Abstract
Objective
To present preliminary results of a simple, minimally interventional, uterus-sparing procedure for uterine prolapse repair.
Methods
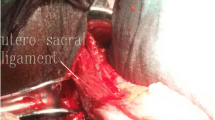
This prospective study was undertaken on women with symptomatic uterine prolapse ≥2nd stage, who declined hysterectomy at the time of prolapse surgery. A 10 mm laparoscope and three 5 mm ancillary trocars were used to perform the procedure. The uterosacral ligament was invested with a nonabsorbable suture. A total of three helical type sutures were placed full-thickness in the uterosacral ligament, beginning in the distal third of the ligament. The ends of the suture were tied with an extra-corporeal knot-tying technique on each side, thus shortening the ligaments. Finally, the round ligaments were plicated to restore the uterus to its correct anatomic position. No additional surgical procedure was performed concomitantly.
Results
Ten patients underwent laparoscopic uterosacral ligaments plication for the treatment of symptomatic uterine prolapse. The median (range) patients age was 45.5 years (36–66). Five (50%) patients were premenopausal and 3 (60%) had not completed their family. The median operating time was 22.5 min (20–45). No intraoperative complications occurred. The median follow-up time was 21 months (range 15–33). The median postoperative difference in POP-Q point C was −3 cm (range 0 to −5). Eight (80%) patients were objectively cured at the last follow-up evaluation and all of them reported a complete resolution of their symptoms. Two women had prolapse recurrence and underwent vaginal hysterectomy 7 and 24 months after primary surgery, respectively.
Conclusion
Laparoscopic uterosacral ligaments plication is a minimally invasive and straightforward simple procedure that appears to be a safe and effective treatment option for women with uterovaginal prolapse who desire uterine preservation.

Similar content being viewed by others
References
Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL (1997) Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol 89:501–506
Brown JS, Waetjen LE, Subak LL, Thom DH, Van den Eeden S, Vittinghoff E (2002) Pelvic organ prolapse surgery in the United States, 1997. Am J Obstet Gynecol 186:712–716
Davies A, Magos AL (1997) Indications and alternatives to hysterectomy. Baillieres Clin Obstet Gynaecol 11:61–75
Zivkovic F, Tamussino K, Ralph G, Schied G, Auer-Grumbach M (1996) Long-term effects of vaginal dissection on the innervation of the striated urethral sphincter. Obstet Gynecol 87:257–260
Barrington JW, Edwards G (2000) Posthysterectomy vault prolapse. Int Urogynecol J Pelvic Floor Dysfunct 11:241–245
Roovers JP, van der Bom JG, Huub van der Vaart C, Fousert DM, Heintz AP (2001) Does mode of hysterectomy influence micturition and defecation? Acta Obstet Gynecol Scand 80:945–951
Gimbel H, Zobbe V, Andersen BM, Filtenborg T, Gluud C, Tabor A (2003) Randomized controlled trial of total compared with subtotal hysterectomy with 1 year follow-up results. BJOG 110:1088–1098
Diwan A, Rardin CR, Kohli N (2004) Uterine preservation during surgery for uterovaginal prolapse: a review. Int Urogynecol J Pelvic Floor Dysfunct 15:286–292
Lin LL, Ho MH, Haessler AL, Betson LH, Alinsod RM, Liu C, Bhatia NN (2005) A review of laparoscopic uterine suspension procedures for uterine preservation. Curr Opin Obstet Gynecol 17:541–546
Wu MP (1997) Laparoscopic uterine suspension for the treatment of uterovaginal prolapse. Int J Gynecol Obstet 59:259–260
Maher CF, Carey MP, Murray CJ (2001) Laparoscopic suture hysteropexy for uterine prolapse. Obstet Gynecol 97:1010–1014
Digesu GA, Khullar V, Selvaggi L, Hutchings A, Nardo L, Milani R (2004) A case of laparoscopic uterosacral ligaments plication: a new conservative approach to uterine prolapse? Eur J Obstet Gynecol Reprod Biol 114:112–115
Seracchioli R, Hourcabie JA, Vianello F, Govoni F, Pollastri P, Venturoli S (2004) Laparoscopic treatment of pelvic floor defects in women of reproductive age. J Am Assoc Gynecol Laparosc 11:332–335
Abrams P, Cardozo L, Fall M Griffiths D, Rosier P, Ulmsten U, Van Kerrebroeck P, Victor A, Wein A, Standardisation Sub-Committee of the International Continence Society (2003) The standardization of terminology of lower urinary tract function: report from the standardisation sub-committee of the ICS. Urology 61:37–49
Bump RC, Mattiasson A, Bo K, Brubaker LP, DeLancey JO, Klarskov P, Shull BL, Smith AR (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175:10–17
DeLancey JOL (1992) Anatomy aspects of vaginal eversion after hysterectomy. Am J Obstet Gynecol 166:1717–1728
Snyder TE, Krantz KE (1991) Abdominal-retroperitoneal sacral colpopexy for the correction of vaginal prolapse. Obstet Gynecol 77:944–949
Farrell SA, Scotti RJ, Ostergard DR, Bent AE (1991) Massive evisceration: a complication following sacrospinous vaginal vault fixation. Obstet Gynecol 78:560–562
Buller JL, Thompson JR, Cundiff GW, Krueger Sullivan L, Schon Ybarra MA, Bent AE. (2001) Uterosacral ligament: description of anatomic relationships to optimize surgical safety. Obstet Gynecol 97:873–879
Diwan A, Rardin CR, Strohsnitter WC, Weld A, Rosenblatt P, Kohli N (2006) Laparoscopic uterosacral ligament uterine suspension compared with vaginal vault suspension for uterovaginal prolapse. Int Urogynecol J Pelvic Floor Dysfunct 17:79–83
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Uccella, S., Ghezzi, F., Bergamini, V. et al. Laparoscopic uterosacral ligaments plication for the treatment of uterine prolapse. Arch Gynecol Obstet 276, 225–229 (2007). https://doi.org/10.1007/s00404-006-0285-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-006-0285-1