Abstract
Background
Traditionally, second intent healing (SIH) in the periocular region is reserved for small and/or concave defects, particularly those located on the medial canthus.
Aim
The purpose of this study was to identify factors impacting outcomes of SIH for periocular tumors following Mohs micrographic surgery (MMS).
Methods
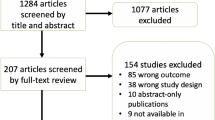
Retrospective analysis was performed of all periocular lesions treated with MMS followed by SIH from a single academic surgical center over a 5-year period. Data regarding tumor characteristics and follow-up was recorded. The modified Manchester scale was utilized to evaluate scar outcomes.
Results
Of the 39 tumors included, 14 (35.9%) were located on the lower eyelid, 12 (30.8%) on the upper eyelid, 6 (15.4%) on the lateral canthus, and 7 (17.9%) on the medial canthus. Involvement of the eyelid margin was seen in 11 (28.2%) of cases. The average defect diameter and area were 1.3 cm and 1.04 cm-squared. Twenty-three cases (59.0%) healed with optimal results. Larger defects were significantly associated with poorer outcomes of SIH (odds ratio 0.205, p = 0.017 by multivariate analysis). Anatomic location, involvement of the lid margin, age, and follow-up interval were not significant factors; however, medial canthus defects were least likely to heal with optimal results. On average, medial canthal lesions were larger in size (mean diameter 1.76 cm, mean area 1.97 cm-squared).
Conclusions
This retrospective study suggests that periorbital defects in all locations with area less than 1.04 cm2 heal well by SIH. In this cohort, larger lesions on the medial canthus healed with worse outcomes.




Similar content being viewed by others
Availability of data and material
All data was available to each of the authors during the process.
References
Cook BE, Bartley GB (2001) Treatment options and future prospects for the management of eyelid malignancies: an evidence-based update. Ophthalmology 108:2088–2098. https://doi.org/10.1016/s0161-6420(01)00796-5
Connolly SM, Baker DR, Coldiron BM, Fazio MJ, Storrs PA, Vidimos AT, Zalla MJ, Brewer JD, Smith Begolka W, Berger TG, Bigby M, Bolognia JL, Brodland DG, Collins S, Cronin TA Jr, Dahl MV, Grant-Kels JM, Hanke CW, Hruza GJ, James WD, Lober CW, McBurney EI, Norton SA, Roenigk RK, Wheeland RG, Wisco OJ (2012) AAD/ACMS/ASDSA/ASMS 2012 appropriate use criteria for Mohs micrographic surgery: a report of the american academy of dermatology, american college of mohs surgery, american society for dermatologic surgery association, and the american society for mohs surgery. J Am Acad Dermatol 67:531–550. https://doi.org/10.1016/j.jaad.2012.06.009
Lowry JC, Bartley GB, Garrity JA (1997) The role of second-intention healing in periocular reconstruction. Ophthalmic Plast Reconstr Surg 13:174–188
Lam L, Weatherhead R (2015) Photographic essay: healing by secondary intention in oculoplastics. Semin Ophthalmol 30:221–223. https://doi.org/10.3109/08820538.2013.835846
Morton JD (2016) Defining the role of secondary intention healing in full-thickness lid margin defects. Plast Reconstr Surg 138:95e–103e. https://doi.org/10.1097/prs.0000000000002252
Zitelli JA (1983) Wound healing by secondary intention. A cosmetic appraisal. J Am Acad Dermatol 9:407–415
Trieu DN, Drosou A, White LE, Goldberg LH (2019) Outcomes of second intention healing of the lower eyelid margin after mohs micrographic surgery. Dermatol Surg 45:884–889. https://doi.org/10.1097/dss.0000000000001951
Jang JU, Kim SY, Yoon ES, Kim WK, Park SH, Lee BI, Kim DW (2016) Comparison of the effectiveness of ablative and non-ablative fractional laser treatments for early stage thyroidectomy scars. Archiv Plastic Surg 43:575–581. https://doi.org/10.5999/aps.2016.43.6.575
Beausang E, Floyd H, Dunn KW, Orton CI, Ferguson MW (1998) A new quantitative scale for clinical scar assessment. Plast Reconstr Surg 102:1954–1961. https://doi.org/10.1097/00006534-199811000-00022
Mehta HK (1981) Spontaneous reformation of lower eyelid. British J Ophthalmol 65:202–208. https://doi.org/10.1136/bjo.65.3.202
Mott KJ, Clark DP, Stelljes LS (2003) Regional variation in wound contraction of mohs surgery defects allowed to heal by second intention. Dermatol Surg 29:712–722
Morton J (2010) Secondary intention healing in lower eyelid reconstruction–a valuable treatment option. JPRAS 63:1921–1925. https://doi.org/10.1016/j.bjps.2010.03.005
Chang EI, Esmaeli B, Butler CE (2018) Reply: defining the role of secondary intention healing in full-thickness lid margin defects. Plast Reconstr Surg 141:786e–787e. https://doi.org/10.1097/prs.0000000000004305
Morton JD (2018) Defining the role of secondary intention healing in full-thickness lid margin defects. Plast Reconstr Surg 141:785e–786e. https://doi.org/10.1097/prs.0000000000004304
Cook JL, Perone JB (2003) A prospective evaluation of the incidence of complications associated with Mohs micrographic surgery. Arch Dermatol 139:143–152. https://doi.org/10.1001/archderm.139.2.143
Mohs F (1958) The chemosurgical method for the microscopically controlled excision of external cancer with reference to eyelid. Trans Am Acad Ophthalmol Otolaryngol 62:355–356
Acknowledgements
This work did not receive any funding sources.
Funding
This work received no funding resources.
Author information
Authors and Affiliations
Contributions
NK, YK, and KS performed the chart review and data extraction; NK, KS, and SRC analyzed the data; NK, YK, DL, SC, and KS were involved in writing the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kibbi, N., Khan, Y., Leffell, D.J. et al. Predicting outcomes following second intent healing of periocular surgical defects. Arch Dermatol Res 313, 483–489 (2021). https://doi.org/10.1007/s00403-020-02122-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00403-020-02122-w