Abstract
Purpose
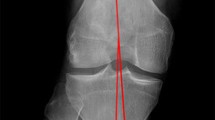
To determine the effect of saucerization surgery on knee joint morphology associated with a complete discoid lateral meniscus (DLM) using magnetic resonance (MR) imaging.
Methods
This retrospective study included cases had undergone saucerization surgery for symptomatic DLM between 2007 and 2022. All cases were divided into two by age group: < 12 (U13) and > 13 (O13). The cases in the match group were randomly selected from preoperative cases in the O13 group matched with the age at the final follow-up (F/U) of cases in the U13 group. The following morphological parameters were evaluated using MR images preoperatively and at the final postoperative F/U in each group: anterior obliquity of the lateral tibial plateau (AOLTP), posterior obliquity of the lateral tibial plateau (POLTP), and the lowest point of the lateral femoral condyle (LPLFC). Each parameter was compared between the U13 preoperative (pre-OP) group and the O13 pre-OP group, the preoperative and final follow-up in the U13, and the U13 group at the final F/U and the match group preoperatively.
Results
A total of 77 cases were evaluated. 31 cases were in the U13 pre-OP group and 46 were in the O13 pre-OP group. With a minimal F/U of 2 years, 27 cases in the U13 group and 36 in the O13 group were included. The mean F/U period was 4.6 years in the U13 group and 3.2 years in the O13 group. 32 cases were included in the match group. In the match group, the inclination of the POLTP was significantly larger (P = 0.042) and the LPLFC was more lateral (P = 0.0034) than at the final F/U in the U13 group.
Conclusions
Saucerization surgery for DLM in juvenile patients can prevent progression to the characteristic bone morphology DLM. These results could help the surgeon making the decision when the surgery would be performed for symptomatic DLM patients.
Level of evidence
Retrospective comparative study; level of evidence, 3.





Similar content being viewed by others
Data availability
The data associated with this study is available from the corresponding author on reasonable request.
Abbreviations
- DLM:
-
Discoid lateral meniscus
- MR:
-
Magnetic resonance
- AOLTP:
-
Anterior obliquity of the lateral tibial plateau
- POLTP:
-
Posterior obliquity of the lateral tibial plateau
- LPLFC:
-
Lowest point of the lateral femoral condyle
References
Atay OA, Pekmezci M, Doral MN, Sargon MF, Ayvaz M, Johnson DL (2007) Discoid meniscus: an ultrastructural study with transmission electron microscopy. Am J Sports Med 35(3):475–478
Habata T, Uematsu K, Kasanami R, Hattori K, Takakura Y, Tohma Y, Fujisawa Y (2006) Long-term clinical and radiographic follow-up of total resection for discoid lateral meniscus. Arthroscopy 22(12):1339–1343
Räber DA, Friederich NF, Hefti F (1998) Discoid lateral meniscus in children. Long-term follow-up after total meniscectomy. J Bone Joint Surg Am 80(11):1579–1586
Wang J, Xiong J, Xu Z, Shi H, Dai J, Jiang Q (2015) Short-term effects of discoid lateral meniscectomy on the axial alignment of the lower limb in adolescents. J Bone Joint Surg Am 97(3):201–207
Zhang P, Zhao Q, Shang X, Wang Y (2018) Effect of arthroscopic resection for discoid lateral meniscus on the axial alignment of the lower limb. Int Orthop 42(8):1897–1903
Lee CR, Bin SI, Kim JM, Lee BS, Kim NK (2018) Arthroscopic partial meniscectomy in young patients with symptomatic discoid lateral meniscus: an average 10-year follow-up study. Arch Orthop Trauma Surg 138(3):369–376
Li M, Liu H, He ZY, Di ZL, Zhang JH, Jin QH (2015) Lessons learned from a case with valgus deformity of the knee following partial removal of lateral discoid meniscus. Chin Med J (Engl) 128(21):2967–2968
Smith RA, Vandenberg CD, Pace JL (2018) Management of long-term complications in the setting of lateral meniscal deficiency after saucerization of a discoid lateral meniscus in an adolescent patient: a case report and review of the literature. JBJS Case Connect 8(4):e102
Okazaki K, Miura H, Matsuda S, Hashizume M, Iwamoto Y (2006) Arthroscopic resection of the discoid lateral meniscus: long-term follow-up for 16 years. Arthroscopy 22:967–971
Abdon P, Turner MS, Pettersson H, Lindstrand A, Stenstrom A, Swanson AJ (1990) A long-term follow-up study of total meniscectomy in children. Clin Orthop Relat Res 257:166–170
Manzione M, Pizzutillo PD, Peoples AB, Schweizer PA (1983) Meniscectomy in children: a long-term follow-up study. Am J Sports Med 11:111–115
