Abstract
Purpose
To evaluate the influence of three-dimensional (3D) high-definition (HD) visualisation in laparoscopic hysterectomy in normal weight, overweight and obese women.
Methods
A retrospective analysis of 180 patients undergoing total laparoscopic hysterectomy (TLH: n = 90) or laparoscopic supracervical hysterectomy (LASH: n = 90) was performed. The study collective consisted of 90 women (TLH: n = 45, LASH: n = 45), who underwent laparoscopic hysterectomy with a 3D HD laparoscopic system. Ninety matched (uterine weight, previous surgeries) women with hysterectomy (TLH: n = 45, LASH: n = 45) performed by the same surgeon with conventional two-dimensional laparoscopy formed the control group. Statistical analysis was accomplished stratifying patients according to body mass index (BMI) (≤24.9, 25–29.9, ≥30.0 kg/m2). In each BMI, collective subtypes of surgery (TLH, LASH) as well as hysterectomies as a whole were analysed. Demographic data and surgical parameters were evaluated.
Results
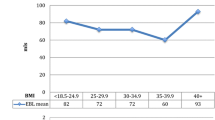
In all BMI subgroups, there were no significant differences concerning demographic parameters. Number of trocar site incisions needed was significantly less in women undergoing 3D compared to 2D laparoscopy independent of BMI. Furthermore, a significantly lower blood loss was revealed using 3D visualisation in LASH subgroups of the normal and overweight collectives. Three-dimensional laparoscopy was additionally associated with a significantly shorter duration of surgery in the TLH subgroup in overweight patients and a lower haemoglobin drop in the LASH subgroup of the obese.
Conclusion
The need of less trocar site incisions concerning all weight groups as well.
Similar content being viewed by others
References
Ng M, Fleming T, Robinson M, Thomson B, Graetz N, Margono C, Mullany EC, Biryukov S, Abbafati C, Abera SF, Abraham JP, Abu-Rmeileh NM, Achoki T, AlBuhairan FS, Alemu ZA, Alfonso R, Ali MK, Ali R, Guzman NA, Ammar W, Anwari P, Banerjee A, Barquera S, Basu S, Bennett DA, Bhutta Z, Blore J, Cabral N, Nonato IC, Chang JC, Chowdhury R, Courville KJ, Criqui MH, Cundiff DK, Dabhadkar KC, Dandona L, Davis A, Dayama A, Dharmaratne SD, Ding EL, Durrani AM, Esteghamati A, Farzadfar F, Fay DF, Feigin VL, Flaxman A, Forouzanfar MH, Goto A, Green MA, Gupta R, Hafezi-Nejad N, Hankey GJ, Harewood HC, Havmoeller R, Hay S, Hernandez L, Husseini A, Idrisov BT, Ikeda N, Islami F, Jahangir E, Jassal SK, Jee SH, Jeffreys M, Jonas JB, Kabagambe EK, Khalifa SE, Kengne AP, Khader YS, Khang YH, Kim D, Kimokoti RW, Kinge JM, Kokubo Y, Kosen S, Kwan G, Lai T, Leinsalu M, Li Y, Liang X, Liu S, Logroscino G, Lotufo PA, Lu Y, Ma J, Mainoo NK, Mensah GA, Merriman TR, Mokdad AH, Moschandreas J, Naghavi M, Naheed A, Nand D, Narayan KM, Nelson EL, Neuhouser ML, Nisar MI, Ohkubo T, Oti SO, Pedroza A, Prabhakaran D, Roy N, Sampson U, Seo H, Sepanlou SG, Shibuya K, Shiri R, Shiue I, Singh GM, Singh JA, Skirbekk V, Stapelberg NJ, Sturua L, Sykes BL, Tobias M, Tran BX, Trasande L, Toyoshima H, van de Vijver S, Vasankari TJ, Veerman JL, Velasquez-Melendez G, Vlassov VV, Vollset SE, Vos T, Wang C, Wang X, Weiderpass E, Werdecker A, Wright JL, Yang YC, Yatsuya H, Yoon J, Yoon SJ, Zhao Y, Zhou M, Zhu S, Lopez AD, Murray CJ, Gakidou E (2014) Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet 384(9945):766–781. doi:10.1016/S0140-6736(14)60460-8
Morgan-Ortiz F, Soto-Pineda JM, Lopez-Zepeda MA, Peraza-Garay Fde J (2013) Effect of body mass index on clinical outcomes of patients undergoing total laparoscopic hysterectomy. Int J Gynaecol Obstet 120(1):61–64. doi:10.1016/j.ijgo.2012.08.012
Aarts JW, Nieboer TE, Johnson N, Tavender E, Garry R, Mol BW, Kluivers KB (2015) Surgical approach to hysterectomy for benign gynaecological disease. Cochrane Database Syst Rev 8:CD003677. doi:10.1002/14651858.CD003677.pub5
