Abstract
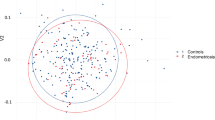
Endometriosis (EM) in reproductive females has an incidence of 6–10% and greatly affects female fertility, quality of life, and long-term health. The gut microbiota can affect the physiological and pathological processes of humans through various pathways, such as those involving the nervous and endocrine systems and immunity, and it plays important roles in endocrine and inflammatory diseases. Whether the gut microbiota plays a role in EM has gradually attracted researchers’ attention. In the present study, fecal and blood samples were collected from 12 patients with stage 3/4 EM and 12 healthy controls. We performed 16S rRNA high-throughput sequencing to compare the gut microbiota between the EM and control groups. Serum levels of hormones and inflammatory cytokines were measured. We found that compared with the control group, the EM group had a lower α diversity of gut microbiota and a higher Firmicutes/Bacteroidetes ratio. The abundances of various taxa (such as Actinobacteria, Tenericutes, Blautia, Bifidobacterium, Dorea, and Streptococcus) were significantly different between the two groups. The taxon with the highest abundance in the EM group was Prevotella_7, and that in the control group was Coprococcus_2. The serum levels of E2 and IL-8 were significantly higher in the EM group than in the control group (E2: EM group 74.7 ± 22.5 pg/L vs CON group 47.9 ± 12.5 pg/L; IL-8: EM group 6.39 ± 1.59 pg/mL vs CON group 4.14 ± 0.73 pg/mL). Additionally, the gut microbiota of the EM group was enriched for the microbial function categories environmental information processing, endocrine system, and immune system. Correlations were detected between each of Blautia and Dorea abundance and estradiol level and between Subdoligranulum abundance and IL-8 level. This study elucidated the associations between the gut microbiota and both serum hormones and inflammatory factors in EM. However, the findings need to be verified in future studies.





Similar content being viewed by others
References
Hogg C, Horne AW, Greaves E (2020) Endometriosis-associated macrophages: origin, phenotype, and function. Front Endocrinol 11:7. https://doi.org/10.3389/fendo.2020.00007
Barko PC, McMichael MA, Swanson KS, Williams DA (2018) The gastrointestinal microbiome: a review. J Vet Intern Med 32(1):9–25. https://doi.org/10.1111/jvim.14875
Shigesi N, Kvaskoff M, Kirtley S, Feng Q, Fang H, Knight JC, Missmer SA, Rahmioglu N, Zondervan KT, Becker CM (2019) The association between endometriosis and autoimmune diseases: a systematic review and meta-analysis. Hum Reprod Update 25(4):486–503. https://doi.org/10.1093/humupd/dmz014
Kvaskoff M, Mu F, Terry KL, Harris HR, Poole EM, Farland L, Missmer SA (2015) Endometriosis: a high-risk population for major chronic diseases? Hum Reprod Update 21(4):500–516. https://doi.org/10.1093/humupd/dmv013
Yuan M, Li D, Zhang Z, Sun H, An M, Wang G (2018) Endometriosis induces gut microbiota alterations in mice. Hum Reprod 33(4):607–616. https://doi.org/10.1093/humrep/dex372
Bailey MT, Coe CL (2002) Endometriosis is associated with an altered profile of intestinal microflora in female rhesus monkeys. Hum Reprod 17(7):1704–1708. https://doi.org/10.1093/humrep/17.7.1704
Schenken RS, Guzick DS (1997) Revised endometriosis classification: 1996. Fertil Steril 67(5):815–816. https://doi.org/10.1016/s0015-0282(97)81390-8
Zhou L, Ni Z, Cheng W, Yu J, Sun S, Zhai D, Yu C, Cai Z (2020) Characteristic gut microbiota and predicted metabolic functions in women with PCOS. Endocr Connect 9(1):63–73. https://doi.org/10.1530/EC-19-0522
