Abstract
Introduction
Tibial slope is a parameter that is important to recognize in knee kinematics and knee surgery. A very wide range of values governing posterior tibial slope exist in the literature. This study is based on the hypothesis that age, gender and region may have an effect on the tibial slope.
Materials and methods
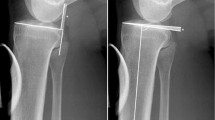
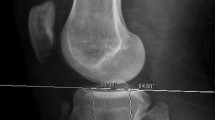
A total of 1800 lateral knee radiographies from five different countries [Turkey, Germany, Italy, Spain, and the United Kingdom (UK)] were utilized to measure the native posterior tibial slope. Participants were categorized in deciles with each decade of age after 40 years determined as a separate age group. Accordingly, four different age categories were formed in total, namely, the 40- to 49-, 50- to 59-, 60–69, and 70- to 79-year-old groups. Patients with severe knee osteoarthritis, those with a history of arthroscopic and open surgery around the knee, and those with severe morbid obesity and those outside the specified age group were excluded from the study. The angle between the line tangential to the medial tibial plateau and the proximal anatomical axis of the tibia was measured.
Results
The tibial slope values of both males and females in the Turkish population were found to be higher than those in other populations. It was observed that tibial slope values increased with age in females in all populations, except for those in the Spanish and UK populations. In the male population, it was found that tibial slope values increased with age in all populations except in the Spanish population.
Conclusions
Region, age, and gender affect tibial slope in different populations in various ways. Our study shows that the region an individual lives in and living conditions affect the tibial slope.




Similar content being viewed by others
Data availability
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
References
Ahmad R, Patel A, Mandalia V, Toms A (2016) Posterior tibial slope: effect on, and Interaction with, knee kinematics. JBJS Rev. https://doi.org/10.2106/JBJS.RVW.O.00057
Wordeman SC, Quatman CE, Kaeding CC, Hewett TE (2012) In vivo evidence for tibial plateau slope as a risk factor for anterior cruciate ligament injury: a systematic review and meta-analysis. Am J Sports Med 40:1673–1681. https://doi.org/10.1177/0363546512442307
Fujimoto E, Sasashige Y, Tomita T et al (2014) Significant effect of the posterior tibial slope on the weight-bearing, midflexion in vivo kinematics after cruciate-retaining total knee arthroplasty. J Arthroplasty 29:2324–2330. https://doi.org/10.1016/J.ARTH.2013.10.018
Korthaus A, Krause M, Pagenstert G et al (2022) Tibial slope in the posterolateral quadrant with and without ACL injury. Arch Orthop Trauma Surg 142:3917–3925. https://doi.org/10.1007/S00402-021-04298-W
Dejour H, Bonnin M (1994) Tibial translation aj3ter anterior cruciate ligament rupture two radiological tests compared
Moore TM, Harvey JPJR (1974) Roentgenographic measurement of tibial-plateau depression due to fracture. J Bone Jt Surg 56:155–160
Brazier J, Migaud H, Gougeon F et al (1996) Evaluation of methods for radiographic measurement of the tibial slope. A study of 83 healthy knees. Rev Chir Orthop Reparatrice Appar Mot 82:195–200
Haddad B, Konan S, Mannan K, Scott G (2012) Evaluation of the posterior tibial slope on MR images in different population groups using the tibial proximal anatomical axis. Acta Orthop Belg 78:757–763
de Boer JJ, Blankevoort L, Kingma I, Vorster W (2009) In vitro study of inter-individual variation in posterior slope in the knee joint. Clin Biomech (Bristol, Avon) 24:488–492. https://doi.org/10.1016/J.CLINBIOMECH.2009.03.008
Hashemi J, Chandrashekar N, Gill B et al (2008) The geometry of the tibial plateau and its influence on the biomechanics of the tibiofemoral joint. J Bone Jt Surg Am 90:2724–2734. https://doi.org/10.2106/JBJS.G.01358
