Abstract
Purpose
The objectives of this study were to determine the incidence of UI in a large cohort of primiparous women before and during pregnancy and over the course of 30-months postpartum, and to identify risk factors for UI during and after pregnancy.
Methods
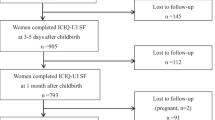
Nulliparous women aged 18–35 years with singleton pregnancies were interviewed in their third trimester and asked about urinary incontinence before and during pregnancy (n = 3001). After delivery these women were interviewed at 1, 6, 12, 18, 24 and 30-months postpartum and asked about urinary incontinence occurring in the month prior to each interview. Multivariable logistic regression models identified risk factors for UI during pregnancy and during the follow-up period.
Results
Overall, 4% reported having urinary incontinence before pregnancy and 36.8% during pregnancy. The strongest predictor of urinary incontinence during pregnancy was urinary incontinence before pregnancy (adjusted OR 13.11, 95% CI 7.43–23.13). Among the women with no subsequent pregnancies, the rate of urinary incontinence increased from 12.5% at 6-months postpartum to 27.4% at 30-months postpartum, 52.1% reported UI at one or more postpartum data collection stages, and the strongest predictors of postpartum UI were UI before pregnancy (adjusted OR 3.95 (95% CI 1.60–9.75) and during pregnancy (adjusted OR 4.36, 95% CI 3.24–5.87).
Conclusion
Our findings suggest that primiparous women who report UI before and during pregnancy should be monitored for the continuation or worsening of UI over the course of the first 2–3 years postpartum, and treatment options discussed.

Similar content being viewed by others
Data availability
The First Baby Study datasets are available from the principal investigator, Kristen Kjerulff, khk2@psu.edu.
Code availability
Not applicable.
Abbreviations
- UI:
-
Urinary incontinence
- FBS:
-
First Baby Study
- UTI:
-
Urinary tract infection
- OR:
-
Odds ratio
- CI:
-
Confidence interval
References
Haylen BT, Freeman RM, Swift SE et al (2011) An international urogynecological association (IUGA)/international continence society (ICS) joint terminology and classification of the complications related directly to the insertion of prostheses (meshes, implants, tapes) and grafts in female pelvic flo. Neurourol Urodyn. https://doi.org/10.1002/nau.21036
Subak LL, Brown JS, Kraus SR et al (2006) The “costs” of urinary incontinence for women. Obstet Gynecol. https://doi.org/10.1097/01.AOG.0000206213.48334.09
Macaulay AJ, Stern RS, Holmes DM, Stanton SL (1987) Micturition and the mind: Psychological factors in the aetiology and treatment of urinary symptoms in women. Br Med J (Clin Res Ed). https://doi.org/10.1136/bmj.294.6571.540
Viktrup L, Rortveit G, Lose G (2008) Does the impact of subsequent incontinence risk factors depend on continence status during the first pregnancy or the postpartum period 12 years before? A cohort study in 232 primiparous women. Am J Obstet Gynecol 199:73.e1-73.e4. https://doi.org/10.1016/j.ajog.2007.11.069
Thomason AD, Miller JM, DeLancey JO (2007) Urinary incontinence symptoms during and after pregnancy in continent and incontinent primiparas. Int Urogynecol J. https://doi.org/10.1007/s00192-006-0124-8
Eftekhar T, Hajibaratali B, Ramezanzadeh F, Shariat M (2006) Postpartum evaluation of stress urinary incontinence among primiparas. Int J Gynecol Obstet. https://doi.org/10.1016/j.ijgo.2006.04.042
Thom DH, Rortveit G (2010) Prevalence of postpartum urinary incontinence: a systematic review. Acta Obstet Gynecol Scand 89:1511–1522. https://doi.org/10.3109/00016349.2010.526188
Arrue M, Diez-Itza I, Ibañez L et al (2011) Factors involved in the persistence of stress urinary incontinence from pregnancy to 2 years post partum. Int J Gynecol Obstet 115(3):256–259
Burgio KL, Borello-France D, Richter HE et al (2007) Risk factors for fecal and urinary incontinence after childbirth: the childbirth and pelvic symptoms study. Am J Gastroenterol. https://doi.org/10.1111/j.1572-0241.2007.01364.x