Cani PD, Possemiers S, Van de Wiele T, Guiot Y, Everard A, Rottier O, Geurts L, Naslain D, Neyrinck A, Lambert DM, Muccioli GG, Delzenne NM (2009) Changes in gut microbiota control inflammation in obese mice through a mechanism involving GLP-2-driven improvement of gut permeability. Gut 58(8):1091–1103. https://doi.org/10.1136/gut.2008.165886
Sohail MU, Elrayess MA, Al Thani AA, Al-Asmakh M, Yassine HM (2019) Profiling the oral microbiome and plasma biochemistry of obese hyperglycemic subjects in Qatar. Microorganisms. https://doi.org/10.3390/microorganisms7120645
Yang M, Bose S, Lim SK, Kim H (2019) Preventive effects of Pyungwi-san against dextran sulfate sodium- and clostridium difficile-induced inflammatory bowel disease in mice. Int J Mol Sci. https://doi.org/10.3390/ijms20246346
Biarc J, Nguyen IS, Pini A, Gosse F, Richert S, Thierse D, Van Dorsselaer A, Leize-Wagner E, Raul F, Klein JP, Scholler-Guinard M (2004) Carcinogenic properties of proteins with pro-inflammatory activity from Streptococcus infantarius (formerly S. bovis). Carcinogenesis 25(8):1477–1484. https://doi.org/10.1093/carcin/bgh091
Abdulamir AS, Hafidh RR, Bakar FA (2010) Molecular detection, quantification, and isolation of Streptococcus gallolyticus bacteria colonizing colorectal tumors: inflammation-driven potential of carcinogenesis via IL-1, COX-2, and IL-8. Mol Cancer 9:249. https://doi.org/10.1186/1476-4598-9-249
Flores R, Shi J, Fuhrman B, Xu X, Veenstra TD, Gail MH, Gajer P, Ravel J, Goedert JJ (2012) Fecal microbial determinants of fecal and systemic estrogens and estrogen metabolites: a cross-sectional study. J Transl Med 10(1):253. https://doi.org/10.1186/1479-5876-10-253
Goedert JJ, Hua X, Bielecka A, Okayasu I, Milne GL, Jones GS, Fujiwara M, Sinha R, Wan Y, Xu X, Ravel J, Shi J, Palm NW, Feigelson HS (2018) Postmenopausal breast cancer and oestrogen associations with the IgA-coated and IgA-noncoated faecal microbiota. Br J Cancer 118(4):471–479. https://doi.org/10.1038/bjc.2017.435
Kitawaki J, Kado N, Ishihara H, Koshiba H, Kitaoka Y, Honjo H (2002) Endometriosis: the pathophysiology as an estrogen-dependent disease. J Steroid Biochem Mol Biol 83(1–5):149–155. https://doi.org/10.1016/s0960-0760(02)00260-1
Belkaid Y, Hand TW (2014) Role of the microbiota in immunity and inflammation. Cell 157(1):121–141. https://doi.org/10.1016/j.cell.2014.03.011
Tao X, Xie Y, Wang L, Gu W, Yu X, Zhou X (2014) The expression of Cox-2, NF-kappaB, and VEGF in ectopic endometrial tissues within fallopian tubes suggests different etiologies. Int J Gynecol Pathol 33(4):411–417. https://doi.org/10.1097/PGP.0000000000000080
Funding
This study was supported by a Grant from the National Natural Science Foundation of China (no. 81703874 to Shuai Sun, 81603646 to Chaoqin Yu).
Author information
Authors and Affiliations
Contributions
CY and SS designed the research. JS, ZN, WC and LZ performed this study. DZ analyzed the data. JS and ZN wrote the paper. JS was responsible for the critical revision of the paper. JS and ZN contributed equally to this work. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shan, J., Ni, Z., Cheng, W. et al. Gut microbiota imbalance and its correlations with hormone and inflammatory factors in patients with stage 3/4 endometriosis. Arch Gynecol Obstet 304, 1363–1373 (2021). https://doi.org/10.1007/s00404-021-06057-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-021-06057-z