Jenny JY, Boéri C, Ballonzoli L, Meyer N (2005) Difficulties and reproducibility of radiological measurement of the proximal tibial axis according to Lévigne. Rev Chir Orthop Reparatrice Appar Mot 91:658–663. https://doi.org/10.1016/S0035-1040(05)84470-8
Hudek R, Schmutz S, Regenfelder F et al (2009) Novel measurement technique of the tibial slope on conventional MRI. Clin Orthop Relat Res 467:2066–2072. https://doi.org/10.1007/S11999-009-0711-3
Misir A, Yildiz KI, Kizkapan TB (2019) Wider femoral and mediolaterally narrower tibial components are required for total knee arthroplasty in Turkish patients. Knee Surg Sports Traumatol Arthrosc 27:2155–2166. https://doi.org/10.1007/S00167-019-05448-9
Li P, Tsai TY, Li JS et al (2014) Morphological measurement of the knee: race and sex effects. Acta Orthop Belg 80:260–268
Han H, Oh S, Chang CB, Kang SB (2016) Anthropometric difference of the knee on MRI according to gender and age groups. Surg Radiol Anat 38:203–211. https://doi.org/10.1007/S00276-015-1536-2
Kim TK, Phillips M, Bhandari M et al (2017) What differences in morphologic features of the knee exist among patients of various races? A systematic review. Clin Orthop Relat Res 475:170–182. https://doi.org/10.1007/S11999-016-5097-4
Medda S, Kundu R, Sengupta S, Pal AK (2017) Anatomical variation of posterior slope of tibial plateau in adult Eastern Indian population. Indian J Orthop 51:69–74. https://doi.org/10.4103/0019-5413.197545
Kacmaz IE, Topkaya Y, Basa CD et al (2020) Posterior tibial slope of the knee measured on X-rays in a Turkish population. Surg Radiol Anat 42:673–679. https://doi.org/10.1007/S00276-020-02430-W
Kuwano T, Urabe K, Miura H et al (2005) Importance of the lateral anatomic tibial slope as a guide to the tibial cut in total knee arthroplasty in Japanese patients. J Orthop Sci 10:42–47. https://doi.org/10.1007/S00776-004-0855-7
Moller JT, Weeth RE, Keller JO, Nielsen S (1985) Unicompartmental arthroplasty of the knee. Cadaver study of the importance of the anterior cruciate ligament. Acta Orthop Scand 56:120–123. https://doi.org/10.3109/17453678508994333
Pangaud C, Laumonerie P, Dagneaux L et al (2020) Measurement of the posterior tibial slope depends on ethnicity, sex, and lower limb alignment: a computed tomography analysis of 378 healthy participants. Orthop J Sports Med. https://doi.org/10.1177/2325967119895258
Winkler PW, Godshaw BM, Karlsson J et al (2021) Posterior tibial slope: the fingerprint of the tibial bone. Knee Surg Sports Traumatol Arthrosc 29:1687–1689. https://doi.org/10.1007/S00167-021-06578-9
Bisicchia S, Scordo GM, Prins J, Tudisco C (2017) Do ethnicity and gender influence posterior tibial slope? J Orthop Traumatol 18:319–324. https://doi.org/10.1007/S10195-017-0443-1
Chen Y, Ding J, Dai S et al (2022) Radiographic measurement of the posterior tibial slope in normal Chinese adults: a retrospective cohort study. BMC Musculoskelet Disord. https://doi.org/10.1186/S12891-022-05319-4
Sun YH, Chen LX, de Jiao Z et al (2015) Age-related changes of posterior tibial slope and its roles in anterior cruciate ligament injury. Int Surg 101:70–77. https://doi.org/10.9738/INTSURG-D-15-00127.1
Weinberg DS, Williamson DFK, Gebhart JJ et al (2017) Differences in medial and lateral posterior tibial slope: an osteological review of 1090 tibiae comparing age, sex, and race. Am J Sports Med 45:106–113. https://doi.org/10.1177/0363546516662449
Hashemi J, Chandrashekar N, Mansouri H et al (2010) Shallow medial tibial plateau and steep medial and lateral tibial slopes: new risk factors for anterior cruciate ligament injuries. Am J Sports Med 38:54–62. https://doi.org/10.1177/0363546509349055
Thilak J, George MJ (2016) Patient - implant dimension mismatch in total knee arthroplasty: is it worth worrying? An Indian scenario. Indian J Orthop 50:512–517. https://doi.org/10.4103/0019-5413.189618
Fan L, Xu T, Li X et al (2017) Morphologic features of the distal femur and tibia plateau in Southeastern Chinese population: a cross-sectional study. Medicine. https://doi.org/10.1097/MD.0000000000008524
