Abstract
Purpose
The purpose to the study was to determine the relationship, if any, between the placental location site and antepartum complications of pregnancy.
Methods
A University research librarian conducted a comprehensive literature search using the search engines PubMed and Web of Science. The search terms were “placental location” AND “pregnancy complications” OR “perinatal complications. There were no limits put on the years of the search.
Results
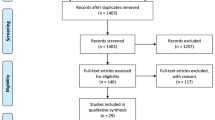
The search identified 110 articles. After reviewing all the abstracts, relevant full articles, and references of full articles, there were 22 articles identified specific to antepartum complications. Central + fundal locations compared to all lateral were associated with a lower risk of hypertension during pregnancy RR = 0.47, 95% CI: 0.31–0.71]. Central location compared to all lateral was also associated with lower risk of hypertension during pregnancy [RR = 0.39, 95% CI: 0.26–0.59]. Placenta locations in the lower uterine segment were associated with greater risk of antepartum hemorrhage (APH) [RR = 2.99, 95% CI: 1.16–7.75] compared to above the lower uterine segment. No differences were observed in placental locations and gestational diabetes (GDM), preterm prelabor rupture of membranes (PPROM), preterm delivery (PTD) or on a placental abruption.
Conclusion
Central and fundal location sites and central location alone decreased the risk of hypertension during pregnancy. Low uterine segment location sites increased the risk for APH. There were no effects of placenta location sites on the development of GDM, PPROM, PTD or abruption.







Similar content being viewed by others
References
Booth RT, Wood C, Beard RW, Gibson JR, Pinkerton JH (1962) Significance of site of placental attachment in uterus. Br Med J 1(5294):1732–1734
Fung TY, Sahota DS, Lau TK, Leung TY, Chan LW, Chung TK (2011) Placental site in the second trimester of pregnancy and its association with subsequent obstetric outcome. Prenat Diagn 31(6):548–554
Kore SJ, Khot R, Supe P, Kanavia D, Thunga C, Nandanwar Y (2017) Prediction of pre-eclampsia: role of placental laterality by ultrasonography. New Indian J Obstet Gynaecol 5(2017):5
Liberati M, Rotmensch S, Zannolli P, Perrino S, Celentano C, Tiboni GM, Bellati U (1997) Uterine artery Doppler velocimetry in pregnant women with lateral placentas. J Perinat Med 25(2):133–138
J.P. Pai MV, (2005) Placental laterality by ultrasound- a simple yet reliable predictive test for preeclampsia. J Obstet Gynecol India 55(5):431–433
Yousuf S, Ahmad A, Qadir S, Gul S, Tali SH, Shaheen F, Akhtar S, Dar R (2016) Utility of placental laterality and uterine artery doppler abnormalities for prediction of preeclampsia. J Obstet Gynaecol India 66(Suppl 1):212–216
Zia S (2013) Placental location and pregnancy outcome. J Turk Ger Gynecol Assoc 14(4):190–193
Seckin KD, Cakmak B, Karsli MF, Yeral MI, Gultekin IB, Oz M, Danisman N (2015) Is lateral localisation of placenta a risk factor for adverse perinatal outcomes? J Obstet gynaecol 35(7):696–698
Magann EF, Doherty DA, Turner K, Lanneau GS Jr, Morrison JC, Newnham JP (2007) Second trimester placental location as a predictor of an adverse pregnancy outcome. J Perinatol 27(1):9–14
Bieniarz J (1959) The patho-mechanism of late pregnancy toxemia and obstetrical hemorrhages. II. Placental site and venous drainage of the pregnant uterus. Am J Obstet Gynecol 78(2):385–398
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, Moher D, Becker BJ, Sipe TA, Thacker SB (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Observ Studies Epidemiol (MOOSE) Group JAMA 283(15):208–212
S.B. Wells GA, O'Connell D, Peterson J, Welch V, Losos M, Tugwell P (2020) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomized studies in meta-analyses. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. (Accessed 20 Mar 2020).
