Abstract
Introduction
Conventional total knee arthroplasty (C-TKA) implants have well-established mid- and long-term outcomes. The novel TKA (N-TKA) implants provide morphogenic implant components with smaller size increments to facilitate anatomical replication. The aim of the study is to evaluate if these advantages provides better clinical outcomes.
Materials and methods
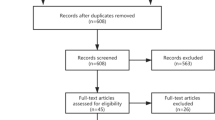
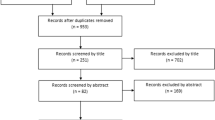
Registry data prospectively collected within a single institution from 2014 to 2018 was reviewed and propensity score matching was performed to match C-TKA to N-TKA. 70 pairs of cruciate retaining (CR) TKA and 116 pairs of posterior stabilized (PS) TKA were identified. Range of motion, SF-36, Knee Society Knee Score (KSKS), Knee Society Function Score (KSFS) and Oxford Knee Score (OKS) were assessed preoperatively, 6 and 24 months postoperatively. Satisfaction was assessed 6 and 24 months postoperatively. Independent T test was performed for parametric data, whereas Wilcoxon rank-sum analysis was performed for non-parametric data.
Results
Both C-TKA and N-TKA cohorts demonstrated statistically significant improvement for KSKS, KSFS, OKS and SF-36 at 6 and 24 months postoperatively. C-TKA CR patients had better flexion at 6 months as compared to N-TKA CR (108.7° versus 98.3°, respectively, p = 0.046). At 24 months, there was no difference between C-TKA and N-TKA for range of motion, KSKS, KSFS, OKS and SF-36 PCS, regardless of insert type (p > 0.05).
Conclusions
Both models showed great postoperative improvements in KSFS, KSKS, OKS and SF-36 and have comparable early and mid-term outcomes, suggesting that N-TKAs are suitable substitutes for C-TKA. Longer follow-up studies are required to evaluate the long-term outcomes of N-TKAs.
Level of evidence
lll.


Similar content being viewed by others
Availability of data
The datasets generated and/or analysed during the current study are available from the first author.
References
Inacio MCS, Graves SE, Pratt NL, Roughead EE, Nemes S (2017) Increase in total joint arthroplasty projected from 2014 to 2046 in Australia: a conservative local model with international implications. Clin Orthop Relat Res 475(8):2130–2137. https://doi.org/10.1007/s11999-017-5377-7
Kurtz SM et al (2011) International survey of primary and revision total knee replacement. Int Orthop. https://doi.org/10.1007/s00264-011-1235-5
NCT03568123 (2018) A comparison of the Persona Total Knee Arthroplasty System using CR or MC polyethylene. https://clinicaltrials.gov/show/nct03568123. 2018 [Online]. Available: https://www.cochranelibrary.com/central/doi/10.1002/central/CN-01660618/full
Kahlenberg CA, Nwachukwu BU, McLawhorn AS, Cross MB, Cornell CN, Padgett DE (2018) Patient satisfaction after total knee replacement: a systematic review. HSS J 14(2):192–201. https://doi.org/10.1007/s11420-018-9614-8
Dunbar MJ, Richardson G, Robertsson O (2013) I can’t get no satisfaction after my total knee replacement: rhymes and reasons. Bone Jt J 95(11):148–152. https://doi.org/10.1302/0301-620X.95B11.32767
Patil KD, Sancheti PK, Patil AA, Shyam A (2017) What makes patients of TKR unhappy? A study of subjective patient satisfaction. Arthrosc J Arthrosc Relat Surg 33(10):e117. https://doi.org/10.1016/j.arthro.2017.08.134
Howells N, Murray J, Wylde V, Dieppe P, Blom A (2016) Persistent pain after knee replacement: do factors associated with pain vary with degree of patient dissatisfaction? Osteoarthr Cartil 24(12):2061–2068. https://doi.org/10.1016/j.joca.2016.07.012
Al-Hadithy N, Rozati H, Sewell MD, Dodds AL, Brooks P, Chatoo M (2012) Causes of a painful total knee arthroplasty. Are patients still receiving total knee arthroplasty for extrinsic pathologies? Int Orthop 36(6):1185–1189. https://doi.org/10.1007/s00264-011-1473-6
Nicoll D, Rowley DI (2010) Internal rotational error of the tibial component is a major cause of pain after total knee replacement. J Bone Jt Surg Ser B. https://doi.org/10.1302/0301-620X.92B9.23516
Ranawat CS, White PB, West S, Ranawat AS (2017) Clinical and radiographic results of attune and PFC sigma knee designs at 2-year follow-up: a prospective matched-pair analysis. J Arthroplasty 32(2):431–436. https://doi.org/10.1016/j.arth.2016.07.021
