Abstract
Purpose
Pruritus during pregnancy is associated with adverse maternal, pregnancy, and neonatal outcomes. We opted to assess the association between term pruritus and long-term neuropsychiatric hospitalizations of the offspring.
Methods
In a population-based retrospective cohort study, the incidence of long-term neuropsychiatric hospitalizations was compared between offspring born to women with or without pruritus at term. Neuropsychiatric morbidity was assessed up to the age of 18 years according to ICD-9 codes associated with hospitalization of the offspring. A Kaplan–Meier survival curve was used to compare cumulative neuropsychiatric hospitalizations incidence and Cox proportional hazards models were used to control for confounders. The study included 226,918 deliveries of which 600 (0.26%) were in women with term pruritus.
Results
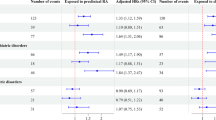
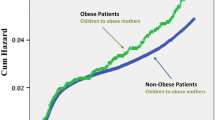
Offspring born to women with pruritus exhibited a higher rate of long-term neuropsychiatric hospitalizations, specifically due to developmental and neurodegenerative disorders. Kaplan–Meier survival curve demonstrated a significantly higher cumulative incidence of long-term neuropsychiatric hospitalizations in offspring of women with pruritus. Using several Cox proportional hazards models, being born to a woman with pruritus was independently associated with an increased risk of long-term neuropsychiatric hospitalizations.
Conclusions
Maternal term pruritus was found to be independently associated with long-term neuropsychiatric hospitalizations of the offspring.

Similar content being viewed by others
References
Tyler KH (2015) Physiological skin changes during pregnancy. Clin Obstet Gynecol 58(1):119–124. https://doi.org/10.1097/GRF.0000000000000077
Szczęch J, Wiatrowski A, Hirnle L, Reich A (2017) Prevalence and relevance of pruritus in pregnancy. Biomed Res Int 2017:4238139. https://doi.org/10.1155/2017/4238139
Bergman H, Melamed N, Koren G (2013) Pruritus in pregnancy: treatment of dermatoses unique to pregnancy. Can Fam Physician 59(12):1290–1294
Beard MP, Millington GW (2012) Recent developments in the specific dermatoses of pregnancy. Clin Exp Derm 37(1):1–5. https://doi.org/10.1111/j.1365-2230.2011.04173.x
Hallaji Z, Mortazavi H, Ashtari S, Nikoo A, Abdollahi M, Nasimi M (2016) Pemphigoid gestationis: clinical and histologic features of 23 patients. Int J Womens Derm 3(2):86–90. https://doi.org/10.1016/j.ijwd.2016.11.004
Liu C, Gao J, Liu J et al (2020) Intrahepatic cholestasis of pregnancy is associated with an increased risk of gestational diabetes and preeclampsia. Ann Transl Med 8(23):1574. https://doi.org/10.21037/atm-20-4879
Freud A, Wainstock T, Sheiner E et al (2019) Maternal chorioamnionitis and long term neurological morbidity in the offspring. Eur J Paediatr Neurol 23(3):484–490. https://doi.org/10.1016/j.ejpn.2019.03.005
Gasparrini E, Rosati F, Gaetti MT (2019) Long-term follow-up of newborns at neurological risk. Ital J Pediatr 45(1):38. https://doi.org/10.1186/s13052-019-0629-7
Fitzgerald E, Hor K, Drake AJ (2020) Maternal influences on fetal brain development: The role of nutrition, infection and stress, and the potential for intergenerational consequences. Early Hum Dev 150:105190. https://doi.org/10.1016/j.earlhumdev.2020.105190
Buss C, Entringer S, Swanson JM, Wadhwa PD (2012) The role of stress in brain development: the gestational environment’s long-term effects on the brain. Cerebrum 2012:4
McMillin M, DeMorrow S (2016) Effects of bile acids on neurological function and disease. FASEB J 30(11):3658–3668. https://doi.org/10.1096/fj.201600275R
Sadik CD, Lima AL, Zillikens D (2016) Pemphigoid gestationis: toward a better understanding of the etiopathogenesis. Clin Derm 34(3):378–382. https://doi.org/10.1016/j.clindermatol.2016.02.010
Šimják P, Pařízek A, Vítek L et al (2015) Fetal complications due to intrahepatic cholestasis of pregnancy. J Perinat Med 43(2):133–139. https://doi.org/10.1515/jpm-2014-0089
Farahvar S, Walfisch A, Sheiner E (2019) Gestational diabetes risk factors and long-term consequences for both mother and offspring: a literature review. Expert Rev Endocrinol Metab 14(1):63–74. https://doi.org/10.1080/17446651.2018.1476135
