Abstract
Background
Osteonecrosis of the humeral head (ONHH) is a severe complication after the internal fixation of proximal humeral fractures (IFPHF). The risk factors remain controversial though many studies have reported. In this research, meta-analysis was used to evaluate which surgeon-level factors can be modified to lower the risk and we hope to provide evidence-based support for preventing ONHH.
Methods
Literature was retrieved from PubMed, Cochrane Library, Embase, Web of Science, and Scopus for eligible studies published up to January 2023. The pooled odds ratios (ORs) were calculated with their corresponding 95% confidence intervals (CIs) to evaluate. STATA 15.1 software was applied for data synthesis, sensitivity synthesis, and publication bias.
Results
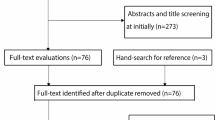
45 articles were published between 2000 and 2022, and 2482 patients were finally included. All articles were observational research, with 7 case–control studies and 38 cohort studies, and the Newcastle Ottawa Scale (NOS) score ranged from 7 to 9. The pooled results suggested that age (OR 0.32, 95% CI 0.14–0.74, P = 0.01), reduction quality (OR 0.08, 95% CI 0.01–0.44, P = 0.00), fracture type (OR 0.44, 95% CI 0.25–0.78, P = 0.01), surgical approach (OR: 4.06, 95% CI 1.21–13.61, P = 0.02) and fixation implant (OR = 0.68, 95% CI = 0.34–1.33, P = 0.02) were risk factors for ONHH after IFPHF. According to sensitivity analysis, Begg (P = 0.42) and Egger (P = 0.68) tests, the results were stable and exhibited no publication bias.
Conclusions
The study showed that age, reduction quality, fracture type, surgical approach and fixation implant were risk factors for ONHH after IFPHF, while gender, varus or valgus, timely operation, injured side, and the existence of medial support have little influence on ONHH, as they could not be considered risk factors and still need further investigations.





Similar content being viewed by others
Data availability
The data presented in this study are available on request from the corresponding author.
Code availability
Not applicable.
References
Calvo E, Morcillo D, Foruria AM, Redondo-Santamaría E, Osorio-Picorne F, Caeiro JR (2011) Nondisplaced proximal humeral fractures: high incidence among outpatient-treated osteoporotic fractures and severe impact on upper extremity function and patient subjective health perception. J Shoulder Elbow Surg 20(5):795–801
Sanchez-Sotelo J (2018) Proximal humerus fractures. Mayo Clinic Principles of Shoulder Surgery
Maier D, Jaeger M, Izadpanah K, Strohm PC, Suedkamp NP (2014) Proximal humeral fracture treatment in adults. J Bone Jt Surg 96(3):251–261
Miquel J, Martínez R, Santana F, Marimon P, Torrens C (2021) Surgical treatment of proximal humeral fractures with the transosseous suture fixation. J Orthop Surg Res 16(1):405
Neviaser RJ, Resch H, Neviaser AS, Crosby LA (2015) Proximal humeral fractures: pin, plate, or replace. Instr Course Lect 64:203–214
Gómez-Mont Landerreche JG, Gil-Orbezo F, Morales-Domínguez H, Flores-Carrillo A, Levy-Holden G, Capuano-Tripp P (2015) Proximal humerus fractures: clinical assessment and functional outcome in patients with osteonecrosis of the humeral head. Acta Ortop Mex 29(2):88–96
Howard L, Berdusco R, Momoli F et al (2018) Open reduction internal fixation vs non-operative management in proximal humerus fractures: a prospective, randomized controlled trial protocol. BMC Musculoskelet Disord 19(1):299
Helfen T, Siebenbürger G, Fleischhacker E, Biermann N, Böcker W, Ockert B (2018) Open reduction and internal fixation of displaced proximal humeral fractures. Does the surgeon’s experience have an impact on outcomes? PLoS ONE 13(11):e0207044
Franceschi F, Franceschetti E, Paciotti M et al (2017) Surgical management of osteonecrosis of the humeral head: a systematic review. Knee Surg Sports Traumatol Arthrosc 25(10):3270–3278
Harreld KL, Marker DR, Wiesler ER, Shafiq B, Mont MA (2009) Osteonecrosis of the humeral head. J Am Acad Orthop Surg 17(6):345–355
Gruson KI, Kwon YW (2009) Atraumatic osteonecrosis of the humeral head. Bull NYU Hosp Jt Dis 67(1):6–14
Large TM, Adams MR, Loeffler BJ, Gardner MJ (2019) Posttraumatic avascular necrosis after proximal femur, proximal humerus, talar neck, and scaphoid fractures. J Am Acad Orthop Surg 27(21):794–805