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315(7109):629–634
Duval S, Tweedie R (2000) Trim and fill: A simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics 56(2):455–463
Law M, Jackson D, Turner R, Rhodes K, Viechtbauer W (2016) Two new methods to fit models for network meta-analysis with random inconsistency effects. BMC Med Res Methodol 16:87
Rücker G, Schwarzer G (2015) Ranking treatments in frequentist network meta-analysis works without resampling methods. BMC Med Res Methodol 15:58
Antsaklis A, Daskalakis G, Tzortzis E, Michalas S (2000) The effect of gestational age and placental location on the prediction of pre-eclampsia by uterine artery Doppler velocimetry in low-risk nulliparous women. Ultra Obstet Gynecol Off J Internat Soc Ultra Obstet Gynecol 16(7):635–639
Contro E, Maroni E, Cera E, Youssef A, Bellussi F, Pilu G, Rizzo N, Pelusi G, Ghi T (2010) Unilaterally increased uterine artery resistance, placental location and pregnancy outcome. Eur J Obstet Gynecol Reprod Biol 153(2):143–147
Devarajan K, Kives S, Ray JG (2012) Placental location and newborn weight. J Obstet Gynaecol Canada JOGC J Obstetrique et Gynecol Canada JOGC 34(4):325–329
Gizzo S, Noventa M, Vitagliano A, Quaranta M, Giovanni VD, Borgato S, Saccardi C, D’Antona D (2015) Sonographic assessment of placental location: a mere notional description or an important key to improve both pregnancy and perinatal obstetrical care? A large cohort study. Int J Clin Exp Med 8(8):13056–13066
Jani PS, Patel UM, Gandhi MR, Thakor NC, Kakani CR (2017) Placental laterality and uterine artery resistance as predictor of preeclampsia: a prospective study at GMERS Medical College Dharpur-Patan North Gujarat India. Menoufia Med J 3(6):4
Kakkar T, Singh V, Razdan R, Digra SK, Gupta A, Kakkar M (2013) Placental laterality as a predictor for development of preeclampsia. J Obstet Gynaecol India 63(1):22–25
Kofinas AD, Penry M, Swain M, Hatjis CG (1989) Effect of placental laterality on uterine artery resistance and development of preeclampsia and intrauterine growth retardation. Am J Obstet Gynecol 161(6 Pt 1):1536–1539
Chapman MG, Furness ET, Jones WR, Sheat JH (1979) Significance of the ultrasound location of placental site in early pregnancy. Br J Obstet Gynaecol 86(11):846–848
Little WA (1964) Significance of placental position in utero. Am J Obstet Gynecol 90:328–333
Ogueh O, Morin L, Usher RH, Benjamin A (2003) Obstetric implications of low-lying placentas diagnosed in the second trimester. Internat J Gynaecol Obstet Official Organ Internat Feder Gynaecol Obstet 83(1):11–17
Osmundson SS, Wong AE, Gerber SE (2013) Second-trimester placental location and postpartum hemorrhage. J Ultra Med Official J Am Instit Ultra Med 32(4):631–636
Robinson AJ, Muller PR, Allan R, Ross R, Baghurst PA, Keirse MJ (2012) Precise mid-trimester placenta localisation: does it predict adverse outcomes? Aust N Z J Obstet Gynaecol 52(2):156–160
Lurie S, Gomel A, Sadan O, Ginath S, Rotmensch S, Glezerman M (2003) The duration of the third stage of labor is subject to the location of placental implantation. Gynecol Obstet Invest 56(1):14–16
Zhao J, Zhang Q, Wang Y, Li Y (2014) Endometrial pattern, thickness and growth in predicting pregnancy outcome following 3319 IVF cycle. Reprod Biomed Online 29(3):291–298
Bu Z, Yang X, Song L, Kang B, Sun Y (2019) The impact of endometrial thickness change after progesterone administration on pregnancy outcome in patients transferred with single frozen-thawed blastocyst. Reprod Biol Endocrinol 17(1):99
von Wolff M, Fäh M, Roumet M, Mitter V, Stute P, Griesinger G, Kohl SA (2018) Thin endometrium is also associated with lower clinical pregnancy rate in unstimulated menstrual cycles: a study based on natural cycle IVF. Front Endocrinol (Lausanne) 20(9):776