Nahum Sacks K, Friger M, Shoham-Vardi I, Sergienko R, Spiegel E, Landau D, Sheiner E (2019) Long-term neuropsychiatric morbidity in children exposed prenatally to preeclampsia. Early Hum Dev 130:96–100. https://doi.org/10.1016/j.earlhumdev.2019.01.016
Luo M, Tang M, Jiang F et al (2021) Intrahepatic cholestasis of pregnancy and associated adverse maternal and fetal outcomes: a retrospective case-control study. Gastroenterol Res Pract 2021:6641023. https://doi.org/10.1155/2021/6641023
Hämäläinen ST, Turunen K, Mattila KJ, Kosunen E, Sumanen M (2019) Intrahepatic cholestasis of pregnancy and comorbidity: a 44-year follow-up study. Acta Obstet Gynecol Scand 98(12):1534–1539. https://doi.org/10.1111/aogs.13695
Roth MM (2011) Pregnancy dermatoses: diagnosis, management, and controversies. Am J Clin Dermatol 12(1):25–41. https://doi.org/10.2165/11532010-000000000-00000
Geenes V, Lövgren-Sandblom A, Benthin L et al (2014) The reversed feto-maternal bile acid gradient in intrahepatic cholestasis of pregnancy is corrected by ursodeoxycholic acid. PLoS ONE 9(1):e83828. https://doi.org/10.1371/journal.pone.0083828
Monteiro-Cardoso VF, Corlianò M, Singaraja RR (2021) Bile acids: a communication channel in the gut-brain axis. Neuromolecular Med 23(1):99–117. https://doi.org/10.1007/s12017-020-08625-z
Elhakham D, Wainstock T, Sheiner E, Sergienko R, Pariente G (2020) Inter-pregnancy interval and long-term neurological morbidity of the offspring. Arch Gynecol Obstet 303(3):703–708. https://doi.org/10.1007/s00404-020-05788-9
Sarusi MM, Wainstock T, Sheiner E, Pariente G (2022) Maternal epilepsy- perinatal outcome and long-term neurological morbidity of the offspring: a population-based cohort study. Arch Gynecol Obstet 305(1):55–62. https://doi.org/10.1007/s00404-021-06114-7
Davidesko S, Pariente G, Wainstock T, Sheiner E (2021) Maternal known drug allergy and long-term neurological hospitalizations of the offspring. Am J Reprod Immunol 85(1):e13335. https://doi.org/10.1111/aji.13335
Neuhaus ZF, Gutvirtz G, Pariente G, Wainstock T, Landau D, Sheiner E (2020) Maternal obesity and long-term neuropsychiatric morbidity of the offspring. Arch Gynecol Obstet 301(1):143–149. https://doi.org/10.1007/s00404-020-05432-6
Pariente G, Wainstock T, Walfisch A, Landau D, Sheiner E (2019) Placental abruption and long-term neurological hospitalizations in the offspring. Paediatr Perinat Epidemiol 33(3):215–222. https://doi.org/10.1111/ppe.12553
Pataia V, Dixon PH, Williamson C (2017) Pregnancy and bile acid disorders. Am J Physiol Gastrointest Liver Physiol 313(1):G1 (Epub 2017 Apr 27)
Seikku L, Gissler M, Andersson S et al (2016) Asphyxia, neurologic morbidity, and perinatal mortality in early-term and postterm birth. Pediatrics 137(6):e20153334. https://doi.org/10.1542/peds.2015-3334
Funding
This research received no funding.
Author information
Authors and Affiliations
Contributions
Conceptualization, ES and GP; methodology, ES; software, ES; validation, ES; formal analysis, ES; investigation, OL and GP; resources, GP; data curation, ES; writing—original draft preparation, OL; writing—review and editing, OL, GP, ES, and DK; visualization, OL; supervision, GP and ES; project administration, GP All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
The study was conducted in accordance with the Declaration of Helsinki, and approved by the Institutional Review Board of Soroka University Medical Center (SUMC) (protocol code SOR-19-0357, date of approval 10 October 2019).
Consent to participate
Patient consent was waived due to the retrospective design using anonymous coding.
Consent to publish
Patient consent was waived due to the retrospective design using anonymous coding.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Levanony, O., Sheiner, E., Kluwgant, D. et al. Maternal term pruritus and long-term neuropsychiatric hospitalizations of the offspring. Arch Gynecol Obstet 308, 857–862 (2023). https://doi.org/10.1007/s00404-022-06742-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-022-06742-7