Abstract
Objective
To better understand the risk stratification and outcomes of gynecologic PEComas.
Methods
Clinicopathological features and outcomes of gynecologic PEComas cases reported in both English and Chinese literature before September, 2020 were evaluated. The efficacy of three proposed criteria were compared to verify their practicability in gynecologic PEComas. The Chi-square test and Cox proportional hazard model were performed for statistical analysis.
Results
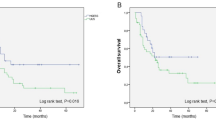
A total of 210 cases were retrieved: 95 from English literature and 115 from Chinese literature. The Flope criterion achieved an accuracy of 47% for detecting malignancy of gynecologic PEComas, 64.2% for the Schoolmeester criterion, and 63.8% for the WHO criterion. Both Chi-square test and uni-variate analysis showed that tumor size ≥ 5 cm, infiltrative growth pattern, mitotic rate ≥ 1/50 high per filed (HPF), high nuclear grade and cellularity, necrosis, and vascular invasion were significantly related to recurrence and/or metastasis (R/M) of gynecologic PEComas. Still only high mitotic rate (≥ 1/50 HPF), high nuclear grade and cellularity, and necrosis significantly influenced the long-term survival. Multi-variate analysis showed high nuclear grade and cellularity was an independent risk factor for R/M of gynecologic PEComas. No model was fitted for the death rate due to a small number of events. When defined malignant PEComas cases as meeting three or more out of six clinicopathologic features, the accuracy of such attempt was 62%, but the false-negative rate dropped by 37–55%.
Conclusions
Gynecologic PEComas with three or more high-risk factors may be considered as malignant. Further efforts should be invested to look for new potential prognostic factors.

Similar content being viewed by others
Data availability
The authors confirm that the data supporting the findings of this study within the article are available within this article and supplementary materials.
References
WHO Classification of Tumours Editorial Board (2020) WHO Classification of Tumours of Soft Tissue and Bone, 5th edn. IARC Press, Lyon, France
Bleeker JS, Quevedo JF, Folpe AL (2012) “Malignant” perivascular epithelioid cell neoplasm: risk stratification and treatment strategies. Sarcoma 2012:541626. https://doi.org/10.1155/2012/541626
Folpe AL, Mentzel T, Lehr HA, Fisher C, Balzer BL, Weiss SW (2005) Perivascular epithelioid cell neoplasms of soft tissue and gynecologic origin: a clinicopathologic study of 26 cases and review of the literature. Am J Surg Pathol 29(12):1558–1575. https://doi.org/10.1097/01.pas.0000173232.22117.37
Conlon N, Soslow RA, Murali R (2015) Perivascular epithelioid tumours (PEComas) of the gynaecological tract. J Clin Pathol 68(6):418–426. https://doi.org/10.1136/jclinpath-2015-202945
Schoolmeester JK, Howitt BE, Hirsch MS, Dal CP, Quade BJ, Nucci MR (2014) Perivascular epithelioid cell neoplasm (PEComas) of the gynecologic tract: clinicopathologic and immunohistochemical characterization of 16 cases. Am J Surg Pathol 38(2):176–188. https://doi.org/10.1097/PAS.0000000000000133
Oluwole F (2008) Perivascular epithelioid cell tumor (PEComa) of the uterus: an outcome-based clinicopathologic analysis of 41 reported cases. Adv Anat Pathol 15(2):63–75. https://doi.org/10.1097/PAP.0b013e31816613b0
Bennett JA, Braga AC, Pinto A, Vijver KVD, Oliva E (2018) Uterine PEComas: a morphologic, immunohistochemical, and molecular analysis of 32 tumors. Am J Surg Pathol 42(10):1. https://doi.org/10.1097/PAS.0000000000001119
Martin AA, Adley BP (2017) Predicting the behavior of perivascular epithelioid cell tumors of the uterine corpus. Arch Pathol Lab Med 141(3):463–469. https://doi.org/10.5858/arpa.2016-0092-RS
Bing Z, Yao Y, Pasha T, Tomaszewski JE, Zhang PJ (2012) p53 in pure epithelioid PEComa: an immunohistochemistry study and gene mutation analysis. Int J Surg Pathol 20(2):115–122. https://doi.org/10.1177/1066896912441829
Liu F, Zhang R, Wang Z-Y, Xia Q, Shen Q, Shi S, Tu P, Shi Q, Zhou X, Rao Q (2014) Malignant perivascular epithelioid cell tumor (PEComa) of cervix with TFE3 gene rearrangement: a case report. Int J Clin Exp Pathol 7(9):6409–6414
Oluwole F, Vinita P, Yesim Y, Rajan MM, Linglei Ma, Denise H, Qumsiyeh MB, Pei H (2004) Perivascular epithelioid cell tumor (PEComa) of the uterine cervix associated with intraabdominal “PEComatosis”: A clinicopathological study with comparative genomic hybridization analysis. World J Surg Oncol 2(1):35. https://doi.org/10.1186/1477-7819-2-35
Agaram NP, Sung YS, Zhang L et al (2015) Dichotomy of genetic abnormalities in PEComas with therapeutic implications[J]. Am J Surg Pathol 39(6):813. https://doi.org/10.1097/PAS.0000000000000389
Roberta S, Jones RL, Jean-Yves B, Axel LC, Salvatore P, Georgios A, Olivier M, Giovanni F, Elena F, Rossella B, Silvia S, Mehdi B, Federica G, Armelle D, Nadia H, Marta S, Alessandro G, Paola C, Dei Tos Angelo P, Casali PG (2019) Role of chemotherapy, VEGFR inhibitors, and mTOR inhibitors in advanced perivascular epithelioid cell tumors (PEComas). Clin Cancer Res 25(17):5295–5300. https://doi.org/10.1158/1078-0432.CCR-19-0288
Uhlenhopp DJ, West J, Heckart J, Campbell R, Elhaddad A (2020) Rapidly enlarging malignant abdominal PEComa with hepatic metastasis: a promising initial response to sirolimus following surgical excision of primary tumor. Oxf Med Case Rep 2020(3):013. https://doi.org/10.1093/omcr/omaa013
Funding
This work was supported by Hunan Provincial Key Research and Development Project, China (2020SK2073).
Author information
Authors and Affiliations
Contributions
Great thanks for all authors’ contribution to this paper. YJ: statistical analysis and drafting; XL: data acquisition; QX: data acquisition. SZ: instruction for statistics. QW: critical revision; KG: critical revision; LC: study design and supervision. All authors commented on previous version of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Jiang, Y., Liu, X., Zhang, S. et al. Risk stratification and outcomes in 210 gynecologic perivascular epithelioid cell tumors (PEComas) cases. Arch Gynecol Obstet 307, 681–687 (2023). https://doi.org/10.1007/s00404-022-06470-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-022-06470-y