Calek AK, Hochreiter B, Hess S et al (2022) High inter- and intraindividual differences in medial and lateral posterior tibial slope are not reproduced accurately by conventional TKA alignment techniques. Knee Surg Sports Traumatol Arthrosc 30:882–889. https://doi.org/10.1007/S00167-021-06477-Z
Weber P, Gollwitzer H (2022) Arthroplasty of the knee: current techniques for implant alignment. Z Orthop Unfall 160:149–159. https://doi.org/10.1055/A-1304-3854
Chen Z, Chen K, Yan Y et al (2021) Effects of posterior tibial slope on the mid-term results of medial unicompartmental knee arthroplasty. Arthroplasty (London, England). https://doi.org/10.1186/S42836-021-00070-Y
Okazaki K, Tashiro Y, Mizu-uchi H et al (2014) Influence of the posterior tibial slope on the flexion gap in total knee arthroplasty. Knee 21:806–809. https://doi.org/10.1016/J.KNEE.2014.02.019
Seo SS, Kim CW, Kim JH, Min YK (2013) Clinical results associated with changes of posterior tibial slope in total knee arthroplasty. Knee Surg Relat Res 25:25–29. https://doi.org/10.5792/KSRR.2013.25.1.25
Okamoto S, Mizu-uchi H, Okazaki K et al (2015) Effect of tibial posterior slope on knee kinematics, quadriceps force, and patellofemoral contact force after posterior-stabilized total knee arthroplasty. J Arthroplasty 30:1439–1443. https://doi.org/10.1016/J.ARTH.2015.02.042
Weber P, Gollwitzer H (2021) Kinematic alignment in total knee arthroplasty. Oper Orthop Traumatol 33:525–537. https://doi.org/10.1007/S00064-021-00729-4
Bernhardson AS, DePhillipo NN, Daney BT et al (2019) Posterior tibial slope and risk of posterior cruciate ligament injury. Am J Sports Med 47:312–317. https://doi.org/10.1177/0363546518819176
Hohmann E, Bryant A, Reaburn P, Tetsworth K (2011) Is there a correlation between posterior tibial slope and non-contact anterior cruciate ligament injuries? Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/S00167-011-1547-4
Giffin JR, Vogrin TM, Zantop T et al (2004) Effects of increasing tibial slope on the biomechanics of the knee. Am J Sports Med 32:376–382. https://doi.org/10.1177/0363546503258880
Hees T, Zielke J, Petersen W (2023) Effect of anterior tibial bowing on measurement of posterior tibial slope on conventional X-rays. Arch Orthop Trauma Surg. https://doi.org/10.1007/S00402-022-04507-0
Sessa P, Fioravanti G, Giannicola G, Cinotti G (2015) The risk of sacrificing the PCL in cruciate retaining total knee arthroplasty and the relationship to the sagittal inclination of the tibial plateau. Knee 22:51–55. https://doi.org/10.1016/J.KNEE.2014.10.006
Waiwaiole A, Gurbani A, Motamedi K et al (2016) Relationship of ACL injury and posterior tibial slope with patient age, sex, and race. Orthop J Sports Med. https://doi.org/10.1177/2325967116672852
Nazzal EM, Zsidai B, Pujol O et al (2022) Considerations of the posterior tibial slope in anterior cruciate ligament reconstruction: a scoping review. Curr Rev Musculoskelet Med. https://doi.org/10.1007/S12178-022-09767-2
Rozinthe A, van Rooij F, Demey G et al (2022) Tibial slope correction combined with second revision ACLR grants good clinical outcomes and prevents graft rupture at 7–15-year follow-up. Knee Surg Sports Traumatol Arthrosc 30:2336–2341. https://doi.org/10.1007/S00167-021-06750-1
Weiler A, Gwinner C, Wagner M et al (2022) Significant slope reduction in ACL deficiency can be achieved both by anterior closing-wedge and medial open-wedge high tibial osteotomies: early experiences in 76 cases. Knee Surg Sports Traumatol Arthrosc 30:1967–1975. https://doi.org/10.1007/S00167-022-06861-3
Funding
No funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There is no conflict of interest of the authors.
Ethical approval
Ethical approval obtained.
Informed consent
This study is a radiographic study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Akçaalan, S., Akkaya, M., Dogan, M. et al. Do age, gender, and region affect tibial slope? A multi-center study. Arch Orthop Trauma Surg 143, 6983–6991 (2023). https://doi.org/10.1007/s00402-023-04976-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-04976-x