Osler M, Daugbjerg S, Frederiksen BL, Ottesen B (2011) Body mass and risk of complications after hysterectomy on benign indications. Hum Reprod 26(6):1512–1518. doi:10.1093/humrep/der060
Blikkendaal MD, Schepers EM, van Zwet EW, Twijnstra AR, Jansen FW (2015) Hysterectomy in very obese and morbidly obese patients: a systematic review with cumulative analysis of comparative studies. Arch Gynecol Obstet 292(4):723–738. doi:10.1007/s00404-015-3680-7
Garry R, Fountain J, Brown J, Manca A, Mason S, Sculpher M, Napp V, Bridgman S, Gray J, Lilford R (2004) EVALUATE hysterectomy trial: a multicentre randomised trial comparing abdominal, vaginal and laparoscopic methods of hysterectomy. Health Technol Assess 8(26):1–154
Eltabbakh GH, Piver MS, Hempling RE, Recio FO (1999) Laparoscopic surgery in obese women. Obstet Gynecol 94(5 Pt 1):704–708
Honeck P, Wendt-Nordahl G, Rassweiler J, Knoll T (2012) Three-dimensional laparoscopic imaging improves surgical performance on standardized ex vivo laparoscopic tasks. J Endourol 26(8):1085–1088. doi:10.1089/end.2011.0670
Kong SH, Oh BM, Yoon H, Ahn HS, Lee HJ, Chung SG, Shiraishi N, Kitano S, Yang HK (2010) Comparison of two- and three-dimensional camera systems in laparoscopic performance: a novel 3D system with one camera. Surg Endosc 24(5):1132–1143. doi:10.1007/s00464-009-0740-8
Taffinder N, Smith SG, Huber J, Russell RC, Darzi A (1999) The effect of a second-generation 3D endoscope on the laparoscopic precision of novices and experienced surgeons. Surg Endosc 13(11):1087–1092
Wagner OJ, Hagen M, Kurmann A, Horgan S, Candinas D, Vorburger SA (2012) Three-dimensional vision enhances task performance independently of the surgical method. Surg Endosc 26(10):2961–2968. doi:10.1007/s00464-012-2295-3
Tuschy B, Berlit S, Brade J, Sutterlin M, Hornemann A (2014) Full high-definition three-dimensional gynaecological laparoscopy–clinical assessment of a new robot-assisted device. Vivo 28(1):111–115
Kuczmarski RJ, Carroll MD, Flegal KM, Troiano RP (1997) Varying body mass index cutoff points to describe overweight prevalence among U.S. adults: NHANES III (1988–1994). Obes Res 5(6):542–548
Becker H, Melzer A, Schurr MO, Buess G (1993) 3-D video techniques in endoscopic surgery. Endosc Surg Allied Technol 1(1):40–46
Köster S, Volz J, Melchert F (1996) Indication for 3D laparoscopy in gynaecology. Geburtshilfe Frauenheilkd 56:431–433
van Bergen P, Kunert W, Buess GF (2000) The effect of high-definition imaging on surgical task efficiency in minimally invasive surgery: an experimental comparison between three-dimensional imaging and direct vision through a stereoscopic TEM rectoscope. Surg Endosc 14(1):71–74
Buchs NC, Volonte F, Pugin F, Toso C, Morel P (2012) Three-dimensional laparoscopy: a step toward advanced surgical navigation. Surg Endosc. doi:10.1007/s00464-012-2481-3
Storz P, Buess GF, Kunert W, Kirschniak A (2012) 3D HD vs. 2D HD: surgical task efficiency in standardised phantom tasks. Surg Endosc 26(5):1454–1460. doi:10.1007/s00464-011-2055-9
Sorensen SM, Savran MM, Konge L, Bjerrum F (2016) Three-dimensional vs. two-dimensional vision in laparoscopy: a systematic review. Surg Endosc 30(1):11–23. doi:10.1007/s00464-015-4189-7
Kaufman Y (2007) The three-dimensional “insect eye” laparoscopic imaging system—a prospective randomized study. Gynecol Surg 4:31–34
Usta TA, Karacan T, Naki MM, Calik A, Turkgeldi L, Kasimogullari V (2014) Comparison of 3-dimensional vs. 2-dimensional laparoscopic vision system in total laparoscopic hysterectomy: a retrospective study. Arch Gynecol Obstet 290(4):705–709. doi:10.1007/s00404-014-3253-1
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that there is no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Berlit, S., Hornemann, A., Sütterlin, M. et al. Laparoscopic hysterectomy in the overweight and obese: does 3D imaging make a change?. Arch Gynecol Obstet 295, 125–131 (2017). https://doi.org/10.1007/s00404-016-4215-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-016-4215-6