Martin JR, Jennings JM, Watters TS, Levy DL, McNabb DC, Dennis DA (2017) Femoral implant design modification decreases the incidence of patellar crepitus in total knee arthroplasty. J Arthroplasty. https://doi.org/10.1016/j.arth.2016.11.025
Mohamadi A et al (2021) Evolution of knowledge on meniscal biomechanics: a 40 year perspective. BMC Musculoskelet Disord. https://doi.org/10.1186/s12891-021-04492-2
Zhang L et al (2020) Knee joint biomechanics in physiological conditions and how pathologies can affect it: a systematic review. Appl Bionics Biomech. https://doi.org/10.1155/2020/7451683
Saffarini M, Demey G, Nover L, Dejour D (2016) Evolution of trochlear compartment geometry in total knee arthroplasty. Ann Transl Med. https://doi.org/10.3978/j.issn.2305-5839.2015.12.53
Koo JH, Choi SH, Lee SA, Wang JH (2015) Comparison of medial and lateral meniscus root tears. PLoS ONE. https://doi.org/10.1371/journal.pone.0141021
A. A. Report (2021) Hip, knee & shoulder arthroplasty annual report 2021. Australian Orthopaedic Association National Joint Replacement Registry, 2021. https://aoanjrr.sahmri.com/documents/10180/732916/AOA+2022+AR+Digital/f63ed890-36d0-c4b3-2e0b-7b63e2071b16. Accessed 11 Dec 2022
Alkan BM, Fidan F, Tosun A, Ardiçoǧlu Ö (2014) Quality of life and self-reported disability in patients with knee osteoarthritis. Mod Rheumatol 24(1):166–171. https://doi.org/10.3109/14397595.2013.854046
McHorney CA, Ware JE, Raczek AE (1993) The MOS 36-Item Short-Form Health Survey (Sf-36): II. Psychometric and clinical tests of validity in measuring physical and mental health constructs. Med Care. https://doi.org/10.1097/00005650-199303000-00006
Ware JE (2000) SF-36 Health Survey update. Spine. https://doi.org/10.1097/00007632-200012150-00008
Scuderi GR, Bourne RB, Noble PC, Benjamin JB, Lonner JH, Scott WN (2012) The new Knee Society Knee Scoring System. Clin Orthop Relat Res 470(1):3–19. https://doi.org/10.1007/s11999-011-2135-0
Home. https://www.kneesociety.org/. Accessed 01 May 2022
Murray DW et al (2007) The use of the Oxford hip and knee scores. J Bone Jt Surg Ser B 89(8):1010–1014. https://doi.org/10.1302/0301-620X.89B8.19424
Beard DJ, Pandit H, Ostlere S, Jenkins C, Dodd CAF, Murray DW (2007) Pre-operative clinical and radiological assessment of the patellofemoral joint in unicompartmental knee replacement and its influence on outcome. J Bone Jt Surg Ser B. https://doi.org/10.1302/0301-620X.89B12.19260
Hassaballa MA, Porteous AJ, Newman JH, Rogers CA (2003) Can knees kneel? Kneeling ability after total, unicompartmental and patellofemoral knee arthroplasty. Knee. https://doi.org/10.1016/S0968-0160(02)00148-5
Kim JK, Park JY, Lee HJ, Ro DH, Han HS, Lee MC (2020) Do the increment of femoral condyle curvature and the change of tibia shape improve clinical outcome in total knee arthroplasty? A propensity score matching analysis. Knee Surg Sport Traumatol Arthrosc 28(9):2980–2989. https://doi.org/10.1007/s00167-019-05727-5
Rajgopal A, Aggarwal K, Kumar S (2020) A five-year comparative functional and clinical evaluation of two contemporary cruciate-retaining knee implants. Arthroplast Today. https://doi.org/10.1016/j.artd.2020.05.009
Fehring TK, Odum S, Griffin WL, Mason JB, Nadaud M (2001) Early failures in total knee arthroplasty. Clin Orthop Relat Res 392:315–318. https://doi.org/10.1097/00003086-200111000-00041
Sharkey PF, Hozack WJ, Rothman RH, Shastri S, Jacoby SM (2002) Why are total knee arthroplasties failing today? Clin Orthop Relat Res 404:7–13. https://doi.org/10.1097/00003086-200211000-00003
Petersen W et al (2014) Anterior knee pain after total knee arthroplasty: a narrative review. Int Orthop 38(2):319–328. https://doi.org/10.1007/s00264-013-2081-4
Koh IJ, In Y, Kim MS, Choi YJ, Choi KY (2017) Patellar-friendly implant does not affect patient perception of patellar management following total knee arthroplasty: a simultaneous bilateral randomized study. Arthrosc J Arthrosc Relat Surg. https://doi.org/10.1016/j.arthro.2017.08.090
van Jonbergen HPW, Reuver JM, Mutsaerts EL, Poolman RW (2014) Determinants of anterior knee pain following total knee replacement: a systematic review. Knee Surg Sports Traumatol Arthrosc 22(3):478–499. https://doi.org/10.1007/s00167-012-2294-x
Dai Y, Scuderi GR, Bischoff JE, Bertin K, Tarabichi S, Rajgopal A (2014) Anatomic tibial component design can increase tibial coverage and rotational alignment accuracy: a comparison of six contemporary designs. Knee Surg Sport Traumatol Arthrosc 22(12):2911–2923. https://doi.org/10.1007/s00167-014-3282-0
