Abstract
Methods
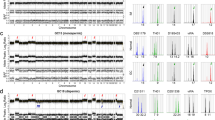
In this study, to investigate the significance of mismatch repair genes (MMR) promoter methylation and expression in the pathogenesis and malignant transformation of hydatidiform moles, we assayed promoter methylation and protein expression of the MMR genes hMLH1 and hMSH2 in gestational trophoblastic diseases (GTDs). DNA was extracted from normal placentas, partial hydatidiform moles, complete hydatidiform moles, and invasive moles, over-digested by methylation-sensitive endonuclease Hpa II, and then the promoters were amplificated by polymerase chain reaction. The protein expression was detected by immunohistochemistry.
Results
In the normal placentas, neither hMLH1 nor hMSH2 promoter methylation was detected. Expression of hMLH1 and hMSH2 in cytotrophoblasts was strongly positive. In partial hydatidiform moles and complete hydatidiform moles, hMLH1 and hMSH2 promoter methylation rates were significantly higher than that of normal placentas (P=0.000), and the protein expression in cytotrophoblasts was significantly lower (P=0.000). In the invasive moles, hMLH1 and hMSH2 promoter methylation was not significantly different compared with the partial hydatidiform moles and complete hydatidiform moles (P>0.05). Expression of hMLH1 in the invasive moles (54.5%, 6 out of 11) was not significantly different compared with the partial hydatidiform moles and complete hydatidiform moles (P>0.05). But hMSH2 expression in the invasive moles (36.5%, 4 out of 11) was weaker than that in complete hydatidiform moles (P=0.044). Promoter methylation and less expression of hMSH2 were correlated in complete hydatidiform moles (P=0.001) and invasive moles (P=0.039).
Conclusions
These results indicated that strong expression of hMLH1 and hMSH2 in the cytotrophoblasts of normal placentas may maintain genome stability. Promoter methylation and down-regulation of the expression of hMLH1 and hMSH2 are probably involved in the pathogenesis of hydatidiform moles.


Similar content being viewed by others
References
Ariel I, Lustig O, Oyer CE (1994) Relaxation of imprinting in trophoblastic disease. Gynecol Oncol 53:212–219
Fleisher AS, Esteller M, Wang S (1999) Hypermethylation of the hMLH1 gene promoter in human gastric cancers with microsatellite instability. Cancer Res 59:1090–1095
Kane MF, Loda M, Gaida GM, Lipman J, Mishra R, Goldman H, Jessup JM, Kolodner R (1997) Methylation of the hMLH1 promoter correlates with lack of expression of hMLH1 in sporadic colon tumors and mismatch repair-defective human tumor cell lines. Cancer Res 57:808–811
Leung SY, Yuen ST, Chung LP (1999) hMLH1 promoter methylation and lack of hMLH1 expression in sporadic gastric carcinomas with high-frequency microsatellite instability. Cancer Res 59:159–164
Liu B, Nicolaides NC, Markowitz S (1995) Mismatch repair gene defects in sporadic colorectal cancers with microsatellite instability. Nat Genet 9:48–55
Richard F, Teresa W, Mut S (1997) Homologs in mammalian cells. Curr Opin Genet Dev 7:105–113
Salvesen HB, MacDonald N, Ryan A, Iversen OE, Jacobs IJ, Akslen LA, Das S (2000) Methylation of hMLH1 in a population-based series of endometrial carcinomas. Clin Cancer Res 6:3607–3613
Tuncer ZS, Vegh GL, Fulop V, Genest DR, Mok SC, Berkowitz RS (2002) Expression of epidermal growth factor receptor-related family products in gestational trophoblastic diseases and normal placenta and its relationship with development of postmolar tumor. Gynecol Oncol 77:389–393
Yamamoto H, Itoh F, Nakamura H, Fukushima H, Sasaki S, Perucho M, Imai K (2001) Genetic and clinical features of human pancreatic ductal adenocarcinomas with widespread microsatellite instability. Cancer Res 61:3139–3144
Zhu YM, Das-Gupta EP, Russell NH (1999) Microsatellite instability and p53 mutations are associated with abnormal expression of the MSH2 gene in adult acute leukemia. Blood 94:733–740
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chen, H., Ye, D., Xie, X. et al. Mismatch repair gene promoter methylation and expression in hydatidiform moles. Arch Gynecol Obstet 272, 35–39 (2005). https://doi.org/10.1007/s00404-004-0665-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-004-0665-3