Abstract
Purpose
Aim of this prospective study was to investigate the effectiveness of eutectic mixture of local anaesthetic (EMLA®) patches on every abdominal incision for pain relief after gynaecologic laparoscopic surgery.
Methods
A total of 121 women were prospectively randomised to receive either placebo (control group) or EMLA® (study group) patches on all abdominal incisions. Postoperative pain was assessed 24 and 48 h after surgery using the short form of the McGill Pain Questionnaire (SF-MPQ). The amount of analgesic pain medication on demand was assessed in both groups.
Results
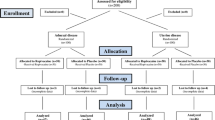
Sixty women were allocated to the study group and 61 patients to the control group before laparoscopic surgery. There were no statistically significant differences regarding age, body mass index (BMI), duration of surgery and blood loss comparing both groups. There were no statistically significant differences between both groups with regard to postoperative total pain scores 24 h (McGill total score: 31.77 ± 27.95 vs. 36.80 ± 31.39, p = 0.3535) and 48 h (McGill total score: 19.18 ± 20.09 vs. 26.61 ± 27.70, p = 0.0942) after surgery. Time to mobilisation after surgery (hours) was significantly shorter in the study group (5.01 ± 3.72 vs. 5.78 ± 3.04, p = 0.0423).
Conclusion
Despite of a significant reduction of time for mobilisation transdermal anaesthetic patches after gynaecologic laparoscopic surgery did not lead to decreased postoperative pain scores.
Similar content being viewed by others
References
Rosenberg J, Kehlet H (1999) Does effective postoperative pain management influence surgical morbidity? Eur Surg Res 31(2):133–137 8631 [pii]
Apfelbaum JL, Chen C, Mehta SS, Gan TJ (2003) Postoperative pain experience: results from a national survey suggest postoperative pain continues to be undermanaged. Anesth Analg 97(2):534–540 (Table of contents)
Lovatsis D, Jose JB, Tufman A, Drutz HP, Murphy K (2007) Assessment of patient satisfaction with postoperative pain management after ambulatory gynaecologic laparoscopy. J Obstet Gynaecol Can 29(8):664–667
Filos KS, Lehmann KA (1999) Current concepts and practice in postoperative pain management: need for a change? Eur Surg Res 31(2):97–107 8627 [pii]
Ke RW, Portera SG, Bagous W, Lincoln SR (1998) A randomized, double-blinded trial of preemptive analgesia in laparoscopy. Obstet Gynecol 92(6):972–975 S0029-7844(98)00303-2
Edwards ND, Barclay K, Catling SJ, Martin DG, Morgan RH (1991) Day case laparoscopy: a survey of postoperative pain and an assessment of the value of diclofenac. Anaesthesia 46(12):1077–1080
Madsen MR, Jensen KE (1992) Postoperative pain and nausea after laparoscopic cholecystectomy. Surg Laparosc Endosc 2(4):303–305
Zimberg SE (2003) Reducing pain and costs with innovative postoperative pain management. Manag Care Q 11(1):34–36
Coughlin SM, Karanicolas PJ, Emmerton-Coughlin HM, Kanbur B, Kanbur S, Colquhoun PH (2010) Better late than never? Impact of local analgesia timing on postoperative pain in laparoscopic surgery: a systematic review and metaanalysis. Surg Endosc 24(12):3167–3176. doi:10.1007/s00464-010-1111-1
Melzack R (1987) The short-form McGill Pain Questionnaire. Pain 30(2):191–197 0304-3959(87)91074-8
Tuschy B, Berlit S, Brade J, Sutterlin M, Hornemann A (2013) Gynaecological laparoscopic surgery for benign conditions: do women care about incisions? Eur J Obstet Gynecol Reprod Biol 169(1):84–87. doi:10.1016/j.ejogrb.2013.02.002
Bisgaard T, Klarskov B, Rosenberg J, Kehlet H (2001) Characteristics and prediction of early pain after laparoscopic cholecystectomy. Pain 90(3):261–269
Sarli L, Costi R, Sansebastiano G, Trivelli M, Roncoroni L (2000) Prospective randomized trial of low-pressure pneumoperitoneum for reduction of shoulder-tip pain following laparoscopy. Br J Surg 87(9):1161–1165. doi:10.1046/j.1365-2168.2000.01507.x