Logan CA, Tepolt FA, Kocher SD, Feroe AG, Micheli LJ, Kocher MS (2021) Symptomatic discoid meniscus in children and adolescents: a review of 470 cases. J Pediatr Orthop 41(8):496–501
Yamasaki S, Hashimoto Y, Takigami J, Terai S, Takahashi S, Nakamura H (2017) Risk factors associated with knee joint degeneration after arthroscopic reshaping for juvenile discoid lateral meniscus. Am J Sports Med 45(3):570–577
Ng YH, Tan SHS, Lim AKS, Hui JH (2021) Meniscoplasty leads to good mid-term to long-term outcomes for children and adolescents with discoid lateral meniscus. Knee Surg Sports Traumatol Arthrosc 29(2):352–357
Ahn JH, Kim K, Wang JH, Jeon JW, Cho YC, Lee SH (2015) Long-term results of arthroscopic reshaping for symptomatic discoid lateral meniscus in children. Arthroscopy 31(5):867–873
Perkins CA, Busch MT, Christino MA, Willimon SC (2021) Saucerization and repair of discoid lateral menisci with peripheral rim instability: intermediate-term outcomes in children and adolescents. J Pediatr Orthop 41(1):23–27
Tagliero AJ, Kennedy NI, Leland DP, Camp CL, Milbrandt TA, Stuart MJ, Krych AJ (2020) Meniscus repairs in the adolescent population-safe and reliable outcomes: a systematic review. Knee Surg Sports Traumatol Arthrosc 28(11):3587–3596
Hagino T, Ochiai S, Senga S, Yamashita T, Wako M, Ando T, Haro H (2017) Arthroscopic treatment of symptomatic discoid meniscus in children. Arch Orthop Trauma Surg 137(1):89–94
Kose O, Celiktas M, Egerci OF, Guler F, Ozyurek S, Sarpel Y (2015) Prognostic factors affecting the outcome of arthroscopic saucerization in discoid lateral meniscus: a retrospective analysis of 48 cases. Musculoskelet Surg 99(2):165–170
Chadel B, Morin V, Saragaglia D (2015) Meniscoplasty for lateral discoid meniscus tears: Long-term results of 14 cases. Orthop Traumatol Surg Res 101(6):699–702
Sabbag OD, Hevesi M, Sanders TL, Camp CL, Dahm DL, Levy BA, Stuart MJ, Krych AJ (2019) High rate of recurrent meniscal tear and lateral compartment osteoarthritis in patients treated for symptomatic lateral discoid meniscus: a population-based study. Orthop J Sports Med 7(7):19
Choi NH (2006) Radial displacement of lateral meniscus after partial meniscectomy. Arthroscopy 22(5):575.e1–4
Lee YS, Teo SH, Ahn JH, Lee OS, Lee SH, Lee JH (2017) Systematic review of the long-term surgical outcomes of discoid lateral meniscus. Arthroscopy 33(10):1884–1895
Choi SH, Ahn JH, Kim KI, Ji SK, Kang SM, Kim JS, Lee SH (2015) Do the radiographic findings of symptomatic discoid lateral meniscus in children differ from normal control subjects? Knee Surg Sports Traumatol Arthrosc 23:1128–1134
Ha CW, Jang JW, Kim M, Na SE, Lee HJ, Park YB (2017) The utility of the radiographic condylar cut-off sign in children and adolescents with complete discoid lateral meniscus. Knee Surg Sports Traumatol Arthrosc 25:3862–3868
Hino T, Furumatsu T, Fujii M, Kodama Y, Miyazawa S, Kamatsuki Y, Yamada K, Ozaki T (2017) Tibial eminence width can predict the presence of complete discoid lateral meniscus: a preliminary study. J Orthop Sci 22:1084–1088
Jiang W, Li X, Su H, Yang C (2016) A new method to diagnose discoid lateral menisci on radiographs. Knee Surg Sports Traumatol Arthrosc 24:1519–1524
Kim SJ, Moon SH, Shin JS (2000) Radiographic knee dimensions in discoid lateral meniscus: comparison with normal control. Arthroscopy 16:511–516
Milewski MD, Krochak R, Duarte AJ, Marchese JW, Kostyun RO, Pace JL, Broom AM, Solomito MJ (2018) Do age and weightbearing radiographs affect lateral joint space and fibular height measurements in patients with discoid lateral meniscus? Orthop J Sports Med 6:1–7
Park YB, Ha CW, Jang JW, Kim M, Lee HJ, Park YG (2018) Prediction models to improve the diagnostic value of plain radiographs in children with complete discoid lateral meniscus. Arthroscopy 34:479–489
Song JG, Hana JH, Kwon JH, Shetty GM, Franco LAM, Kwon DY, Nha KW (2015) Radiographic evaluation of complete and incomplete discoid lateral meniscus. Knee 22:163–168
Kinoshita T, Hashimoto Y, Nishida Y, Iida K, Nakamura H (2022) Evaluation of knee bone morphology in juvenile patients with complete discoid lateral meniscus using magnetic resonance imaging. Arch Orthop Trauma Surg 142(4):649–655
Xu Z, Chen D, Shi D, Dai J, Yao Y, Jiang Q (2016) Evaluation of posterior lateral femoral condylar hypoplasia using axial MRI images in patients with complete discoid meniscus. Knee Surg Sports Traumatol Arthrosc 24:909–914