Da Silva T, Ehrhard DB, Chuchuy TM, Knop C, Merkle T (2022) Protective and risk factors for humerus head necrosis after proximal humerus fracture treated with internal locking plate. Indian J Orthopaed 56(3):429–436
Hertel R, Hempfing A, Stiehler M, Leunig M (2004) Predictors of humeral head ischemia after intracapsular fracture of the proximal humerus. J Shoulder Elbow Surg 13(4):427–433
Aaron D, Shatsky J, Paredes JC, Jiang C, Parsons BO, Flatow EL (2013) Proximal humeral fractures: internal fixation. Instr Course Lect 62:143–154
Patel S, Colaco HB, Elvey ME, Lee MH (2015) Post-traumatic osteonecrosis of the proximal humerus. Injury 46(10):1878–1884
Hasan SS, Romeo AA (2002) Nontraumatic osteonecrosis of the humeral head. J Shoulder Elbow Surg 11(3):281–298
Moher D, Liberati A, Tetzlaff J, Altman DG (2010) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg (Lond, Engl) 8(5):336–341
Wells GA, Shea B, O'Connell J (2014) The Newcastle-Ottawa scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses
Soliman OA, Koptan WM (2013) Four-part fracture dislocations of the proximal humerus in young adults: results of fixation. Injury 44(4):442–447
Gavaskar AS, Tummala NC (2015) Locked plate osteosynthesis of humeral head-splitting fractures in young adults. J Shoulder Elbow Surg 24(6):908–914
Dimitriou D, Waldmann S, Antoniadis A, Liebhauser M, Helmy N, Riede U (2020) Early locking plate removal following open reduction and internal fixation of proximal humeral fractures could prevent secondary implant-related complications. J Orthop 17:106–109
Pak P, Eng K, Page RS (2013) Fixed-angle locking proximal humerus plate: an evaluation of functional results and implant-related outcomes. ANZ J Surg 83(11):878–882
Kloub M, Holub K, Urban J, Látal P, Peml M, Křivohlávek M (2019) Intramedullary nailing of displaced four-part fractures of the proximal humerus. Injury 50(11):1978–1985
Ogawa K, Kobayashi S, Ikegami H (2011) Retrograde intramedullary multiple pinning through the deltoid “V” for valgus-impacted four-part fractures of the proximal humerus. J Trauma 71(1):238–244
Hinds RM, Garner MR, Tran WH, Lazaro LE, Dines JS, Lorich DG (2015) Geriatric proximal humeral fracture patients show similar clinical outcomes to non-geriatric patients after osteosynthesis with endosteal fibular strut allograft augmentation. J Shoulder Elbow Surg 24(6):889–896
Wachtl SW, Marti CB, Hoogewoud HM, Jakob RP, Gautier E (2000) Treatment of proximal humerus fracture using multiple intramedullary flexible nails. Arch Orthop Trauma Surg 120(3–4):171–175
Schnetzke M, Bockmeyer J, Loew M, Studier-Fischer S, Grützner PA, Guehring T (2018) Rate of avascular necrosis after fracture dislocations of the proximal humerus: timing of surgery. Obere Extremitat 13(4):273–278
Thalhammer G, Platzer P, Oberleitner G, Fialka C, Greitbauer M, Vécsei V (2009) Angular stable fixation of proximal humeral fractures. J Trauma 66(1):204–210
Barco R, Barrientos I, Encinas C, Antuña SA (2012) Minimally invasive poly-axial screw plating for three-part fractures of the proximal humerus. Injury 43(Suppl 2):S7-11
Handschin AE, Cardell M, Contaldo C, Trentz O, Wanner GA (2008) Functional results of angular-stable plate fixation in displaced proximal humeral fractures. Injury 39(3):306–313
Gorschewsky O, Puetz A, Klakow A, Pitzl M, Neumann W (2005) The treatment of proximal humeral fractures with intramedullary titanium helix wire by 97 patients. Arch Orthop Trauma Surg 125(10):670–675
Jung WB, Moon ES, Kim SK, Kovacevic D, Kim MS (2013) Does medial support decrease major complications of unstable proximal humerus fractures treated with locking plate? BMC Musculoskelet Disord 14:102
Archer LA, Furey A (2016) Rate of avascular necrosis and time to surgery in proximal humerus fractures. Musculoskelet Surg 100(3):213–216
Willauschus M, Schram L, Millrose M et al (2022) Specific radiologic risk factors for implant failure and osteonecrosis of the humeral head after interlocking nailing with the targon PH(+) of proximal humeral fractures in a middle to old population. J Clin Med 11:9
Belayneh R, Lott A, Haglin J, Konda S, Zuckerman JD, Egol KA (2018) Osteonecrosis after surgically repaired proximal humerus fractures is a predictor of poor outcomes. J Orthop Trauma 32(10):e387–e393
