Abstract
Background
The aim of this study was to establish the prognostic import of spontaneous fetal heart-rate deceleration, a sign of fetal distress.
Methods
This retrospective study enrolled 169 patients with fetal heart-rate deceleration treated at Shin-Kong Wu Ho Su Memorial Hospital from 1 January 1998 to 24 November 2000. Reviewed variables included type of fetal heart-rate irregularity (including early, variable, late, and spontaneous variants), neonatal outcome, Doppler results, gestational age and weight at birth, and amniotic fluid index.
Results
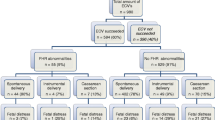
The spontaneous form of fetal heart-rate deceleration was determined for 11 of the 169 patients (6.5%) diagnosed with fetal heart-rate deceleration, with a 5-min Apgar score below 7 observed for 5 (45.5%) of these subjects, and neonatal complications for 9 (81.8%). Mean gestational age was 32.2±3.8 weeks; mean birth weight was 1,560±723.9 g. Spontaneous deceleration has a sensitivity of 29%, specificity of 99%, positive predictive value of 81.8%, and negative predictive value of 86.1%.
Conclusion
Although of the different fetal heart-rate deceleration types the spontaneous variant has the lowest incidence rate, the complication and mortality rates are highest and it is also associated with lower birth weight and higher incidence of pre-term labor. Failure of the fetus to cope with the compromised placental flow and uterine compression resulting from oligohydramnios may be fundamental to the etiology of spontaneous fetal-heart rate deceleration. Once diagnosed, Doppler ultrasound may be used to assess placental-vessel flow. Emergency treatment may be mandatory if deterioration is noted.

Similar content being viewed by others
Abbreviations
- AFI:
-
Amniotic fluid index
- ITP:
-
Idiopathic thrombocytopenic purpura
- GDM:
-
Gestational diabetes mellitus
- SGA:
-
Small for gestational age restriction
- PPV:
-
Positive predictive value
- NPV:
-
Negative predictive value
- S/D ratio:
-
Systolic/diastolic ratio
- bpm:
-
Beats per minute
- IUGR:
-
Intrauterine growth
- IUFD:
-
Intrauterine fetal death
- PPROM:
-
Pre-term premature rupture of membrane
- RDS:
-
Respiratory distress syndrome
References
Barcroft J (1847) Researches on pre-natal life. Thomas, Springfield
Barron DH (1952) The exchange of the respiratory gases in the placenta. Neonatal Stud 1:3
Chan FY, Lam C, Lam YH, To WK, Pun TC, Lee CP (1994) Umbilical artery Doppler velocimetry compared with fetal heart rate monitoring as a labor admission test. Eur J Obstet Gynecol Reprod Biol 54:1–6
Cunningham FG, McDonald PC, Gant MF et al (1996) Intrapartum assessment. In: Cunningham FG, Williams JW (eds) Williams obstetrics, 20th edn. McGraw-Hill, New York, pp 356–357
Daws GS (1985) The control of fetal heart rate and its variability in counts. In: Kunzel W (ed) Fetal heart rate monitoring. Springer, Berlin Heidelberg New York, p 88
FIGO (1987) New guidelines for the use of fetal monitoring. Int J Gynecol Obstet 25:159–167
Fleischer A, Schulman H, Jagani N, Mitchell J, Randolph G (1982) The development of fetal acidosis in the presence of an abnormal fetal heart rate tracing. Am J Obstet Gynecol 144:55–60
Hon EH (1958) The electronic evaluation of the fetal heart rate. Am J Obstet Gynecol 175:1215
Itskovitz J, LaGamma EF, Rudolph AM (1983) Heart rate and blood pressure responses to umbilical cord compression in fetal lambs with special reference to the mechanism of variable deceleration. Am J Obstet Gynecol 147:451–457
James LS, Weisbrot IM, Prince CE et al (1958) The acid-base status of human infants in relation to birth asphyxia and the onset of respiration. J Pediatr 52:379
King RG, Gude NM, DiIulio JL, Brenneck SP (1995) Factors regulation of human placental fetal vessel tone: role of nitric oxide. Reprod Fertil Dev 7:1407–1411
Kubli F, Ruttgers H, Haller V, Bogdan C, Ramzin M (1972) Antepartum fetal heart rate. II. Baseline levels, baseline irregularity and deceleration with antepartum fetal death. Z Geburtshilfe Perinatol 176:309–323
Myatt L, Eis AL, Brockman DE, Greer IA, Lyall F (1997) Endothelial nitric oxide synthase in placental villous tissue from normal, pre-eclamptic and intrauterine growth restricted pregnancies. Hum Reprod 12:167–172
Ogunyemi D, Stanley R, Lynch C, Edwards D, Fukushima T (1992) Umbilical artery velocimetry in predicting perinatal outcome with intrapartum fetal distress. Obstet Gynecol 80:377–380
Pazos R, Vuolo K, Aladjem S, Lueck J, Anderson C (1982) Association of spontaneous fetal heart rate deceleration during antepartum non-stress testing and IUGR. Am J Obstet Gynecol 144:574–577
Phelan JP, Ahn MO, Smith CV, Rutherford SE, Anderson E (1987) Amniotic fluid index measurements during pregnancy. J Reprod Med 32:601–604
Read MA, Leitch IM, Giles WB, Bisits AM, Boura AL, Walter WA (1999) U46619-mediated vasoconstriction of fetal placental vasculature in vitro in normal and hypertensive pregnancy. J Hypertens 17:389–396
Simmons LA, Hennessy A, Gillin AG, Jeremy RW (2000) Uteroplacental blood flow and placental vascular endothelial growth factor in normotensive and pre-eclamptic pregnancy. Br J Obstet Gynaecol 107:678–685
Solum T, Sjoberg N (1980) Antenatal cardiotocography and intrauterine death. Acta Obstet Gynecol Scand 59:481–487
Trimbos JB, Keirse NJNC (1977) Non-specific deceleration in the fetal heart rate during high risk pregnancies. Br J Obstet Gynaecol 84:732–736
Zuspan FP, Quilligan EJ, Iams JD et al (1979) NICHD Consensus Development Task Force Report. Predictors of intrapartum fetal distress; the role of electronic fetal monitoring. J Reprod Med 23:207–212
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chuang, J., Chou, CT., Cheng, WC. et al. Spontaneous fetal heart rate deceleration: an ominous sign for fetal outcome. Arch Gynecol Obstet 269, 254–258 (2004). https://doi.org/10.1007/s00404-002-0354-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-002-0354-z