Magann EF, Evans SF, Newnham JP (1998) Placental implantation at 18 weeks and migration throughout pregnancy. South Med J 91(11):1025–1027
Schwartz N, Sammel MD, Leite R, Parry S (2014) First-trimester placental ultrasound and maternal serum markers as predictors of small-for-gestational-age infants. Am J Obstet Gynecol 211(3):253.e1–8
Hasija A, Balyan K, Debnath E, Kumar M (2021) Prediction of hypertension in pregnancy in high risk women using maternal factors and serial placental profile in second and third trimester. Placenta 104:236–242
Awuah SP, Okai I, Ntim EA, Bedu-Addo K (2020) Prevalence, placenta development, and perinatal outcomes of women with hypertensive disorders of pregnancy at Komfo Anokye Teaching Hospital. PLoS ONE 15(10):e0233817
Pomar L, Lambert V, Madec Y, Vouga M, Pomar C, Matheus S, Fontanet A, Panchaud A, Carles G, Baud D (2020) Placental infection by Zika virus in French Guiana. Ultrasound Obstet Gynecol 56(5):740–748
Kittipornpechdee N, Hanamornroongruang S, Lekmak D, Treetipsatit J (2018) Fetal and placental pathology in congenital syphilis: a comprehensive study in perinatal autopsy. Fetal Pediatr Pathol 37(4):231–242
Berceanu C, Tetileanu AV, Ofiţeru AM, Brătilă E, Mehedinţu C, Voicu NL, Szasz FA, Berceanu S, Vlădăreanu S, Navolan DB (2018) Morphological and ultrasound findings in the placenta of diabetic pregnancy. Rom J Morphol Embryol 59(1):175–186
Acknowledgements
We would like to thank Donna Eastham, BA, CRS for her assistance in manuscript editing and submission. We would also like to thank Sheila Thomas, MA(LS), MEd for her assistance with the literature search.
Funding
This research received no funding.
Author information
Authors and Affiliations
Contributions
R: Protocol/project development, Data collection and management, Manuscript writing/editing. M: Data collection, Manuscript writing/editing. S: Data collection, Manuscript writing/editing. O: Data analysis, Manuscript writing/editing. H: Data analysis, Manuscript writing/editing. W: Protocol/project development, Data collection and management, Manuscript writing/editing. Q: Project development, Manuscript writing/editing. M: Protocol/project development, Data management, Manuscript writing/editing.
Corresponding author
Ethics declarations
Conflict of interest
Everett F. Magann, MD is the author of an UptoDate article on Amniotic Fluid Volume Assessment: Oligohydramnios, and receives royalties for this work. All other authors report nothing to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Julie R. Whittington is a military service member. The views expressed in this article reflect the results of research conducted by the author(s) and do not necessarily reflect the official policy or position of the Department of the Navy, Department of Defense, or the United States Government. This work was prepared as part of my official duties. Title 17 U.S.C. 105 provides that “Copyright protection under this title is not available for any work of the United States government.” Title 17 U.S.C. 101 defines a United States government work as a work prepared by a military service member or employee of the United States government as part of that person’s official duties.
Rights and permissions
About this article
Cite this article
Racher, M.L., Morris, M., Scott, A.P. et al. Placental location site and adverse antepartum pregnancy complications: a meta-analysis and review of the literature. Arch Gynecol Obstet 305, 1265–1277 (2022). https://doi.org/10.1007/s00404-021-06253-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-021-06253-x