Mohan K, Hintze JM, Morrissey D, Molony D (2021) Incidence of avascular necrosis following biceps tenodesis during proximal humerus open reduction and internal fixation. Acta Orthop Belg 87(2):339–346
Borer J, Schwarz J, Potthast S et al (2020) Mid-term results of minimally invasive deltoid-split versus standard open deltopectoral approach for PHILOS™ (proximal humeral internal locking system) osteosynthesis in proximal humeral fractures. Eur J Trauma Emerg Surg 46(4):825–834
Solberg BD, Moon CN, Franco DP, Paiement GD (2009) Locked plating of 3- and 4-part proximal humerus fractures in older patients: the effect of initial fracture pattern on outcome. J Orthop Trauma 23(2):113–119
Foruria AM, Martinez-Catalan N, Valencia M, Morcillo D, Calvo E (2021) Proximal humeral fracture locking plate fixation with anatomic reduction, and a short-and-cemented-screws configuration, dramatically reduces the implant related failure rate in elderly patients. JSES Int 5(6):992–1000
Büyükkuşcu M, Kulduk A, Mısır A, Çetinkaya E, Çamurcu İY, Gürsu ŞS (2020) Effect of surgical approaches on deltoid innervation and clinical outcomes in the treatment of proximal humeral fractures. Jt Dis Related Surg 31(3):515–522
Hepp P, Theopold J, Voigt C, Engel T, Josten C, Lill H (2008) The surgical approach for locking plate osteosynthesis of displaced proximal humeral fractures influences the functional outcome. J Shoulder Elbow Surg 17(1):21–28
Wu CH, Ma CH, Yeh JJ, Yen CY, Yu SW, Tu YK (2011) Locked plating for proximal humeral fractures: differences between the deltopectoral and deltoid-splitting approaches. J Trauma 71(5):1364–1370
Dimakopoulos P, Panagopoulos A, Kasimatis G (2007) Transosseous suture fixation of proximal humeral fractures. J Bone Jt Surg 89(8):1700–1709
Schnetzke M, Bockmeyer J, Porschke F, Studier-Fischer S, Grützner PA, Guehring T (2016) Quality of reduction influences outcome after locked-plate fixation of proximal humeral type-C fractures. J Bone Jt Surg 98(21):1777–1785
Kloub M, Holub K, Polakova S (2014) Nailing of three- and four-part fractures of the humeral head—long-term results. Injury 45(Suppl 1):S29-37
Hung CY, Yeh CY, Wen PC, Yeh WL, Lin SJ (2022) The effect of medial calcar support on proximal humeral fractures treated with locking plates. J Orthop Surg Res 17(1):467
Shen P, Zhu Y, Zhu L, Li X, Xu Y (2019) Effects of medial support screws on locking plating of proximal humerus fractures in elderly patients: a retrospective study. Ann Transl Med 7(20):560
Osterhoff G, Ossendorf C, Wanner GA, Simmen HP, Werner CM (2011) The calcar screw in angular stable plate fixation of proximal humeral fractures–a case study. J Orthop Surg Res 6:50
Zhao L, Qi YM, Yang L et al (2019) Comparison of the effects of proximal humeral internal locking system (PHILOS) alone and PHILOS combined with fibular allograft in the treatment of neer three- or four-part proximal humerus fractures in the elderly. Orthop Surg 11(6):1003–1012
Halvachizadeh S, Berk T, Rauer T et al (2020) Treatment of proximal humerus fractures in geriatric patients—Can pathological DEXA results help to guide the indication for allograft augmentation? PLoS ONE 15(4):e0230789
Cui X, Chen H, Ma B, Fan W, Li H (2019) Fibular strut allograft influences reduction and outcomes after locking plate fixation of comminuted proximal humeral fractures in elderly patients: a retrospective study. BMC Musculoskelet Disord 20(1):511
Lee SH, Han SS, Yoo BM, Kim JW (2019) Outcomes of locking plate fixation with fibular allograft augmentation for proximal humeral fractures in osteoporotic patients: comparison with locking plate fixation alone. Bone Jt J 101(3):260–265
Chen H, Yin P, Wang S et al (2018) The augment of the stability in locking compression plate with intramedullary fibular allograft for proximal humerus fractures in elderly people. Biomed Res Int 2018:3130625
Kim YK, Kang SW, Jung KH, Oh YK (2022) The potential of locking plate with intramedullary fibular allograft to manage proximal humeral fracture with an unstable medial column. Arch Orthop Trauma Surg 142(1):91–97