Sangsawang B (2014) Risk factors for the development of stress urinary incontinence during pregnancy in primigravidae: a review of the literature. Eur J Obstet Gynecol Reprod Biol 178:27–34
Blomquist JL, Muñoz A, Carroll M, Handa VL (2018) Association of delivery mode with pelvic floor disorders after childbirth. JAMA - J Am Med Assoc. https://doi.org/10.1001/jama.2018.18315
Zhu L, Li L, Lang JH, Xu T (2012) Prevalence and risk factors for peri- and postpartum urinary incontinence in primiparous women in China: a prospective longitudinal study. Int Urogynecol J 23(5):563–572
Arrue M, Ibañez L, Paredes J et al (2010) Stress urinary incontinence six months after first vaginal delivery. Eur J Obstet Gynecol Reprod Biol. https://doi.org/10.1016/j.ejogrb.2010.02.039
Kjerulff KH, Velott DL, Zhu J et al (2013) Mode of first delivery and women’s intentions for subsequent childbearing: findings from the first baby study. Paediatr Perinat Epidemiol 27:62–71. https://doi.org/10.1111/ppe.12014
Kjerulff KH, Paul IM, Weisman CS et al (2020) Association between mode of first delivery and subsequent fecundity and fertility. JAMA Netw open. https://doi.org/10.1001/jamanetworkopen.2020.3076
von Elm E, Altman DG, Egger M et al (2014) The strengthening the reporting of observational studies in epidemiology (STROBE) statement: Guidelines for reporting observational studies. Int J Surg. https://doi.org/10.1016/j.ijsu.2014.07.013
IOM (2009) Weight gain during pregnancy: reexamining the guidelines
Gyhagen M, Bullarbo M, Nielsen TF, Milsom I (2013) The prevalence of urinary incontinence 20 years after childbirth: a national cohort study in singleton primiparae after vaginal or caesarean delivery. BJOG An Int J Obstet Gynaecol. https://doi.org/10.1111/j.1471-0528.2012.03301.x
Gartland D, MacArthur C, Woolhouse H et al (2016) Frequency, severity and risk factors for urinary and faecal incontinence at 4 years postpartum: a prospective cohort. BJOG An Int J Obstet Gynaecol. https://doi.org/10.1111/1471-0528.13522
Fritel X, Ringa V, Quiboeuf E, Fauconnier A (2012) Female urinary incontinence, from pregnancy to menopause: a review of epidemiological and pathophysiological findings. Acta Obstet Gynecol Scand 91(8):901–910
DeLancey JOL, Kane Low L, Miller JM et al (2008) Graphic integration of causal factors of pelvic floor disorders: an integrated life span model. Am J Obstet Gynecol. https://doi.org/10.1016/j.ajog.2008.04.001
Hendrix SL, Cochrane BB, Nygaard IE et al (2005) Effects of estrogen with and without progestin on urinary incontinence. J Am Med Assoc. https://doi.org/10.1001/jama.293.8.935
Huebner M, Antolic A, Tunn R (2010) The impact of pregnancy and vaginal delivery on urinary incontinence. Int J Gynecol Obstet. https://doi.org/10.1016/j.ijgo.2010.04.019
Hvidman L, Hvidman L, Foldspang A et al (2002) Correlates of urinary incontinence in pregnancy. Int Urogynecol J. https://doi.org/10.1007/s001920200061
Brown SJ, Donath S, MacArthur C et al (2010) Urinary incontinence in nulliparous women before and during pregnancy: prevalence, incidence, and associated risk factors. Int Urogynecol J. https://doi.org/10.1007/s00192-009-1011-x
MacArthur C, Glazener CM, Wilson PD, Lancashire RJ, Herbison GP, Grant AM (2006) New postnatal urinary incontinence: obstetric and other risk factors in primiparae. BJOG An Int J Obstet Gynaecol. https://doi.org/10.1111/j.1471-0528.2005.00818.x
Wesnes SL, Rortveit G, Bø K, Hunskaar S (2007) Urinary incontinence during pregnancy. Obstet Gynecol. https://doi.org/10.1097/01.AOG.0000257120.23260.00
Rortveit G, Daltveit AK, Hannestad YS, Hunskaar S (2003) Vaginal delivery parameters and urinary incontinence: the Norwegian EPINCONT study. Am J Obstet Gynecol. https://doi.org/10.1067/S0002-9378(03)00588-X
Groutz A, Helpman L, Gold R et al (2007) First vaginal delivery at an older age: does it carry an extra risk for the development of stress urinary incontinence? Neurourol Urodyn. https://doi.org/10.1002/nau.20414
Pandit M, Jol D, Ashton-Miller JA et al (2000) Quantification of intramuscular nerves within the female striated urogenital sphincter muscle. Obstet Gynecol. https://doi.org/10.1097/00006250-200006000-00003
