Abstract
Introduction/objectives
Psoriasis is a chronic inflammatory dermatosis with significant physical and psychological impact leading to negative influence on the quality of life among patients with psoriasis. Other than the disease characteristics many external factors could operate in South Asian context. Lack of a reliable disease-specific instrument prevents objective estimation and monitoring of disability in patients with psoriasis and hence we aim to validate assess the psychometric properties of the Sinhala version of PDI.
Methods
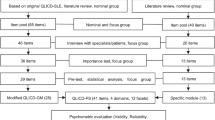
A cross-sectional study conducted at dermatology clinic at a tertiary care National Hospital in Sri Lanka. Patients with psoriasis and on therapy at least 4 weeks prior to enrollment, aged more than 18 years, were included while those with already diagnosed psoriatic arthritis and/or nail psoriasis alone without any skin involvement and generalized pustular psoriasis de novo were excluded. All patients were examined by dermatologist to obtain disease characteristics. The reliability was assessed by internal consistency using Cronbach’s α and item-total correlation. Convergent validity was measured with the known groups.
Results
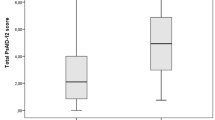
Of 199 patients studied, the PDI Sinhala version showed Cronbach’s α of 0.86 (all 15 items) and ranged from 0.57 to 0.77 for subscales. PDI score and Dermatology Life Quality Index (DLQI) showed good correlation of coefficient 0.76 (p < 0.01). Positive associations were noted with extent and severity of psoriasis when using sample medians (p < 0.05). The dimensionality of the PDI was determined using exploratory factor analysis and four factors were structured.
Conclusion
The PDI Sinhala version is proved to be valid and reliable tool to assess the burden of psoriasis among Sinhala conversant patients in Sri Lanka




Similar content being viewed by others
References
Levenson JL (2008) Psychiatric issues in dermatology, part 1: Atopic dermatitis and psoriasis. Primary psychiatry 15(7):35–38
Richards HL, Fortune DG, Griffiths CE, Main CJ (2001) The contribution of perceptions of stigmatisation to disability in patients with psoriasis. J Psychosom Res 50(1):11–15
Colombo D, Perego R (2013) Quality of life in psoriasis. In: Lima H (ed) Psoriasis-types, causes and medication. IntechOpen. https://doi.org/10.5772/53998
Choi J, Koo JY (2003) Quality of life issues in psoriasis. J Am Acad Dermatol 49(2):57–61
Rapp SR, Feldman SR, Exum ML, Fleischer AB Jr, Reboussin DM (1999) Psoriasis causes as much disability as other major medical diseases. J Am Acad Dermatol 41(3):401–407
Finlay AY, Coles E (1995) The effect of severe psoriasis on the quality of life of 369 patients. Br J Dermatol 132(2):236–244
Ratnayake DRD, Ranasinghe JMSD, Undugodage CM, Dedigama MC, Kamaladasa SD (2009) Assessment of dermatology life quality index (DLQI) in patients attending skin clinics in CSTH. Sri Lanka J Dermatology 13:18–19
Rukshani B, Samarakoon G, Maduka W, Kumarasinghe S, Senadheera A (2017) Physical, social, and psychological impacts of psoriasis. In: Proceeding of the 15th Open University Research Sessions (OURS 2017), The Open University of Sri Lanka, November 2017, ISSN 2012-9916, pp 229–232
Muldoon MF, Barger SD, Flory JD, Manuck SB (1998) What are quality of life measurements measuring? BMJ 316(7130):542
Sampogna F, Sera F, Abeni D (2004) Measures of clinical severity, quality of life, and psychological distress in patients with psoriasis: a cluster analysis. J Investig Dermatol 122(3):602–607
Kitchen H, Cordingley L, Young H, Griffiths C, Bundy C (2015) Patient-reported outcome measures in psoriasis: the good, the bad and the missing! Br J Dermatol 172(5):1210–1221
Finlay A (1997) Quality of life measurement in dermatology: a practical guide. Br J Dermatol 136(3):305–314
Psoriasis Disability Index. Cardiff University. Available via https://www.cardiff.ac.uk/medicine/resources/quality-of-life-questionnaires/psoriasis-disability-index. Accessed 5 Oct 2020
Nijsten T, Whalley D, Gelfand J, Margolis D, McKenna SP, Stern RS (2005) The psychometric properties of the psoriasis disability index in United States patients. J Investig Dermatol 125(4):665–672
Lewis VJ, Finlay AY (2005) Two decades experience of the Psoriasis Disability Index. Dermatology 210(4):261–268
Suraweera C, Hanwella R, Sivayokan S, de Silva V (2013) Rating scales validated for Sri Lankan populations. Sri Lanka J Psychiatry 4(2):16–24
Madarasingha NP, de Silva P, Satgurunathan K (2011) Validation study of Sinhala version of the dermatology life quality index (DLQI). Ceylon Med J 56(1):18–22
Finlay AY, Khan G (1994) Dermatology Life Quality Index (DLQI)—a simple practical measure for routine clinical use. Clin Exp Dermatol 19(3):210–216
Gudu T, Gossec L (2018) Quality of life in psoriatic arthritis. Expert Rev Clin Immunol 14(5):405–417
Imafuku S, Zheng M, Tada Y, Zhang X, Theng C, Thevarajah S et al (2018) Asian consensus on assessment and management of mild to moderate plaque psoriasis with topical therapy. J Dermatol 45(7):805–811
Barker DJP, Hall AJ (1991) Practical epidemiology. Churchill Livingstone, Edinburgh, New York
He Z, Lu C, Ou A, Fang J, Wang D, Deng J et al (2012) Reliability and validity of the Chinese version of the Psoriasis Disability Index (PDI) in Chinese patients with psoriasis. Health Qual Life Outcomes 10(1):37
Mir AA, Chattopadhyay A, Pramanick J, Gautam A, Mir SA, Koley M et al (2020) Psychometric validation of the psoriasis disability index questionnaire (Translated Bengali Version): a cross-sectional study. J Dermatol Dermatol Surg 24(1):25
Zedan HM, Gaber HD, Ibrahim AK, Refaa EZ (2016) Reliability and validity of the Arabic version of the Psoriasis Disability Index questionnaire. J Egypt Women’s Dermatolc Soc 13(3):143–150
Elangasinghe V, Lee KY, Levell NJ (2014) An historical account of dermatology in Buddhist Sri Lankan literature. Int J Dermatol 53(3):390–392
Acknowledgements
The authors acknowledge of Dr. A Y Finlay for granting free license (License ID CUQoL1461) to use the PDI for validation of Sinhala version of Psoriasis Disability Index
Funding
The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. The material preparation was done by Dr. Achala Liyanage and Dr. Gayani Liyanage. Data collection done by Dr. Achala Liyanage, Dr. Janaka Akarawita and Dr. Chalukya Gunasekera. The data analysis was performed by Dr. Achala Liyanage and Prof. Sarath Lekamwasam. The first draft of the manuscript was written by Dr. Achala Liyanage and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
Authors declare no conflicts of interest.
Ethical approval
The study obtained ethical approval from the Ethical Review Committee of Faculty of Medicine, University of Ruhuna (Ref No. 15.02.2018:3.6) and is accordance with the 1964 Helsinki declaration.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Liyanage, A., Liyanage, G., De Silva, V. et al. Validation of psoriasis disability index (PDI) questionnaire Sinhala version. Arch Dermatol Res 314, 61–69 (2022). https://doi.org/10.1007/s00403-021-02210-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00403-021-02210-5