic factors for survival in cervical cancer with lymph node metastasis. J Obstet Gynaecol Res 47(6):2175–2184
Cai J, He X, Wang H, Dong W, Zhang Y, Zhao J et al (2021) Topographic distribution of lymph node metastasis in patients with stage IB1 cervical cancer: an analysis of 8314 lymph nodes. Radiat Oncol 16(1):54
Tekalegn Y, Sahiledengle B, Woldeyohannes D, Atlaw D, Degno S, Desta F et al (2022) High parity is associated with increased risk of cervical cancer: systematic review and meta-analysis of case-control studies. Womens Health 18:17455065221075904
Acknowledgements
The authors affiliated to the IRCCS Istituto Tumori “Giovanni Paolo II”, Bari, are responsible for the views expressed in this article, which do not necessarily represent the Institute.
Funding
This research received no external funding. The authors have no relevant financial or non-financial interests to disclose.
Author information
Authors and Affiliations
Contributions
FA and VL performed the study conception. GC and CL contributed to the study design. Material preparation and data collection were performed by VV, AC and MM. The first draft of the manuscript was written by FA and GC. VL, ES and CL performed the data visualization. The manuscript was reviewed by AK, GC and VL under the supervision of GC. The project was administrated by FA. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Ethical approval
The study was conducted in accordance with the Declaration of Helsinki, and the protocol was endorsed by the Scientific Board University of Bari, Bari, Italy (protocol code 6398, date of approval 10 June 2020).
Consent to participate
Informed consent was obtained from all subjects involved in the study at baseline consultation.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Arezzo, F., Cormio, G., Mongelli, M. et al. Machine learning applied to MRI evaluation for the detection of lymph node metastasis in patients with locally advanced cervical cancer treated with neoadjuvant chemotherapy. Arch Gynecol Obstet 307, 1911–1919 (2023). https://doi.org/10.1007/s00404-022-06824-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-022-06824-6