Abstract
Purpose
Intrahepatic cholestasis of pregnancy and preeclampsia are two major pregnancy complications. We aimed to investigate the association between intrahepatic cholestasis of pregnancy (ICP) and preeclampsia.
Methods
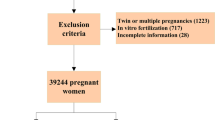
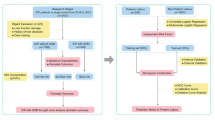
Single-center retrospective study. Study group included 180 women (162 singletons and 18 twin gestations) who were diagnosed with ICP based on clinical presentation, elevated liver enzymes and bile acids. The reference group included 1618 women (1507 singletons and 111 twin gestations) who delivered during the study period, and were matched according to age, gravidity, parity and singleton or twin gestation.
Results
The incidence of ICP was 0.36%. The incidence of preeclampsia was higher in women with ICP compared to reference group (7.78% vs 2.41%, aOR, 3.74 95% CI 12.0–7.02, p < 0.0001), for either without—(3.89% vs 1.61%, aOR 2.83, 95% CI 1.23–6.5, p = 0.145) or with severe features (3.89% vs 0.80%, aOR 5.17 95% CI 2.14–12.50, p = 0.0003). For both singleton and twin pregnancies, overall preeclampsia rates were higher in the ICP group (5.56% vs 2.19%, aOR 2.91 95% CI 1.39–6.07 p = 0.0045; and 27.78% vs 5.41%, aOR 10.9 95% CI 2.16–47.19, p = 0.0033, respectively). Earlier diagnosis of ICP was associated with higher incidence of preeclampsia (31.1 ± 3.8 vs 34.86 ± 6.2 gestational weeks, p = 0.0259). The average time between ICP diagnosis and to the onset of preeclampsia was 29.7 ± 24 days.
Conclusion
ICP is associated with an increased risk for preeclampsia. We suggest intensified follow-up for preeclampsia in women with ICP, especially among those with early ICP presentation and twins’ gestations.

Similar content being viewed by others
References
Laifer SA, Stiller RJ, Siddiqui DS, Dunston-Boone G, Whetham JC (2001) Ursodeoxycholic acid for the treatment of intrahepatic cholestasis of pregnancy. J Matern Fetal Med 10(2):131–135
Lee RH, Goodwin TM, Greenspoon J, Incerpi M (2006) The prevalence of intrahepatic cholestasis of pregnancy in a primarily Latina Los Angeles population. J Perinatol 26(9):527–532
Larson SP, Kovilam O, Agrawal DK (2016) Immunological basis in the pathogenesis of intrahepatic cholestasis of pregnancy. Expert Rev Clin Immunol 12(1):39–48
Kong X, Kong Y, Zhang F, Wang T, Zhu X (2018) Expression and significance of dendritic cells and Th17/Treg in serum and placental tissues of patients with intrahepatic cholestasis of pregnancy. J Matern Neonatal Med 31:901–906
Yang X, Zhang J, Ding Y (2017) Association of microRNA-155, interleukin 17A, and proteinuria in preeclampsia. Medicine (United States) 96:1–8
Cao W, Wang X, Chen T, Xu W, Feng F, Zhao S, Wang Z, Hu Y, Xie B (2018) Maternal lipids, BMI and IL-17/IL-35 imbalance in concurrent gestational diabetes mellitus and preeclampsia. Exp Ther Med 16:427–435
Dixon PH, Williamson C (2016) The pathophysiology of intrahepatic cholestasis of pregnancy. Clin Res Hepatol Gastroenterol 40(2):141–153
Gonzalez MC, Reyes H, Arrese M, Figueroa D, Lorca B, Andresen M, Segovia N, Molina C, Arce S (1989) Intrahepatic cholestasis of pregnancy in twin pregnancies. J Hepatol 9(1):84–90
Geenes V, Williamson C (2009) Intrahepatic cholestasis of pregnancy. World J Gastroenterol 15(17):2049–2066
Atabey S, Duvan CI, Eren U, Turhan NO (2007) Intrahepatic cholestasis and eclampsia: a case report. Hypertens Pregnancy 26(4):363–369
Lo TK, Lau WL, Lam HS, Leung WC, Chin RK (2007) Obstetric cholestasis in Hong Kong—local experience with eight consecutive cases. Hong Kong Med J 13(5):387–391
Raz Y, Lavie A, Vered Y, Goldiner I, Skornick-Rapaport A, Landsberg Asher Y, Maslovitz S, Levin I, Lessing JB, Kuperminc MJ, Rimon E (2015) Severe intrahepatic cholestasis of pregnancy is a risk factor for preeclampsia in singleton and twin pregnancies. Am J Obstet Gynecol 213(3):395.e1–8
Baliutavičienė D, Zubruvienė N, Zalinkevičius R (2011) Pregnancy outcome in cases of intrahepatic cholestasis of pregnancy. Int J Gynaecol Obstet 112(3):250–251