Bisgaard T, Klarskov B, Kristiansen VB, Callesen T, Schulze S, Kehlet H, Rosenberg J (1999) Multi-regional local anesthetic infiltration during laparoscopic cholecystectomy in patients receiving prophylactic multi-modal analgesia: a randomized, double-blinded, placebo-controlled study. Anesth Analg 89(4):1017–1024
Ure BM, Troidl H, Spangenberger W, Dietrich A, Lefering R, Neugebauer E (1994) Pain after laparoscopic cholecystectomy. Intensity and localization of pain and analysis of predictors in preoperative symptoms and intraoperative events. Surg Endosc 8(2):90–96
Radosa JC, Radosa MP, Mavrova R, Rody A, Juhasz-Boss I, Bardens D, Brun K, Solomayer EF, Baum S (2013) Five minutes of extended assisted ventilation with an open umbilical trocar valve significantly reduces postoperative abdominal and shoulder pain in patients undergoing laparoscopic hysterectomy. Eur J Obstet Gynecol Reprod Biol 171(1):122–127. doi:10.1016/j.ejogrb.2013.08.014
Kim TH, Kang H, Choi YS, Park JM, Chi KC, Shin HY, Hong JH (2013) Pre- and intraoperative lidocaine injection for preemptive analgesics in laparoscopic gastrectomy: a prospective, randomized, double-blind, placebo-controlled study. J Laparoendos Adv Surg Tech A 23(8):663–668. doi:10.1089/lap.2012.0542
Manjunath AP, Chhabra N, Girija S, Nair S (2012) Pain relief in laparoscopic tubal ligation using intraperitoneal lignocaine: a double masked randomized controlled trial. Eur J Obstet Gynecol Reprod Biol 165(1):110–114. doi:10.1016/j.ejogrb.2012.06.035
Alessandri F, Lijoi D, Mistrangelo E, Nicoletti A, Crosa M, Ragni N (2006) Topical diclofenac patch for postoperative wound pain in laparoscopic gynecologic surgery: a randomized study. J Minim Invasive Gynecol 13(3):195–200. doi:10.1016/j.jmig.2006.02.001
Varvel JR, Shafer SL, Hwang SS, Coen PA, Stanski DR (1989) Absorption characteristics of transdermally administered fentanyl. Anesthesiology 70(6):928–934
Muijsers RB, Wagstaff AJ (2001) Transdermal fentanyl: an updated review of its pharmacological properties and therapeutic efficacy in chronic cancer pain control. Drugs 61(15):2289–2307 611514 [pii]
Liang CL, Lu K, Liliang PC, Chung MC, Chi SC, Chen HJ (2011) Topical anesthetic EMLA for postoperative wound pain in stereotactic gamma knife radiosurgery: a perspective, randomized, placebo-controlled study. Minim Invasive Neurosurg 54(2):75–78. doi:10.1055/s-0031-1277229
Kwon YS, Kim JB, Jung HJ, Koo YJ, Lee IH, Im KT, Woo JS, Im KS (2012) Treatment for postoperative wound pain in gynecologic laparoscopic surgery: topical lidocaine patches. J Laparoendos Adv Surg Tech A 22(7):668–673. doi:10.1089/lap.2011.0440
Sinatra R (2005) The fentanyl HCl patient-controlled transdermal system (PCTS): an alternative to intravenous patient-controlled analgesia in the postoperative setting. Clin Pharmacokinet 44(Suppl 1):1–6
Jeal W, Benfield P (1997) Transdermal fentanyl. A review of its pharmacological properties and therapeutic efficacy in pain control. Drugs 53(1):109–138
Perez-Caballero Macarron C, Perez Palomino A, Moreno Fernandez L (2005) Probable methemoglobinemia following EMLA administration. An Pediatr (Barc) 63(2):179–180
Taddio A, Ohlsson A, Einarson TR, Stevens B, Koren G (1998) A systematic review of lidocaine-prilocaine cream (EMLA) in the treatment of acute pain in neonates. Pediatrics 101(2):E1
Nieboer TE, Johnson N, Lethaby A, Tavender E, Curr E, Garry R, van Voorst S, Mol BW, Kluivers KB (2009) Surgical approach to hysterectomy for benign gynaecological disease. Cochrane Database Syst Rev 3:CD003677. doi:10.1002/14651858.CD003677.pub4
Conflict of interest
The authors declare that they do not have any conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
S. Berlit and B. Tuschy contributed equally to this work.
Rights and permissions
About this article
Cite this article
Berlit, S., Tuschy, B., Brade, J. et al. Topical anaesthetic patches for postoperative wound pain in laparoscopic gynaecological surgery: a prospective, blinded and randomised trial. Arch Gynecol Obstet 291, 585–590 (2015). https://doi.org/10.1007/s00404-014-3462-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-014-3462-7