Lorenz G, Schönthaler W, Huf W, Komjati M, Fialka C, Boesmueller S (2021) Complication rate after operative treatment of three- and four-part fractures of the proximal humerus: locking plate osteosynthesis versus proximal humeral nail. Eur J Trauma Emerg Surg 47(6):2055–2064
Gadea F, Favard L, Boileau P et al (2016) Fixation of 4-part fractures of the proximal humerus: can we identify radiological criteria that support locking plates or IM nailing? Comparative, retrospective study of 107 cases. Orthopaed Traumatol Surg Res OTSR 102(8):963–970
Matziolis D, Kaeaeb M, Zandi SS, Perka C, Greiner S (2010) Surgical treatment of two-part fractures of the proximal humerus: comparison of fixed-angle plate osteosynthesis and Zifko nails. Injury 41(10):1041–1046
Konrad G, Audigé L, Lambert S, Hertel R, Südkamp NP (2012) Similar outcomes for nail versus plate fixation of three-part proximal humeral fractures. Clin Orthop Relat Res 470(2):602–609
Lan W, Xie F, Que W, Tu X, Wang X (2022) Efficacy of intramedullary nailing in the treatment of comminuted proximal humeral fractures and its influence on shoulder joint function recovery. J Healthc Eng 2022:7272385
Neer CS 2nd (1970) Displaced proximal humeral fractures. I. Classification and evaluation. J Bone Jt Surg 52(6):1077–1089
Cadet ER, Ahmad CS (2012) Hemiarthroplasty for three- and four-part proximal humerus fractures. J Am Acad Orthop Surg 20(1):17–27
Zlotolow DA, Catalano LW 3rd, Barron OA, Glickel SZ (2006) Surgical exposures of the humerus. J Am Acad Orthop Surg 14(13):754–765
Chou YC, Tseng IC, Chiang CW, Wu CC (2013) Shoulder hemiarthroplasty for proximal humeral fractures: comparisons between the deltopectoral and anterolateral deltoid-splitting approaches. J Shoulder Elbow Surg 22(8):e1-7
Clavert P, Hatzidakis A, Boileau P (2016) Anatomical and biomechanical evaluation of an intramedullary nail for fractures of proximal humerus fractures based on tuberosity fixation. Clin Biomech (Bristol, Avon) 32:108–112
Shi X, Liu H, Xing R et al (2019) Effect of intramedullary nail and locking plate in the treatment of proximal humerus fracture: an update systematic review and meta-analysis. J Orthop Surg Res 14(1):285
Wijgman AJ, Roolker W, Patt TW, Raaymakers EL, Marti RK (2002) Open reduction and internal fixation of three and four-part fractures of the proximal part of the humerus. J Bone Jt Surg 84(11):1919–1925
Crosby LA, Finnan RP, Anderson CG, Gozdanovic J, Miller MW (2009) Tetracycline labeling as a measure of humeral head viability after 3- or 4-part proximal humerus fracture. J Shoulder Elbow Surg 18(6):851–858
Fuster JJ, Andrés V (2006) Telomere biology and cardiovascular disease. Circ Res 99(11):1167–1180
Minamino T, Mitsialis SA, Kourembanas S (2001) Hypoxia extends the life span of vascular smooth muscle cells through telomerase activation. Mol Cell Biol 21(10):3336–3342
Ahluwalia A, Narula J, Jones MK, Deng X, Tarnawski AS (2010) Impaired angiogenesis in aging myocardial microvascular endothelial cells is associated with reduced importin alpha and decreased nuclear transport of HIF1 alpha: mechanistic implications. J Physiol Pharmacol 61(2):133–139
Harman D (1972) The biologic clock: the mitochondria? J Am Geriatr Soc 20(4):145–147
Hoenig MR, Bianchi C, Rosenzweig A, Sellke FW (2008) Decreased vascular repair and neovascularization with ageing: mechanisms and clinical relevance with an emphasis on hypoxia-inducible factor-1. Curr Mol Med 8(8):754–767
Acknowledgements
None.
Funding
This research received no external funding.
Author information
Authors and Affiliations
Contributions
The authors confirm contribution toward study conception and design: ZXO, QYF and MQZ; Data collection: ZXO and QYF; Analysis and interpretation of results: ZXO, QYF, MQZ and LQP; Draft manuscript preparation: ZXO, QYF, MQZ and LQP, SR, XT. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent to publish
The authors affirm that human research participants provided informed consent for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ou, Z., Feng, Q., Peng, L. et al. Risk factors for osteonecrosis of the humeral head after internal fixation of proximal humeral fractures: a systematic review and meta-analysis. Arch Orthop Trauma Surg 144, 31–40 (2024). https://doi.org/10.1007/s00402-023-05020-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-05020-8