Marathe JA, Lim WH, Metz MP, Scheil W, Dekker GA, Hague WM (2017) A retrospective cohort review of intrahepatic cholestasis of pregnancy in a South Australian population. Eur J Obstet Gynecol Reprod Biol 218:33–38
Shemer WE, Marschall HU, Ludvigsson JF, Stephansson O (2013) Intrahepatic cholestasis of pregnancy and associated adverse pregnancy and fetal outcomes: a 12-year population-based cohort study. BJOG 120(6):717–723
Dollberg S, Haklai Z, Mimouni FB, Gorfein I, Gordon ES (2005) Birth weight standards in the live-born population in Israel. Isr Med Assoc J 7(5):311–314
Royal College of Obstetricians and Gynaecologists (2011) Obstetric Cholestasis Green-top Guideline No. 43. https://www.rcog.org.uk/globalassets/documents/guidelines/gtg_43.pdf. Accessed 22 Dec 2019
American College of Obstetricians and Gynecologists; Task Force on Hypertension in Pregnancy (2013) Hypertension in pregnancy. Report of the American College of Obstetricians and Gynecologists’ Task Force on hypertension in pregnancy. Obstet Gynecol 122(5):1122–1131
Goulis DG, Walker IA, de Swiet M, Redman CW, Williamson C (2004) Preeclampsia with abnormal liver function tests is associated with cholestasis in a subgroup of cases. Hypertens Pregnancy 23(1):19–27
Martineau M, Raker C, Powrie R, Williamson C (2014) Intrahepatic cholestasis of pregnancy is associated with an increased risk of gestational diabetes. Eur J Obstet Gynecol Reprod Biol 176:80–85
Geenes V, Chappell LC, Seed PT, Steer PJ, Knight M, Williamson C (2014) Association of severe intrahepatic cholestasis of pregnancy with adverse pregnancy outcomes: a prospective population-based case-control study. Hepatology 59(4):1482–1491
Sepúlveda WH, González C, Cruz MA, Rudolph MI (1991) Vasoconstrictive effect of bile acids on isolated human placental chorionic veins. Eur J Obstet Gynecol Reprod Biol 42(3):211–215
van Patot MC, Valdez M, Becky V, Cindrova-Davies T, Johns J, Zwerdling L, Jauniaux E, Burton GJ (2009) Impact of pregnancy at high altitude on placental morphology in non-native women with and without preeclampsia. Placenta 30(6):523–528
Shemer WE, Thorsell M, Östlund E, Blomgren B, Marschall HU (2012) Stereological assessment of placental morphology in intrahepatic cholestasis of pregnancy. Placenta 33(11):914–918
Heazell AE, Moll SJ, Jones CJ, Baker PN, Crocker IP (2007) Formation of syncytial knots is increased by hyperoxia, hypoxia and reactive oxygen species. Placenta 28(Suppl A):S33–S40
Oztas E, Ozler S, Ersoy AO, Erkenekli K, Sucak A, Ergin M, Uygur D, Danisman N (2016) Placental ADAMTS-12 levels in the pathogenesis of preeclampsia and intrahepatic cholestasis of pregnancy. Reprod Sci 23(4):475–481
Laasanen J, Hiltunen M, Romppanen EL, Punnonen K, Mannermaa A, Heinonen S (2003) Microsatellite marker association at chromosome region 2p13 in Finnish patients with preeclampsia and obstetric cholestasis suggests a common risk locus. Eur J Hum Genet 11(3):232–236
Funding
None received.
Author information
Authors and Affiliations
Contributions
MM: protocol/project development, data collection or management, data analysis, and manuscript writing/editing. AS: data collection or management, data analysis, and manuscript writing/editing. EK: data collection or management, data analysis, and manuscript writing/editing. RB: data collection or management, data analysis, and manuscript writing/editing. OS-A: data collection or management, data analysis, and manuscript writing/editing. MB: protocol/project development, data analysis, and manuscript writing/editing. NA: protocol/project development, data collection or management, data analysis, and manuscript writing/editing. EH: protocol/project development, data analysis, and manuscript writing/editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mor, M., Shmueli, A., Krispin, E. et al. Intrahepatic cholestasis of pregnancy as a risk factor for preeclampsia. Arch Gynecol Obstet 301, 655–664 (2020). https://doi.org/10.1007/s00404-020-05456-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-020-05456-y