Perucchini D, DeLancey JOL, Ashton-Miller JA et al (2002) Age effects on urethral striated muscle changes in number and diameter of striated muscle fibers in the ventral urethra. Am J Obstet Gynecol. https://doi.org/10.1067/mob.2002.121089
Keane DP, Sims TJ, Abrams P, Bailey AJ (1997) Analysis of collagen status in premenopausal nulliparous women with genuine stress incontinence. BJOG An Int J Obstet Gynaecol. https://doi.org/10.1111/j.1471-0528.1997.tb12055.x
Ulmsten U, Ekman G, Giertz G, Malmstrom A (1987) Different biochemical composition of connective tissue in continent and stress incontinent women. Acta Obstet Gynecol Scand. https://doi.org/10.3109/00016348709022054
Møller LA, Lose G, Jørgensen T (2000) The prevalence and bothersomeness of lower urinary tract symptoms in women 40–60 years of age. Acta Obstet Gynecol Scand. https://doi.org/10.1034/j.1600-0412.2000.079004298.x
Dinç A (2018) Prevalence of urinary incontinence during pregnancy and associated risk factors. LUTS Low Urin Tract Symptoms. https://doi.org/10.1111/luts.12182
Kocaöz S, Talas MS, Atabekoǧlu CS (2010) Urinary incontinence in pregnant women and their quality of life. J Clin Nurs. https://doi.org/10.1111/j.1365-2702.2010.03421.x
Moore EE, Jackson SL, Boyko EJ et al (2008) Urinary incontinence and urinary tract infection: temporal relationships in postmenopausal women. Obstet Gynecol. https://doi.org/10.1097/AOG.0b013e318160d64a
Brown JS, Vittinghoff E, Kanaya AM et al (2001) Urinary tract infections in postmenopausal women: effect of hormone therapy and risk factors. Obstet Gynecol. https://doi.org/10.1016/S0029-7844(01)01630-1
Bhatia NN, Bergman A (1986) Cystometry: unstable bladder and urinary tract infection. Br J Urol 58:134–137. https://doi.org/10.1111/j.1464-410x.1986.tb09012.x
Angelini K (2017) Pelvic floor muscle training to manage overactive bladder and urinary incontinence. Nurs Womens Health 21(1):51–57
Kegel AH (1948) Progressive resistance exercise in the functional restoration of the perineal muscles. Am J Obstet Gynecol. https://doi.org/10.1016/0002-9378(48)90266-X
Dumoulin C, Hay-Smith EJC, MacHabée-Séguin G (2014) Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women. Cochrane Database Syst Rev 34(4):300–308
Liang CC, Chang SD, Lin SJ, Lin YJ (2012) Lower urinary tract symptoms in primiparous women before and during pregnancy. Arch Gynecol Obstet. https://doi.org/10.1007/s00404-011-2124-2
Wesnes SL, Hunskaar S, Bo K, Rortveit G (2010) Urinary incontinence and weight change during pregnancy and postpartum: a cohort study. Am J Epidemiol. https://doi.org/10.1093/aje/kwq240
Diez-Itza I, Ibañez L, Arrue M et al (2009) Influence of maternal weight on the new onset of stress urinary incontinence in pregnant women. Int Urogynecol J. https://doi.org/10.1007/s00192-009-0923-9
Scarpa KP, Herrmann V, Palma PCR et al (2006) Prevalence and correlates of stress urinary incontinence during pregnancy: a survey at UNICAMP medical school São Paulo Brazil. Int Urogynecol J. https://doi.org/10.1007/s00192-005-1361-y
Chiarelli P, Campbell E (1997) Incontinence during pregnancy Prevalence and opportunities for continence promotion. Aust New Zeal J Obstet Gynaecol. https://doi.org/10.1111/j.1479-828X.1997.tb02220.x
Jain P, Parsons M (2011) The effects of obesity on the pelvic floor. Obstet Gynaecol. https://doi.org/10.1576/toag.13.3.133.27664
Bump RC, Sugerman HJ, Fantl JA, McClish DK (1992) Obesity and lower urinary tract function in women: effect of surgically induced weight loss. Am J Obstet Gynecol. https://doi.org/10.1016/S0002-9378(11)91418-5
Fjerbæk A, Søndergaard L, Andreasen J, Glavind K (2020) Treatment of urinary incontinence in overweight women by a multidisciplinary lifestyle intervention. Arch Gynecol Obstet. https://doi.org/10.1007/s00404-019-05371-x
MacLennan AH, Taylor AW, Wilson DH, Wilson D (2000) The prevalence of pelvic floor disorders and their relationship to gender, age, parity and mode of delivery. Br J Obstet Gynaecol. https://doi.org/10.1111/j.1471-0528.2000.tb11669.x