Suga N, Nakasa T, Ishikawa M, Nakamae A, Hayashi S, Yoshikawa M, Sumida Y, Tsuyuguchi Y, Adachi N (2018) Characteristic morphology of the proximal tibiofibular joint in patients with discoid lateral meniscus. Knee 25(6):1027–1032
Kinoshita T, Hashimoto Y, Iida K, Nakamura H (2022) Evaluation of the knee joint morphology associated with a complete discoid lateral meniscus, as a function of skeletal maturity, using magnetic resonance imaging. Arch Orthop Trauma Surg 2022:15
Kim JH, Bin S, Lee BS, Kim JM, Kim NK, Lee CR (2018) Does discoid lateral meniscus have inborn peripheral rim instability? Comparison between intact discoid lateral meniscus and normal lateral meniscus. Arch Orthop Trauma Surg 138:1725–1730
Rohren EM, Kosarek FJ, Helms CA (2001) Discoid lateral meniscus and the frequency of meniscal tears. Skeletal Radiol 30:316–320
Samoto N, Kozuma M, Tokuhisa T, Kobayashi K (2002) Diagnosis of discoid lateral meniscus of the knee on MR imaging. Magn Reson Imaging 20:59–64
Nishino K, Hashimoto Y, Nishida Y, Yamasaki S, Nakamura H (2021) Magnetic resonance imaging T2 relaxation times of articular cartilage before and after arthroscopic surgery for discoid lateral meniscus. Arthroscopy 37(2):647–654
Ahn JH, Lee SH, Yoo JC, Lee YS, Ha HC (2008) Arthroscopic partial meniscectomy with repair of the peripheral tear for symptomatic discoid lateral meniscus in children: results of minimum 2 years of follow-up. Arthroscopy 24(8):888–898
Hashimoto Y, Yamasaki S, Reid JB 3rd, Guttmann D, Nishino K, Nakamura H (2021) Arthroscopic saucerization with inside-out repair and anterocentral shift of a discoid lateral meniscus with retention of adequate volume of residual meniscus. Arthrosc Tech 10(11):e2553–e2557
Hashimoto Y, Yamasaki S, Reid JB 3rd, Guttmann D, Nishino K, Nakamura H (2022) Surgical management of discoid lateral meniscus with anterior peripheral instability: retaining an adequate residual meniscus volume. Arthrosc Tech 11(7):e1141–e1147
Zhang F, Zeinstra SMB, Oei EHG, Turkiewicz A, Englund M, Runhaar J (2017) Factors associated with meniscal body extrusion on knee MRI in overweight and obese women. Osteoarthr Cartil 25:694–699
Takigami J, Hashimoto Y, Tomihara T, Yamasaki S, Tamai K, Kondo K, Nakamura H (2018) Predictive factors for osteochondritis dissecans of the lateral femoral condyle concurrent with a discoid lateral meniscus. Knee Surg Sports Traumatol Arthrosc 26(3):799–805
Mitsuoka T, Shino K, Hamada M, Horibe S (1999) Osteochondritis dissecans of the lateral femoral condyle of the knee joint. Arthroscopy 15(1):20–26
Yamaguchi M, Chosa E, Tajima T, Morita Y, Yokoe T (2022) Symptomatic discoid lateral meniscus shows a relationship between types and tear patterns, and between causes of clinical symptom onset and the age distribution. Knee Surg Sports Traumatol Arthrosc 30(4):1436–1442
Ahn JH, Lee YS, Ha HC, Shim JS, Lim KS (2009) A novel magnetic resonance imaging classification of discoid lateral meniscus based on peripheral attachment. Am J Sports Med 37(8):1564–1569
Acknowledgements
We would like to thank Editage (https://www.editage.com) for English language editing.
Funding
The authors did not receive support from any organization for the submitted work. No funding was received to assist with the preparation of this manuscript. No funding was received for conducting this study. No funds, grants, or other support was received. The authors have no relevant financial or non-financial interests to disclose. All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest or non-financial interest in the subject matter or materials discussed in this manuscript. The authors have no financial or proprietary interests in any material discussed in this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no conflicts of interest to declare that are relevant to the content of this article.
Ethical approval
This study approved by the hospital ethics committee and the internal review board of our institution (3071, 3072).
Informed consent
Informed consent was obtained from all participants include in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kinoshita, T., Hashimoto, Y., Nishino, K. et al. Saucerization of complete discoid lateral meniscus is associated with change of morphology of the lateral femoral condyle and tibial plateau. Arch Orthop Trauma Surg 143, 7019–7026 (2023). https://doi.org/10.1007/s00402-023-04999-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-04999-4