Stulberg SD, Goyal N (2015) Which tibial tray design achieves maximum coverage and ideal rotation: anatomic, symmetric, or asymmetric? An MRI-based study. J Arthroplasty 30(10):1839–1841. https://doi.org/10.1016/j.arth.2015.04.033
Maciąg BM et al (2021) Does the anatomic design of total knee prosthesis allow for a better component fit than its nonanatomic predecessor? A matched cohort Study. Arthroplast Today 12:62–67. https://doi.org/10.1016/j.artd.2021.09.001
Jin C, Song EK, Prakash J, Kim SK, Chan CK, Seon JK (2017) How much does the anatomical tibial component improve the bony coverage in total knee arthroplasty? J Arthroplasty 32(6):1829–1833. https://doi.org/10.1016/j.arth.2016.12.041
Indelli PF, Graceffa A, Baldini A, Payne B, Pipino G, Marcucci M (2015) Relationship between tibial baseplate design and rotational alignment landmarks in primary total knee arthroplasty. Arthritis 2015:1–8. https://doi.org/10.1155/2015/189294
Martin S, Saurez A, Ismaily S, Ashfaq K, Noble P, Incavo SJ (2014) Maximizing tibial coverage is detrimental to proper rotational alignment knee. Clin Orthop Relat Res 472(1):121–125. https://doi.org/10.1007/s11999-013-3047-y
Kim YH, Park JW, Kim JS, Park SD (2014) The relationship between the survival of total knee arthroplasty and postoperative coronal, sagittal and rotational alignment of knee prosthesis. Int Orthop. https://doi.org/10.1007/s00264-013-2097-9
Bédard M, Vince KG, Redfern J, Collen SR (2011) Internal rotation of the tibial component is frequent in stiff total knee arthroplasty. Clin Orthop Relat Res 469(8):2346–2355. https://doi.org/10.1007/s11999-011-1889-8
Bizzozero P, Bulaid Y, Flecher X, Ollivier M, Parratte S, Argenson JN (2018) Morphometric tibial implant decreases posterior overhang rate and improves clinical outcomes: results of a prospective, matched controlled study. J Arthroplasty. https://doi.org/10.1016/j.arth.2018.04.020
Lee JK, Choi CH (2012) Total knee arthroplasty in rheumatoid arthritis. Knee Surg Relat Res. https://doi.org/10.5792/ksrr.2012.24.1.1
Shan Wang X, Xin Zhou Y, Yi Shao H, Jin Yang D, Huang Y, Fang Duan F (2020) Total knee arthroplasty in patients with prior femoral and tibial fractures: outcomes and risk factors for surgical site complications and reoperations. Orthop Surg 12(1):210–217. https://doi.org/10.1111/os.12610
Dietz MJ, Sprando D, Hanselman AE, Regier MD, Frye BM (2017) Smartphone assessment of knee flexion compared to radiographic standards. Knee 24(2):224–230. https://doi.org/10.1016/j.knee.2016.11.014
Galea VP, Botros MA, Madanat R, Nielsen CS, Bragdon C (2019) Promising early outcomes of a novel anatomic knee system. Knee Surg Sport Traumatol Arthrosc 27(4):1067–1074. https://doi.org/10.1007/s00167-018-5248-0
Mathijssen NMC, Verburg H, London NJ, Landsiedl M, Dominkus M (2019) Patient reported outcomes and implant survivorship after total knee arthroplasty with the persona knee implant system: two year follow up. BMC Musculoskelet Disord. https://doi.org/10.1186/s12891-019-2470-y
Annual reports. National Joint Registry. https://www.njrcentre.org.uk/njrcentre/Reports-Publications-and-Minutes/Annual-reports. Accessed 10 Dec 2021
2021-AOANJRR. Australian Orthopaedic Associate National Joint Replacement Registry. https://aoanjrr.sahmri.com/annual-reports-2021. Accessed 10 Dec 2021
Koster LA, Meinardi JE, Kaptein BL, VanderLinden-VanderZwaag E, Nelissen RGHH (2021) Two-year RSA migration results of symmetrical and asymmetrical tibial components in total knee arthroplasty: a randomized controlled trial. Bone Jt J. https://doi.org/10.1302/0301-620X.103B5.BJJ-2020-1575.R2
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
All authors contributed to the design of the study, data collection and processing and analysis of data. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest. The authors of this paper have no conflicts of interest to declare.
Ethical approval
An Institutional Review Board approval (CIRB 2020-2750) was granted for this study.
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sim, C.H.S., Chen, J.D.Y., Pang, H.N. et al. Novel morphogenic knee implant delivers comparable mid-term outcomes as compared to conventional non-morphogenic implants. Arch Orthop Trauma Surg 143, 7159–7167 (2023). https://doi.org/10.1007/s00402-023-04990-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-04990-z