Kepenekci I, Keskinkilic B, Akinsu F et al (2011) Prevalence of pelvic floor disorders in the female population and the impact of age, mode of delivery, and parity. Dis Colon Rectum. https://doi.org/10.1007/DCR.0b013e3181fd2356
Altman D, Ekström Å, Forsgren C et al (2007) Symptoms of anal and urinary incontinence following cesarean section or spontaneous vaginal delivery. Am J Obstet Gynecol. https://doi.org/10.1016/j.ajog.2007.03.083
Fritel X, Fauconnier A, Levet C, Benifla JL (2004) Stress urinary incontinence 4 years after the first delivery: a retrospective cohort survey. Acta Obstet Gynecol Scand. https://doi.org/10.1111/j.0001-6349.2004.00457.x
Gyhagen M, Bullarbo M, Nielsen TF, Milsom I (2013) A comparison of the long-term consequences of vaginal delivery versus caesarean section on the prevalence, severity and bothersomeness of urinary incontinence subtypes: a national cohort study in primiparous women. BJOG An Int J Obstet Gynaecol. https://doi.org/10.1111/1471-0528.12367
Memon HU, Handa VL (2013) Vaginal childbirth and pelvic floor disorders. Women’s Heal 9(3):265–277
Funding
This study was funded by the Eunice Kennedy Shriver National Institute of Child Health and Human Development, National Institutes of Health, R01 HD052990.
Author information
Authors and Affiliations
Contributions
KP: Manuscript writing. JL: Manuscript writing, editing. SB: Manuscript editing. KK: protocol/project development, data collection, data analysis, manuscript writing.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Ethics approval
This study received all required approvals from the Penn State College of Medicine Institutional Review Board (IRB), as well as the IRB’s of all hospitals and organizations involved with participant recruitment.
Consent to participate
Written and signed informed consent was obtained from all individual participants included in this study.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix 1
Appendix 1
Urinary incontinence questions asked in the First Baby Study.
Asked in the baseline interview, third trimester of pregnancy
Q1. During your pregnancy, how often have you experienced any amount of accidental urine loss? | ||
|---|---|---|
2 or more times a day | 1 | = > Q2 |
Once a day | 2 | = > Q2 |
2 or more times a week | 3 | = > Q2 |
Once a week | 4 | = > Q2 |
1–3 times per month | 5 | = > Q2 |
Never | 6 | = > Q3 |
Don’t know | 8 | = > Q3 |
Declined to answer | 9 | = > Q3 |
Q2. How much urine do you usually lose each time, drops, small splashes or more? | |
|---|---|
Drops | 1 |
Small splashes | 2 |
More | 3 |
Do not know | 8 |
Declined to answer | 9 |
Q3. Before you became pregnant, how often did you experience any amount of accidental urine loss? | |
|---|---|
2 or more times a day | 1 |
Once a day | 2 |
2 or more times a week | 3 |
Once a week | 4 |
1–3 times per month | 5 |
Never | 6 |
Don't know | 8 |
Declined to answer | 9 |
Asked in the 1-month postpartum interview
Q1. Since your delivery, how often have you experienced any amount of accidental urine loss? | |
|---|---|
2 or more times a day | 1 |
Once a day | 2 |
2 or more times a week | 3 |
Once a week | 4 |
1–3 times per month | 5 |
Never | 6 |
Don't know | 8 |
Declined to answer | 9 |
Asked at 6, 12, 18, 24, and 30-months postpartum
Q1. In the past month, how often have you experienced any amount of accidental urine loss? | ||
|---|---|---|
2 or more times a day | 1 | = > Q2 |
Once a day | 2 | = > Q2 |
2 or more times a week | 3 | = > Q2 |
Once a week | 4 | = > Q2 |
1–3 times per month | 5 | = > Q2 |
Never | 6 | = > Q3 |
Do not know | 8 | = > Q3 |
Declined to answer | 9 | = > Q3 |
Q2. How much urine do you usually lose each time, drops, small splashes or more? | |
|---|---|
Drops | 1 |
Small splashes | 2 |
More | 3 |
Don't know | 8 |
Declined to answer | 9 |
Rights and permissions
About this article
Cite this article
Patel, K., Long, J.B., Boyd, S.S. et al. Natural history of urinary incontinence from first childbirth to 30-months postpartum. Arch Gynecol Obstet 304, 713–724 (2021). https://doi.org/10.1007/s00404-021-06134-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-021-06134-3